Class
Description
1
Healthy patient
2
Mild systemic disease – no functional limitation
3
Severe systemic disease – definite functional limitation
4
Severe systemic disease that is a constant threat to life
5
A moribund patient who is not expected to survive for 24 h with or without operation
Despite these shortcomings, the ASA classification system is useful in helping to determine a child’s suitability to receive sedation in the dental office. Children classified as ASA 1 or 2 are generally acceptable candidates for treatment in the dental office. Children classified as ASA 4 are best managed in a hospital setting as inpatients. Patients classified as ASA 3 who are stable and well controlled can be safely managed in the dental office provided the procedures planned are of short duration and the targeted depth of sedation is anxiolysis. Unstable ASA 3 patients or ASA 3 patients who require longer, invasive dental procedures are best managed in a hospital setting under general anesthesia. For all patients with a preexisting medical problem (ASA 2–4), medical consultation is advisable prior to undertaking the dental procedure.
Preoperative Assessment
There are several reasons for completing a preoperative assessment and review of systems. Information gathered in the preoperative assessment influences decisions made during the remainder of the sedation appointment and in the postoperative period. A preoperative assessment provides the opportunity for the practitioner to identify risk factors which may impact on treatment planning, engage in a discussion with the parent and staff about the risks identified, and take steps to eliminate or reduce the impact of risks. Most importantly, the preoperative assessment helps the clinician to determine if the child is fit for the procedure. Completing a thorough preoperative assessment may help to reduce parent and/or child anxiety as a result of education and communication which occurs during the assessment. A preoperative assessment also allows the practitioner to determine if further investigations including laboratory investigations or medical consultations are necessary prior to initiating treatment further mitigating risk. Lastly, discussion about the anticipated procedure during the preoperative assessment ensures that the parent, and patient if necessary, has been informed appropriately about the anticipated risks and benefits of the proposed treatment and give consent for treatment.
Medical History
The standard of care dictates that, at the initial dental appointment, all practitioners must obtain an accurate medical history. It is important to remember that the medical history form is a synopsis of the child’s medical history. It is a historical account of the child’s medical experiences since birth. For the purposes of sedation, however, updating the medical history requires focusing on several key areas. This can be accomplished by the dentist themselves or delegated to a trained auxiliary. Often, a medical history update is completed while the child is assessed physically. The dentist should read the medical history update, confirm its accuracy, and seek clarification where necessary. Table 3.2 outlines key items in the medical history that should be reviewed prior to the sedation appointment. Answers to questions asked in this regard should be recorded and dated in the dental record.
Table 3.2
Sedation-specific medical history review
|
Allergies, in general, and drug allergies, specifically
|
|
Adverse drug reactions and outcomes
|
|
Current medications including herbal remedies – frequency, dosage
|
|
Previous hospitalizations and ER visits – reason, course, and outcome
|
|
Previous general anesthetics or sedation – outcomes and complications
|
|
Diseases, disorders, or physical abnormalities – current management, responsible physician(s)
|
|
Respiratory system – asthma, frequent infections
|
|
Cardiovascular system – murmurs, congenital anomalies
|
|
GU (renal) system – diseases/anomalies affecting drug clearance
|
|
GI system – diseases/anomalies affecting drug absorption/metabolism
|
|
Central nervous system – developmental delay, emotional or psychiatric disorders
|
|
Special medical conditions – cancer, chemotherapy, visual or aural impairment
|
|
Family history of diseases or disorders
|
Review of Systems
It is most important to review and assess the current status of the major systems before beginning the procedure as this provides the best indication of the child’s fitness for the intended procedure. Important details obtained during the medical history review can be clarified during the review of systems and physical assessment. Generally, the review of systems and physical assessment is completed with the parent present. This may provide emotional comfort for the child but it also provides an opportunity for the dentist to ask the parent questions pertaining to each system as they are reviewed. A quiet environment without distractions helps to maintain child’s attention as well as ensuring that the clinician can discern and interpret subtle sounds or signs. The results of the physical assessment should be recorded on the sedation record.
