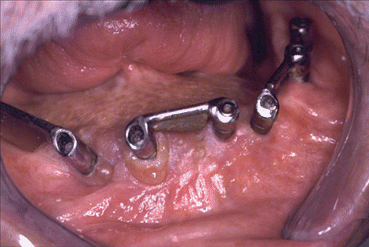
Fig. 1.1
Mandibular tumor (ameloblastoma)
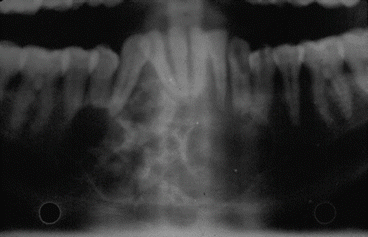
Fig. 1.2
Preoperative OPT
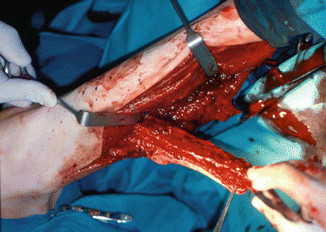
Fig. 1.3
Fibula flap dissection
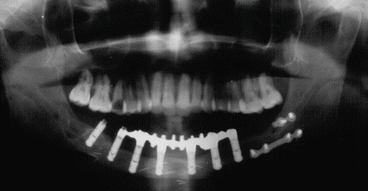
Fig. 1.4
Postoperative OPT with dental implants
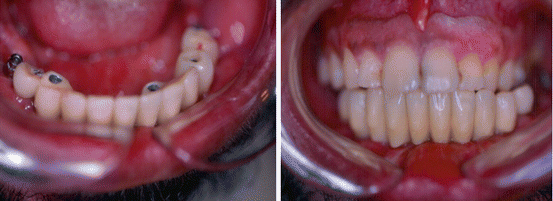
Fig. 1.5
Dental prosthesis and occlusion
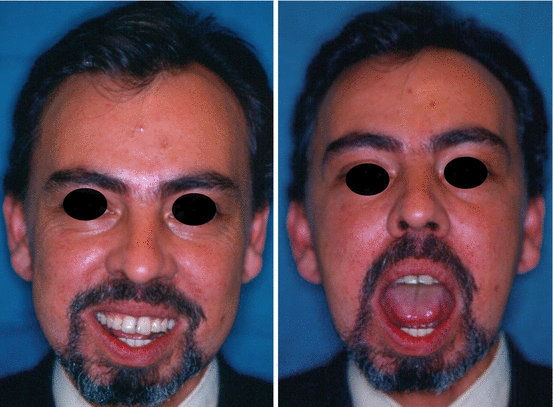
Fig. 1.6
Postoperative view
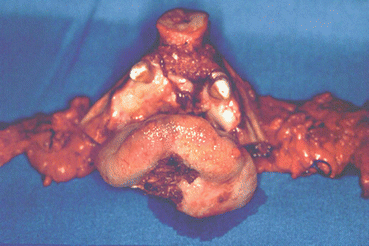
Fig. 1.7
Ablative resection
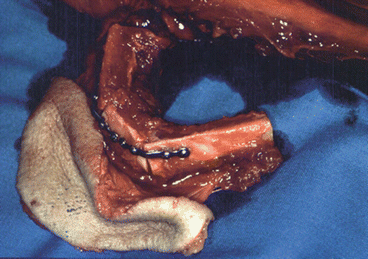
Fig. 1.8
Fibula flap intraoperative design
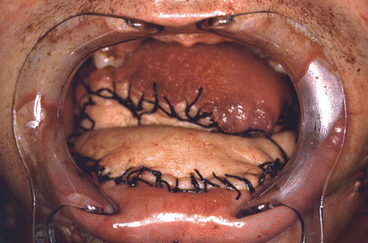
Fig. 1.9
Immediate postoperative reconstruction
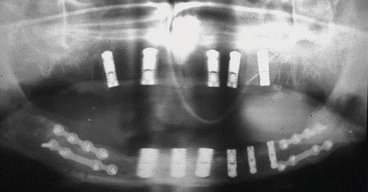
Fig. 1.10
Postoperative OPT
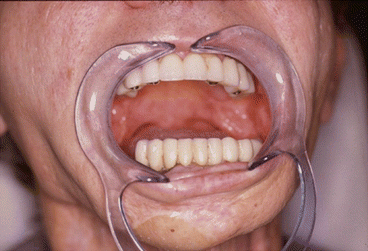
Fig. 1.11
Definitive occlusion
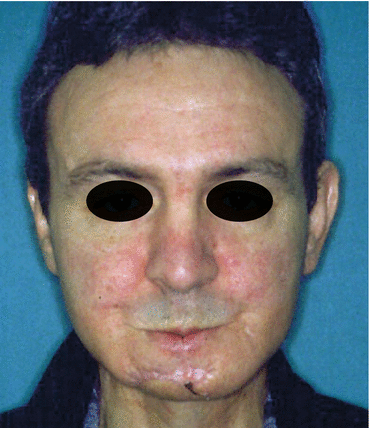
Fig. 1.12
Postoperative view
1.8.2 Iliac Crest Flap
The iliac crest flap is based on the deep circumflex iliac artery, which arises from the external iliac artery 1–2 cm cranially to the inguinal ligament. It runs toward the anterosuperior iliac spine, internal face of the iliac bone, and between the iliacus and transversus abdominis muscles. It gives off an ascending branch, which supplies the lesser oblique muscle, periosteal and endosteal branches that supply the bone, and musculocutaneous perforating branches toward the skin.
Venous drainage is from the deep circumflex iliac vein, which is usually a double vein, into the external iliac vein.
