Fig. 5.1
Vascular pedicle
5.1.3 Indications
The temporalis myofascial flap can be used in whole or in part depending on the area and volume of the defect and on the functional requirements of the reconstruction to be used for facial paralysis.
Given its anatomical proximity and considerable versatility, the temporalis myofascial flap is very useful for treating defects of the oral cavity [6]. Disinsertion of the muscle and rotation medially toward the zygomatic arch enable reconstruction to be performed from the maxillary midline in patients whose health status or older age contraindicates microsurgery with bone tissue. The temporalis myofascial flap is very useful for reducing the dead space remaining after orbital exenteration. It provides volume and reduces the risk of cerebrospinal fluid leak [7]. These are our preferred indications for this flap.
The temporalis myofascial flap can also be useful for the reconstruction of other defects of the middle third such as the malar region, orbital border, and oroantral fistulas.
The temporalis myofascial flap plays an important role in patients with facial paralysis for whom a microvascular muscle flap cannot be used. It enables traction of the oral commissure in order to create a smile despite the lesion of the buccal branch of the facial nerve. It is also possible to pull the frontal region upward, thus enabling the patient to raise the eyebrows and correcting the defect resulting from lesion of the frontal branch of the facial nerve [8]. Innervation of the temporalis muscle by the trigeminal nerve has the drawback that for the dynamic outcome to be aesthetically pleasing and symmetrical, the patient must undergo rehabilitation and a learning process, since the facial nerve is responsible for mobilizing the muscles of facial expression on the healthy side. The trigeminal nerve is sensory and supplies the muscles of mastication but not those of facial expression (Fig. 5.2).
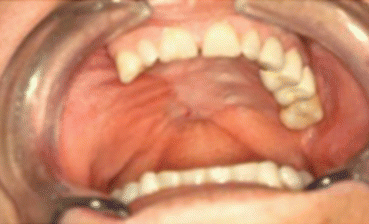

Fig. 5.2
Reconstruction of the right palate with temporalis muscle flap
5.1.4 Complications
The temporalis muscle flap is very predictable, with the result that associated complications are very uncommon. Potential complications include hemorrhage, hematoma, and seroma. In dentulous patients, every effort must be made to ensure that the flap does not interfere with occlusion in order to prevent vascular complications arising from involuntary mechanical pressure on the part of the patient.
Clinical follow-up requires physical examination of the flap, since it may be affected by partial or complete necrosis, although this is uncommon. The veins are more commonly compromised than the arteries. Care must be taken when turning the flap to prevent the pedicle from twisting and when sliding it medially toward the zygomatic arch for reconstruction of intraoral defects. If the flap is compromised, the arch should be cut and repositioned with plates and screws once the maneuver has been completed.
Knowledge of the anatomy of the facial nerve is essential during shaping of these flaps, since there is a risk of damaging the facial nerve, especially the frontal branch.
A drawback of the temporalis myofascial flap is the cosmetic defect in the temporal fossa. Throughout history, various materials have been used to avoid the unsightly defect resulting from the loss of tissue in the temporal region. The materials used include autologous bone grafts, bone cement (methyl methacrylate, hydroxyapatite), porous high-density polyethylene prostheses [9, 10], preformed acrylic prostheses, and titanium mesh [11]. All of these materials are susceptible to infection and exposure.
5.2 Pectoralis Myocutaneous Flap
5.2.1 Introduction
The pectoralis myocutaneous flap was first used in 1979 by Ariyan to transplant pedunculated tissue for reconstruction of head and neck defects [12]. Later, in 1980, Cuono and Ariyan reported on the inclusion of the fifth rib in the pectoralis osteomyocutaneous flap for reconstruction of composite defects [13].
5.2.2 Vascularization
The pectoralis major has two distinct vascular territories. The more cranial region is supplied by the pectoral branch of the thoracoacromial artery and the muscular branches of the first, second, and third perforating branches of the intercostal arteries and branches of the internal thoracic artery [14]. The more caudal region of the pectoralis muscle is supplied by the fourth, fifth, and sixth perforating branches of the internal thoracic artery [15].
Venous drainage of the pectoralis major is by venae comitantes that follow the course of the arteries of the same name (see above) before emptying into the axillary vein [16].
5.2.3 Indications
Since the end of the twentieth century, the pectoralis flap has been used to resolve major tissue defects of the head and neck. With the advent of new microsurgical reconstruction techniques, we can now provide the quantity and type of tissue necessary with better functional and cosmetic outcome [17]. Therefore, this flap has been relegated to the role of “rescue” flap, for use in patients with defects of the middle third or intraoral and cervical defects in which microvascular free flaps and pharyngeal-laryngeal reconstructive surgery are not used [18]. It can prove useful for the reconstruction of total glossectomy in patients who are not candidates for microsurgical free flaps such as the rectus abdominis flap or anterolateral thigh flap.
Within the oral cavity, it is possible to reconstruct both cranial and ipsilateral soft palate defects. Outside the oral cavity, it is possible to cover skin and soft tissue defects in the orbitozygomatic region [19]. The flap can be used with the muscle pedicle external to the skin of the neck in patients with associated comorbidities. If no complications have arisen 3 weeks after surgery, the flap pedicle can be cut in order to improve the appearance of the face and facilitate the patient’s return to a normal social life (Figs. 5.3, 5.4, 5.5, 5.6, and 5.7).
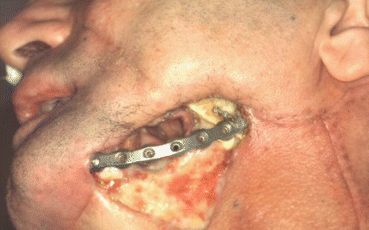
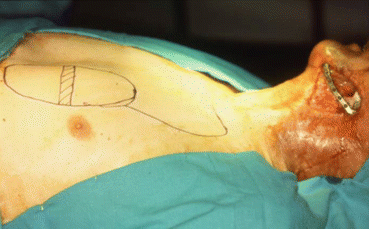
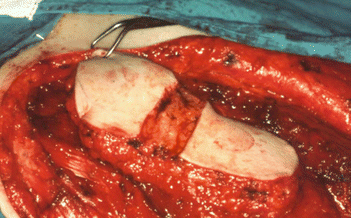
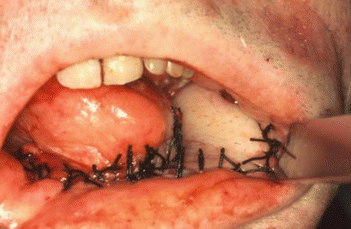
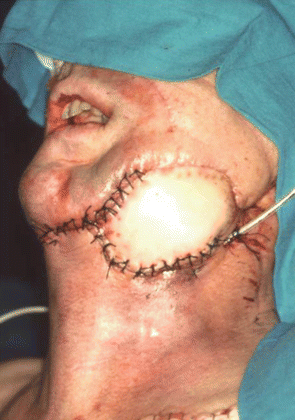