The physical assessment procedure should follow a logical routine beginning peripherally with nonthreatening procedures such as weight measurement and proceeding to those procedures which require more cooperation of the child such as blood pressure measurement. Beginning with relatively simple procedures for which the child is cooperative will help the child to gain confidence, thereby allowing more involved procedures to proceed. In addition to recording the results of a review of systems, clinicians should also record the child’s age, weight, and the time when the child last ate and drank.
A general assessment of physical stature is also important. The recent reports of increasing prevalence of obesity in children are concerning to dentists who sedate children [2, 3]. Obesity has a significant impact on cardiovascular, respiratory, gastrointestinal, endocrine, and hepatic systems [2]. Management of the obese patient’s airway during sedation can be tenuous at times. An increase in body mass and redundant oropharyngeal airway tissue can result in upper airway obstruction if the clinician is not vigilant in monitoring airway patency or if the patient becomes deeply sedated. Obese patients are also at risk for pulmonary aspiration secondary to increased gastric volume and gastric reflux. Because of these concerns, obese children needing dental treatment with sedation are best managed under general anesthesia. Table 3.3 summarizes the multisystem effects of obesity [4].
Table 3.3
Multisystem effects of obesity in children
|
Pulmonary
|
Cardiovascular
|
Gastrointestinal
|
|---|---|---|
|
Chest wall mass ↑
|
Cardiac output ↑
|
Intra-abdominal pressure ↑
|
|
CO2 production ↑
|
Hypertension
|
Intragastric pressure ↑
|
|
Functional reserve ↓ ↓
|
Stroke volume ↑
|
Risk of aspiration ↑
|
|
Pulmonary compliance ↓
|
||
|
Total O2 consumption ↑
|
||
|
Work of breathing ↑
|
Evaluating Social and Psychological Factors
Clinicians, mistakenly, may overlook social and psychological factors during the assessment of the child believing that physical findings gained from a hands-on assessment are of greater importance than psychosocial issues. A child’s personality, social situation, and experiences will determine how they will react to an experience like sedation for dental treatment. Gathering information about the family, its composition and dynamics, and the child’s personality and temperament will assist the clinician in utilizing a communication style that is appropriate to the situation. Moreover, this information is very helpful in selecting a sedation regimen which is appropriate for the treatment required, the length of the appointment necessary, and the child’s temperament. Is the household led by a single parent? Is the family blended? How many siblings does the child have, their ages, and their relationships with the patient? What communication style does the parent(s) use? Is there a language barrier? What parenting style is most evident? How has the child been socialized? What previous healthcare experiences has the child had, negative and positive, and how have these affected the child’s subsequent behavior in healthcare settings?
Negative experiences are more likely to create anxiety about impending dental treatment especially for the young and inexperienced child or for the timid child. Gathering this information requires that the dental team interview the parent and observe the child. Asking the parent about how their child reacts in other social situations can be revealing especially if the situation is perceived by the child to be potentially threatening. For example, a parent who relates that their child clings to them and cries when visiting the family physician or meeting new people is providing information that is most likely predictive of the same reaction in the dental office. Observing the child’s body language, facial expression, and willingness to make eye contact all help the clinician in developing a sedation plan.
If the child is developmentally delayed, the clinician must learn more about the developmental issues and how it impacts on the child’s cognitive level, expressive and receptive language abilities, comprehension, and attention span. Consulting with the family physician or pediatrician is wise when dealing with a developmentally delayed child. Many developmentally delayed children have associated sensory deficits or hypersensitivities and learning disabilities and often demonstrate behavioral problems which may make the development and implementation of a sedation plan difficult.
Evaluating the Respiratory System
Physical assessment of the child’s respiratory system can often commence with observations of the child while the history is being updated. Mouth or noisy breathing, the allergic salute, and a cough are all important signs to be noted. Important areas to consider in the history as related to the respiratory system are summarized in Table 3.4.
