The purpose of this article is to review the common neoplasms, infections, and inflammatory dermatoses that may present around or near the mouth. Dental professionals are well positioned to evaluate perioral skin conditions, further contributing to patients’ general health. This article includes a review of seborrheic keratosis, warts, actinic keratoses, actinic cheilitis, and squamous cell carcinoma, among several other perioral cutaneous lesions.
Key points
- •
Neoplasms, infections, and inflammatory dermatoses may present around or near the mouth.
- •
Dental professionals are well positioned to evaluate perioral skin conditions.
- •
Early recognition and treatment of perioral lesions and dermatoses provide best clinical outcomes.
Introduction
The purpose of this article is to review the common neoplasms, infections, and inflammatory dermatoses that may present around or near the mouth. Dental professionals are well positioned to evaluate perioral skin conditions, further contributing to patients’ general health. This article includes a review of seborrheic keratosis, warts, actinic keratoses, actinic cheilitis, and squamous cell carcinoma, among several other perioral cutaneous lesions.
Introduction
The purpose of this article is to review the common neoplasms, infections, and inflammatory dermatoses that may present around or near the mouth. Dental professionals are well positioned to evaluate perioral skin conditions, further contributing to patients’ general health. This article includes a review of seborrheic keratosis, warts, actinic keratoses, actinic cheilitis, and squamous cell carcinoma, among several other perioral cutaneous lesions.
Seborrheic keratosis
Introduction
Seborrheic keratoses are very common and usually multiple, presenting as oval, slightly raised, tan or light brown to black, sharply demarcated papules or plaques that usually measure less than 3 cm in diameter.
Cause
The pathogenesis of seborrheic keratosis is unknown. In about one-third or more of cases, mutations in FGFR3 and PI3K have been implicated. Advanced age is a well-established risk factor, although the relationship between seborrheic keratosis and sun exposure has been debated.
Epidemiology
The age of onset usually falls within the fourth to fifth decade, and males and females are equally affected.
Prognosis
These lesions are benign with no risk of malignant transformation.
Clinical Features
Seborrheic keratoses have a characteristic stuck-on appearance and are often described as waxy and smooth. When removed, the underside of the warty lesions reveals a raw, moist base. Although most are asymptomatic, some lesions cause itching, bleeding, or pain. The chest and back tend to be the primary sites affected; but seborrheic keratosis commonly involves the scalp, face, neck, and extremities. Some patients, particularly Caucasians, may have hundreds of these lesions on the trunk. A variant of the central face, known as dermatosis papulosa nigra , is common in African Americans and Asians.
Because of its classic appearance, the diagnosis of seborrheic keratosis is primarily clinically based. Although the histology does vary, seborrheic keratoses universally show a proliferative process, with hyperkeratosis and acanthosis without dysplasia. Biopsy is rarely indicated unless lesions are difficult to distinguish from melanoma. Clinicians should also be aware that the sudden onset of multiple seborrheic keratoses has been thought to represent a paraneoplastic syndrome from an occult malignancy, such as stomach or colon cancer. However, this phenomenon, known as the sign of Leser-Trélat , has recently been questioned.
Management
As a benign lesion, seborrheic keratosis may be treated electively. The primary indication for surgical removal is cosmetic, though chronic bleeding, irritation, and blistering may warrant treatment. Removal is also considered when the diagnosis is unclear. Shave excision, electrodessication and curettage, and cryotherapy are common surgical options but may be associated with recurrence, scarring, and changes in pigmentation. Consequently, the use of lasers (erbium YAG, carbon dioxide [CO 2 ], and 532 diode) has become more popular. Medical therapies, such as topical and systemic vitamin D, have shown limited efficacy.
Warts
Introduction
Warts (verrucae) are caused by human papillomaviruses (HPVs), small DNA viruses of the papovavirus family, with more than 100 different HPV types being described. Cutaneous lesions often present as small papules, single or multiple, throughout all age groups.
Cause
HPVs are classified according to mucosal and cutaneous types caused by HPV 1, 2, and 4. Planar or flat warts on the face are caused by HPV-3 and 10. Mucosal types are divided into low risk and high risk. Low risk (HPV-6, 11) is defined by never being found in invasive squamous cell carcinomas (SCC), whereas high-risk types, such as HPV-16, 18, and others, are prevalent in this instance.
