Pre-cooperative children <4 years old
School-aged children with extensive dental needs whose behavior makes treatment completion unlikely
Children who decompensate following one or more minimal or moderate sedation appointments
Older children with extreme dental anxiety, usually due to past negative dental experiences
Patients with special needs (e.g., cleft lip/palate, intellectual disability, etc.)
Patients with inability to achieve adequate local anesthesia
Children with extensive dental needs in rural areas with few dental resources
Significant oral surgical procedures
Children whose parents want to avoid restraint to complete dental treatment
Children whose parents want to prevent negative early dental experiences
Some social/societal constraints lead to indication for DS/GA. Patients living in rural areas with limited access to care and with extensive dental needs may not have transportation options for several dental appointments. Alternatively, parents taking extensive days off work may be a significant economic hardship placing them in the difficult dilemma of choosing to provide food or other necessities for their family or taking time off for multiple dental visits in a faraway city. Certainly, some oral surgical procedures may require DS/GA for optimal surgical results. Many parents view early dental surgical experiences as very stressful for their children. In an effort to maintain a positive long-term dentist-child relationship, they opt for DS/GA for early age dental care relying on later long-term rapport building during examinations and dental cleanings. Lastly, inadequate local anesthesia for painful teeth requiring extraction or endodontic procedures presents yet another indication. This provides a partial list of common indications for DS/GA.
Definitions
The AAPD definitions of deep sedation and general anesthesia are listed in Boxes 10.1 and 10.2. These are very similar to the ADA definitions but have some added explanations which help amplify some critical points. Some details, however, still require clarification. Deep sedation is a state of consciousness that lies between moderate sedation and general anesthesia. In its most common form, as is typically provided in oral surgery offices where the technique was actually developed, baseline moderate sedation is provided with benzodiazepines and opioids followed by administration of small doses of short-acting intravenous general anesthetic drugs intended to produce short periods of unconsciousness. The patient is then allowed to slowly regain consciousness until they reenter a state of moderate sedation. At this point, if necessary, additional small doses of general anesthetic agents are administered to bring the patient back to a state of light general anesthesia, and this cycle repeats itself throughout the procedure. Because there are periods of light general anesthesia, risks such as pulmonary aspiration of blood, irrigation fluids, dental items, or emesis as well as laryngospasm can occur. These are the same risks that can occur when intended oral moderate sedation progresses to deep sedation. The patient becomes unconscious, airway support is usually needed, and the patient responds to deep painful stimulation with only partial or minimal arousal. According to ADA Guidelines, no treatment should be provided by moderate sedation providers until the patent returns to a state of moderate sedation to minimize the serious complications noted above.
Box 10.1. AAPD definition of deep sedation [1]
“Deep sedation” (“deep sedation/analgesia”): a drug-induced depression of consciousness during which patients cannot be easily aroused but respond purposefully after repeated verbal or painful stimulation (e.g., purposefully pushing away the noxious stimuli)a. The ability to independently maintain ventilatory function may be impaired. Patients may require assistance in maintaining a patent airway, and spontaneous ventilation may be inadequate. Cardiovascular function is usually maintained. A state of deep sedation may be accompanied by partial or complete loss of protective airway reflexes
a Not simply reflex withdrawal (au)
Box 10.2. AAPD definition of general anesthesia [1]
“General anesthesia”: a drug-induced loss of consciousness during which patients are not arousable, even by painful stimulation. The ability to independently maintain ventilatory function is often impaired. Patients often require assistance in maintaining a patent airway, and positive pressure ventilation may be required because of depressed spontaneous ventilation or drug-induced depression of neuromuscular function. Cardiovascular function may be impaired
When profound local anesthesia of a surgical site can be obtained, as for most dental surgical procedures, it is possible to maintain a state of deep sedation or what has perhaps been more accurately termed “ultralight general anesthesia” in which unconsciousness is maintained unless a deeply painful stimulus occurs. The inclusion of high-quality local anesthesia allows administration of smaller amounts of intravenous general anesthetic agents since minimal surgical stimulation and patient arousal occur. General anesthesia is a state where the patient is continually unconscious and unresponsive to surgical and other stimuli even without local anesthesia.
