INTRODUCTION
MATRICING
• Parts of Matrix
• Functions of a Matrix
• Requirements of a Matrix Band
• Classification of Matrices
• Ivory Matrix Holder (Retainer) No. 1
• Ivory Matrix Band (Retainer) No. 8
• Tofflemire Universal Matrix Band Retainer
• Steele’s Siqveland Self-adjusting Matrix Holder for Tapering Teeth
• Anatomical Matrix Band/Compound Supported Matrix
• Retainerless Automatrix System
• T-shaped Matrix Band
• S-shaped Matrix Band
• Full Circle or Ring Bands
• Plastic Matrix Strips
• Precontoured Matrix/Palodent Bitine System
• Aluminium or Copper Collars
• Transparent Crown Forms Matrices
• Anatomic Custom Made Matrix
TOOTH SEPARATION
• Reason for Tooth Separation
• Methods of Tooth Separation
INTRODUCTION
Teeth and periodontium are designed in such a manner that mutually they significantly contribute to their own health and support. They are complimentary to each other. Proper form and alignment of teeth protect periodontium. During mastication, the contours of teeth as a unit protect the periodontium. A breach in the continuity of contacts of teeth give rise to diseases of periodontium resulting in loss of teeth.
Ideal tooth form of interproximal area is as follows:
1. Interproximal embrasures extend on all the four sides of a tooth with definite shape around each contact area. These four embrasures are gingival, occlusal, lingual and facial.
2. Anterior teeth have less pronounced embrasures than posterior teeth (Fig. 6.1).
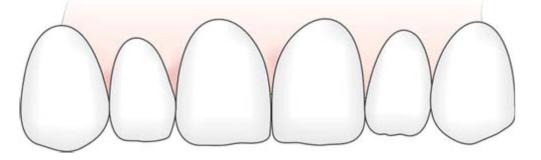
Fig. 6.1: Interproximal spaces of anterior teeth
3. Interproximal space between the adjacent teeth is proper triangular in shape with apex at the contact area and base towards the outer surface (Fig. 6.2). This triangle increasingly widens out in from the contact area of all the four directions-occlusal, lingual, gingival and facial.
Consequences ofnot restoring proximal areas
• Food impaction leading to recurrent caries (Fig. 6.3).
• Change in occlusion and intercuspal relations
• Rotation and drifting of teeth
0 Trauma to the periodontium.
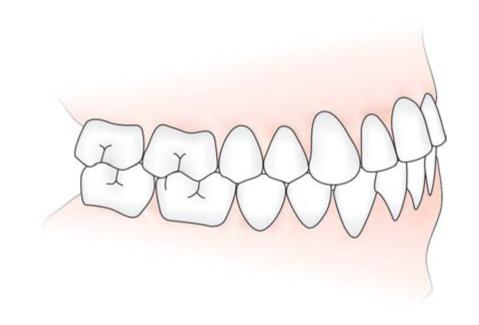
Fig. 6.2: Interproximal spaces of posterior teeth
MATRICING
Restoration of a tooth requires great clinical acumen so as to reproduce the original contours and contacts of the tooth. In case of large missing wall of the tooth, support has to be provided while placing and condensing the restorative material. Usually a metallic strip serves this function and is known as the matrix band. Matrix band which forms the temporary walls is held in its place by means of a matrix band retainer which may be a mechanical device, floss, wire, thread or impression materials, etc.
MATRICING: It is the procedure by which a temporary wall is built opposite to the axial wall, surrounding the tooth structure which has been lost during the tooth preparation.
MATRIX: It is an instrument which is used to hold the restoration within the tooth while it is setting.
Parts of Matrix
Retainer
It holds a band in desired position and shape.
Band
It is a piece of metal or polymeric material, intended to give support and form to the restoration during its insertion and setting. Commonly used materials for bands are:
1. Stainless steel
2. Polyacetate
3. Cellulose acetate
4. Cellulose nitrate.
Matrix band should extend 2 mm above the marginal ridge height and 1 mm below gingival margin of the preparation. Matrices range in width from 6.35 mm (1/4″) to 9.525 mm (3/8″) for permanent teeth and 3.175 mm (1/8″) to 7.9375 mm (5/16″) for deciduous teeth. Their thickness may range between 0.0381 mm (0.0015″) to 0.0508 mm (0.002″).