Epidemiology
Estimates suggest a prevalence of common warts in 3.5% of adults and up to 33% of children. There is an increased incidence in immunosuppressed patients, including those with human immunodeficiency virus (HIV) disease and organ transplantation recipients.
Prognosis
Warts may cause pain or cosmetic distortions; however, treatment may cause similar issues. Regression is often spontaneous, with immune mechanisms playing an important role; however, this is often slow. Although rare, malignant transformation may occur. It is mostly noted in the setting of immunosuppression.
Clinical Features
HPVs demonstrate a variety of mucocutaneous manifestations: common warts, plantar warts, verruca plana, anogenital warts, epidermodysplasia verricuformis, oral warts, condyloma, focal epithelial hyperplasia (Heck disease), nasal and conjunctival papillomas, laryngeal papillomatosis, and cervical lesions.
Common warts typically present as small papules with a verrucous and hyperkeratotic surface, ranging in size from 1 to 10 mm. Although lesions typically occur on the hands and fingers, they may occur in other locations. Periorally, lesions may also appear flat, as verruca plana, or filiform with fingerlike projections ( Fig. 1 ). Histologically, verrucae are characterized by hyperkeratosis, acanthosis, and papillomatosis. Often the edges of the lesions project inward, known as arborization. Tiers of parakeratosis are often noted, with an increased granular cell layer and coarse keratohyalin granules. Koilocytes, cells with a pyknotic nucleus and clear halo, are often but not always noted.
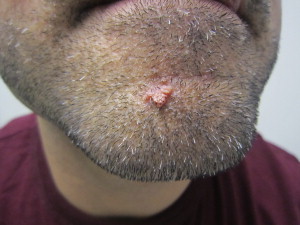
Flat warts are usually multiple, flat-topped, smooth papules, often skin colored. They may regress. Before regression, they may be preceded by an eruption of multiple lesions. Histologically, the features are similar to common warts; however, papillomatosis is mild and parakeratosis is often absent.
Management
The treatment of warts is difficult and failures are common. Multiple treatment options are available, and it is important to note that none are completely effective. Treatments range from observation, because warts may regress spontaneously, to topical therapy, surgical therapy, and even systemic therapies. Topical therapy includes salicyclic acid; cantharidin (an extract from a blister beetle); contact sensitizers, such as squaric acid and diphencyclopropenone, tricholoacetic acid, podophyllin, imiquimod, tretinoin; and the application of duct tape. Liquid nitrogen cryotherapy is a frequently used technique, which may induce blistering.
For more recalcitrant lesions, topical cidofovir, photodynamic therapy with aminolevulinic acid and blue light exposure, 5-fluorouracil, intralesional bleomycin, and intralesional candida antigen can be used. CO 2 , pulsed dye, and Nd:YAG lasers have been used for more resistant lesions. Electrodessication and curettage may be used; however, it has a high risk of scarring.
Systemic oral therapies for multiple and recalcitrant warts have been tried, including cimetidine and oral retinoids. It has been shown that cimetidine activates Th1 cells to produce interleukin 2 (IL-2) and interferon (IFN)-γ, which correlates with wart remission. High-dose cimetidine (30–40 mg/kg/d) has been helpful for recalcitrant warts, although the treatment time is often lengthy, requiring weeks to months of therapy. Vaccines are available currently for low and high-risk types. The vaccines are effective against diseases caused by HPV types 16 and 18. One vaccine additionally protects again HPV types 6 and 11. Vaccination is recommended for females and males aged 9 through 26 years in a series of 3 doses. Of note, the vaccine produces higher antibody titers when given at 11 to 12 years of age compared with older ages.
Facial actinic keratosis
Introduction
Actinic keratoses are scaly, erythematous skin lesions that are induced by UV solar radiation. They are considered a premalignant lesion.
Cause
Besides sun exposure, other risk factors include fair skin, advanced age, male sex, and immunosuppression. The inciting event in the process of photodamage that leads to actinic keratosis is a mutation in the tumor suppressor factor p53 initiated from solar radiation.
Epidemiology
In the United States and Europe, the incidence of actinic keratosis is approximately 10% to 15%. Actinic keratosis is important to recognize because it may progress to SCC in nearly 15% of cases. Actinic keratoses are most common in fair-skinned Caucasian individuals.
Prognosis
The progression of actinic keratosis to squamous cell is variable but may occur within carcinoma and takes approximately 2 years.
Clinical Features
Actinic keratosis is usually diagnosed clinically. Characteristically, the affected areas present as slightly erythematous, rough, scaly macules, distributed on sun-exposed areas of the skin. However, because it is on a continuum with SCC, there are instances when actinic keratosis cannot reliably be distinguished from its malignant counterpart without a biopsy.
Management
The management of actinic keratosis includes medical and surgical therapies. Local-directed approaches include cryotherapy and electrodessication with curettage; field-directed treatment encompasses photodynamic therapy; topical chemotherapeutic agents, including 5-fluorouracil and imiquimod; dermabrasion; and CO 2 laser resurfacing. The most common technique for managing actinic keratosis is liquid nitrogen cryotherapy, although topical chemotherapy using 5-fluorouracil has been shown to be one of the most effective methods. The therapy of choice depends on a variety of factors, such as the number and extent of lesions, patient compliance with medical therapies, surgical experience of the clinician, and previously failed therapies.
Actinic cheilitis
Introduction
Actinic cheilitis is a premalignant lesion of the lips that has the potential to develop into invasive SCC. Caused by solar damage, it occurs more commonly in fair-skinned (primarily Caucasian) individuals.
Cause
Sun exposure, especially among fair-skinned middle-aged to older patients, is the primary risk factor for actinic cheilitis.
Epidemiology
Women are less often affected, possibly because of the protective barrier effects of lipstick.
Prognosis
Actinic cheilitis has similar malignant potential to actinic keratosis, with advanced disease leading to the development of SCC. The presence of actinic chelitis may more than double the risk of SCC. Of note, the risk of invasion and involvement of the cervical lymph nodes is higher in SCC of the lip than that of the skin.
Clinical Features
The lower lip is the most common site of involvement likely because of its direct exposure to sunlight. Clinically, these lesions are multifocal and are most often characterized as dry, atrophic, and scaly. Some patients may present with a blurred demarcation between the lip vermilion border and the skin or marked folds along the lip vermilion. These presentations require careful evaluation including biopsy.
Management
The ultimate goal in the management of actinic cheilitis is preventing UV light–induced skin damage by applying sunscreen when outdoors and reducing sun exposure.
The multifocal nature of the disease makes it difficult to correlate clinical findings with histologic findings. Therapies include those used for actinic keratosis, such as CO 2 laser, cryotherapy, and 5-fluoracil, in addition to vermilionectomy in cases of severe dysplasia.
SCC of the lip
Introduction
SCC of the lip is a common head and neck malignancy. Most lesions occur on the lower lip from the vermillion border.
Cause
SCC of the lip is related to chronic sun exposure. It may be seen in younger individuals who are immunosuppressed. Solar/UV radiation is the most important risk factor, with UVB (290–320 nm) being more carcinogenic than UVA (320–400 nm). Other factors also play a role, including smoking, excessive alcohol use, HPV, race, family and genetic predisposition, immunosuppressive state, poor diet, and socioeconomic situation.
Epidemiology
SCC of the lip has a higher incidence in Caucasian men and primarily affects people greater than 60 years of age.
Prognosis
SCC of the lip is typically considered a disease of low aggressiveness and favorable prognosis because it tends to progress slowly. When diagnosed early, it has a cure rate of 80% to 90% and a mortality rate between 10% and 15%. Metastases tend to occur at a later stage; in these cases, the mean survival in 5 years decreases to 25%.
Clinical Features
Initially, it may be difficult to distinguish from actinic cheilitis because it is often asymptomatic. Lesions present as white or pink atrophic plaques, which may have persistent fissuring, scaling, or crusting. Over time, the lesion may ulcerate, cause pain, and demonstrate infiltration at the base. In more advanced stage, ulcerations with indurated borders persist without healing. Exophytic, verrucous nodules may also be appreciated. It is helpful to palpate both the internal mucosa and external surface to help identify the true extent of the lesion.
Histopathologically, SCC of the lip is characterized by invasive islands of malignant squamous epithelial cells. The cells are enlarged with hyperchromatic nuclei, an increased nuclear-to-cytoplasmic ratio, and an eosinophilic glassy cytoplasm. Keratin pearl formation occurs, and individual cells may prematurely keratinize. SCC of the lip is characterized as well, moderately, and poorly differentiated. Well-differentiated tumors tend to grow slowly. Poorly differentiated tumors are characterized by atypical mitoses, nuclear pleomorphism, little or no keratinization, and rapid growth. Tumors with characteristics between these are classified as moderately differentiated. Tumor thickness greater than 4 to 5 mm has been shown to be a predictor for developing nodal disease. Perineural invasion has been shown to increase the risk for both local recurrence and metastasis.
