Traumatic dental and maxillofacial injuries are common occurrences, and affect worldwide approximately 20% to 30% of permanent dentition, often with serious aesthetic, functional, psychological, and economic consequences. With such a high frequency of injuries, prevention becomes a primary goal. A prevention approach relies on the identification of etiologic factors, and on giving rise to measures aimed at avoiding those factors or at reducing their impact. This article reviews the etiology and preventive strategy regarding dental injuries, and examines the role and manufacture of appliances, especially mouthguards, in preventive dentistry.
Traumatic dental and maxillofacial injuries are common occurrences, and affect worldwide approximately 20% to 30% of the permanent dentition, often with serious esthetic, functional, psychological, and economic consequences. With such a high frequency of injuries, prevention becomes a primary goal. A prevention approach relies on the identification of etiologic factors, and on giving rise to measures aimed at avoiding those factors or at reducing their impact ( Fig. 1 ).
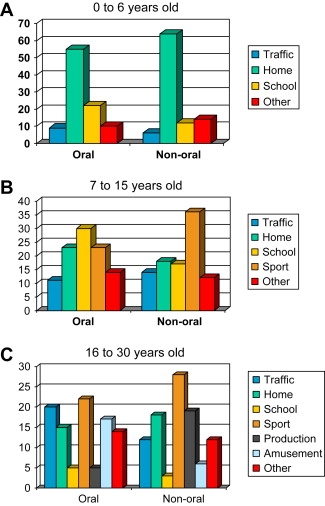
Several epidemiologic studies have examined the etiology of injuries. However, only a few have offered analysis leading to indications of preventive measures that could be instituted to interfere in the etiology of injuries. Fig. 1 shows data regarding the environment in which the traumatic injuries occur: traffic, home, school, and others. It appears from Fig. 1 that injuries in those older than 7 years occur more frequently during sports activities. Fortunately, sport is the activity for which preventive measures seem feasible and that may be effective in reducing the rate and severity of oral trauma. Traffic accidents are the next most frequent cause of oral trauma, and here also preventive measures to avoid or reduce the consequences of severe impacts are feasible.
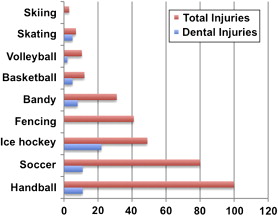
A significant number of oral and dental injuries result from contact sports such as American football, basketball, rugby, soccer, boxing, wrestling, or “stick sports” ( Fig. 2 ). However, there is a growing indication that oral and dental injuries occur as much if not more often during children’s play or leisure activities. For example, in a study by Skaare and Jacobsen in Norway in 2003, nearly half (48%) of the 1275 injured individuals reported were injured at school. Sports and traffic accidents were less common in their sample. Organized sports accidents represented only 8% of the total number of injuries, similar to the number of individuals injured by violence. The investigators concluded that probably only one-third of the injuries were preventable. The same results were reported by Andreasen in 2001 from a sample of 3655 dental casualty insurance claims from a major Danish insurance company. Thus, 7% of the dental trauma claims were due to organized sports whereas 93% resulted from varied and unpreventable causes. In both studies, the investigators felt that it is neither easy to prevent dental injuries nor to create guidelines on prevention. Based on these studies, it seems that promoting the use of mouthguards and facial masks is an insufficient strategic measure to prevent oral trauma.
Education as a preventive strategy for traumatic dental injuries
The best strategic measure for preventing dental and oral injuries is probably education. Education should be targeted equally at children, teenagers, and those in the vicinity (parents, school officials, and youth leaders), particularly in situations whereby potential risks for injuries exist. Information should be given on how to avoid injuries and on how to manage them, preferably at the site of the injury. It should be the aim of every dentist to discuss risk factors that could lead to dental or oral injury during routine dental visits. This education should be aimed at both genders equally. Even though some older epidemiologic data indicated that boys were more prone to sustain oral and dental injury, with increased participation of girls in traditionally male sports (eg, basketball and soccer), as well as in leisure activities (eg, roller-blades and skateboarding), the gap seems to be narrowing, at least in some geographic areas.
