Child’s status
Age
Cognition
Emotional responses
Behaviors in clinic
Dental needs
Intervention
Infant
Birth – 1 year
Basic receptive andexpressive language
Calm
Quiet
Degrees and intensitiesof crying
Social smile
Grimacing
Sitting up
Crawling
Likely extraction of natal/neonatal teeth
Trauma
Topical anesthesia
General anesthesia
Toddler
1–3 years
Rapidly evolving
Language acquisitionand purposeful use
Calm
Quiet
Laughter
Crying to screaming
Pouting
Anger
Joy
Surprise
Shyness
Smiles appropriately
Crying and temper tantrumin response to frustration
Social adaptabilityor maladaptation
Clumsy locomotion and coordination
Kicking
Hitting
Caries
Trauma
Short TSD
Distraction
Positive reinforcement
Rewards
Sedation (usually moderate to deep)
General anesthesia
Preschooler
3–6 years
Language skills rapidly progressing
Speaks what he/she hears
Imagination and magic dominate
Calm
Quiet
Laughter with purpose
Crying with purpose
Anger
Sadness
Recognition of others’emotions
Smiles
Cries
Kicking
Hitting
Spitting
Obstinacy
Caries
Trauma
Space maintenance
TSD
Distraction
Positive reinforcement
Rewards
Voice control
Nitrous oxide
Mild to deep sedation
General anesthesia
Primary school
6–12 years
Language skills approaching adult levels
General compliance with authority figures(e.g., teachers) begins to dominate
Calm
Quiet
Laughter with purpose
Crying with purpose
Anger
Sadness
Compassionate
Interactive
Smiles
Cries
Obstinacy
Moody
Cooperative
Caries
Trauma
Space maintenance
Orthodontics
TSD
Distraction
Positive reinforcement
Nitrous oxide
Mild to moderate sedation
High schooland teenagers
13–19 years
Adult cognition
Calm
Quiet
Laughter
Moody
Anger
Avoidance
Challenging
Peer orient
Smiles
Obstinacy
Moody
Cooperative
Caries (rampant)
Trauma
Space maintenance
Orthodontics
Tobacco-related periodontal issues
TSD
Distraction
Positive reinforcement
Nitrous oxide
Mild to moderate sedation
Since children may exhibit a variety of behaviors that are not compatible with a smooth, collaborative interaction desirable in a clinician–patient relationship, negative consequences may occur. The most simple and often most tragic consequential behavior of a “bad dental experience” is the patient’s future avoidance of the dental environment. In classical reinforcement theory, avoiding a potentially fearful or negative situation is actually reinforcing or “pleasurable.” Hence, avoidance behaviors are likely to increase in the future.
Disruptive Behaviors in the Dental Operatory and Their Causes
The disruptive behaviors best known and witnessed by the experienced clinician in managing children are vocalizations, movements, and “delay”-designed tactics (see Box 2.1). The vocalizations vary from normal speech to types of crying (viz., sobbing, whimpering, and loud crying), to frank and painful ear-piercing screams. Movements include, among others, covering the face, attempts to strike out at others (whether real or “shadow boxing”), grabbing the clinicians’ arms and instruments inappropriately, biting, displaced aggressions toward the immediate family caregiver, repeated kicking of the legs and/or feet against the dental chair, or integrated active attempts to escape from the chair and operatory. Procedurally related delay tactics also may be present. In this case, the child will make statements, like “wait, wait, wait!!!,” “I have to tell you something,” “I have to use the bathroom,” or “I can’t breathe,” all of which are designed to delay the procedure.