Skin is obtained via the perforators along the internal part of the crest that cross the three muscles of the abdominal wall. Therefore, a considerable part of the major and minor oblique muscles and the transversus abdominis must remain attached to the internal portion to carry the perforators. It is also necessary to design a wide skin flap to incorporate as large a number as possible of perforators (between three and nine in a field that extends longitudinally 9 cm posterior to the anterosuperior iliac spine and 2.5 cm medial to the crest). The wide mesentery of the skin flap limits the relative mobility of the skin.
The anatomical characteristics of this flap are as follows: short vascular pedicle (5–7 cm); 1.5–3 mm diameter at its origin; bone length, 14–16 cm; lesser oblique muscle of 10 × 15 cm; and skin surface of 15 × 25 cm.
Its main indications are as follows:
-
Mandibular bone defects. We think that the iliac crest has the best quality, height, and thickness for mandibular reconstruction of all the bone flaps; however, as it is only 10–12 cm long, larger defects require a fibular flap. It takes the thickest and longest osseointegrated implants, which can be inserted during the same procedure.
-
In defects of the symphysis, the flap can be molded to the form of the defect using osteotomies and preserving the periosteum of the internal surface to maintain the supply to the bone. When the defect includes the body and ascending ramus of the mandible, the ramus can be contoured by designing an “L”-shaped flap.
-
Bone defects associated with extraoral soft tissue defects. In this case, the cutaneous part of the flap is used to reconstruct the defect, although inguinal skin is considerably paler in color. The cutaneous part can also be used to monitor the flap