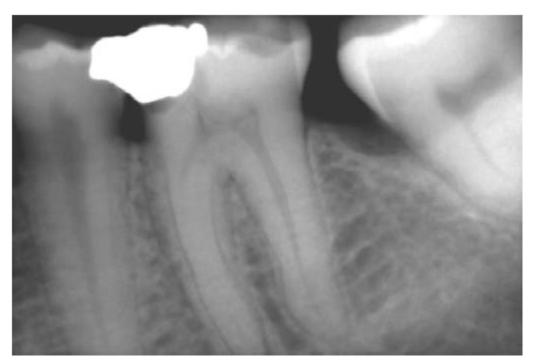
Fig. 6.3: Radiograph showing incorrectly done proximal restoration
Functions of a Matrix
1. To confine the restoration during setting
2. To provide proper proximal contact and contour
3. To provide optimal surface texture for restoration
4. To prevent gingival overhangs.
Requirements of a Matrix Band
To achieve an optimal restoration, matrix band should have following requirements:
1. Rigidity. The matrix band should be rigid enough so as to withstand the pressure of condensation applied during restoration, placement and maintains its shape during hardening.
2. Adaptability: The matrix band should be able to match to almost any size and shape of tooth.
3. Easy to use: The band should be simple in design so that it does not cause any difficulty to the patient, or hindrance to the operator during restoration of the tooth.
4. It should be able to displace the gingiva and rubber dam for ease in working.
5. Nonreactive: It should be inert to tissues and the restorative material.
6. Height and contour. The matrix band should not extend more than 2 mm beyond the occlusogingival height of the crown of tooth. This facilitates vision and speeds up working. The matrix band helps in formation of a physiologic proximal contact relationship.
7. Application: The matrix band should be such that it can be applied and removed easily.
8. Sterilization: It should be easy to sterilize.
9. Inexpensive: It should be inexpensive.
Classification of Matrices
Depending upon their Method of Retention
1. Mechanically retained, e.g. Ivory matrix retainers no. 1 and 8, Tofflemire universal dental matrix band retainer.
2. Self-retained, e.g. copper or stainless steel bands.
Depending upon its Preparation
• Mechanical matrix, e.g. Ivory matrix retainers no. 1 and 8
• Anatomic/custom made matrix, e.g. compound supported.
On the Basis of Transparency
1. Transparent matrices, e.g. cellophane, celluloid
2. Nontransparent matrices, e.g. stainless steel.
Depending upon the Tooth Preparation for which they are Used
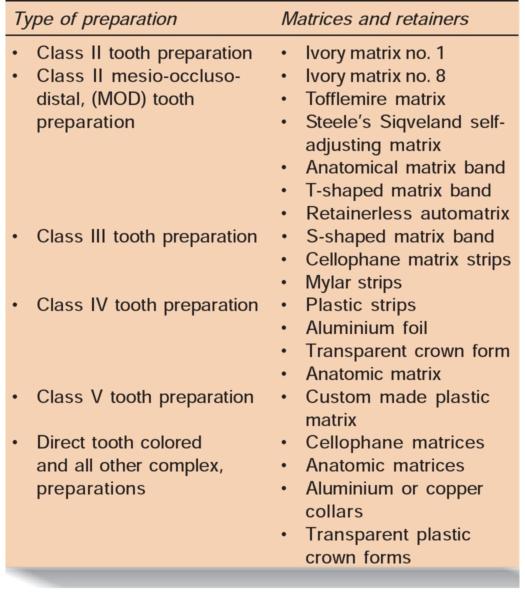
Ivory Matrix Holder (Retainer) No. 1
Ivory matrix holder no. 1 is most commonly used matrix band holder for unilateral class II tooth preparations. The matrix holder has a claw at one end with two flat semicircle arms having a pointed projection at the end (Fig. 6.4). On the other end of the matrix band holder, there is a screw which when tightened, brings the ends of both the claws closer to each other. Band used with this matrix has one margin slightly projected in its middle part. This projected margin is kept towards the gingiva on the side of tooth preparation. The band of suitable size is selected and encircled around the tooth. Keeping the matrix band around the tooth, the screw of the retainer is tightened so that the band perfectly fits around the tooth. After this, wedge is placed which also helps in further adaptation of the matrix band to the tooth (Fig. 6.5).