Box 2.1. Common Disruptive Behaviors in the Dental Operatory
-
Vocalizations
-
Sobbing
-
Whimpering
-
Loud, controlled crying
-
Ear-piercing screams or yelling
-
Delay tactics
-
-
Movement
-
Grabbing arms or hands of dental team members
-
Hiding their face
-
Repeated kicking of heels against dental chair seat
-
Swinging of arms (shadow boxing)
-
Frank attempts to escape from dental chair
-
-
Others
-
Biting
-
Scratching
-
Spitting
-
Cursing
-
These behaviors may be frustrating for the dental team and, in the less experienced practitioner, may elicit negative feelings toward the child. Such feelings may even impact the quality of care delivered. Ignoring or not responding to the child’s pleadings, once appreciated as a delay tactic, actually is known in behavior modification theory as “extinguishing” the response (i.e., typically, the response rate decreases). One should appreciate that these types of behaviors are usually in response to dental stimuli and procedures, some of which may be perceived as unpleasant to a patient who is awake (see Table 2.2).
Table 2.2
Dental stimuli that may trigger pain, anxiety, and uncooperative behaviors
|
Potential provokingprocedures
|
Key considerations
|
|---|---|
|
Injection of localanesthetic
|
Sites of painful injection
Anterior maxillary infiltration
Palatal infiltration
Inferior alveolar injection
Long buccal and mandibular infiltration
Rate of solution administration
Extraneous maneuvers
Soft tissue vibration/movement
|
|
Application ofrubber dam clamp
|
Inadequate soft tissue anesthesia
Intrasulcular pressures
Incorporated soft tissue
|
|
Tooth preparation
|
Transmitted auditory sounds
Inadequate nerve blockage with local anesthetic
Vibratory sensations
|
|
Crown placement
|
Pressure during placement
Inadequate anesthesia
Intratubular pressures
|
|
Elevation andextractions
|
Pressures
Inadequate anesthesia
Encroachment on unanesthetized tissues
Excessive temporomandibular joint movement
|
Cooperation refers generally to the child and provider interacting in a bidirectional fashion that is mutually supportive and beneficial. The process in which this occurs depends on such factors, among others, of timing, goal orientation, and personality characteristics of the two parties. Children may smile, listen intently, and wish to undergo the process with eagerness and ease. Some children are overtly shy and take longer to accept the explanations. Others frankly refuse to participate in cooperative interactions, sometimes issuing spine-tingling screams and escape movements that can become dangerous to both parties.
The concept of personal intrusiveness is also an important, but a rarely discussed consideration. One can appreciate that every individual has a “psychological space” within which the individual feels comfortable with his/her surroundings and situation (Fig. 2.1). This imaginary space can manifest both as a physical distance from one’s face and a psychologically sphere that includes an emotional comfort zone when one interacts with another person. Intrusiveness refers to a sense of one’s perceptions and feelings generated by another person who has, to some degree, physically or psychologically invaded this psychological space. More likely than not, the intrusion causes the individual some internalized distress possibly resulting in defensive responses. Children, for example, may turn their head, raise their hands, and protest by pushing away a doctor-guided, approaching nasal hood used for delivering nitrous oxide. Even basic techniques such as tell-show-do, as conveyed by the dental team, may not be sufficient to overcome the defensive reactions of the child in these circumstances.
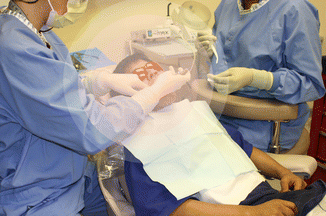

Fig. 2.1
Photograph illustrating an example of the “psychological space” surrounding a person. The variably colored spheres around the patient’s head indicate that the size of the individual’s psychological space may change depending on social and environmental settings. For example, the size of the space may be expected to be much larger when in the presence of a stranger versus that of a family member. Intrusion by another person into an individual’s space may cause the individual to experience anxiety and react in unexpected ways
Consequently, the dentist may function as a chairside psychologist who is exquisitely aware of each child’s range of capabilities in expressing a multitude of responses in the dental setting. Repeated experiences, appropriate training, and dedication provide a basic platform for management techniques and skills necessary for the chairside psychologist. Nonetheless, the amount of effort invested in managing this wide expression of behavior is often physically and emotionally exhausting at the end of the day.