-
Bone defects associated with intraoral soft tissue defects. In these cases, the flap is only feasible if it contains internal oblique muscle. The large volume of soft tissue renders it inadequate for this type of reconstruction. We prefer other types of osteocutaneous flap, such as the fibula, scapula, and trapezius osteocutaneous flaps.
The excellent quality of the bone in an iliac crest flap makes it possible to fit a sufficient number of implants for the rehabilitation of most patients with an implant-supported prosthesis. Since the height of the flap is similar to that of the remnant mandible, for dentulous patients the crown-implant ratio obtained is optimal (1:3; the crown accounts for 33 % of the total length of the crown-pillar-implant complex). Implants can be fitted during mandibular reconstruction with a balanced occlusal relationship. We obtained a 94 % osseointegration success rate with Mozo Grau implants (MG osseous) and, in the long term, a 12 % failure rate [64].
In our opinion, the iliac crest flap is the best flap for mandibular bone reconstruction when we do not need to reconstruct soft tissue and for the reconstruction of the symphysis and mandibular body up to 10 cm (Figs. 1.13, 1.14, 1.15, 1.16, 1.17, 1.18, and 1.19).
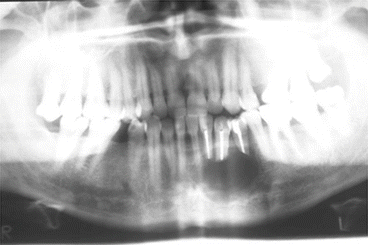
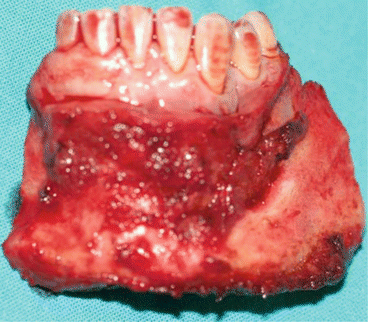
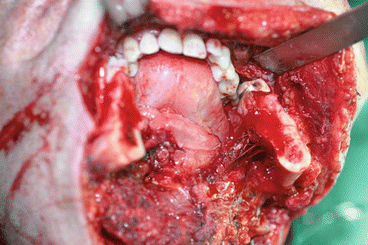
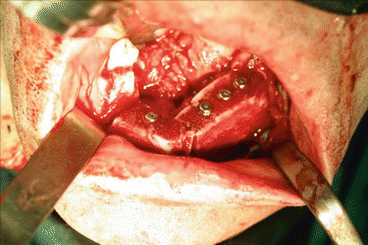
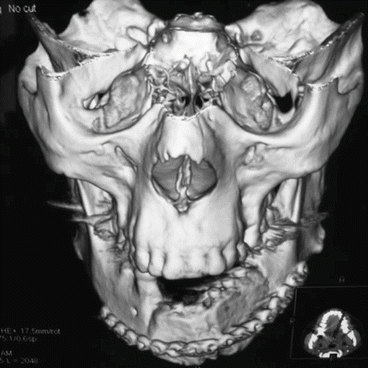
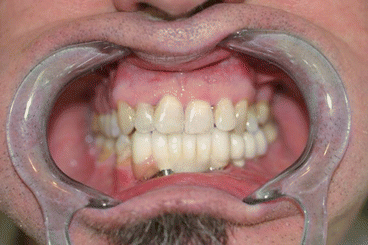
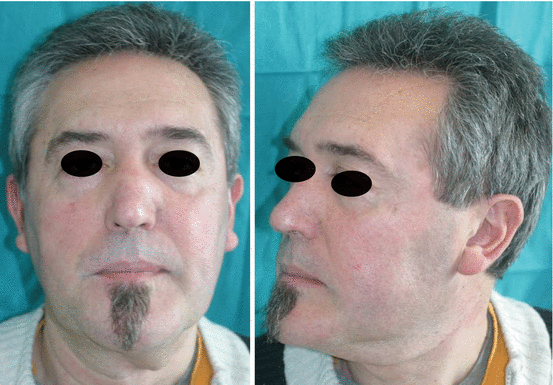