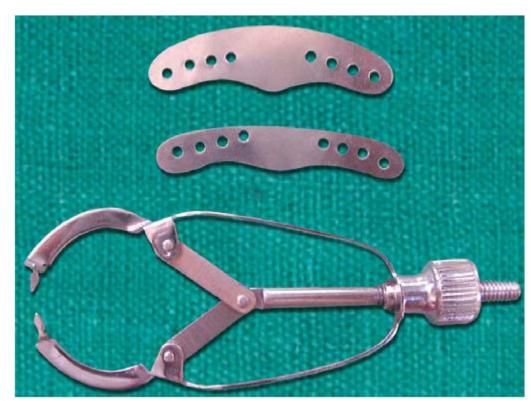
Fig. 6.4: Ivory no. 1 matrix retainer and band
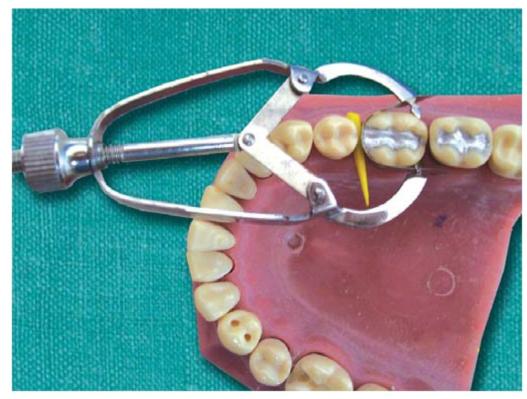
Fig. 6.5: Matrix and band used in class II restoration
Indication
For unilateral class II tooth preparations.
Advantages
• Economical
• Used for restoring class II tooth preparations
• Can be sterilized.
Disadvantage
Cumbersome to apply and remove.
Ivory Matrix Band (Retainer) No. 8
Ivory matrix band retainer holds the matrix band that encircles the tooth to provide missing walls on both proximal sides. The matrix band is made up of thin sheet of metal so that it can pass through the contact area of the unprepared proximal side of the tooth (Fig. 6.6). The circumference of the band can be adjusted using the screw present in the matrix band retainer.

Fig. 6.6: Ivory no. 8 matrix and bands
Indications
• Unilateral or bilateral class II preparations (MOD).
• Class II compound tooth preparations having more than two missing walls.
Advantages
• Economical
• Can be sterilized.
Disadvantage
Cumbersome to apply and remove.
Tofflemire Universal Matrix Band Retainer
It was designed by Dr BF Tofflemire. It is also well known as `universal’ matrix because it can be used in all types of tooth preparations of posterior teeth. In this, the matrix band is fitted onto the retainer and then fitted loosely over the tooth, which then can be tightened in position by means of the screw (Fig. 6.7).

Fig. 6.7: Tofflemire retainer
Toff lemire matrix
• Also known as universal matrix
• Design given by DrTofflemire (Name based on inventor)
• Preferred for class II and compound amalgam restorations
Indications
• Class I tooth preparations with buccal or lingual extensions.
• Unilateral or bilateral class II (MOD) tooth preparations.
• Class II compound tooth preparations having more than two missing walls.
Advantages
• Can be used from both facial and lingual sides
• Economical
• Sturdy and stable in nature
• Provides good contact and contours
• Can be easily removed
• Can be sterilized.
Disadvantages
• Cannot be used in badly broken teeth
• Does not offer optimal results with resin restorations.
Types of Tofflemire Matrix
1. Based on type of head
a. Straight (Fig. 6.7):
i. Head of matrix system is straight
I Placed only from buccal side
b. Contra-angle (Fig. 6.8):
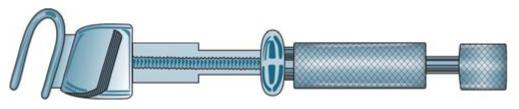
Fig. 6.8: Angulated Tofflemire retainer
i. Head is angulated
ii. Placed either from buccal or lingual side.
2. Based on type of dentition
a. Standard-used in permanent dentition
b. Small-used in primary dentition.
Parts of Tofflemire Retainer
Head
• Uses slots for positioning of matrix
• U-shaped head with two slots in open side
• Open side of the head should be facing gingivally when the band is placed around the tooth (Figs 6.9 and 6.10).
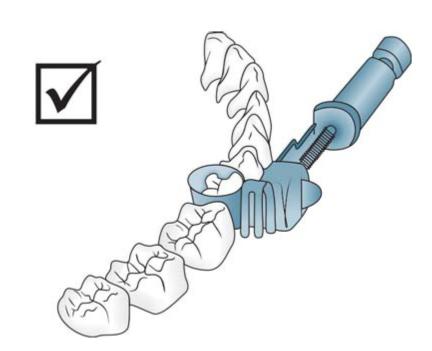
Fig. 6.9: Slots of head should always be directed gingivally
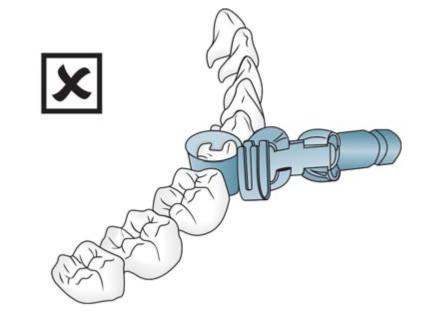
Fig. 6.10: Slots should not be directed occlusally
Slide (Diagonal slot)
1. Amount of band extending beyond the slot depends upon type of tooth to be treated.
2. This portion is located near the head for installation of band in the retainer, helps in placement of band around the tooth.
Knurled nuts
1. Two knurled knots in retainer
a. Large knurled nut-near the matrix band
b. Small knurled nut.
a. Large knurled nut (Also known as rotating spindle)
• Helps in adapting the loop of matrix band against the tooth.
• Helps in adjusting the size of loop of matrix band against the tooth.
b. Small knurled nut-helps in tightening the band to retainer.
Assemblyofretainer. When band and retainer are assembled, two ends of band must be of same length protruding from the diagonal slot (Fig. 6.11).

Fig. 6.11: Assembled Tofflemire matrix band with retainer
Loop extending from retainer can project in following ways (Fig. 6.12):
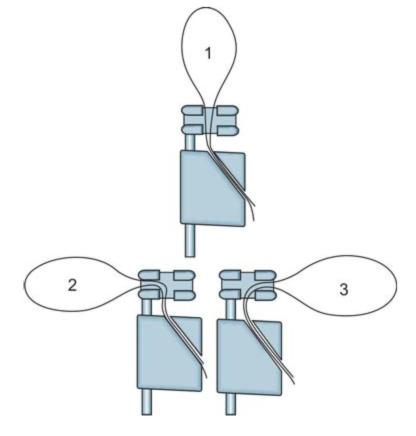
Fig. 6.12: Loop from band can extend in straight, right or left direction
1. Straight-used near anterior teeth
2. Left/right-used mostly in posterior areas of oral cavity.
While adapting the matrix band to retainer loop of the matrix, band appears as funnel-shaped, i.e. one side of the opening has greater diameter than other (Fig. 6.13). Opening with greater diameter should be placed occlusally while with lesser diameter should be placed gingivally.

Fig. 6.13: Tofflemire with band in place
Types of bands
Two types of bands are usually used:
1. Flat bands
2. Precontoured bands.
1. Flat bands
a. Available in two thicknesses
i. 0.0020 inches
ii. 0.0015 inches
Any of these thicknesses can be used, it depends upon operators preference.
b. According to shapes, three shapes of flat bands are available (Fig. 6.14)
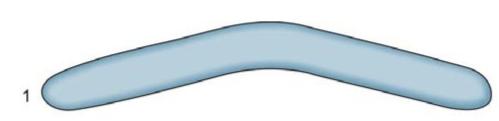
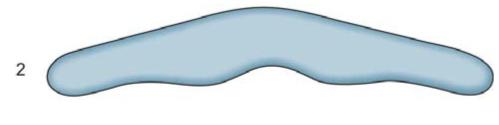
Fig. 6.14: Three types of Tofflemire bands
i. No. 1 or universal band
ii. No. 2 or (MOD band): It has two extensions projecting at gingival edge. It is commonly used in molars.
iii. No. 3: Similar to No. 2 band in design but narrower than No. 2.
• Flat band needs to be contoured before placing it in retainer. Contouring of band can be done with the help of:
i. Ovoid burnisher
ii. Spoon excavator (using its convex side).
2. Precontoured bands: They are also available but less commonly used. While removing these bands, one must take care of contour of band. Band should be rotated in such a way that its trailing end should not fracture the restoration.
Operative instruction for placement (Figs 6.15A to D)
1. First open the large knurled nut so that slide is at least 1/4 inch from the head (Fig. 6.15A).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