Is there a way to preoperatively characterize and, better yet, identify these challenging children? Not always, but some child characteristics have been investigated or empirically noted as prominent features that aid in anticipating disruptive behaviors. For instance, children who may be challenging are very young (i.e., 3 years of age or less); generally lack well-developed effective social and intrapersonal coping mechanisms; are temperamentally distressed and shy; suffer from fearful, anxious, or angry states, of which they cannot easily control; are mentally or cognitively challenged; or have chronic physical illness requiring frequent medical challenges sometimes involving unpleasant interventions. Unfortunately, many of these “challenging” children may also have dental caries; others may have suffered orofacial trauma, both of which likely require procedural interventions.
Age
A child’s age and cognitive development are helpful in predicting the likelihood of disruptive behaviors associated with dental procedures. As a general rule of which there are exceptions, children who are 3 years of age or less may be expected to have a short attention span, be fearful of strangers, or lack sufficient cognitive and language skills, all of which can contribute to unfavorable reactions in the dental setting. Often, the primary coping responses of these toddlers are crying, expectations of immediate parental protective intervention, and avoidance behaviors. As the child approaches school age, the fear of strangers may subside, language and communication skills become more effective, and subtle socialization gains including better emotional control often become apparent. Once children are of school age, changes in cognition are notable. This developmentally cognitive and emotional growth often translates into fewer incidences of disruptive behaviors. Again, exceptions to this expected developmental change can and do occur.
From a sedation perspective, one can anticipate that toddlers will likely require deeper levels of sedation creating less opportunity for effective behavioral guidance in obtaining successful procedural outcomes. But as the child’s age and cognitive/emotional states mature, the depth of sedation targeted may generally ebb more toward a need for only minimal to moderate depths of sedation along with a heavier emphasis on behavioral guidance.
Role of Anxiety and Fear
There are many factors associated with disruptive, uncooperative behaviors exhibited in the dental setting by children, but anxiety and fear likely top the list. The prevalence of anxiety and fear of children in the dental setting has been estimated as ranging from 6 to 20 % [9, 12]. That’s probably an underestimate.
In one review, fear and anxiety reportedly were more prevalent in the youngest of children decreasing with age, are associated with gender, and temperamental traits were notable. Temperamental characteristics of shyness, negative emotionality, poor adaptability, and high activity and intensity were consistent with anxiety and fear. Anxiety and fear are often thought to be the predominant states underlying many of these expressions of behavior. However, as pointed out by others, dental fear does not necessarily equate to the primary cause of disruptive behaviors, and such uncooperative behaviors do not necessarily imply that dental fear is the culprit [12].
Anxiety and fear cause a complex range of emotional behaviors. Recent neurobiological evidence has evolved aiding in the understanding of these states. Apparently, fear-elicited response patterns in the human are mediated primarily and initially in the limbic system of the CNS and, more specifically, in the area of the amygdala of the midbrain [13–15]. This system is genetically geared to rapidly assess impending danger and, within microseconds, initiate and orchestrate a pattern of motor, emotional, and autonomic responses designed specifically to protect the organism. Furthermore, the system seems particularly sensitive to and organized in such a way as to memorize and categorize each threatening situation in an attempt to prepare the organism for future encounters. Toxic stress likely plays an influencing factor on this system.
Behavioral inhibition has been described as a temperamental trait of young children who tend to withdraw from novel or unfamiliar stimuli [16–18]. Inhibited behaviors, such as avoidance of novelty, represent a coping mechanism by which the fearful reaction is decreased. Over time, coping with fear through avoidance is thought to reinforce the associated physiological responses and behaviors leading to continued behavioral inhibition and social wariness: a positive reinforcement cycle. Interestingly, it has been hypothesized that temperament types may be associated with different response sets within the limbic system.
Parenting and Environmental Influences
Evidence of change manifested as generational differences in parental management styles is associated with disruptive behaviors of children in the dental setting. Pediatric dentists are reporting that today’s children are less cooperative, cry more, and are more disruptive in response to normal guidance techniques than children of a decade or more ago [19]. In order to address these changes, evidence is slowly accumulating suggesting a movement toward greater use of pharmacological management of children than has been done in the past.