Fig. 1.13
Preoperative

Fig. 1.14
Tumor resection

Fig. 1.15
Defect after ablative surgery

Fig. 1.16
Intraoperative reconstruction with iliac crest free flap and MG osseous implants

Fig. 1.17
Postoperative CT

Fig. 1.18
Final occlusion

Fig. 1.19
One year postoperative views
As shown in the indications (see above), reconstruction of soft tissue requires the use of the internal oblique muscle, which is excessively bulky. Navarro Cuellar et al. [65] present an alternative technique that enables mandibular reconstruction using an iliac crest flap combined with one or two nasolabial flaps to reconstruct intraoral soft tissues. This technique combines the advantages of mandibular reconstruction and insertion of osseointegrated implants (MG osseous) using an iliac crest flap in combination with reconstruction of anatomically adapted intraoral soft tissue defects, avoiding the dissection of internal oblique muscle (Figs. 1.20, 1.21, 1.22, 1.23, 1.24, and 1.25).
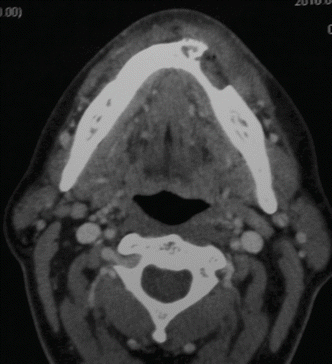
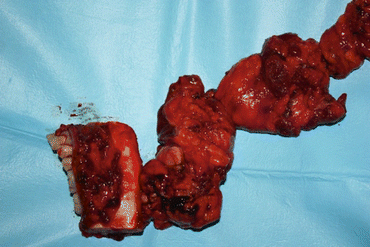
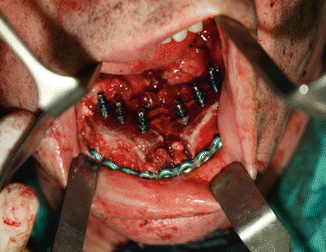
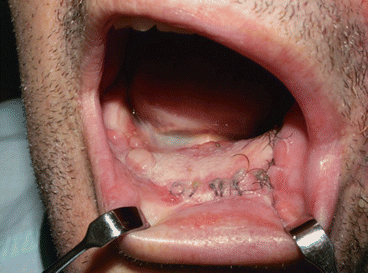
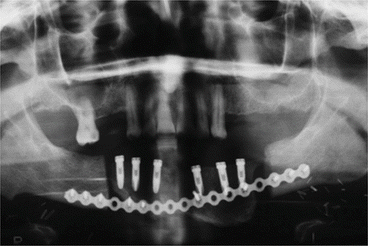
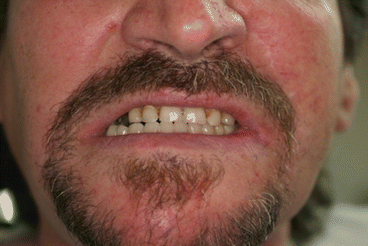

Fig. 1.20
Preoperative CT

Fig 1.21
Squamous cell carcinoma resection with cervical dissection

Fig. 1.22
Iliac crest free flap reconstruction with MG osseous implants

Fig. 1.23
Nasolabial flap covering iliac crest flap

Fig. 1.24
Postoperative OPT

Fig. 1.25
Final occlusion
1.8.3 Scapular Flap
In 1981, Teot et al. [66] described the scapular and parascapular osteomyocutaneous flap. Swartz et al. [67], Baker and Sullivan [68], and Sullivan et al. [69] subsequently reported the use of the scapular osteocutaneous free flap for immediate mandibular reconstruction.
The skin covering the posterior surface of the scapula and the periosteum of the lateral border of the scapula are vascularized by the scapular circumflex artery, a branch of the subscapular artery.
The circumflex artery exits the triangular space and divides into a horizontal branch (scapular flap) and a vertical branch (parascapular flap), which supply the skin field (14 × 21 cm) covering the scapula.
The specific anatomical distribution of the vessels means that the bony part of the flap can be placed independently in three dimensions with respect to the skin flap. The mobility of the soft tissue with respect to the bone makes it possible to reconstruct complex orofacial defects in which soft tissue requirements are as important as the bone defect itself.
Many options are available for reconstruction using this flap, since it can be exclusively muscular, musculocutaneous, osteomyocutaneous, or combined with the latissimus dorsi and serratus anterior (megaflap).
In addition, the skin covering the scapula is thin, hairless, pliable, and similar in color to facial skin [70].
The flap provides well-vascularized corticocancellous bone (1.5–3 cm wide and 10–14 cm long). We can also obtain a further 3–4 cm from the angle of the scapula if we include the angular branch of the thoracodorsal artery.
The disadvantages of this flap are the need to rotate the patient, thus preventing two surgical teams from working simultaneously. It has been suggested that this disadvantage could be avoided by placing the patient on his/her side, although it is still difficult for two teams to work simultaneously. Furthermore, the amount of bone is limited, thus hindering reconstruction of large defects and placement of implants. The resulting scar is usually unsightly, and sensory reinnervation of the flap is not possible.
The characteristics of the scapular flap are as follows: pedicle diameter, 3–4 mm; length, according to Swartz et al. [67] and Neukam et al. [71], is 4–6 cm from the scapular border to the axillary artery (6–9 cm if bone is not taken; if bone is included, the pedicle is shortened); bone length, 14 cm in men and 10 cm in women (if we include the tip, we gain a further 3–4 cm); bone thickness, 1.5 × 3 cm; and skin surface, 14 × 21 cm (sizes greater than 12 cm hinder direct closing).
The scapular flap is our last option for mandibular reconstruction. We think it has very specific indications, as follows:
-
Three-dimensional orofacial defects with large defects of bone and soft tissue (intraoral and extraoral), since the mobility between these parts is considerable
-
If the patient has peripheral vascular disease involving the iliofemoral and tibiofibular system and the defect cannot be reconstructed using a trapezius osteomyocutaneous flap
As reported by Deschler and Hayden [72], the contralateral scapula is usually shaped to the defect for two reasons. First, removal of the scapular flap requires disinsertion of several muscles from the upper edge (long part of the triceps, teres major and minor, and subscapular muscle), thus weakening the arm. If we proceed to radical dissection, the shoulder will be even more limited. Therefore, in order to prevent weakening of the arm and of the shoulder, the contralateral scapula is shaped to the defect and radical dissection performed. Second, by using the contralateral scapula and moving the lateral border of the scapula downward in the neomandible, we ensure that the pedicle emerges distally, in the area of the angle. Thus, the orientation of the pedicle in the neck is optimal.
Weakness of the upper arm is minimized by immobilization for a few days after surgery and rigorous physiotherapy [70] (Figs. 1.26, 1.27, 1.28, 1.29, and 1.30).
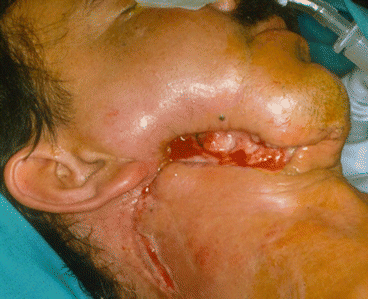
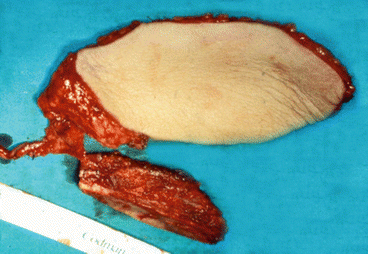
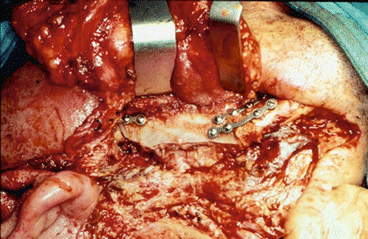
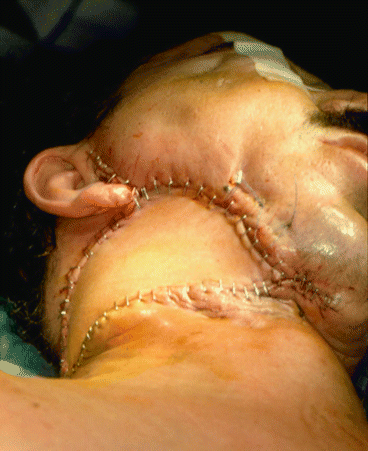
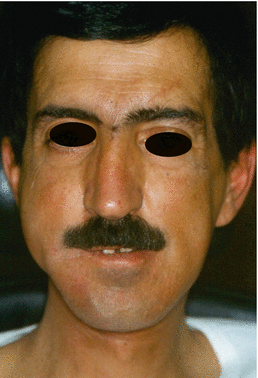

Fig. 1.26
Mandible tumor [87]

Fig. 1.27
Scapular free flap dissection

Fig. 1.28
Scapular free flap adapted at the defect

Fig. 1.29
Immediately postoperative view

Fig. 1.30
Final appearance
1.9 Pedicle Flaps
1.9.1 Trapezius Osteomyocutaneous Flap
The trapezius osteomyocutaneous flap was first described in 1977 by Demergasso and Piazza [73]. It is formed by the upper and middle portion of the trapezius muscle, a skin island from the shoulder and scapular spine, and the acromion of the scapula.
The flap is supplied by the superficial transverse cervical artery, its main pedicle, and receives an accessory supply from the dorsal scapular artery, the occipital artery, and the intercostal arteries.
This supply makes it possible to obtain three different myocutaneous flaps [74]: the superior trapezius myocutaneous flap, which is based on the occipital artery and the intercostal paraspinal perforators; the lateral trapezius osteomyocutaneous flap, which is based on the superficial transverse cervical artery; and the inferior trapezius flap, which is based on the dorsal scapular artery and the deep branch of the transverse cervical artery.
We only discuss the lateral trapezius osteomyocutaneous flap (trapezius island flap), since it is the only one of the three that includes richly vascularized scapular bone [75].
It is based on the superficial transverse cervical artery and vein. In 80 % of cases, the superficial transverse cervical artery arises in the thyrocervical trunk; in the remaining 20 %, it arises in the subclavian artery [76]. When the artery arises directly from the subclavian artery, it can course deeply or via the brachial plexus, thus seriously limiting the arc of rotation of the pedicle and necessitating the use of another flap (10 % of cases) [74].
Venous anatomy is much more variable than arterial anatomy. The transverse cervical vein drains into the medial subclavian system in two-thirds of cases and into the external jugular vein (close to its union with the subclavian vein) in the remaining third [77] (Fig. 1.31).
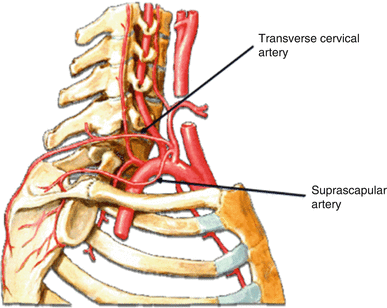

Fig. 1.31
Vascular pedicle [88]
In our experience, the skin paddle and anatomical references must be drawn with the patient seated and arms tight to the trunk. We center the paddle on the acromioclavicular joint. The paddle can be as long as 12–20 cm from the back and up to 10 cm from the shoulder [78].
Including the acromion, the scapular spine measures about 13.5 cm in length and 0.7 cm in height at its medial border and up to 4 cm at its lateral border. Its width ranges between 1 and 2.4 cm.
Depending on the location of the mandibular defect, we use the acromion, spine, or both, as follows:
1.
Symphyseal defect: can be reconstructed exclusively with the acromion and respecting the scapular spine
2.
Lateral defect: can be reconstructed with the scapular spine respecting the acromion at its anatomical site
3.
Mixed anterior and lateral defect: requires both the acromion and the scapular spine
In order to prevent functional sequelae, the muscle at the donor site must be reconstructed at closure: the supraspinatus muscle is sutured to the infraspinatus muscle. Once joined, both muscles are sutured to the deltoid, and the anterior group is anchored to the clavicle by nonabsorbable suture through purpose-made openings. The skin island is closed with a posterior rotation flap.
One of the reasons this flap has fallen into disuse was the fact that it was impossible to insert dental implants, without which only 10 % of patients could wear stable prostheses. In their study of cadaver scapulas, Navarro Vila et al. [74] showed that the acromion can take 13-mm implants in 100 % of cases, whereas the lateral border of the spine can do so in 80 % and the medial border in 20 %.
The trapezius island flap is indicated for mandibular reconstruction in patients with intraoral bone and soft tissue defects who simultaneously undergo radical ipsilateral dissection. The acromion and the scapular spine can be used to reconstruct the mandibular bone defect, while the skin island is used to repair the intraoral soft tissue defect. This flap makes it possible to repair bone defects of up to 10–12 cm. In some cases, the skin paddle has been unfolded to repair intraoral and extraoral tissue. The main contraindications are exclusively bone defects (iliac crest or fibula free flaps are preferred) and situations where cervical dissection is functional rather than radical. Using the trapezius muscle for the flap limits external rotation of the scapula, which is necessary for raising the shoulder and elevation and separation of the arm by 180°. It is also necessary to resect the sternocleidomastoid muscle to leave space in the neck so that the flap can be passed through to the mouth. If the dissection is radical, the nerves of the trapezius are always cut (XI pair) and the sternocleidomastoid is resected; therefore, the trapezius flap does not involve added morbidity. A final contraindication is secondary reconstruction after previous cervical dissection, because the pedicle could have been damaged during the first procedure.
A clear advantage of the trapezius flap is that it is a regional flap; consequently, morbidity is reduced, surgical time is shortened, and there is no need for two surgical teams.
Since this flap is more sensitive to the adverse effects of radiation therapy than microsurgical flaps [79], implants must always be placed immediately.
Before microsurgical flaps began to be widely used, Navarro Vila et al. [74] used the trapezius osteomyocutaneous flap to reconstruct the mandible in 78 cases, most of which (52 %) involved squamous cell carcinoma of the floor of the mouth. The cosmetic results were excellent, and the percentage of total/partial failures for this flap at all sites was only 14 %.
Today, this flap is only used when severe arteriosclerosis prevents reconstruction with microsurgical flaps, since the superficial transverse cervical vessels are not usually involved. In addition, as the reconstruction is with a pedicle, there is no need for anastomosis (Figs. 1.32, 1.33, 1.34, 1.35, and 1.36).
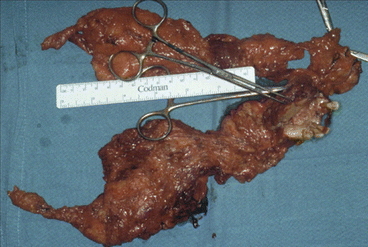
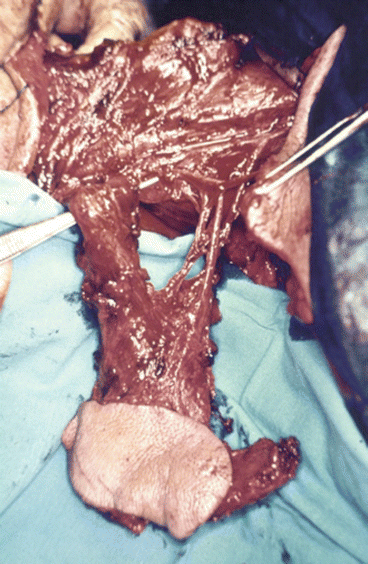

Fig. 1.32
Tumor dissection

Fig. 1.33
Osteomyocutaneous trapezius flap isolated in its vascular pedicle
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses