Fig. 5.1
Affected female patient with X-linked hypohidrotic ectodermal dysplasia (HED) demonstrating many of the phenotypic features of HED including alopecia, dry skin, thin nose, prominent chin point, periorbital pigmentation, etc. Carrier females with X-linked HED often demonstrate a range of phenotypic expression depending on when X-inactivation occurs during development
In regard to the dental malformations, the largest physiological issues are loss of function, lack of alveolar ridge development, arch length tooth size discrepancies, and hyposalivation. The latter can place the patient at a high risk of dental decay. The North American National Foundation for Ectodermal Dysplasias (www.NFED.org) has led an effort to create a consensus on timing, dental therapy, and realistic approaches to oral rehabilitation in children and young adults affected with the EDs. These guidelines outline tooth replacement therapy that is both fixed to teeth and removable with or without oral implant options. Implant therapy is primarily for the skeletally mature adult [3–8]. A leading principle of these guidelines is to provide age-appropriate therapies that holistically respect the integrity of the patient and cultural competency and provide staged therapies allowing the patient to adapt to each approach as they are undergoing what growth potential they have [9–11]. Note also, in this discussion, that it is often better to use the medical term “care plan” rather than “treatment plan” since the latter suggests something is needed (when it may not) and indicates the long-term interests of the patient and their holistic perceived outcomes of care are more important (patient-centric care) than any clinical perception of care or the superiority thereof [10–16].
In the young child (age 0–6), a care plan involving removable prosthesis can usually be considered around the age of 3 (shortly after being potty trained, a relative perception of body awareness). Any young child should see a dentist by the age of 1 (American Academy of Pediatric Dentistry recommendations), and if multiple teeth are missing, a potential diagnosis of one of the ectodermal dysplasias should be contemplated (Fig. 5.2). A pediatric dentist is often the lead consultant although it may be useful to consult with a prosthodontist who is comfortable managing the affected individual as an adult. In this way, the affected individual builds a bond of trust with the entire care team and there is a better transition of care as they reach adulthood. At the initial appointment, an exam of the number and shape of the current erupted teeth should be made along with palpation of tooth buds. The integrity of the palate and the degree of salivation should be noted. Generally a removable or pediatric fixed prosthesis can be considered (Fig. 5.3) [6]. This is usually performed by a pediatric dentist and/or coordinated with a prosthodontist. The dentures and denture teeth need to be age appropriate in shape, size, and dimensions [17, 18]. If a partial or overdenture approach is used, the parents/caregiver has to be sure to clean the retainer teeth thoroughly on a daily basis and to consider the use of aggressive preventive therapies (e.g., 5 % NaF varnish). If decalcification occurs on the primary teeth, composite resin, zirconium, stainless steel, or related crowns may be indicated. Note that with HED, the incisors and canines often erupt with very sharp fang-like shapes (Fig. 5.2). In this case, the most conservative approach is to bond composite and dome these either as overdenture abutments or fashion the crown shape into an age-appropriate dimension.
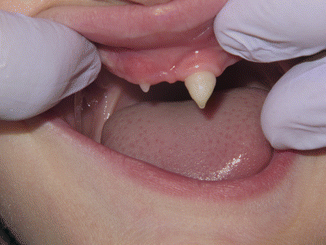
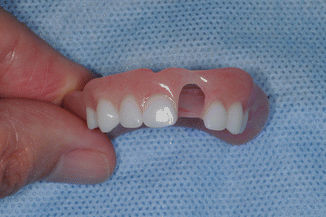

Fig. 5.2
Common presenting oral condition in the X-linked HED including multiple missing teeth (oligodontia); sharp, pointed incisal development of the central incisors; and thin or aplastic ridge development

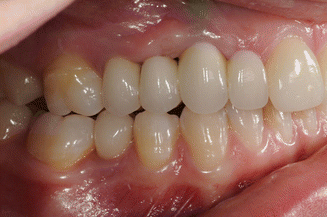
Fig. 5.3
Denture fabrication in the young child is limited to complete or simple acrylic partial dentures with space provided to allow continued eruption of the teeth
In the young child, the prosthetic steps are often simplified relative to the adult complete or partial denture approaches due to timing, need for replacement, resources, and patient tolerance. In a young patient presenting with multiple missing primary and permanent teeth, making a final impression, often with a well-fitting stock tray and a fast setting impression material (e.g., occlusal registration material), may be sufficient. It is also useful to have a pediatric dentist as the lead of the care team and a prosthodontist in a supporting role. A jaw relationship appointment and delivery appointment typically work with a measurement of the length of the lip in the premaxilla region (vestibule to vermillion border). Pediatric denture teeth (e.g., milk teeth, Nissin Dental Products, Japan, distributed in North America through Kilgore International, www.kilgoreinternational.com) are positioned on the trial base and an anterior setup evaluated chairside. Often, in a young child, the upper prosthesis can be made first, allowing a period of accommodation, followed by the lower prosthesis 6–12 months later. It is important to relieve the denture in areas where teeth are erupting, often creating holes in the denture to allow maximum tooth eruption. Recall that it is the eruption of the teeth that creates alveolar bone and is responsible for the development of approximately two thirds of the vertical height of the mid and lower face [19]. The parents/caregiver needs to plan on reline and/or remakes about every 2–3 years while the child is growing.
When the child has reached school age (7–12 years), it is important to transition the dentition from the primary to permanent state, allowing for eruption of what permanent teeth will form. Typically, patients will develop certain permanent teeth more often than others (e.g., central incisors, canines, and first molars). It is important to provide replacement teeth in this population to allow for phonetics, mastication, and social/peer awareness [17, 20, 21]. Typically a more removable approach is used in this population to allow for ongoing growth. This is also a time for orthodontic evaluation, especially as permanent teeth erupt and may need to be guided to proper position (Fig. 5.4). Retained primary teeth should be retained to preserve what alveolar bone has formed. Evaluation for ankylosed primary teeth needs to occur (especially in bounded spaces with permanent teeth on either side). In patients congenitally missing all of their mandibular teeth, consideration may be made for one or two oral implants in the anterior mandible [3]. This should be elected with caution with careful discussion as to why the patient (and not the caregiver) cannot adapt to the lower complete denture. The use of mini-implants (<2 mm diameter) is not commonly considered in this population.
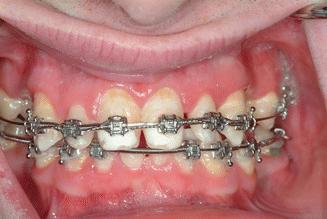

Fig. 5.4
Patient with Witkop’s syndrome (tooth and nail syndrome) during orthodontic treatment showing reposition of teeth into a proper position for long-term rehabilitation
In adolescents to young adults (13 years to maturity), this is an age range when orthodontic therapy should be considered. Comprehensive care in this population should be a team approach between pediatric dentistry, prosthodontics, and orthodontic colleagues. Orthodontic care may be conventional full-banded appliances or assisted with temporary anchoring devices (TADs or “temporary implants”) used to support the orthodontic care (Fig. 5.5). These are removed during or at the completion of the orthodontic phase of care. In cases of hypodontia (e.g., missing maxillary lateral incisors), esthetic tooth replacement can be performed either with a removable partial denture, an orthodontic retainer, or a unilateral bonded pontic (Fig. 5.6a–d). In the latter approach, the bonded pontic is typically made with a zirconia core that is either tribochemical silica-based silinated (e.g., Rocatec Bonding System, 3M ESPE, St. Paul, MN) or the TZP ZrO substructure is pressed with a hydrofluoric acid-etchable glass ceramic (e.g., e.max Press, Ivoclar Vivadent, Amherst, NY) and bonded to the mesial aspect of the canine with a veneer-based cement system (e.g., RelyX Veneer, 3M ESPE) [22]. An important goal for the transitional period is a stable, esthetic, and functional dentition without overtreatment or loss of retained primary teeth that are developing or maintaining alveolar bone. It is most important that the maximal potential of craniofacial growth be accomplished during this period.
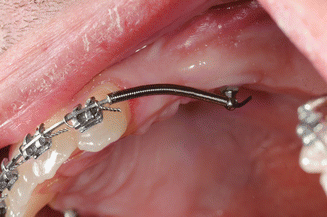
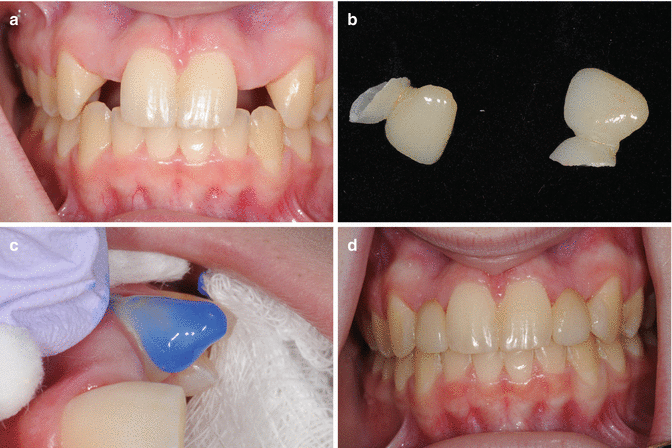

Fig. 5.5
In patients missing multiple teeth, temporary anchoring devices (TADs) which are really temporary non-integrating implants are often used during orthodontic therapy

Fig. 5.6
(a) A 14-year-old female during post-orthodontic retention phase of care with hypodontia (missing lateral incisors). (b) Missing lateral incisors are replaced with zirconia substructure and pressed lithium disilicate pontics adhesively bonded to the mesial aspect of the canines. Note the wrapping support created in the retainer design. (c) The retainer teeth are etched and prepared using a conventional veneer bonding system. (d) The patient at a 3-year recall with the lateral incisors restored with cantilever pontics bonded to the mesial aspect of the canines allowing ongoing growth of the premaxilla, natural individual tooth eruption, and anterior occlusal stability
If denture retention is insufficient, from the patient’s perceptive, oral implant therapy can be considered in the edentulous anterior mandible during this period. Although, it is best to plan for a definitive final prosthetic design in selecting the implant sites [18]. It is also preferable to avoid extensive bone grafting for site development in this age period.
Oral rehabilitation in the skeletally mature adult needs to be based on a comprehensive evaluation of systemic health and oral health risk factors with a strong weighting on patient-oriented outcomes, desires, and values. In this population, a multidisciplinary team is critical with additional orthodontic and oral surgical phases of care (e.g., Le Fort midface orthognathic procedures). The prosthetic outcomes need to be carefully planned by the prosthodontist and strategic decisions made as to retention of primary (or sometimes permanent) teeth, use of root canal therapy (RCT) and RPD overdentures for multiple missing contiguous teeth, and/or need for extensive bone grafting for a multiple oral implant rehabilitation (Fig. 5.7a–d). In any event, the patient needs to understand that any prosthodontic intervention will have significant maintenance issues and will probably need to be replaced multiple times in the patient’s lifetime [12]. The conical or malformed shape of the permanent teeth can be corrected with direct composite bonding or conservative bonded ceramic veneers (partial coverage onlays) based on light surface preparation of the teeth and careful orthodontic planning/spacing to allow optional positioning of the permanent conical-shaped crown in the middle of the planned ceramic veneers (e.g., e.max Press, Ivoclar Vivadent, Amherst, NY) (Fig. 5.8a–f). Oral implant therapy can be very helpful in this population given a proper diagnostic work-up and careful planning is performed. A systematic assessment of risk factors is essential (Table 5.1). Note in Table 5.1 the importance of mucosal tissue thickness and width and the need to use connective tissue grafting (alloplastic or autoplastic) to augment the mucosal tissues in the planned implant sites. In a retrospective survey of 98 patients affected with ED, treated with oral implants at the National Institutes of Health (NIH) in the 1980s, it was observed that a relatively high rate of implant maintenance complications occurred over time [17]. With 56 male and 46 female subjects having 73 % of the implants in the lower jaw, it was noted that 52 % of the implants had complications such as infections, lost implants, loose dentures, remakes/relines, and combinations of these complications. It is interesting to note that most of the subjects were happy with the outcomes regardless of the complications. In a study by Bergendal et al. [23], the authors reported on a retrospective study of Nordic regional treatment centers on ED-affected children treated with oral implants between 1985 and 2005 [23]. Twenty-one children, treated with 33 implants due to agenesis or trauma, with a subgroup of ED-affected children (5 treated with 14 implants) at 5–12 years of age were reported. The authors reported that 9 of the 14 implants were lost prior to loading in the ED cohort, warranting caution with the approach and implant system being used at that time [23]. In the Netherlands, a retrospective study following 129 subjects in the Dutch health-care system having tooth agenesis (mostly hypodontia) noted over an observation period of 3–79 months (mean of 46 months in function) that 36 % of subjects had severe orthodontic root resorption, 12 % had significant bone loss (>5 mm), and 57 % had mucosal discoloration around the implant abutments [24]. In our Craniofacial Clinical Research Center at the University of Iowa, we have longitudinally followed 46 subjects with HED or Witkop’s syndrome (tooth and nail ectodermal dysplasias). In this population with at least 3–28 years of follow-up, we have 32 subjects treated with corticocancellous hip grafts restored with 231 oral implants (3 different systems, 4 turned surface, 227 moderately rough acid-etched or TiO-blasted surfaces) with fixed or removable options. 80 % were treated with a conventional two-stage healing approach. In this cohort, we have one lost implant at 6 weeks following placement (implant with moderately rough surface, anterior mandible in dense type I bone). We have noticed that 78 % of the hip grafted sites over time develop the same mucosal discoloration reported by the Dutch group, emphasizing that autogenous grafting is useful but not stable and long term and that mucosal thickness augmentation procedures (e.g., connective tissue grafting, use of mucosal thickening agents such as AlloDerm (BioHorizons, Birmingham, AL) or PerioDerm (Symbios, DENTSPLY Implants, Waltham, MA) and dermal matrices) should be considered (Fig. 5.9).
