Interdisciplinary treatment was used for an adult patient born with complete bilateral cleft lip and palate. He had a severe maxillary deficiency with a wide cleft involving the alveolar and maxillary bone and palate. Reconstruction of the arches and occlusion in patients who missed the optimal treatment time is a difficult task for orthodontists. The clinical examination showed severe hypogenesis of the maxillary bone with a total crossbite. The maxillary dental arch was extremely narrow, and the maxillary incisors showed extensive caries caused by improper oral hygiene. Fixed and removable expansion appliances were used to improve the lateral crossbite. Alveolar bone grafting and unilateral LeFort I maxillary osteotomy were performed on the right side for alignment of the maxillary arch. Mandibular setback with bilateral sagittal split ramus osteotomy was also performed to correct the anteroposterior skeletal discrepancy. After postsurgical orthodontic treatment, prosthetic treatment was carried out for final reconstruction of esthetics and orthognathic function. Interdisciplinary treatment was necessary for this patient to achieve a proper occlusion and better esthetics.
Cleft lip and palate (CLP) is generally considered to be a congenital birth defect. Miyazaki et al reported that the prevalence of CLP in the Japanese population is 0.18%. The prevalence of patients with complete bilateral CLP is relatively low, and the results of treatment in these patients are less favorable than those achieved in patients with unilateral CLP. The long-term treatment protocol for patients with CLP is well established and includes palatal closure, alveolar bone grafting, and orthognathic surgeries such as maxillary distraction osteogenesis.
In Japan, few patients with bilateral CLP fail to take advantage of this long-term treatment protocol. In this report, we present a young adult patient with severe maxillary retrusion and collapse of the maxillary arch resulting from bilateral CLP; interdisciplinary treatment was provided to correct the functional problems and improve facial esthetics.
Diagnosis and etiology
The patient was a 21-year-old Japanese man. He was born with complete bilateral CLP with no other associated syndromes. He was not examined by an oral surgeon or an orthodontist until he was 21 years old. He complained of difficulty in speech and mastication as well as an unesthetic facial appearance.
Frontal facial photographs before treatment showed that the upper lip was extensively scarred because of the closure of the bilateral cleft lip. He showed no asymmetry in the frontal view. The lateral-view photograph showed a slightly concave facial profile with a protruded lower lip ( Fig 1 ). The maxillary dental arch was severely collapsed. The posterior segments were severely constricted because of scarring in the palatal area; consequently, the premaxillary segment was pushed out. The maxillary and mandibular dental arches showed a total crossbite in which the buccal segments, except for the molars, had nonocclusion ( Fig 2 ). The maxillary incisors and some posterior teeth in both arches showed extensive caries from poor oral hygiene. Overbite and overjet were −3.5 and −3.0 mm, respectively, measured from the maxillary right incisor root stump to the mandibular incisors. The mandibular left first and second premolars were submerged relative to the occlusal plane. The dental cast analysis showed that the maxillary basal arch width was extremely narrow (16.0 mm) compared with the Japanese mean value (49.48 mm).
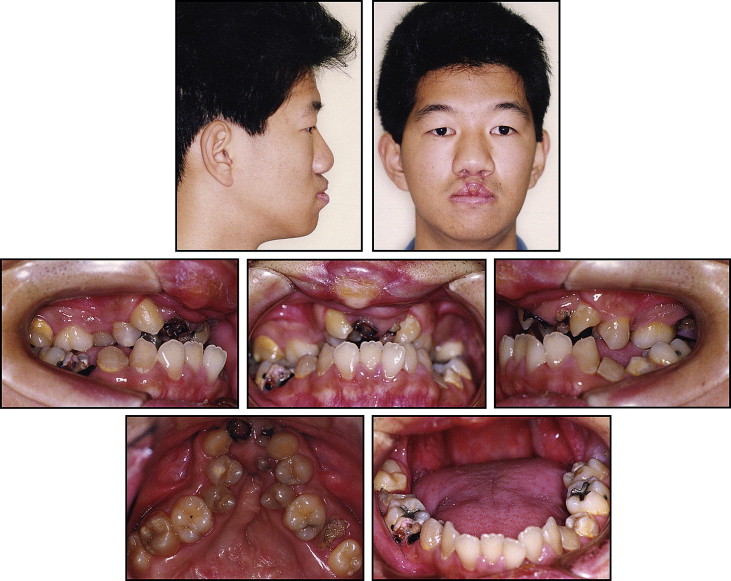
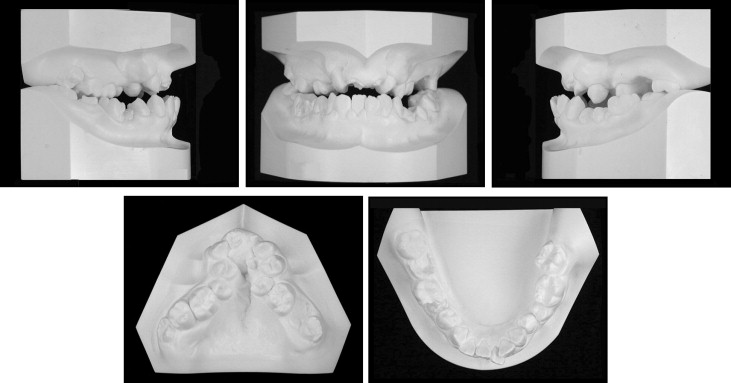
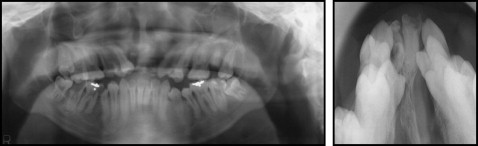
A panoramic radiograph showed the severely decayed teeth in both the maxillary and mandibular arches. The crowns of the maxillary central incisors and left second molar, and the mandibular right second premolar and second molar were severely broken down. Both maxillary lateral incisors were missing, with only the central incisor retaining roots in the premaxillary area. The occlusal radiograph showed a considerable defect in the palatal bone and a small amount of osseous tissue remaining in the premaxillary segment ( Fig 3 ).
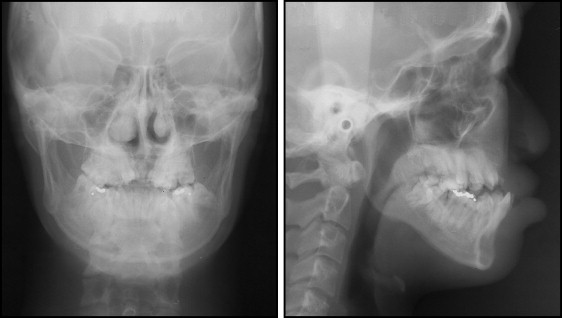
The cephalometric analysis showed that the SNA angle was 76.0°, and the ANB angle was −1.2°, indicating a moderate sagittal skeletal discrepancy ( Fig 4 , Table ). Other values of skeletal and dental parameters were almost normal compared with the Japanese norms. There were no signs or symptoms of temporomandibular joint disorder during mandibular movement.
| Mean | SD | Pretreatment | Posttreatment | |
|---|---|---|---|---|
| Intercanine width | ||||
| Maxillary arch (mm) | 37.92 | 2.68 | 16.0 | 36.7 |
| Mandibular arch (mm) | 28.82 | 2.99 | 26.3 | 29.5 |
| Basal arch width | ||||
| Maxillary arch (mm) | 49.48 | 3.89 | 35.3 | 45.0 |
| Mandibular arch (mm) | 41.78 | 2.92 | 39.9 | 39.1 |
| Skeletal pattern | ||||
| Facial angle (°) | 87.37 | 2.81 | 85.8 | 85.7 |
| SNA (°) | 81.42 | 3.64 | 76.0 | 76.0 |
| SNB (°) | 79.61 | 3.93 | 77.2 | 74.0 |
| ANB (°) | 1.81 | 1.57 | −1.2 | +2.0 |
| FMA (°) | 25.62 | 5.56 | 29.4 | 28.3 |
| Gonial angle (°) | 112.36 | 6.01 | 122.1 | 117.7 |
| Denture pattern | ||||
| L-1 to MP (°) | 94.71 | 6.89 | 94.2 | 89.2 |
| FMIA (°) | 58.01 | 6.00 | 56.4 | 62.5 |
Treatment objectives
The treatment objectives were to (1) expand the extremely collapsed maxillary arch, (2) surgically correct the sagittal skeletal discrepancy between the maxillary and mandibular dental arches, (3) rehabilitate the maxillary incisor area with a prosthetic device, and (4) surgically improve the upper lip and the nose.
Treatment objectives
The treatment objectives were to (1) expand the extremely collapsed maxillary arch, (2) surgically correct the sagittal skeletal discrepancy between the maxillary and mandibular dental arches, (3) rehabilitate the maxillary incisor area with a prosthetic device, and (4) surgically improve the upper lip and the nose.
Treatment alternatives
Treatment options for patients with bilateral cleft palate vary depending on the patient’s age and the severity of the skeletal and dental conditions. For this patient, 2 main problems had to be solved: the extremely collapsed maxillary dental arch and the functional and esthetic disturbances because of the residual roots in the premaxillary area that affected mastication and speech.
The extremely collapsed maxillary dental arch had to be expanded initially. Generally, the 2 main treatment options are rapid palatal expansion and slow expansion. It was difficult to apply a rapid palatal expansion appliance to the extremely collapsed maxillary arch and also difficult for the patient to adapt to the heavy intermittent force because of his age. Therefore, slow expansion was chosen. A fixed slow expansion appliance would be used initially to expand the maxillary arch. When adequate space was gained, a removable expansion appliance with artificial teeth could be placed; this appliance would improve both function and esthetics.
Treatment plan
The patient was told that the treatment would be performed in several stages, as follows: (1) extraction of the residual root tips of the maxillary incisors, followed by expansion of the collapsed maxillary dental arch with a quad-helix and denture-type expansion appliances; (2) secondary alveolar bone grafting in the cleft space on both sides after expansion in both arches with a multi-bracketed appliance; (3) mandibular setback by bilateral sagittal split ramus osteotomy; (4) correction of the soft tissues of the lip and nose by plastic surgery and restoration of the maxillary anterior area with a denture; and (5) retention.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


