Fig. 7.1
Treatment algorithm used in the facial palsy unit of La Paz University Hospital
Below we analyze some of the most common surgical techniques, with emphasis on the main features of surgery and the latest approaches.
7.4 Direct Suture with or Without Interposition Graft
Successful outcome depends mainly on tension at the site of anastomosis [4] and the time since the lesion occurred [5]. Therefore, when feasible, neurorrhaphy should be performed when the lesion occurs. If the suture is tense or it is necessary to bridge a nerve defect, we can use a sural nerve or auricular nerve graft. The great auricular nerve is ideal because it is in the same surgical field and, anatomically, gives off several branches that enable us to reconstruct several branches of the facial nerve when necessary. The sural nerve can be used in cases requiring a very long graft (Figs. 7.2 and 7.3).
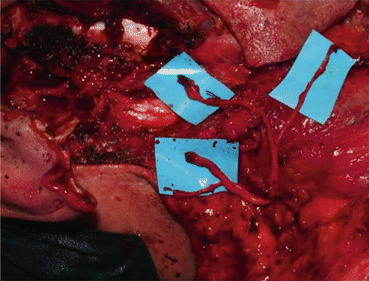
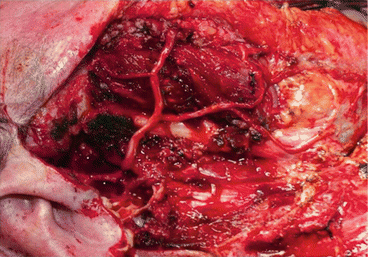

Fig. 7.2
Parotid gland carcinoma. Facial nerve reconstruction from the intramastoid area (facial nerve trunk) to the anterior facial nerve branches

Fig. 7.3
The major auricular nerve is used as a graft with its four branches
Every attempt should be made to reconstruct all the nerve branches to the limit set by the mid-pupillary line. At more anterior sites, it is practically impossible to find a branch for anastomosis.
The surgical technique we use for neurorrhaphy involves several epineural stitches, enough to provide stability to the nerve and prevent the loss of axonal white matter, but not so many that the suture material itself interferes with reinnervation. When suturing is intrapetrous, only two stitches are made on the anterior surface; the posterior surface provides a stable point owing to the location of the nerve in the bony canal. Microsurgical suturing is completed with fibrin sealant (Tissucol®). The best functional results with this technique are achieved if reconstruction is early. Results can even be evaluated as early as the first months after surgery (Fig. 7.4).
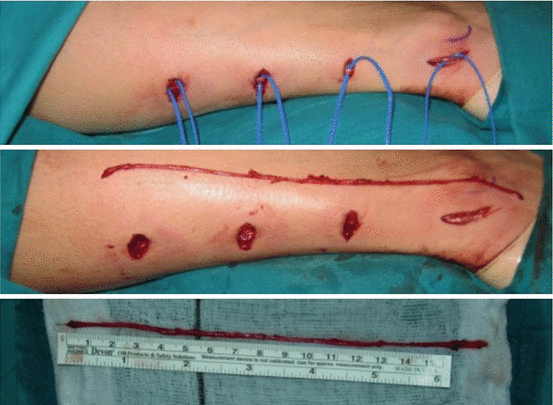

Fig. 7.4
Sural nerve dissection through small transversal incisions
7.5 Hypoglossal–Facial Nerve Anastomosis
In this approach, the hypoglossal nerve is sectioned beyond the descending branch, and end-to-end anastomosis is performed at the distal end of the facial nerve. Sacrificing the hypoglossal nerve leads to hemitongue atrophy, which causes some discomfort. The main advance in recent years has been hypoglossal–facial nerve semi-end-to-end anastomosis, which is performed by dissecting the facial nerve along its intrapetrous course and bringing it down to the level of the hypoglossal nerve, to which it is joined without having to completely section the nerve [8].
Hypoglossal–facial nerve anastomosis is a simple, quick technique with very good results. The first signs of reinnervation generally appear 5–6 months after surgery and include reappearance of expression wrinkles and folds, especially in the nasolabial fold, and a return to facial symmetry at rest. The patient will subsequently be able to develop the first voluntary contractions with the help of rehabilitation and retraining.
This technique is used both as definitive treatment and “babysitter” treatment for maintaining facial muscle tone while waiting for the impulse in the cross-graft performed during surgery [9, 10].
During rehabilitation, the patient is taught to smile using the impulse in the hypoglossal nerve, that is, with tongue movements, despite the limitations, this imposes on the ability to achieve a spontaneous and emotional smile. If the patient has undergone cross-facial nerve grafting, a specific rehabilitation program must be designed to achieve emotional smiling once the electromyographic data show that the impulse has reached the muscles on the paralyzed side from the contralateral facial nerve.
If only one surgical procedure is performed (hypoglossal–facial nerve anastomosis combined with cross-grafting, the microsurgical sutures are end-to-side between the sural nerve and facial nerve grafts on the affected side. Monitoring with electromyography is performed at approximately 12 months. If a contralateral facial nerve impulse is detected in the muscles of the affected side, specific rehabilitation must be started. If surgery is to be performed in two procedures (hypoglossal–facial nerve anastomosis combined with cross-grafting without anastomosing the distal end to the damaged facial nerve), the second procedure will be at approximately 8–10 months in order to anastomose end-to-end the ends of the sural nerve to the facial nerve of the affected side. At 6–8 months after the second procedure, electromyography can show whether the impulse has arrived and, thus, rehabilitation can start.
Both options are feasible. Our series show that long-term results are slightly better in patients who underwent two procedures, probably owing to the better conservation of the facial muscles when the contralateral facial nerve impulse arrives, since it receives a stronger impulse from the hypoglossal nerve. Nevertheless, most interventions involve only one procedure since the results are also good and general anesthesia is used. In addition, the second procedure is often complicated, even though the end of the nerve is marked with synthetic material. It is important to evaluate each patient on an individual basis and take his or her preferences into account (Figs. 7.5, 7.6, 7.7, and 7.8).
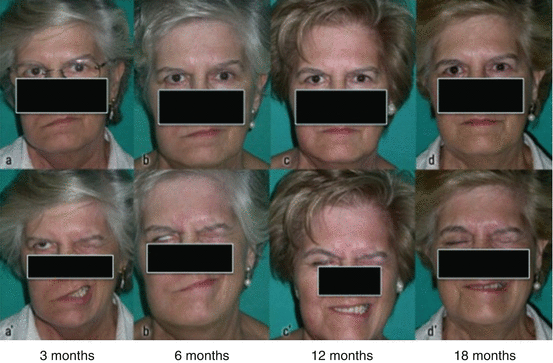
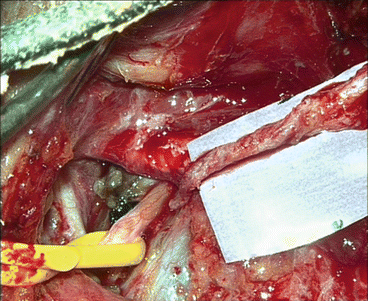
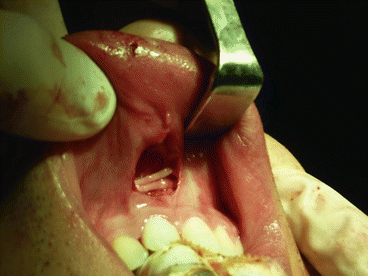
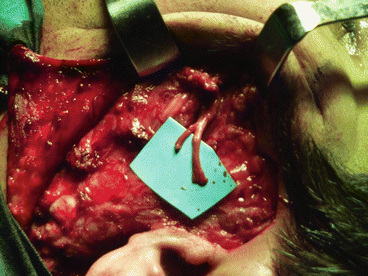

Fig. 7.5
Clinical evolution of a facial nerve reconstruction (orbicularis oris, orbicularis oculi, and zygomaticus muscle branches) using a major auricular nerve graft. The frontal and marginal branches palsy are camouflaged with botulinum toxin

Fig. 7.6
Facial nerve dissected and descended from its temporal location to the hypoglossal nerve

Fig. 7.7
Small superior lip vestibular incision used to tunnel sural nerve grafts

Fig. 7.8
Sural nerve graft ready to be anastomosed on hemifacial palsy side
7.6 Masseteric–Facial Nerve Anastomosis
Facial reinnervation can also be achieved using the masseteric nerve, the motor branch of the trigeminal nerve. The masseteric nerve is easy to locate within the masseter using appropriate references. Sacrifice produces no major sequelae, except for a slight loss of strength when chewing in some cases [11].
The facial nerve can be reinnervated using an auricular nerve graft from the masseteric nerve to the damaged trunk of the facial nerve at the point where it exits the stylomastoid foramen. The procedure can also be performed directly without a graft by dissecting the facial nerve from the ear, especially in totally deaf patients who undergo surgery for tumors of the cerebellopontine angle, and placing it beside the masseteric nerve, as in semi-end-to-end hypoglossal–facial nerve anastomosis. The axons do not have to cross another microsurgical suture, thus facilitating reinnervation and sacrifice of the auricular nerve.
During the rehabilitation process, the patient is taught to smile by using the stimulus from the masseter and instructing him or her to bite down. In principle, this seems to be a more natural way of generating a smile than moving the tongue.
7.7 Cross-Facial Nerve Grafting from the Healthy Side
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