Fig. 5.3
Preoperative defect

Fig. 5.4
Pectoralis muscle flap design

Fig. 5.5
Pectoralis muscle flap with de-epithelialized area

Fig. 5.6
Intraoral reconstruction

Fig. 5.7
External reconstruction
5.2.4 Complications
The pectoralis flap carries a high risk of partial necrosis of the skin paddle and of the underlying muscle, as well as of orocutaneous and pharyngocutaneous fistula. Total necrosis of the flap is unusual, although areas of peripheral epidermolysis are common.
The flap carries a high risk of wound dehiscence, especially in women and in patients aged over 60 years because of the force of gravity and the increase in fatty tissue. If there is a communication with the oral cavity, the risk of infection along the subcutaneous course of the flap increases considerably [17].
5.3 Latissimus Dorsi Myocutaneous Flap
5.3.1 Introduction
The latissimus dorsi myocutaneous flap was used for the first time in head and neck reconstruction by Quillen in 1978 [20], although it has been used in breast reconstruction since the beginning of the twentieth century.
The flap can be free or pedicled. Its almost constant anatomy and the wide caliber of the vessels of the pedicle make it a predictable option for reconstruction. It can be harvested as a muscle flap, musculocutaneous flap, or osteomyocutaneous flap. It contributes a large area of vascularized tissue and volume. The muscle commonly atrophies, although occasionally it will be necessary to use secondary thinning procedures and contour correction [21].
The skin island can be designed in different directions depending on which best suits the reconstruction. Moreover, the scarce variability of the regional and vascular anatomy means that the subscapular system can be used to obtain many free or pedicle flaps for the reconstruction of complex soft tissue and bone defects (Fig. 5.8).
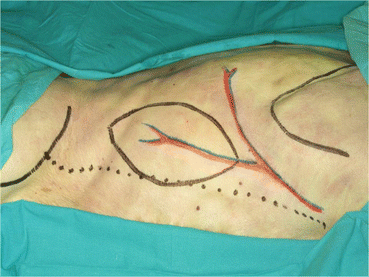

Fig. 5.8
Surgical design
5.3.2 Vascularization
The main flap is formed cranially by the thoracodorsal vein and artery and medially by the circumflex scapular artery in the mid part. Both are branches of the subscapular artery. Additionally, the latissimus dorsi is supplied by the posterior intercostal perforators and perforating branches of the subscapular artery [22]. The most caudal part of the muscle is supplied by branches of the lumbar arteries.
The veins of the scapular system accompany each artery in groups of 2, except in the section of the thoracodorsal artery, where venous return is through a single thoracodorsal vein.
5.3.3 Indications
Given that the latissimus dorsi flap is a pedicle flap, it can be used to cover soft tissue defects in the cervical region. It can also be used to cover defects of the temporal and occipital scalp. This flap can also prove suitable for the reconstruction of tissue defects in the oral cavity, including glossectomy [23, 24], although this is not its most frequent use. Given advances in microsurgical techniques, the latissimus dorsi flap is now reserved for medically compromised patients who are to undergo reconstruction with a free flap, patients who require large reconstructions, and patients without cervical vessels for microsuture [24].
Today, the latissimus dorsi myocutaneous flap is the first choice for many surgeons in scalp reconstruction because it is reliable and easy to harvest and has a large surface area [25]. Very often, because of problems with the length between the pedicle and the area to be reconstructed, a free latissimus dorsi flap with microsurgery techniques is preferred [26]. Thus, distance is no longer a disadvantage, and the risk of wound dehiscence from accidental traction of the pedicle with neck movements is reduced (Figs. 5.9, 5.10, and 5.11).
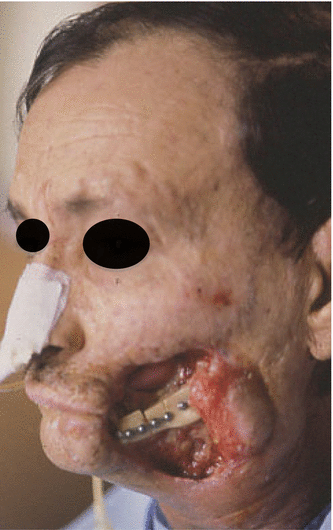
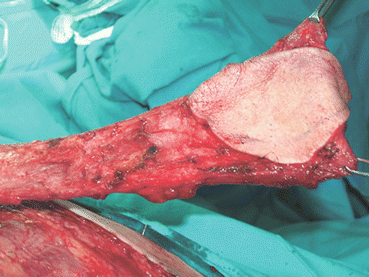
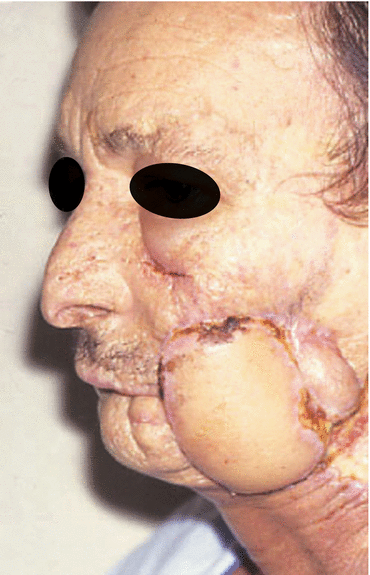

Fig. 5.9
Preoperative defect

Fig. 5.10
Isolated flap

Fig. 5.11
Postoperative view
5.3.4 Complications
As with any flap, the latissimus dorsi myocutaneous flap carries a risk of vascular compromise, either by arterial ischemia or, more frequently, venous damage. Given the wide caliber of the vessels of this flap, these complications are not frequent. The most caudal part of the muscle, which in scalp reconstruction is the most cranial, carries a greater risk of necrosis because the vascularization of the lower third is from the lumbar arteries, which are cut to rotate the flap.
As this is a bulky flap whose pedicle ascends from the donor site to the recipient site on the head or neck, a certain risk of wound dehiscence is expected. Other risks include infection both of the donor site and of the recipient site—especially if the oral cavity is the area to be repaired—and fistula in cases of communication with the oral cavity, parafacial sinuses, or cerebrospinal fluid [27]. In such cases, the borders of the flap and the neighboring tissue should be completely sealed. Seromas and hematomas can form [28].
Loss of function is not normally severe, although this may be the case for patients who use crutches to walk or need a wheelchair and for professionals such as gardeners or sportspeople such as golfers. If there are no contraindications, early rehabilitation of the shoulder should be undertaken within the first week of the intervention. If the shoulder is immobilized for longer periods, the patient tends to adopt antalgic postures that considerably delay normal functioning of the shoulder [29].
5.4 Sternocleidomastoid Myocutaneous Flap
5.4.1 Introduction
The sternocleidomastoid myocutaneous flap was first described by Owens in 1955 [30]. Since then, the use of this flap has been considered controversial, and it has been relegated to adjuvant procedures with limited indications. It can be used as a myocutaneous flap and as an osteomyocutaneous flap if clavicle bone tissue is included.
5.4.2 Vascularization
The main blood supply is from a branch of the superior thyroid artery. However, the occipital artery is largely responsible for the supply of the cranial third of the muscle. In addition, the middle third sometimes receives direct branches from the external carotid artery. The caudal third can receive its supply from the suprascapular artery, cervical transverse artery, the thyrocervical trunk, and the superficial cervical artery [31]. The skin paddle is vascularized by myocutaneous perforators (veins and arteries) [32]. Given that venous return runs parallel to arterial return, the flap can be used cranially or caudally as a pedicle flap.
5.4.3 Indications
Since it was first described, the sternocleidomastoid flap has been heavily criticized because of the safety risk in tumors of the head and neck: the course of the muscle is close to the cervical lymph node chains II, III, IV, and V. Furthermore, partial necrosis of the raised skin paddle is common, affecting 20–52 % of all flaps harvested [33].
This flap is has been used mainly as a partial muscle flap after parotidectomy. It is placed between the skin and the branches of the facial nerve, thus reducing the risk of Frey syndrome [34–36] and the resulting cosmetic defect [35], although the superficial muscular aponeurotic system flap is now more generally used. The sternocleidomastoid flap can also provide bulk and improve contour after a resection. Its volume can be increased by rotation.
The flap can be used for the reconstruction of the floor of the mouth and the tongue, as well as for intraoral, cervical, and facial structures caudal to the zygomatic arch [37]. Greater knowledge of the vascular anatomy of this muscle has made it possible to improve the harvesting technique, thus enabling the flap to be converted to a pedicle perforator flap and improving the arc of rotation of the pedicle. Consequently, as we can be more selective with the quantity of tissue to be transferred, the survival rate of the skin paddle is increased [38].
We use the sternocleidomastoid flap very occasionally to increase facial volume in 3-dimensional reconstructions. Although this is not the flap of choice for mandibular reconstruction, an osteomyocutaneous flap can be harvested based on the insertion in the clavicle. Thus, a longitudinal section of the clavicle can be made, and dental implants can be placed either immediately or at a later date [39]. Given the morbidity associated with resection of the clavicle, we have never used the sternocleidomastoid flap in this way (Figs. 5.12, 5.13, 5.14, and 5.15).
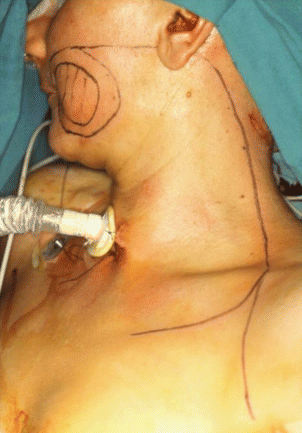
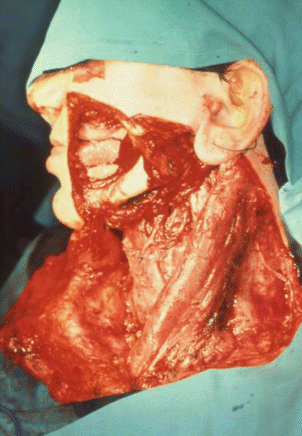
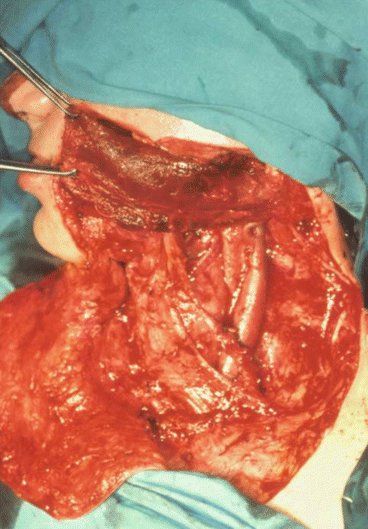
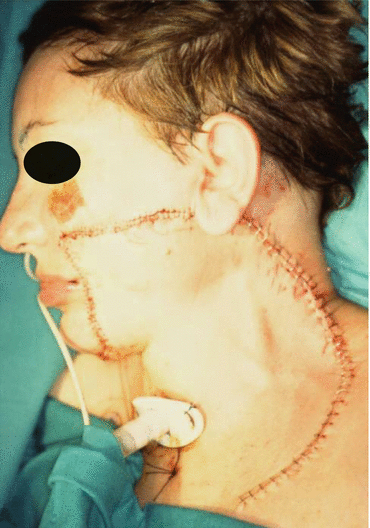

Fig. 5.12
Surgical design

Fig. 5.13
Surgical defect

Fig. 5.14
Sternocleidomastoid muscle providing bulk to the face

Fig. 5.15
Immediate postoperative aspect
5.4.4 Complications
Before harvesting this flap, it is necessary to locate the spinal accessory nerve, which must be spared. Injury of the spinal accessory nerve can affect trapezius muscle function, and problems with rotation, elevation, and adduction of the arm have been reported, as have atrophy and pain in the arm [40].
As with any other flap, the sternocleidomastoid flap can be affected by total or partial necrosis. Total necrosis is uncommon, except in patients who receive radiation therapy as a complementary treatment. Partial necrosis of the skin paddle is quite common. As mentioned above, this complication can be reduced if the flap is harvested as a perforator flap [41].
In the case of intraoral reconstruction, there is a risk of orocutaneous fistula and wound dehiscence, although this risk can be reduced by suturing the flap on several planes. In addition, it is recommended to attach the flap to the bone using a suspension suture and insist on postural measures during the first week after surgery.
5.5 Cervicopectoral Skin Flap
5.5.1 Introduction
The cervicopectoral flap was first described by Becker in 1978 for the reconstruction of head and neck defects [42]. It is well vascularized and has a large skin surface. In addition, its color, texture, and thickness and the disposition of the adnexa are very similar to those of the surrounding tissue. The cosmetic outcome is excellent [43].
5.5.2 Vascularization
One of the advantages of this flap is that it uses the local blood supply from various arterial-venous perforators; consequently, the risk of complete necrosis of the flap is very low [44].
The upper third, from the ala to the chin, is supplied by perforating branches of the facial artery. The perforators of the superior thyroid artery supply the middle part of the flap (cervical region). The vascular network formed by the cervical transverse artery supplies the caudal part of the flap, which includes the neck and chest [45]. The flap is also supplied by blood from the anterior thoracic vessels of the internal mammary artery [46].
5.5.3 Indications
The cervicopectoral flap is the first choice for skin defects that do not require tissue bulk. Although a cervicofacial flap may be sufficient for malar lesions, the cervicopectoral flap is better for more extensive or cranial lesions, since it can completely cover the wound remaining after extirpation of the lesions in the orbit, malar region, parotid region, masseteric region, and chin, as well as in simple reconstruction of the lip [47]. The incision used for this flap can also be used to perform an ipsilateral cervical dissection, thus saving time, reducing morbidity, and providing a more extensive surgical field. In addition, the surgical plane of this flap coincides with that of the flap taken for parotidectomy and cervical dissection [46]. The flap is simple and easy to harvest.
If additional volume is necessary, the cervicopectoral flap can be combined with free muscle flaps, such as the rectus abdominis, or pedicle flaps, such as the pectoral flap, which can then be covered with the cervicopectoral flap. This approach provides volume and is cosmetically acceptable after large resections. The combination is very commonly used in orbital exenteration, where a temporal myofascial flap can be combined with the cervicofacial flap [48]. Its greatest advantage is that it provides an extensive area of skin whose color and texture are similar to those of the face, thus leading to a very acceptable cosmetic outcome (Figs. 5.16, 5.17, 5.18, 5.19, 5.20, and 5.21).
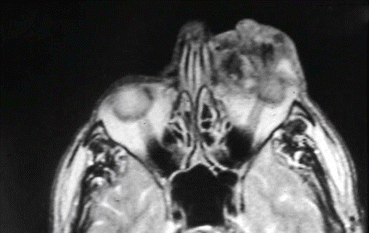
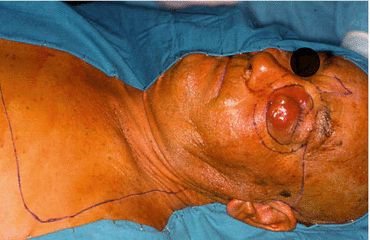
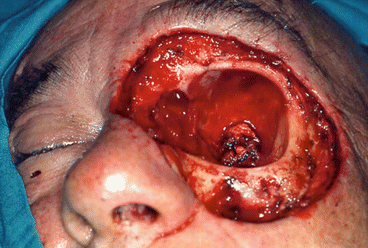
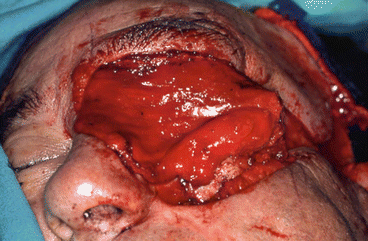
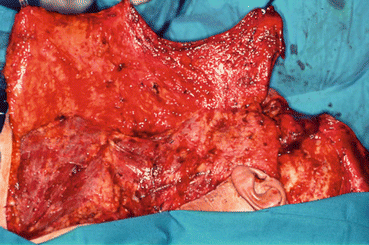
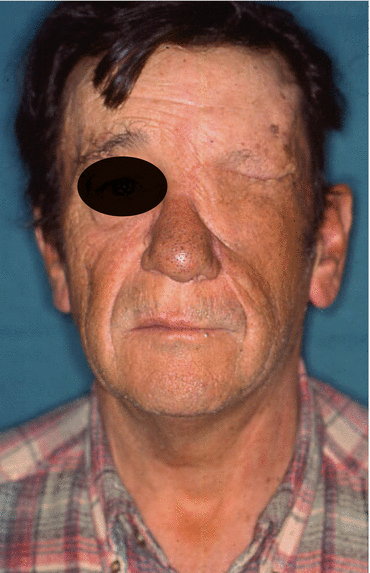

Fig. 5.16
MRI of the tumor

Fig. 5.17
Cervicopectoral design

Fig. 5.18
Surgical defect

Fig. 5.19
Temporalis muscle flap filling the orbit

Fig. 5.20
Elevation of the flap

Fig. 5.21
Final result
5.5.4 Complications
The cervicopectoral flap is frequently affected by superficial epidermolysis [47], although complete necrosis is extremely rare. Scars at the donor site, very old age, and heavy smoking constitute relative contraindications for this flap, since all these factors increase the risk of vascular complications. In the case of epidermolysis, the most likely outcome is that the tissue will scar after second intention healing. Given that the donor site is extensive, there is a risk of hemorrhage, hematoma, and infection.
5.6 Nasolabial Flap
5.6.1 Introduction
The nasolabial flap is a small and predictable flap that is easy to harvest [49]. It can be used for the reconstruction of small defects of the oral cavity, tongue, malar region, commissures, tip of the nose, ala, and lower eyelid [50]. It can be pedicled caudally or cranially and can be used bilaterally depending on the area of tissue to be repaired [51].
5.6.2 Vascularization
The flap is supplied by the angular artery, the infraorbital artery, and the transverse facial artery. This complete supply means that the flap can be obtained as a random or axial flap.
Depending on where the tissue from the nasolabial region is to be placed, the flap can be pedicled to the different vessels that supply it. Thus, the flap can be pedicled superiorly, with the blood supply based on the infraorbital artery, and inferiorly from the angular artery. Lastly, it can be pedicled both medially and laterally after the transverse facial artery [52].
5.6.3 Indications
The nasolabial flap is indicated for small soft tissue defects. If the flap is near the midline, two flaps can be obtained, thus enabling closure of larger midline defects [51]. Its main indication is for defects of the floor of the mouth.
The flap is easy to harvest and leaves a very discreet cosmetic defect, since the scar is camouflaged by the nasolabial groove. It is very useful for the reconstruction of intraoral soft tissue and even the tongue. In men, intraoral reconstruction has the drawback that the flap transports hair. Once the flap has settled, laser technology can be used to prevent hair growth.
In combined defects (bone and soft tissue), the nasolabial flap can be used to cover the bone flap. For example, in defects of the symphysis, bone tissue can be reconstructed using a microvascular iliac crest flap, teeth can be reconstructed with immediate placement of implants on an implant-supported prosthesis, and soft tissue can be reconstructed with a bilateral nasolabial flap [53], thus obviating dissection of the inferior oblique muscle with the iliac crest and reducing the comorbidity of the procedure.
Given its anatomical proximity and versatility, which provide multiple options for blood supply, and color similar to that of the nose [54], the nasolabial flap enables different combinations for repair of soft tissue [55, 56]. In combination with other flaps, it serves as a therapeutic tool for the reconstruction of the lips and perioral tissue [57] (Figs. 5.22, 5.23, 5.24, and 5.25).
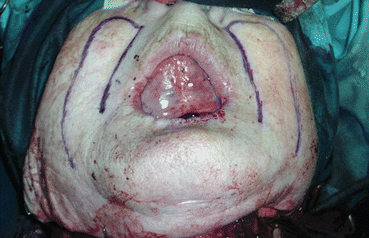
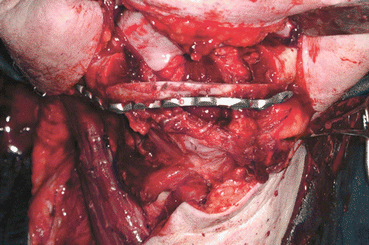
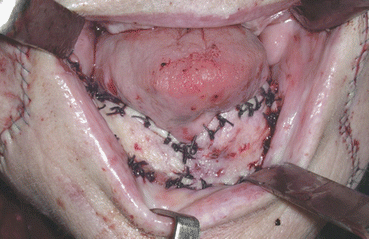
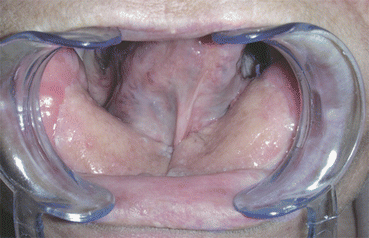

Fig. 5.22
Nasolabial flap design

Fig. 5.23
Surgical defect

Fig. 5.24
Intraoperative view

Fig. 5.25
6 months postoperative
5.6.4 Complications
Detractors of this flap highlight the disadvantage that it leaves a scar on the face. In fact, in patients with no history of hypertrophic or keloid scarring, the scar is barely visible, since it is camouflaged by the nasolabial groove. The cosmetic outcome is satisfactory or very satisfactory for most patients [58].
The risk of wound dehiscence is greater if the flap is used for reconstruction of mobile and intraoral soft tissue, as in the case of tongue reconstruction. Infection of the donor site is rare, since the area exposed during harvesting is small and highly vascularized [49]. Superficial epidermolysis is possible, as are partial necrosis and total necrosis, although the latter is uncommon.
If the flap is used for reconstruction of the infraorbital area, a safety margin of 7 mm from the medial canthus should be left in order to reduce the risk of ectropion [59].
5.7 Buccinator Flap
5.7.1 Introduction
The buccinator flap was first described by Reychler [60] as a myomucosal island flap. It has excellent texture, color, and pliability for reconstruction of intraoral soft tissue defects that are small in area and thickness. Closure of the donor site may be direct and not require an extraoral incision. The flap can be harvested as a mucosal, muscular, or myomucosal flap.
5.7.2 Vascularization
The buccinator muscle is supplied by branches of the facial, internal maxillary, and infraorbital arteries.
The facial artery is the main vessel supplying the buccinator muscle. The buccal artery, a posterior branch of the facial artery, supplies the posterior half, and the inferior buccal and anterior buccal arteries, both of which are branches of the facial artery, supply the inferior and anterior regions [61].
The branches of the internal maxillary artery that supply blood to the buccinator are the buccal artery and the posterior superior alveolar artery. The buccal artery supplies blood to the posterior part of the muscle, whereas the posterosuperior alveolar artery participates in the supply of the posterior superior region [62].
Lastly, the anterior superior region of the buccinator is also supplied by small branches of the infraorbital artery.
All of these vessels converge to form an anastomosis that enables several pedicle flaps to be harvested. On the lateral surface of the muscle, a venous anastomotic system forms the buccal plexus that drains into the facial vein, namely, the pterygoid plexus.
5.7.3 Indications
The buccinator flap can be attached anteriorly, posteriorly, or superiorly. A myomucosal island flap is also possible. The flap obtained is delimited cranially by the parotid duct, anteriorly by the oral commissure, and posteriorly by the pterygomandibular ligament [61].
It can be used for reconstruction of the nasal cavity [63], hard palate [64], soft palate [65], dental alveolus, upper lip, maxillary antrum, and floor of the orbit if it is attached superiorly. When it is attached inferiorly, it can be used to reconstruct the floor of the mouth, lateral border of the tongue [66], mandibular vestibule [67], tonsillar fossa, and lower lip [68]. The island flap described by Zhao et al. [39] makes it possible to reconstruct defects of the lateral wall of the pharynx and of the base of the tongue [41].
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


