Microvascular surgery significantly altered the art and science of maxillofacial reconstructive surgery. Microsurgical technique rapidly gained popularity because of the positive impact it has had on the reliability of reconstructive efforts. A significant difference exists between local-regional flaps and microvascular flaps in that the blood supply to the microsurgical flaps is robust. The majority of the microvascular free tissue transfers are oriented directly over a segmental blood supply. The local-regional flaps universally place the most poorly supplied portions of the entire flap at the defect site. In oral cavity reconstruction, that places the most vulnerable tissue in a very challenging environment. Local-regional flaps do not reliably contain the type and volume of bone often required in maxillofacial reconstructions. Additionally, the majority of the volume of tissue transferred in a local-regional flap is nowhere near the recipient site.
The versatility of microvascular flaps allows the reconstructive surgeon to have myriad options to match the specific needs of each circumstance to the techniques and flap chosen. The type (bone, skin, oral-pharyngeal lining), volume, and character of the tissue can be restored by selecting a flap with those desired characteristics. Microvascular flaps will never completely replace traditional local-regional flaps in all instances. The advantages of the technique, specifically reliability, adaptability, and single stage surgery, make microsurgery an extremely useful and necessary technique for the maxillofacial surgeon.
Etiopathogenesis and Causative Factors
Maxillofacial microvascular surgery is used to manage tumors, trauma, and congenital deformities. The majority of these defects or deficiencies contain composite tissues. Mucosa, skin, and bone must all be replaced in these cases if premorbid or normal form and function is to be completely restored. Microsurgery techniques are the only way to completely reconstruct composite tissue defects in one surgical procedure. Restoration of the dentoalveolar complex is critical in all cases of maxillofacial reconstruction, because several studies report that patients’ quality of life and self-image are closely tied to the ability to chew and swallow normally. Microvascular flap selection is carried out with the intention of replacing the lost or missing tissue in one surgical setting as much as possible. Experience has demonstrated the suitability of certain flaps in specific situations. It is not possible to use one flap for all purposes.
Tumor resection oftentimes produces similar defects that quickly become familiar to the reconstructive surgeon. For example, all microsurgeons have been faced with the challenge of an anterior mandibular defect after the resection of an advanced cancer on the floor of the mouth. This quickly becomes routine, and the surgeon develops considerable finesse in the manipulation of fibula bone segments to achieve the complex contour of the anterior mandible while simultaneously restoring the volume and mobility of the floor of the mouth with the transferred skin component of the flap. Once the three-dimensional assessment of the defect is mastered, tissue that was lost in the tumor ablation can be more accurately replicated. Oral and oral-pharyngeal tissues are commonly replaced with the free radial forearm flap (FRFF), anterolateral thigh flap (ATF), lateral arm flap, or scapula flap. Composite tissue and bone containing defects are generally restored using the free fibula osteocutaneous flap (FFOF) or the deep circumflex iliac artery (DCIA) flap. Occasionally, the composite tissue defect characteristics require the composite scapula flap.
Trauma reconstruction is quite complex because the defects created by the trauma are widely varied. The majority of the trauma defects that require microvascular technique are avulsive injuries associated with high velocity projectiles or blasts. The maxillofacial microsurgeon draws heavily on the experience gained in tumor reconstruction. The same three-dimensional assessment skills developed in tumor surgery allow the microsurgeon to appropriately plan reconstructions for trauma patients, so that surgical interventions are minimized without sacrificing ideal form. The free fibula and DCIA flaps are commonly used in jaw reconstruction, whereas the free radial forearm flap and scapula composite flap are used to restore other structural elements of the maxillofacial region.
Congenital deformities may on occasion benefit from microsurgical technique as well. Hemifacial microsomia and juvenile rheumatoid arthritis may require restoration of a significant portion of the mandible, in particular the temporomandibular joint. Once again, the experience gained in ablative tumor reconstruction, in which mandibular disarticulation is required, provides the maxillofacial microsurgeon with familiarity in this type of defect.
Microvascular Flap Anatomy
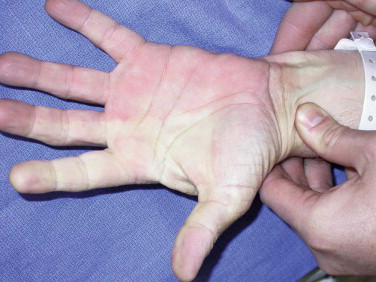
In general, microvascular flap anatomy is based on a named major blood vessel or significant perforating vessel. The vessel anatomy of all the common flaps has been widely studied and reported upon. The diameters of these vessels are in the range of 1.5 to 3 mm. There are two major flaps in which presurgical vessel anatomy assessment is mandatory. The flaps requiring preoperative assessment are the FRFF and the FF. In the cases of the FRFF, the absence of an intact palmar arch could result in ischemia to portions of the hand. This can easily be assessed with the Allen test. The failure to restore normal blood flow to the hand after release of the ulnar artery and exsanguination with both the radial and ulnar arteries occluded signifies an incomplete palmar arch ( Fig. 7-1 ). Another simple and practical test involves occluding the radial artery with a pulse oximeter probe on the thumb of the hand on the planned donor arm. The potential donor leg for the free fibula flap must be assessed for the presence of a peroneal dominant circulation or significant atherosclerotic disease. It is estimated that between 10% and 20% of patients have diminutive anterior tibial or posterior tibial vessels and are reliant on the peroneal artery for perfusion of the distal portions of the lower limb. These conditions could be easily identified by the use of magnetic resonance angiography, which is preferred over arteriography because adequate information can be obtained without the radiation or contrast media exposure. Some maxillofacial microsurgeons have their patients undergo Doppler imaging and mapping of the lateral lower leg to identify the location of septocutaneous perforating vessels to the overlying skin. Studies show the consistent presence of a major perforator with 2 cm of the midpoint of the fibula between the head of the fibula and the lateral malleolus. Additional studies show a predominance of septocutaneous perforators eight tenths of the way along the fibula.
The specific anatomy of the commonly used flaps is discussed in detail in the chapters that follow. For convenience sake, a table summarizing the vascular characteristics of the flaps is included ( Table 7-1 ).
| FLAP | VASCULAR PEDICLE | VESSEL DIAMETER (mm) | PEDICLE LENGTH |
|---|---|---|---|
| Radial forearm | Radial artery | 2.5 | Long |
| Cephalic vein | — | — | |
| Fibula flap | Peroneal A/V | — | Variable |
| Rectus abdominis | Deep inferior epigastic A/V | 3.4 | Long |
| Gracilis | Branch of adductor A/V | 2 | Up to 6 cm |
| DCIA | DCIA/V | 2-3 | 6-8 cm |
| Scapula | Circumflex scapular A/V | 3 | Variable |
| Anterolateral thigh | Profunda femoris A/V | 3 | Variable |
| Lateral arm | Posterior radial collateral A/V | 2.5 | Short |
Recipient vessel selection must be considered early in the planning process for maxillofacial microsurgical reconstruction. Previous irradiation, prior surgery, or the presence of fixed adenopathy can greatly alter the availability or suitability of vessels for microsurgical anastomosis. This is quite similar to the need for extremity microsurgeons to select a microvascular technique that ensures that they are outside the “zone of injury” when selecting the location for microsurgical anastomosis.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