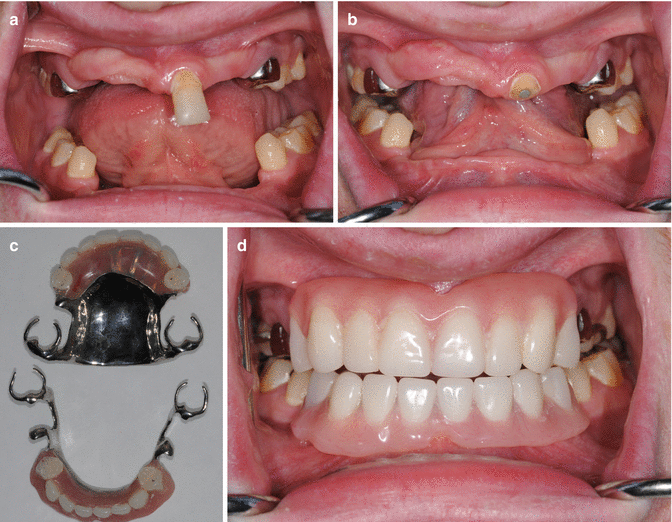
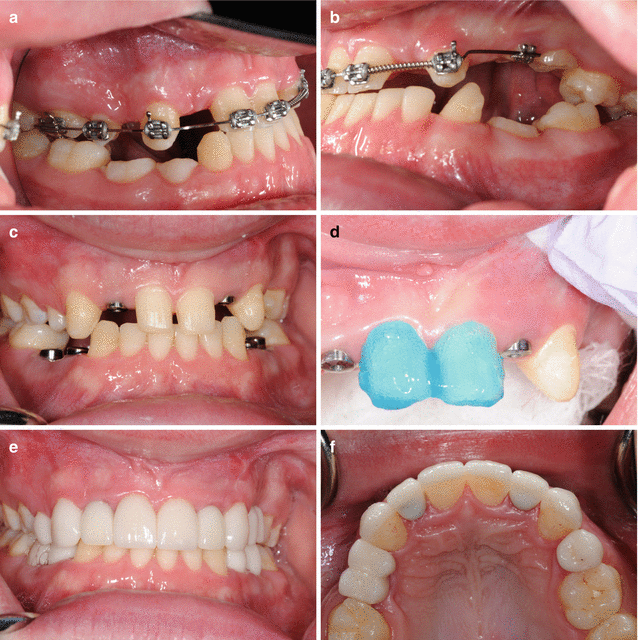

Fig. 5.7
(a) A 20-year-old male with HED presents with multiple missing teeth, supraerupted central incisor, ridge aplasia, and retained primary molars restored with stainless steel crowns. Care plan included root canal therapy on the central and conversation to an overdenture abutment under an RPD. (b) Patient following RCT and central incisor converted to an overdenture abutment. (c) Conventional upper and lower cast partial dentures. The use of RPD is a less expensive approach and rapidly restores the multiple missing teeth for this patient. (d) The patient was restored with the upper RPD overdenture and lower RPD. Excellent oral hygiene is very important with this approach due to the high caries risk in the HED population along with the plaque retention that occurs with these types of prosthesis

Fig. 5.8
(a) A 20-year-old male with Witkop’s syndrome presents with retained primary teeth, ankylosed primary teeth, and class III malocclusion with a dental compensation necessitating an orthodontic and orthognathic midface Le Fort I procedure to correct midface asymmetry. (b) Patient’s occlusion and oligodontia demonstrating both the supraeruption of the lower canine, the distal inclination of the lower incisors, and ankylosed primary teeth (being used for orthodontic anchorage in the maxilla). (c) Anterior view of patient’s occlusion. Orthodontic positioning of the teeth has set up for ceramic veneers on the remaining permanent teeth. Patient had a Le Fort I midface advancement followed by implant placement. (d) Teeth were prepared for the veneers using a conventional three-step adhesive bonding systems. (e) Anterior view following restoration (BL3 shade, e.max lithium disilicate, Ivoclar Vivadent, Amherst, NY). (f) Occlusal view demonstrating veneers on the canines and central incisors (1 mm flat reduction, light facial and cervical preparation). Maxillary right microdontic first premolar was restored with a ceramic onlay to restore normal contours. Maxillary left premolars restored with one implant and a molar-sized crown shaped as two premolars when viewed from the buccal corridor. Maxillary lateral incisors were restored with implants (3.5 mm ASTRA TECH-TX Implant System, DENTSPLY Implants, Waltham, MA) using CAD/CAM abutment and individual crowns (Gold Hue, Atlantis DENTSPLY Implants, Waltham, MA)
Table 5.1
Guidelines for the evaluation of implant-related risk factors and elements of informed consent
|
Guideline
|
Issue
|
Management
|
|
|---|---|---|---|
|
1
|
Three-dimensional mucosal biotype?
|
Thin biotypes (<2 mm thick) are associated with recession and implant bone loss and compromised esthetics. Evaluate for thin bone all around the planned implant site
|
Consider connective tissue grafting, and consider the thickness of the facial plate of the bone. Plan for at least 1–1.5 mm of bone all around the planned implant. If not, plan for site preservation or development grafting procedures. Use CBCT approaches to evaluate implant sites
|
|
2
|
Symmetry of the smile?
|
Asymmetry between the anterior and posterior occlusal planes relative to the lips and smile upon activation of the muscles of mastication
|
Evaluate the posterior occlusal plane relative to the commissures of the lips; evaluate the degree of and asymmetry of the buccal corridor side to side
|
|
3
|
Anterior incisal plane?
|
Asymmetry in the canine to canine tooth size, arch length discrepancy?
|
Orthodontic balancing of the anterior incisal edges (prefer lateral incisors to be offset from the central incisor)
|
|
Danger or ongoing passive eruption leading to changes in the incisal edges of the anterior incisal plane
|
Orthodontic positioning with tight lingual coupling of the maxillary cingulum with the incisal edge of the opposing mandibular incisors. If this cannot be obtained, consider composite resin cingulum stops to prevent nonuniform passive eruption
|
||
|
Mandibular incisor supraeruption? Anterior natural tooth vertical and horizontal overlap (overjet and overbite)
|
May need to consider intrusion or extraction of the opposing teeth if function is compromised in the care plan development
|
||
|
4
|
Tooth to tooth proportions?
|
Balance of tooth proportions in the anterior incisal plane
|
Based on central incisor proportions (e.g., 70–75 % of the width relative to the inciso-gingival dimension), if lateral is 2/3 mesial-distal dimension or less, consider cantilever lateral incisor pontics
|
|
5
|
Tooth to tooth relationships?
|
Asymmetry in canine, lateral and central incisor positions creating nonuniform diastemas
|
Orthodontic management to allow either reshaping, bonding, or ceramic veneers
|
|
6
|
Gingival position of interproximal contact points?
|
Asymmetry can lead to interproximal recession or gingival CEJ symmetry issues
|
Evaluate in provisional restorations, determine if apical position of interproximal contact points needs to be moved more apical
|
|
7
|
Type of defect?
|
Evaluate the degree of hard and mucosal augmentation that will be needed and the impact on timing of the procedures
|
Consult patient about timing of procedures relative to major life events, plan for interim restorations needed during healing and for tissue sculpting
|
|
8
|
History of recession?
|
Evaluate other sites in the oral cavity for signs of recession
|
Carefully evaluate especially in post-orthodontic situation, consider augmentation procedures
|
|
9
|
History of defect?
|
Degree of bone and mucosal defect
|
In sites with congenitally missing teeth, consider orthodontic augmentation approaches and/or staged surgical procedures
|
|
10
|
Mucosal health?
|
Mucosal inflammation, especially with interim restorations, complicates final esthetics
|
Mucosal tissues need to be in optimal health; consider orthodontic extrusion if necessary (esp. in cases of external root resorption)
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses