Periodontal and restorative dentistry are mutually important facets of clinical dentistry. Today’s clinicians have many treatment options at their disposal, including biotolerant restorative materials and implants, to maintain periodontal health. It is crucial for the clinician to understand the biologic principles that form the foundation for restorative reconstruction of the periodontally involved tooth. This article discusses new techniques and trends in the critical management of the restorations, particularly at the gingival margins, and explores the role of implant dentistry as an option for the restorative plan of the periodontal patient.
Periodontal and restorative dentistry are mutually important facets of clinical dentistry. Spear and Cooney well describe the intimate relationship of these facets by stating that, “…for restorations to survive long term, the periodontium must remain healthy…for the periodontium to remain healthy, restorations must be critically managed …so that they are in harmony with their surrounding periodontal tissues.” This article discusses new techniques and trends that mostly involve this second aspect, which is the critical management of the restorations, particularly at the gingival margins. The role of implant dentistry as an option for the restorative plan of the periodontal patient is explored ( Figs. 1 and 2 ).
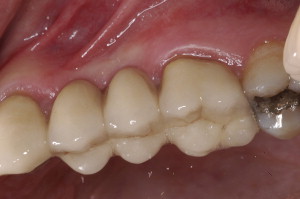
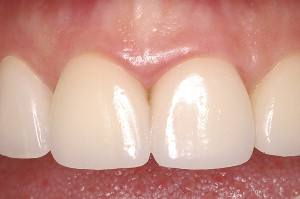
For proper understanding of the complex relationship that exists between restorative dentistry and periodontal health, two important interrelationships are addressed: (1) the placement of the margins of a restoration and their relationship to biologic width and (2) the type of dental materials used to make the restoration.
Before describing the different possibilities available to the restorative dentist, it is essential to review important features of the anatomic structures that are naturally present where the tooth enters the alveolus, the so-called biologic width. Historically, Gargiulo and colleagues described this zone as the tissues that constitute the structures above the bone crest, terminating with the free gingival margin. They promulgated a rule of thumb for the clinician to follow: the tissues above the alveolar crest fill a space composed of gingival fibers, connective tissue, and junctional epithelium that measure approximately 2 mm. Whereas this value is applicable to most clinical cases, the observations that suggested this rule were derived from the study of cadaver specimens. More recently, Vacek and colleagues published a histomorphometric study that examined 171 tooth surfaces from 10 human adult cadaver jaws. This study supported the data from Gargiulo and colleagues; however, it brought attention to the fact that several variations in dimension between subjects are possible. These investigators presented data showing large variations between subjects and, even, within the same person, with some individuals having an average biologic width of 0.75 mm and others of 4.3 mm. These variations were seen mostly within the epithelial attachment, with the connective tissue attachment having the least variability. These findings were also suggested by Gargiulo and colleagues. Thus, it should be concluded that changes within the biologic width depend on the location of the tooth in the dental arch and on the individual subject. Ultimately, the 2.00 mm rule of thumb should be used with caution and interpreted on a case-by-case, tooth-by-tooth basis.
The 2.00 mm of biologic width rule has particularly influenced surgical crown lengthening procedures. The study by Landing and colleagues examined the dimensions of the biologic width before and 3 and 6 months following surgical crown lengthening. Prosthetic treatment started 6 weeks after surgery. The presurgical values of biologic width were found to be reestablished 6 months after completion of the surgical procedures.
To maintain periodontal health, placing the margin of a restoration in the gingival area of the tooth is of critical importance, and violating the biologic width may lead to problems. When correlating biologic width to periodontal health and restorative margins, de Waal and Castellucci suggested that the margin of the final prosthesis should be placed 1 to 2 mm supragingivally wherever possible. If required for aesthetic considerations, the margin can be placed at the gingival crest or, at most, 0.25 mm to 0.5 mm into the gingival sulcus. This ensures that the biologic width remains healthy. Therefore, locating the margins of a restoration too close to the bone may cause periodontal destruction, most likely by preventing thorough plaque removal by routine oral hygiene procedures.
When the biologic width is violated, Maynard and Wilson showed that an inflammatory response results in alveolar bone resorption. Furthermore, this circumstance creates a vicious circle, which leads to increased pocket depths, increased loss of periodontal support, exacerbation of accumulation of subgingival bacteria, increased chronic inflammation, and further localized periodontal breakdown.
To allow the patient the ability to maintain periodontal health, consideration should also be given to the type of crown contour that is used when fabricating the restoration. Becker and Kaldahl reported that the crown contours, together with margin placement and pontic design, affect periodontal health. They suggest that the crown contour should facilitate home-care oral hygiene maneuvers, and caution that over-contoured crowns lead to increased periodontal inflammation. Their study summarizes four critical points that should be taken into account when creating crown contours: (1) buccal and lingual contours should be “flat, not fat”; (2) embrasures should be kept open; (3) the location of contact areas should be oriented toward the incisal and the buccal aspects of the restored tooth; and (4) the crown margins over furcation areas in molars and premolars should be fluted or barreled out.
Restoring molars with periodontal furcation involvement is important when attempting to preserve teeth with compromised prognosis. A recent study by Zafiropoulos and colleagues evaluated the long-term outcome of hemisected mandibular molars versus teeth replaced with implants. In a group of 32 patients, 56 hemisections were performed and compared with a group of 28 patients that received 36 implants that replaced mandibular molars. All patients were categorized as having a history of chronic periodontitis, with a minimum of four sites showing attachment loss of greater than 4.00 mm, bleeding on probing of at least four sites, and radiographic evidence of bone loss. The results reported that in periodontitis patients, hemisected molars were more susceptible to complications than implants, with 32% of the hemisected teeth having some level of complications versus 11% in the implant cases.
Park and colleagues reported similar findings, with 691 hemisected molars in 579 patients showing a 30% failure rate over 10 years. Periodontal complications, tooth fractures, endodontic problems, and dental caries were factors contributing to the failures. It is thus conceivable that implants are more predictable to restore and maintain masticatory function in periodontal patients than is retention of selected compromised natural teeth.
In this regard, despite the long-term success rate of implant therapy, periodontal patients are still most often treated with conventional restorative dentistry. In the past 20 years, the dental industry has allowed the dentist to use more aesthetically pleasing materials for crown fabrication, and these new materials have demonstrated excellent results with respect to periodontal tissue tolerance. The study of Goodson and colleagues conducted on nine subjects who received 42 restorations with margins made of composite gold alloys is instructive in this regard. Microbiological sampling of the crown margins were compared with samples from contralateral normal teeth. The data showed that the margins restored with porcelain/composite gold alloy had significantly fewer bacteria than contralateral normal teeth. Patients in this study were periodontally healthy. Subsequently, in 2002, a study by Gemalnaz and Ergin was conducted on 37 all-ceramic crowns placed in 20 patients. Among other restorative parameters, plaque and gingival scores were also assessed for a period averaging 25 months after cementation. Incisors, premolars, and molars were included in this study. The all-ceramic crowns showed significantly less plaque growth than did natural teeth. Differences in favor of the artificial crowns were also reported when assessing gingival inflammation. When location of margins was considered, subgingival margins were more prone to have bleeding on probing than were supragingival margins. The study by Felton and colleagues of 29 patients indicated that marginal discrepancies were associated with gingival inflammation. An accurate impression technique is always required to reduce subgingival microgaps between the restorative margins and the tooth preparation margins and, therefore, minimize plaque formation.
Summary
Periodontal health and restorative dentistry are inextricably linked. Today’s clinicians have many treatment options at their disposal, including biotolerant restorative materials and implants, to maintain periodontal health. Nevertheless, it is crucial for the clinician to understand the biologic principles that form the foundation for restorative reconstruction of the periodontally involved tooth.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


