Introduction
Hemifacial microsomia is the most common congenital craniofacial anomaly after cleft lip and palate. The purpose of this study was to evaluate the final outcome of team care for patients with hemifacial microsomia after a protocol of growth management, orthodontic treatment, orthognathic surgery, and soft-tissue augmentation.
Methods
This was a retrospective study with chart reviews, radiographs, and photographs to document the treatment interventions and outcomes. Six patients, 2 in each of 3 mandibular types, who had recently completed treatment and had complete records available and were not previously reported, were included. Facial midlines and maxillary and mandibular deviations from the midline were measured.
Results
The maxillary deviation changed by 10.0 ± 4.6 mm to a deviation from the midline of 1.1 ± 0.6 mm. The chin deviation improved by 8.1 ± 2.7 mm to a mean distance of 0.6 ± 0.5 mm from the midline. The occlusal plane cant changed from 7.0° ± 4.2° to 2.3° ± 1.4°. All changes were significant.
Conclusions
Facial asymmetry in patients with hemifacial microsomia can be significantly improved by stepwise orthodontic treatment, orthognathic and facial surgery, and soft-tissue augmentation. As for most craniofacial conditions, team care is essential.
Hemifacial microsomia is the most common congenital craniofacial anomaly after cleft lip and palate, occurring in 1 of every 4000 to 5600 live births. The term oculo-auriculo-vertebral syndrome is used interchangeably with hemifacial microsomia. This congenital condition predominantly involves structures of the first and second branchial arches, such as the ears and the mandible with associated soft tissues, but it can also involve structures that are not derived from the branchial arches, such as the zygoma, the temporal bones, and the teeth. Hemifacial microsomia most often is unilateral, although bilateral involvement can occur. The etiology and pathogenesis of hemifacial microsomia are unknown. The condition is believed to be sporadic, although there are documented examples of familial transmission. A causal gene was mapped to 14q32 in 1 family but not in another affected family, suggesting genetic heterogeneity. The 2 proposed etiopathogenic theories include hematoma occurrence at the first and second branchial arches during fetal development and abnormal neural crest development and migration. Both models explain the variable and asymmetric nature of this condition.
The clinical presentation is variable, and many classification systems have been developed. Three mandibular types were described by Pruzansky. In type I, the temporomandibular joint and ramus are well formed but smaller than normal. In type II, the temporomandibular joint, ramus, and glenoid fossa are hypoplastic and malformed. In type III, the entire ramus is missing. Because the structures that are responsible for mandibular growth are affected, there is usually marked growth disturbance, varying in degree according to the extent of malformation. It is generally accepted that interdisciplinary team care is the most efficacious way to achieve the best outcomes, both functionally and esthetically. Management of the asymmetries in patients with hemifacial microsomia requires a series of treatment phases that target interception and correction of the asymmetries in both the maxilla and the mandible: orthopedic or functional appliance treatment during growth, and presurgical orthodontic treatment followed by mandibular and maxillary surgery. Additionally, genioplasty, rhinoplasty, and soft-tissue augmentation after the occlusal and skeletal corrections are effective in improving facial symmetry.
Computed tomography with 3-dimensional reconstruction is currently routinely used to clearly delineate the asymmetries in patients with hemifacial microsomia. These images not only demonstrate the asymmetry of the facial bones, but also allow assessment of inclination of the teeth, cranial base asymmetries, and soft-tissue deficiencies. However, the posteroanterior cephalogram is still most commonly used for assessing facial asymmetry. On this image, maxillary and mandibular deviations from the midline, differences in ramus height, and occlusal cant can be measured. In conjunction with facial photographs, the posteroanterior radiograph can therefore be useful in assessing facial asymmetry and some treatment outcome parameters.
Treatment goals include good facial symmetry within normal limits, functional jaw movement, good occlusion, and a satisfied patient. Current treatment approaches build on long-term follow-ups and lessons learned. In this article, we present the outcomes of recently treated patients with hemifacial microsomia.
Material and methods
This was a retrospective study carried out on chart reviews and radiographs to document timing, types, and outcomes of treatment interventions. Twenty-two patients with the diagnosis of hemifacial microsomia or oculo-auriculo-vertebral syndrome were included as the beginning sample. The inclusion criteria for subjects in this study were (1) diagnosed with hemifacial microsomia or oculo-auriculo-vertebral without other anomalies, syndromes, or restricted joint movement; (2) completed orthodontic, skeletal, and soft-tissue treatment provided by our team; (3) complete records of cephalograms and facial photographs before and at least 1 year after the last surgery; (4) not previously included in a published study; and (5) representing the 3 major types of mandibular involvement. Four male and 2 female patients met these criteria, with 2 in each of the 3 types of mandibular involvement ( Table I ).
| Patient | Sex | Type | Phase 1 treatment | Early surgery | Phase 2 treatment | Surgical procedures (age) | Ear reconstruction | Fat augmentation |
|---|---|---|---|---|---|---|---|---|
| 1 | Male | I | + | − | + | BSSO, LeFort I, genio (14 y 7 mo) | − | − |
| 2 | Female | I | + | − | + | BSSO, LeFort I (17 y 5 mo) | − | − |
| 3 | Male | II | + | − | + | Right CG, BSSO, LeFort I, genio (21 y 11 mo) | + | − |
| 4 | Male | II | + | − | + | Right distraction, BSSO, LeFort I (18 y 5 mo) | + | + |
| 5 | Female | III | + | − | + | Right CG, BSSO, LeFort I, genio (15 y 4 mo) | − | + |
| 6 | Male | III | + | − | + | Left CG, BSSO, LeFort I, genio (20 y 8 mo) | − | + |
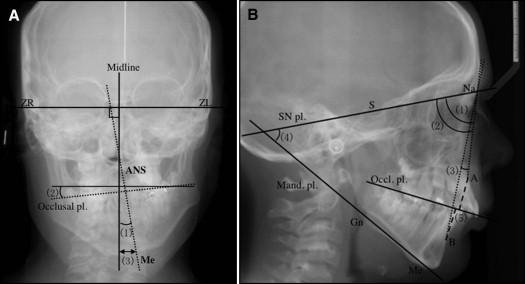
The classification of mandibular type (I, II, or III) was determined from panoramic radiographs. Posteroanterior and lateral cephalometric analysis was done before (T1) and at least 1 year after (T2) orthognathic surgery or soft-tissue augmentation. Tracings of all cephalograms were done by 2 senior orthodontists (S.O. and J.O.), and the means were used. Angular and linear measurements on the posteroanterior and lateral cephalograms are illustrated in Figure 1 . The Sassouni method was used to determine the facial midline, and the deviation from the midline was measured by using the following parameters: maxillomandibular deviation, occlusal plane cant, and chin deviation. Lateral cephalograms were assessed for SNA, SNB, ANB, and SN-MP as the angular measurements. The Wits appraisal was also done.
Statistical analysis
The T1 and T2 measurements were compared by paired t test with a confidence level greater than 95%. All data are presented as means and standard deviations.
Results
Posteroanterior cephalometric measurements at T1 and T2 are shown in Table II . Deviations of the maxilla and the mandible of the facial midline were indicated by a plus sign to the right side and by a minus sign to the left side. Three subjects had right-side deviations, and 3 had left-side deviations. The mean skeletal deviations were 9.9 ± 3.7 mm of the maxilla, and 8.8 ± 2.9 mm of menton. The occlusal cant was 7.0° ± 4.2°. At completion of treatment, all patients showed significant reductions in asymmetry. The maxillary deviation changed by 10.0 ± 4.6 mm to a deviation from the midline of 1.1 ± 0.6 mm. The chin deviation improved by 8.1 ± 2.7 mm to a mean distance of 0.6 ± 0.5 mm from the midline. The occlusal plane cant changed from 7.0° ± 4.2° to 2.3° ± 1.4°. All changes were highly significant.
| Patient | Maxillomandibular deviation (°) | Occlusal plane cant (°) | Lateral shift of menton (mm) | |||
|---|---|---|---|---|---|---|
| Before surgery | After surgery | Before surgery | After surgery | Before surgery | After surgery | |
| 1 | −10.2 | −1.8 | −5.5 | −3 | −10 | −1 |
| 2 | 7.4 | 0.1 | 5.1 | 2.5 | 6 | 0 |
| 3 | 11.4 | −1.7 | 10.3 | 4.7 | 10 | 1 |
| 4 | 16.1 | −1.1 | 12.1 | 2.1 | 13 | 1 |
| 5 | −9.3 | 1 | −0.4 | 0.6 | −9 | 0 |
| 6 | −5 | −1.1 | −9.1 | −1 | −5 | −1 |
| Means | 9.90 ± 3.7 | 1.13 ± 0.6 | 7.08 ± 4.2 | 2.31 ± 1.4 | 8.83 ± 2.9 | 0.66 ± 0.5 |
| Mean change | 10.03 † | 4.96 ∗ | 8.16 † | |||
Lateral cephalometric measurements at T1 and T2 are shown in Table III . Both the maxilla and the mandible were retrognathic according to the norms, with SNA at 76.4° ± 3.8°, SNB at 70.0° ± 4.0°, and mean ANB angle at 6.3° ± 3.6°. The mandibular plane angle (SN-MP) was 49.9° ± 8.57° (adult standard, 33.0° ± 6.0°). The Wits appraisal was 0.6 ± 4.9 mm.
| Patient | SNA (°) | SNB (°) | ANB (°) | SN-MP (°) | Wits appraisal (mm) | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Before surgery | After surgery | Before surgery | After surgery | Before surgery | After surgery | Before surgery | After surgery | Before surgery | After surgery | |
| 1 | 76.2 | 77.2 | 68.7 | 71.2 | 7.5 | 6 | 50 | 49.3 | 8.5 | −0.8 |
| 2 | 83.8 | 82.2 | 76.2 | 77.9 | 7.6 | 4.4 | 37.1 | 37 | 1 | 1.4 |
| 3 | 72.8 | 70.8 | 71.8 | 70 | 1 | 0.7 | 45.8 | 44.3 | −6.1 | −4 |
| 4 | 75.5 | 73.5 | 67.2 | 71.2 | 8.3 | 2.3 | 55.1 | 45.3 | −0.7 | −4.7 |
| 5 | 75.5 | 76.1 | 64.8 | 68.8 | 10.7 | 7.3 | 62.5 | 58.3 | 3 | 0.1 |
| 6 | 74.6 | 75.5 | 71.7 | 74.7 | 2.9 | 0.7 | 48.9 | 45.6 | −1.7 | −4.5 |
| Means | 76.4 ± 3.8 | 75.8 ± 3.8 | 70.0 ± 4.0 | 72.3 ± 3.3 | 6.3 ± 3.6 | 3.5 ± 2.7 | 49.9 ± 8.5 | 46.6 ± 6.9 | — | — |
| Mean change | −0.5 ± 1.4 | 2.2 ± 2.1 | 2.7 ± 1.9 | 3.1 ± 3.5 | −1.1 ± 4.7 | |||||
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