Table 3.4
Respiratory system – medical history
|
Allergies
|
|
Anemia
|
|
Asthma
|
|
Disordered control of breathing
|
|
Upper airway obstructions
|
|
Frequent airway infection
|
|
Chronic congestion
|
|
Bronchopulmonary dysplasia
|
|
Diaphragmatic hernia
|
|
Hyaline membrane disease
|
When evaluating the respiratory system of a child, it is important to have a working knowledge of normal values. Table 3.5 summarizes respiratory variable for various ages.
Table 3.5
Age-dependent respiratory variables
|
3 years
|
5 years
|
12 years
|
Adult
|
|
|
Frequency (breaths/min)
|
24 ± 6
|
23 ± 5
|
18 ± 5
|
12 ± 3
|
|
Tidal volume (mL)
|
112
|
270
|
480
|
575
|
|
VE (minute ventilation, L/min)
|
2.46
|
5.5
|
6.2
|
6.4
|
|
VA (alveolar ventilation, mL/min)
|
1760
|
1800
|
3000
|
3100
|
|
VC (vital capacity, mL)
|
870
|
1160
|
3100
|
4000
|
|
TLC (mL)
|
1100
|
1500
|
4000
|
6000
|
Physical examination of airway should include the following:
-
Identification of obvious anatomic abnormalities
-
Evaluation of mandibular shape and size, especially retrognathia
-
Assessment of the child’s ability to open the mouth
-
Assessment of tonsil/adenoid and tongue size in relation to the volume of the oral cavity and oropharynx
-
Evaluation of the child’s voice
-
Assessment of habitual breathing mode – oral or nasal
Important anatomical and physiological differences between the pediatric and adult airway are cause for concern in pediatric sedation. The pediatric airway is smaller and more compliant than the adult airway. Forceful contraction of the diaphragm can pull the child’s compliant chest wall inward so that even maximal inspiratory efforts cannot generate adequate tidal volumes. The child’s tongue occupies a larger volume in the oropharynx relative to the adult. Posterior displacement of a child’s tongue during sedation by dental instruments or inappropriate head position may cause severe airway obstruction.
Sleep behavior can often give important information about the airway in children. Loud snoring, sleep disturbance, mouth breathing, nasal stuffiness, and frank sleep apnea are all suggestive of adenotonsillar hypertrophy and resultant partial airway obstruction [6]. Nocturnal enuresis and frequent nightmares also often occur in children with disturbed sleep patterns but, on their own in the absence of adenotonsillar hypertrophy, are not contraindications to sedation.
Tonsils and adenoids are often enlarged in children representing an important cause of upper airway obstruction during sedation. To evaluate tonsil size in a child, an airway examination is essential. Various tonsil classification schemata exist but that developed by Brodsky [7] is most applicable to pediatric dental sedations. Tonsil assessment is best done with the child either lying or sitting in a semi-reclined position. A good light is essential. The objective of airway assessment is to determine the size of the tonsils in relation to the pharyngeal airway. Tonsils that occupy 50 % or more of the oropharyngeal volume may be a significant cause of airway obstruction especially in children who are given medications which induce sleep such as chloral hydrate. Figure 3.1 shows tonsils which occupy less than 25 % of the oropharynx and will not constitute an airway obstruction hazard. Figure 3.2 shows tonsils which are kissing in the midline and represent a significant hazard for airway obstruction.
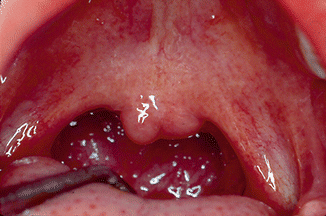

Fig. 3.1
Tonsils which occupy less than 50 % of the oropharyngeal volume are usually not associated with a risk of obstruction during sedation
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