Key Concepts of Behavior Associated with Sedation
Temperament
Temperament describes a child’s overt responses as a basic and daily expression pattern to solitary and social situations. Temperament is believed to have a fairly strong genetic component and is somewhat stable over different situations and developmental phases of an individual’s life. Some children may appear shy, withdrawn, irritable, and moody, whereas others may be friendly, approachable, euphoric, and pleasant during initial interactions with other children or adults.
There is fairly consistent and widespread evidence that temperament affects how children tend to respond in dental as well as other settings [20–22]. In fact, a child’s temperament may aid in predicting, to a certain degree, how the child may respond while under the influence of therapeutic doses of sedatives and during perioperative periods surrounding general anesthetics [23–26]. Some authors have concluded that shy, withdrawn children do not behave as well compared to peers who are less shy and withdrawn [27].
Attachment
Attachment is another psychological concept wherein the presence and strength of emotional bonds to caregivers affect a child’s response in different contextual situations. Evidence suggests that attachment may have implications for one’s health and behaviors. Relationships between attachment and temperament have been reported, but the strength of these associations is not well understood. The interactions between the two concepts appear complex [28–30]. Attachment per se has not been studied in pediatric dentistry as of this writing.
Age
The patient’s age and corresponding cognitive development are important considerations for anticipating different expressions of behaviors in children during dental procedures [31]. Generally speaking and in terms of broad classifications of patient age, the young preschoolers seem to have a higher likelihood of displaying disruptive and uncooperative behaviors [32]. Disruption and uncooperative behaviors usually wane as children age; however, traumatic episodes or series of such episodes may increase the expression of these behaviors. Some school-aged children and adolescents may actually regress and display an unwillingness to participate in dental procedures.
Another important factor of consideration associated with aging and cognitive development of youngsters, albeit not documented in any systematic fashion in dentistry, is language acquisition and its understanding and use [33]. Its importance, as a bridging mechanism for communication between the patient and provider, cannot be overstated and forms the basis of the popular technique of tell-show-do. Sedation of infants and toddlers, who may lack sufficient language skills to understand procedural interventions, is a well accepted and frequent adjunct for many types of medical procedures, thus recognizing the immature state of coping mechanisms characteristic of these very young children.
As children age and their personality begins to congeal, individualized traits and styles of interaction with others become more observable and predictable even into adulthood. Some individuals will have general as well as specific types of traits associated with potential anxiety or fear-provoking situations. The interaction of general and specific qualities in children is complex and not always intuitive. Evidence does suggest that procedural-evoked anxiety can be favorably modified through appropriate interventions. Thus, the astute clinician should make efforts to gain information from parents and guardians in anticipating patient anxieties and fears that may become manifest during dental procedures. Furthermore, the clinician should have a repertoire of interventions whose implementation may lessen these emotionally charged states.
Experience
Children’s experiences with the medical field begin very early in life. Even infants learn quickly and express anguish during routine visits to the physician in anticipation of inoculations. Depending on the general health and incidences of traumatic episodes children may endure, those experiences may be well tolerated or induce a lifelong stigma possibly leading to unwanted avoidance behaviors of medical and dental needs. Family member’s support or hurtful exacerbation (e.g., teasing) of anticipated experiences of planned procedures also may impact the outcome and contribute to the processes of internalizing coping skills of the child. For example, parental or sibling comments such as “next comes the painful shot” sometimes have deleterious effects even if not consciously intended. It is even possible that some degree of discussion about the “shot” has already occurred at home. Either way, these remarks heighten the child’s sense of anticipatory dread of the procedure which at the time of occurrence may immediately overflow into an outburst of disruptive and uncooperative behavior.
Parenting
Parents are usually a beneficial source of knowledge about their children and how they may respond during procedures and interactions with professionals. Generally, parents know the child’s behaviors, limits, adaptive skills, and emotional responses quite well. They are an obvious benefit to the professional who takes the time to understand the parent’s perspective; acts in a caring professional manner when explaining expectations, techniques, procedural processes, and possible outcomes; and gains parental confidence in managing their child’s situation. Parental knowledge of the child’s medical and social history and insights regarding their child’s typical responses in a host of settings is invaluable.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