Techniques of Deep Sedation/General Anesthesia
The airway is of primary concern in anesthesia practice, and techniques of general anesthesia are frequently classified as to the type of airway control that is provided. The three main types of airway management include endotracheal intubation, laryngeal mask airway (LMA), and “open airway.” Open airway refers to techniques in which there is no airway adjunct which provides coverage or blockage of the glottis (laryngeal inlet to trachea and lungs). Nasopharyngeal airways are commonly placed in the open airway technique. General anesthesia can be provided with any of these forms of airway management. The patient may be spontaneously breathing or may require mechanical ventilation, which can only be provided if an endotracheal tube or LMA is used. There is a common misconception that if an endotracheal tube or LMA is used, this determines whether general anesthesia versus deep sedation is provided. The defining characteristic of whether deep sedation or general anesthesia is utilized is level of consciousness and not the type or lack of airway adjunct used.
General anesthesia or deep sedation may be administered in the hospital operating room or emergency department, in ambulatory surgery centers (ASCs), or in the office setting. Deep sedation provided by emergency room physicians in pediatric hospitals is generally limited to very specific indications and will not be discussed here. In the hospital operating room and ASCs, general anesthesia via nasotracheal intubation (see Fig. 10.1a, b) is routinely provided. The nasotracheal route allows the dentist to evaluate the occlusion. For most other surgical procedures, the orotracheal route is used but this does not allow for mouth closure.
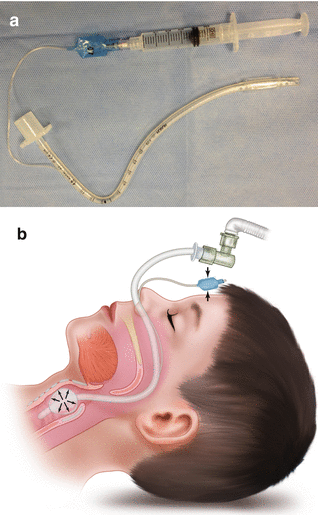

Fig. 10.1
(a) Cuffed nasotracheal tube. (b) Nasotracheal tube in place
To facilitate endotracheal intubation, inhalation induction is commonly provided. In this technique, the child breaths the potent inhalation agent sevoflurane until unconsciousness is attained, an intravenous line is started, nasotracheal intubation is performed, and the patient is maintained on inhalation agents. When treatment is completed, the patient is extubated when awake and transferred to the postanesthesia care unit (PACU). Various intravenous agents such as corticosteroids, antibiotics, neuromuscular blockers, propofol, antiemetics, and/or analgesics may be coadministered. In some hospitals and ASCs, an intravenous line is started while the child is awake with or without the aid of topical skin anesthetics, e.g., EMLA cream, and/or midazolam oral moderate sedation. Intravenous induction is then carried out to facilitate endotracheal intubation prior to potent inhalation maintenance of general anesthesia.
Although the LMA may be used for pediatric dental and oral surgery, it has not found favor in the United States as it has in Europe. When the LMA is used for oral procedures, the “flexible” type is used so the stem may be moved from side to side as needed to facilitate the dental procedure. Clearly, occlusion cannot be assessed as the tube blocks mouth closure (see Fig. 10.2).
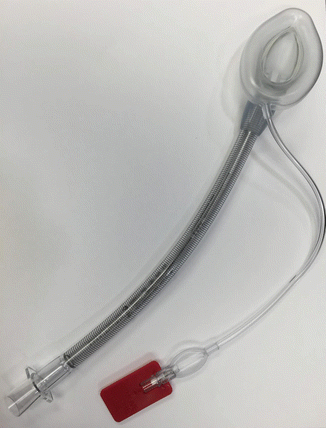

Fig. 10.2
Flexible LMA
In the office setting, either intubated or non-intubated general anesthesia can be utilized, most commonly via a total intravenous anesthesia (TIVA) technique. When an anesthesia machine capable of delivering sevoflurane is not available, as is typical is most dental offices, “induction” is most commonly provided with an intramuscular injection of ketamine and midazolam with or without an anticholinergic, i.e., such as glycopyrrolate or atropine. Common sites of injection include the deltoid and lateral vastus. A state of dissociative anesthesia develops within 2–5 min and allows easy and amnestic separation of the child from the parent with acceptable maintenance of ventilation.
The patient is brought to the treatment room where supplemental oxygen is administered, standard anesthesia monitors are applied, an intravenous line started, and anesthesia is typically maintained with propofol with or without an opioid (commonly alfentanil or remifentanil) via a computer-controlled pump adjusted to an appropriate depth of general anesthesia depending on whether local anesthesia is applied.
Airway management is either via nasotracheal intubation or open airway. In the more common open airway technique, supplemental oxygen is supplied via nasal cannula in the nares. If an airway adjunct is used for this technique, it would be a nasopharyngeal airway placed with the tip in the oropharyngeal to upper-hypopharyngeal region (see Fig. 10.3a, b).
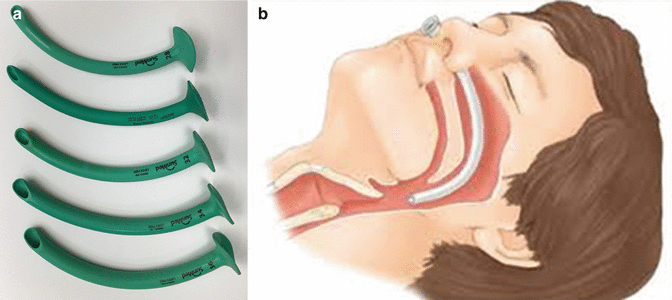

Fig. 10.3
(a) Nasopharyngeal airways. (b) Nasopharyngeal tube in place
The nasal cannula can be cut and placed in the nasopharyngeal airway to deliver supplemental oxygen. Various intravenous agents may also be administered such as corticosteroids, antibiotics, antiemetics, and/or other opioid or non-opioid analgesics. This may be the most common form of dental office-based general anesthesia provided for pediatric dental patients. If local anesthesia is used for treatment, then a lighter plane of anesthesia, such as that approaching ultralight general anesthesia, may be adequate. Although deep sedation can be utilized for children undergoing dental procedures with the open airway technique and adequate local anesthesia, intermittent periods of movement common with this technique are generally not viewed favorably by either dentists or their anesthesia providers. What is termed “deep sedation” in the pediatric setting would better be termed “ultralight general anesthesia,” even when local anesthesia is used in the oral cavity. Deep sedation may be effectively employed, however, for short oral surgical procedures such as tooth extraction.
Intubated office anesthesia can also be easily accomplished. If no anesthesia machine capable of delivering sevoflurane is available, intramuscular (IM) induction as above takes place, monitors are placed, and an intravenous (IV) line is started. Unconsciousness, profound analgesia, and apnea are obtained, most commonly with a combination of propofol and remifentanil; intubation is carried out and a Mapleson circuit (typically a Mapleson D or Jackson-Rees design) or a circle system with a transportable carbon dioxide absorber is used to deliver supplemental oxygen. Once resumption of ventilation takes place, maintenance of anesthesia is via TIVA as for the open airway technique. Extubation may be done “deep” (i.e., while unconscious) or awake.
In all of these techniques, supplemental oxygen is provided with either the dental nitrous oxide-oxygen delivery system or via E cylinders of oxygen. If nitrous oxide is used, attention must be directed to proper scavenging to limit environmental exposure. For anesthesiologists who utilize a portable anesthesia machine delivering sevoflurane, inhalation induction can take place. Anesthesia can be maintained with the TIVA intubated or non-intubated technique discussed above. Alternately, inhalational maintenance via an endotracheal tube may be employed as discussed in the hospital/ASC section above, provided that proper gas scavenging can be provided.