Special strategic measures should be attempted for individuals at high risk, such as those with severe maxillary overjet, as it has been shown that the odds of sustaining dental trauma are significantly and linearly related to the severity of the overjet. It has even been suggested that a preventive orthodontic treatment should be initiated for these individuals to be completed before the age of 11 years, that is, in the early to middle mixed dentition stage, in an attempt to reduce their risk of sustaining trauma.
In addition, it is advisable to give special counseling to individuals who present a history of previous oral trauma, as those seem more likely to sustain a new injury compared with those who have not sustained any. The risk of sustaining multiple injuries has been reported as being 8.4 times higher when the first trauma episode occurred at 9 years of age, compared with it occurring at age 12. Therefore, young children should receive special attention. Their activities, games, and sports involvement should be carefully assessed, and any risky behavior should be discussed with them, their parents, or those who care for them. A typical example is the recent popularity of basketball hoops that can be lowered from standard height, so that 10- to 12-year-olds can “slam-dunk” or place the ball in the net by jumping up and hanging on the net ring that holds the net after letting go of the ball. Because their arms are short at that age, their maxillary incisors are often at the level of the basket. This scenario has now been reported to result in increasing severities of dental trauma whereby multiple teeth are frequently avulsed.
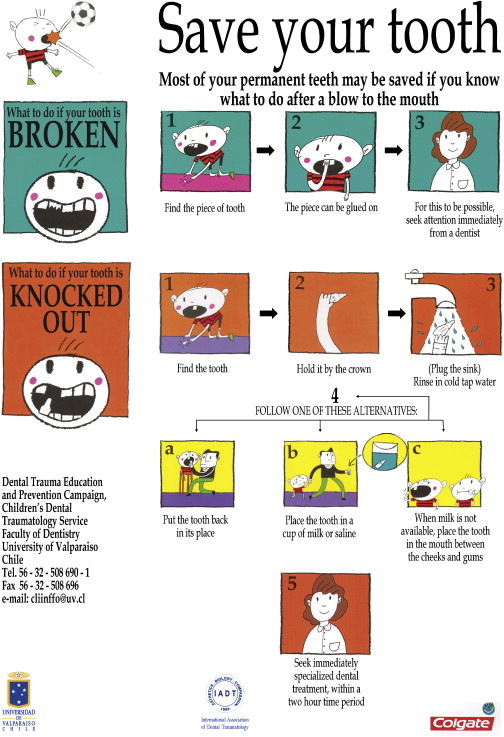
Information campaigns, whether through television or newspapers, or with distribution of brochures and posters, are also useful strategies for the prevention of traumatic dental injuries. All children should be made aware of correct first aid when an injury occurs. Elements like trying to replant an avulsed tooth immediately or alternatively storing it in milk, and looking for all fragments of a broken tooth before running home for help, should be explained to them in clear, simple language. Posters such as the one sponsored by the International Association of Dental Traumatology (IADT) and others ( Fig. 3 ) gain the attention of young individuals and, if widely displayed, should reinforce their knowledge.
Not only the young should be educated about dental trauma but also those who care for them, especially those who are responsible for their safety during school and organized activities. A simple instruction sheet ( Table 1 ) is in most cases sufficient to ensure that injured patients receive proper emergency care at the site of the injury. When educating persons not trained in dentistry it is important to avoid using complicated language. Table 1 suggests a communication form, which is based on the IADT’s guidelines. Its language is clear, and explains in simple terms what to do and what not to do immediately after dental trauma. The form also advises as to the urgency of a necessary dental consultation.
| Term | Type of Injury | Immediate Treatment | Dental Referral |
|---|---|---|---|
| Uncomplicated crown fracture |
|
None | Within 48 hours, especially if the patient has difficulty due to cold sensitivity |
| Complicated crown fracture | Portion of the tooth broken off and bleeding from the fracture | None; do not place any medication on the bleeding pulp. If needed have the patient bite into a gauge | As soon as logistically possible; could wait until the next morning if the patient tolerates eating and drinking |
| Root fracture |
|
None | As soon as possible |
| Tooth concussion and subluxation | Tooth still in its normal place and firm or slightly loose | None | Within 48 hours, for evaluation only |
| Luxation | Tooth very loose and/or the crown has moved from its normal position | Only move the tooth back to normal position if it is easy to move it | As soon as possible, especially if it is not possible to reposition the tooth |
| Avulsion | Tooth completely out of the mouth |
|
Immediately. It is extremely important for prognosis of the tooth to be treated immediately |
Appliances to prevent dental injuries
Traumatic impacts provoke an acute delivery of energy that is released upon soft and hard tissues, resulting in laceration, contusion, or ablation of tissues. Protective devices (eg, mouthguards) to reduce the consequences of such impacts can act by preventing the impact from reaching the oral region or by cushioning, absorbing, or distributing the impact forces. During sports and other activities in which there is a risk of falling or being hit by an object, wearing a faceguard or mouthguard still seems to be the only way to prevent or at least significantly reduce the seriousness of dental injuries. It has been reported that before the mandate of wearing faceguards and mouthguards in United States high school football, facial and oral injuries constituted up to 50% of all reported football injuries. Subsequent to the mandate a significant decrease was noted in reported injuries, down to a few percent. Another common mechanism of oral injury is traffic accidents. Wearing seatbelts in a car, and using a helmet with a chin arch when riding a motorcycle is mandatory in many countries. Most commonly used bicycling helmets provide good protection against head injuries, as shown in Victoria, Australia when after 1 year of mandatory use of helmets, there was a 48% reduction of reported head injuries in cyclists. Unfortunately these same helmets do not offer any mouth or dental protection.
Faceguards
A faceguard is usually a prefabricated cage of metal or composite that is attached to a helmet or a head strap ( Fig. 4 ). Guards made of clear polycarbonate plastic have recently become available, either as prefabricated or custom made. These faceguards seem to provide good protection to the face and teeth, but are not applicable to all activities, and in many cases do not protect the teeth if the individual is hit under the chin.

Few large-scale studies have been conducted on the actual benefits of wearing faceguards in games or practice, but it is clear that the introduction of mandatory helmet and facial protection has been effective in virtually eliminating ocular, facial, and dental injuries in juvenile hockey. However, an unforeseen problem has been reported for the same group of youths: whereas the number of head injuries has been reduced, an increase in catastrophic spinal injuries has been noted. It has been speculated that players get a false sense of security when donning the equipment, leading them to take excessive and unwarranted risks due to the protection they are supposedly afforded. One of the few intervention studies on the effectiveness of faceguards was performed by Danis and colleagues on a group of youth league baseball teams in the United States. Approximately one-half of the teams were supplied with guard helmets (intervention); all others used this protection at their discretion (comparison). The investigators found that the intervention teams reported a reduction in the incidence of oculofacial injuries compared with comparison team respondents ( P = .04). Half facemasks have been popular in hockey, as it has been speculated that a full face shield may increase the risk of concussions and neck injuries, offsetting the benefits of protection from dental, facial, and ocular injuries. A recent study found that the use of full face shields is associated with a significantly reduced risk of sustaining facial and dental injuries without an increase in the risk of neck injuries, concussions, or other injuries.
With the emergence of many new fiber composites, custom-fabricated faceguards will become easily available and affordable. Studies confirming their benefits must be conducted.
Mouthguards
The use of mouthguards in contact sports has been reported in the past to reduce the occurrence of dental injuries up to 90% or more. Because rules regarding the use of headgear and mouthguards in high school football were established in the 1960s, facial and dental injuries sustained on the field have dropped by approximately 48%.
Few studies have specifically investigated, prospectively or in real time, whether athletes who wear mouthguards sustain significantly fewer dental injuries than those who do not. The first study to do so involved a sample population of 272 high school rugby players. The athletes received a preseason clinical examination by a team of dentists and completed a questionnaire. Mouthguards were fitted 1 week later and the players were instructed in their use. At the end of the season, a follow-up questionnaire was completed. There was a significant difference in the number of tooth fractures between mouthguard wearers and those without mouthguards. The second study, which evaluated United States male college basketball players (age 18–22 years), collected real-time data. Trainers reported information about their teams on a weekly basis using an interactive Web site. The results of this study are likely to be significant, as it captured 70,936 athlete exposures (an athletic exposure is a one athlete participating in a game or practice, whether it was one play, one quarter, one half, or the entire game). The study found that mouthguard users had significantly lower rates of dental injuries and dentist referrals than nonusers. However, there was no significant difference between mouthguard users and nonusers in the rate of soft tissue injuries. Of note, this study reported significantly more oral or dental injuries than reported by the National Collegiate Athletic Association for the same season. In a more recent study, trainees participating in basic military training at Fort Leonard Wood, Missouri, who were not wearing mouthguards during certain training exercises (eg, unarmed combat, rifle/bayonet training, confidence/obstacle course) were significantly (almost twice) more likely to sustain orofacial injury compared with another group of trainees who were required to wear a mouthguard during all exercises. Not all studies have demonstrated a beneficial effect of mouthguards. In a cross-sectional study, a sample of 321 university rugby players participating on 555 player occasions was examined. The results of that study indicated no statistically significant association between oral, dental, and lip injuries sustained during rugby playing with the use or nonuse of mouthguards. This study, like most mouthguard studies irrespective whether they demonstrated a beneficial effect, is relatively small and therefore likely to have only limited statistical power. Large-scale studies are therefore needed.
Role of mouthguards
It has been suggested that a mouthguard should protect the wearer against injuries in five different ways:
- •
Preventing tooth injuries by absorbing and deflecting blows to the teeth
- •
Shielding the lips, tongue, and gingival tissues from laceration
- •
Preventing opposing teeth from coming into violent contact
- •
Providing the mandible with resilient support, which absorbs an impact that might fracture the unsupported angle or condyle of the mandible
- •
Preventing neck and cerebral brain injuries
Various materials and methods have been used in attempts to achieve these basic protective functions of mouthguards; and as many test protocols and devices have been tried to confirm their effectiveness. The main problem with testing mouthguards’ eventual protective role is that there is no in vivo model ethically feasible, and in vitro models are at best crude approximations. To further complicate matters, large prospective cohort studies, which could be useful in reaching higher statistical significance, are difficult to conduct and are, to some degree, equally unethical, due to the need for crossover or control groups.
Although no conclusions can be drawn so far from the literature confirming that mouthguards are effective in protecting the wearer, some elements are worth noting:
- •
In recent studies from a Japanese group an attempt was made to investigate actual objects that could hit mouthguards and teeth during an athletic event, rather than a steel drop-ball that has been frequently used in studies on mouthguards. These studies indicated that transmitted forces were less when a standard single-layer mouthguard was used compared with no mouthguard but, just as important, they demonstrated that the effect was significantly influenced by the object type. The steel ball showed the biggest (62.1%) absorption ability whereas the wooden bat showed the second biggest (38.3%). Other objects, baseball, field hockey ball, and hockey puck, showed from 0.6% to 6.0% absorbency. These results show that it is important to test the effectiveness of mouthguards on specific types of sports equipment rather than using standard experimental equipment that may provide an unrealistic outcome.
- •
It has been shown that the physical and mechanical properties vary with their chemical composition, and this itself varies with different brands of the same material (see later in this article). The resilience of PVAc-PE materials seems to vary inversely with the magnitude of the impact energy at which they are tested. Several factors may be responsible for this variation, including the degree of crosslinking between polymer chains, the proportion of plasticizer present, and the volume of filler particles.
- •
It has been suggested that laminated thermoplastic mouthguards are dimensionally more stable in use.
- •
It has been suggested that high-energy absorption does not necessarily indicate that the material will give maximum protection, because some of the absorbed energy may be transmitted directly to the underlying dental structures. Research elucidating this matter is needed.
The fifth suggested protective role of a mouthguard is to prevent neck or cerebral brain injuries. Through the years there has been a great deal of discussion in the literature on whether mouthguards contribute toward prevention of cerebral concussion in athletes. However, most of the articles have been solely case reports or opinions, unfortunately not based on controlled scientific studies. The two articles usually cited as a foundation of this presumed preventive effect were written by Stenger and colleagues in 1964 and Hickey and colleagues in 1967, both of which are based on limited research and extremely small sample size. With careful scrutiny of scientific evidence in the literature, this claim of protectiveness of the mouthguard on cerebral injuries has been called into serious question. Two large studies using an interactive Web site to collect weekly information on incidence of cerebral brain concussion in athletes have failed to show any benefits. In the first study, a comparison was made between those who wore a mouthguard and those who did not in US College men’s basketball. Almost 71,000 athletic exposures were reported, but there was no significant difference in the rate of brain concussion between the groups. The second study compared boil-and-bite versus custom-made mouthguards worn by American college football players. More than 500,000 athletic exposures were recorded but again, there was no significant difference between the two groups. These two studies did not assess the mechanism of injury, for example, blow under the chin versus fall to the ground. However and unfortunately, these two studies do not indicate that wearing a mouthguard helps to reduce cerebral brain concussion in any significant way. Manufacturers of stock mouthguards have in recent years started to make unsubstantiated claims regarding their product, and have even gone as far as to market stock mouthguards under brand names like “Brain Pad” and “Brain Pad plus.” A study compared the effectiveness of one of these padded dual-jaw mouthguards, the Wipss Brain Pad (Wipss Products Inc., Conshohocken, PA) with other currently used mouthguards in the prevention of concussion injuries in athletes participating in university football and rugby. The study design was a multicenter, cluster-randomized, controlled trial including five Canadian universities for one season. No dental trauma events occurred. The researcher found no significant difference in the concussion rates between players who wore the Wipss Brain Pad mouth guard and those who wore other types of mouthguard. Of note is that no dental injury was reported in the study group during the observation time.
Types of mouthguards
Mouthguards can be divided into 3 basic types based on how they are manufactured and used:
- •
Stock prefabricated
- •
Mouth formed
- •
Custom made
Some of these basic types now have several subgroups, especially the custom-made ones.
- •
Stock mouthguards may be made from rubber or plastic materials. Stock mouthguards are generally available in 2 or 3 sizes; and are supposed to have a universal fit, sometimes aided by flanges in the molar area. Modification is limited to trimming the margins to relieve the frenula. The loose fit means that the wearer must occlude to prevent the guard from being displaced. The main advantage of this type of mouthguard is that they are inexpensive and may be purchased by the public in sports shops. Also, because they do not require any preparation, a replacement is readily available. Most reports agree that these types of mouthguard provide the least protection of all available types due to their poor fit, though admittedly there is no conclusive scientific data confirming this opinion. However, it is unquestioned that these mouthguards are uncomfortable for the wearers; they tend to obstruct speech and breathing because the wearer literally must keep them in place by clenching or supporting it with his or her tongue. Therefore they are less likely to be worn and when needed, could be blown out of the mouth before impact with the ground or other obstacles.
- •
There are two types of mouth-formed mouthguards that may be made from a manufactured kit. The first consists of a hard and fairly rigid outer shell that provides a smooth, durable surface and a soft, resilient lining that is adapted to the teeth ( Fig. 5 ). The outer shell of vinyl chloride may be lined with a layer of self-curing methyl-methacrylate or silicone rubber. The outer shell is fitted and trimmed, if necessary, around the sulci and frenal attachments. The shell is filled with the soft lining and seated in the mouth. Care must be taken to ensure that it is centrally placed. The lining is allowed to polymerize for 3 to 5 minutes. Excess material is trimmed with a sharp knife, and the margins smoothed with dental stones. This type of mouthguard tends to be bulky, and the margins of the outer shell may be sharp unless protected by an adequate thickness of the lining material. The most commonly used type of mouth-formed protector is constructed from a preformed thermoplastic shell of PVAc-PE copolymer or PVC that is softened in warm water and then molded in the mouth by the user (see Fig. 5 ). These mouthguards have several distinct advantages over the stock mouthguard. If carefully adapted, they give a closer fit and are more easily retained than stock protectors. Care must be taken during the molding process so that the mouthguard fits accurately. The temperature necessary to allow adequate adaptation to the teeth is fairly high, so additional care must be taken to avoid burning the gingiva. Similar to the stock mouthguard, this type of mouthguard is relatively inexpensive, readily available to the general public, and can be formed into a decent appliance with some care.
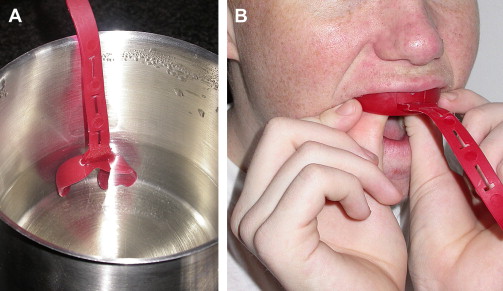
Fig. 5 Boil-and-bite being formed in the mouth. ( A ) The stock mouthguard is heated in boiling water and then inserted in the mouth. ( B ) The index fingers are used to adapt the mouthguard as well as possible to the facial sides of the molars, while the thumbs press on the palatal side. - •
Custom mouthguards are individually made in a laboratory, on plaster of Paris models poured from impressions of the player’s mouth. Many studies have shown that these mouthguards are more acceptable and comfortable to athletes than the other types There is no evidence, however, that custom-made protectors are more effective in preventing injuries. Historically, three groups of materials have been used to fabricate custom-made mouth protectors: molded velum rubber, latex rubber, and resilient acrylic resins. By far the most common material being used currently for custom-made mouthguards is ethylene vinyl acetate (EVA) copolymers. Polyvinylchloride and soft acrylic resins such as polyurethane were also used previously, but the superiority of the EVA copolymers has practically eliminated the others. Its popularity is mainly due to its elastomeric softness and flexibility, and it can be relatively easily processed. Also, the material has good clarity and gloss, barrier properties, low-temperature toughness, stress-crack resistance, and little or no odor. Many prefabricated plates of EVA are now commercially available; but it is important to know that the percentage of vinyl acetate (often marked %) can vary between manufacturers, therefore the plates can show different properties. When higher proportions of vinyl acetate are copolymerized (higher % marking), the EVA plate is more flexible, stretchable, softer, and tougher. This higher percentage also lowers the softening temperature, allowing manipulation of the material within a comfortable temperature. The most common EVA copolymers used for fabrication of mouthguards contain 28% vinyl acetate. It should be remembered, though, that the actual performance of a mouthguard relies not only on its intrinsic material properties but also on its design and thickness, and on the type of traumatic impact on the mouth.
The EVA mouthguard material can be bought in varying colors, thickness, and hardness. There has been discussion on whether there should be a different stiffness or hardness for different sports. Thus, whereas the low-stiffness guards absorb shock during hard-object collisions (eg, baseballs), they may not protect the tooth bone during soft-object collisions (eg, boxing gloves). To date, clinical studies to substantiate such recommendations are lacking.
In 1985 Chaconas and colleagues described a laminated thermoplastic mouthguard that showed significantly less dimensional change than other materials tested (ie, poly(vinyl acetate-ethylene) copolymer clear thermoplastic, polyurethane). This type was the first of several different subcategories within custom-made mouthguards. A few years ago, layered EVA stock plates were introduced ( Fig. 6 ), with the intention of further strengthening the mouthguard without losing its protective capacity. When a stock plate of EVA is fabricated, it is drawn out in one direction so that the polymer chains are more or less parallel, like the grain in wood. This stretching can theoretically make a difference to the plate’s properties whether the grains are running faciopalatally or mesiodistally on the crown of the tooth. To eliminate this and increase the stiffness without adding bulk, manufacturers have started to market two- or three-layered stock EVA, whereby the layers have been added perpendicular to each other. Some manufacturers have even added a low-percentage EVA plate between layers, which is designed to further stiffen the mouthguard palatally behind the anterior incisors. There is not much, if any, scientific proof that this can increase the protectiveness of the mouthguard and again raises the question of whether a too stiff mouthguard could cause other damage to the teeth or alveolus. Some alarming findings were reported in a recent study. A hard insert resulted in reduced energy absorption when compared with a control sheet of the same material and approximate thickness but without the hard inserts. The same research group has, however, shown improved impact characteristics of the EVA mouthguard material with regulated air inclusions. However, as yet there are no clinical data available to support this finding, and durability of air-included mouthguards is unknown.

Another version of this layered concept is the fusion of two plates of different stiffness. However, these plates only seem to improve the mouthguard when the softer material is next to the teeth. A study by Kim and Mathieu, using a finite element model, showed that a soft outer layer covering a hard core had no significant difference from a monolayer in stress distribution and impact force. However, a soft core was found to have a significant effect on stress distribution. This effect could be increased by controlling ratios of modulus and volume fractions of the core and outer layer.
The main question regarding these various types of mouthguards is whether there is any actual protective difference between them. Few studies have investigated the efficacy of the different types in preventing dental injuries with large enough samples to have significant power. In one study on 98 professional rugby players, custom-made mouthguards did not significantly reduce the amount of dental injuries sustained compared with mouth-formed mouthguards. At a follow-up clinical examination, there was no damage to teeth when either custom-made or boil-and-bite mouthguards were worn. Stokes and colleagues compared mouth-formed and custom-made mouthguards. This study showed that although there were no dental injuries in either group, the users preferred laboratory-formed mouthguards for reasons of comfort. In a large study on college football players, trainers reported data every week for the entire season, through an interactive Web site, on the number of players, mouthguard use, and dental and oral injuries. There was no apparent difference reported between boil-and-bite or custom-made mouthguards. The sample consisted of 87 (76%) of a possible 114 Division I teams, with a total of 506,297 athletic exposures recorded. Most of the teams used a mixture of custom and boil-and-bite mouthguards, so there was a possibility that the benefits of one particular mouthguard might not be clearly defined. Therefore, the data were further analyzed whereby a subselection of 14 teams were selected, 7 of which used exclusively custom-made mouthguards and the other 7, exclusively boil-and-bite. The results were the same, as no statistically significant benefit of one type of mouthguard was found over the other. It is important to stress that in this study there was no attempt to inspect the quality of the mouthguard used or the comfort of one type over the other. One more recent study does, however, indicate that there might be some difference. In that study Australian Rules football community teams were randomly allocated to use either a custom-made mouthguard or stock mouthguard during games. The results showed that there was a significant protective effect of custom-made mouthguards, relative to using stock mouthguards. However, the study reported on head and oral injures combined, not solely on dental injuries. Also, it lacked a control group.
Wear and tear affects all mouthguards; and it has been suggested that they should be replaced regularly not only due to lack of fit but also because of reduction in protective properties. It has been shown recently in a simulated aging study on different types of custom-made mouthguards that aging induced various dimensional changes. Most of the dimensional changes for all types of mouthguards occurred at the central incisor region. However, pressure-laminated mouthguard specimens showed the lowest range of changes at the central incisor region, suggesting potentially improved fit, comfort, and protection.
Fabrication of mouthguards
Organizations such as the Federation Dentaire International (FDI) have created and published recommended criteria on the construction of an effective mouthguard. Most of these recommendations state the same things:
- 1.
The mouthguard should be made of a resilient material, which can be easily washed and cleaned, and readily disinfected.
- 2.
It should have adequate retention to remain in position during sporting activity, and allow for a normal occlusal relationship to give maximum protection.
- 3.
It should absorb and disperse the energy of a shock by:
- •
Covering the maxillary dental arch
- •
Excluding interference
- •
Reproducing the occlusal relationship
- •
Allowing mouth breathing
- •
Protecting the soft tissues
- •
Furthermore, the FDI also recommends that mouthguards be made by dentists from an impression of the athlete’s teeth.
Fabrication of a mouth-formed mouthguard
Regardless of type, the key for functionality is selection of a stock that fits the arch. If too small, it is likely that the molars will not be properly covered, thereby reducing retention and fit ( Fig. 7 ). Once the proper size is found and fitted, the mouthguard should be made strictly following the manufacturer’s guidelines or recommendations.