It should be noted that for some children 8 years or older, a full anesthesia facemask can be used to administer nitrous oxide 40–70 % in oxygen, with or without midazolam PO, in order to obtain IV access. This is frequently quite effective for painless and often amnestic placement of an intravenous line with subsequent intravenous induction of general anesthesia.
Monitoring
Monitoring for general anesthesia and deep sedation is more intensive than that required for moderate sedation. In addition to continuous blood pressure readings at least every 5 min and continuous pulse oximetry and pulse rate monitoring, continuous electrocardiography and ventilation monitoring is required. Ventilation may be monitored via either nasal cannula end-tidal CO2 and/or precordial/pretracheal stethoscope for open airway cases. For intubated or LMA cases, end-tidal CO2 monitoring is used and may be supplemented with precordial/pretracheal stethoscope.
Temperature monitoring is required when triggering agents for malignant hyperthermia are used (potent inhalation anesthetics and succinylcholine). Routine use of temperature monitoring is helpful for determining intraoperative hypothermia, which is common during prolonged procedures under general anesthesia. When neuromuscular blockers are used for paralysis, nerve stimulators (aka “twitch monitors”) are used to determine degree of paralysis and return of normal neuromuscular function. Glucometers for regular blood glucose monitoring are mandatory for diabetic patients. More advanced invasive cardiovascular monitoring and other special monitors are used in specific clinical situations mainly in hospital operating rooms.
Anesthesia Providers
Various anesthesia providers deliver anesthesia in all the settings noted above. Dentist anesthesiologists provide the majority of dental office-based anesthetics for dentistry. Physician anesthesiologists, with or without the aid of certified registered nurse anesthetists (CRNAs) or anesthesiology assistants (AAs – physician assistants who complete 24–30 months of training post baccalaureate degree), provide the bulk of hospital-based general anesthetics. With the increasing development of “Dental Surgery Centers,” i.e., accredited ASCs dedicated to dental and oral surgery, both dentist and physician anesthesiologists, with or without CRNAs or AAs, are commonly found in these settings.
Nurse anesthetists often require direction by an anesthesiologist or supervision by a surgeon, usually a physician. All physician surgeons get training in presurgical medical evaluation of patients requiring general anesthesia, but most dentists do not. Therefore, most states require that dentists providing dental/oral surgical treatment to have a general anesthesia permit to supervise a nurse anesthetist providing deep sedation or general anesthesia in the dental office. This is not a universal requirement, and in some states nurse anesthetists are allowed to practice without supervision. However, should an adverse event occur, the liability of the dentist in this scenario is less clear than if a dentist or physician anesthesiologist was present.
Dentist anesthesiologists must complete 3 years of dedicated anesthesia residency after graduation from dental school. Accredited Dental Anesthesiology Residency programs, as per the Commission on Dental Accreditation, are the only anesthesia training programs that require outpatient dental anesthesia experience and specifically office-based experience. Additionally, these programs have arguably the most rigorous clinical pediatric patient requirements of any of the anesthesia providers (at least 125 children aged 7 or under) except for pediatric physician anesthesiologists. This is also true for patients with special needs (see Table 10.2; http://www.ada.org/~/media/CODA/Files/anes.ashx).
Table 10.2
Training requirements in overall months and for pediatrics for general anesthesia providers and oral surgeons
|
Anesthesia provider
|
Months in DS/GA training (minimum/usual)
|
Number of children required
|
Ages
|
Number of pts. with special needs required
|
Office-based experience required
|
|---|---|---|---|---|---|
|
Dentist anesthesiologist
|
24/31
|
125
|
≤7 years
|
75
|
Yes
|
|
Physician anesthesiologist
|
30/32
|
100 total
75
20
5
|
<12 years
<3 years
<3 months
|
No special requirement
|
No
|
|
CRNA
|
24/24
|
35 total
25
10
|
2–12 years
<2 years
|
No special requirement
|
No
|
|
Oral surgeon
|
6/6
|
50
|
≤18 years
|
No special requirement
|
Yes
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