Management
Treatment of SCC of the lip without nodal involvement is either by Mohs micrographic surgery, surgical excision, or radiation therapy, depending on the functionality and cosmetic outcomes. Adjuvant radiation therapy should be considered in the setting of close or positive margins to reduce the risk of local recurrence, in the range of 40 to 70 Gy, fractionated. Currently, there is no consensus defining an acceptable surgical margin in cutaneous SCC, ranging from 2 to 4 mm. It is important to note that margin status, including the lip, is a well-documented risk for developing local relapse, thus local adjuvant radiation therapy may benefit in reducing local recurrence. SCC of the lip is considered a higher-risk lesion and has a greater risk of metastasis compared with other cutaneous sites. There is growing evidence showing the prognostic benefits of sentinel node biopsy in high-risk patients with SCC with clinically negative regional nodal disease. Although this has been adopted for cutaneous malignant melanoma, further studies are needed to address its utility in SCC of the lip.
Basal cell carcinoma
Introduction
Basal cell carcinoma is the most common malignancy in man, with more than 2 million cases diagnosed in the United States annually. In most cases, it is very treatable, with a very low risk of metastasis.
Cause
Exposure to sunlight, particularly to UVB radiation, is the primary risk factor for basal cell carcinoma, with regions of higher altitude and closer proximity to the equator exhibiting a greater prevalence. Fair-skinned individuals, such as those of Scandinavian or Irish descent, tend to sunburn easily and are more prone to basal cell carcinoma compared with those with more darkly pigmented skin.
Epidemiology
Basal cell carcinoma composes 75% of all nonmelanoma skin cancers and is responsible for 25% of all cancers diagnosed in the United States. Incidence estimates range from 124 to 849 per 100,000 people per year and has been increasing over the past 2 decades. Most basal cell carcinomas are identified between the ages of 40 and 60 years, with a male-to-female ratio of 2:1. Risk increases substantially with advancing age, although an increasing number of younger people are presenting with basal cell carcinoma, presumably caused by sunbathing.
Prognosis
Basal cell carcinomas are slow growing, ranging from a few millimeters to several centimeters in diameter. They rarely metastasize and, thus, are associated with low mortality. However, they have the potential to cause significant morbidity through local invasion and subsequent loss of function and disfigurement. Therefore, appropriate and timely diagnosis and management is essential. Lesions suspicious for basal cell carcinoma should be biopsied. The type of biopsy—shave, punch, or complete excision—depends on the size and architecture of the lesion. Any pigmented tumor suspicious for melanoma always warrants a full-thickness biopsy.
Clinical Features
Basal cell carcinoma arises from the keratinocytes of the epidermis, hair follicles, and eccrine sweat ducts. Basophilic cells with large nuclei are observed histologically, and 5 major patterns are recognized: nodular (21%), superficial (17%), micronodular (15%), infitrative (7%), and morpheaform (1%). Nearly 40% of all cases exhibit a mixed pattern of 2 or more subtypes. Clinically, the nodular subtype most commonly presents as a pearly pink or white, dome-shaped papule that develops sizable telangiectasias with growth. There is a predilection for the head and neck areas, most commonly the nasal tip and ala followed by the cheeks and forehead. Other nodular forms can present as blue, brown, or black on account of melanin accumulation, mimicking melanoma. If left alone, these lesions can reach a large size and be locally destructive to areas like the nose, eyelid, ear, or lip, leaving a significant ulcer (rodent ulcer). Micronodular and infiltrative basal cell carcinomas are are more aggressive and have a higher risk of recurrence. Superficial basal cell carcinoma occurs most commonly on the trunk and extremities, although they have been reported on the head and neck. It features a scaly plaque similar to eczema or psoriasis, but it also has pearly raised borders similar to the nodular type. Morpheaform basal cell carcinoma may resemble a scar or localized scleroderma in that it is an indurated, ill-defined, ivory lesion sometimes with overlying telangiectasia. It is known for its subclinical spread and high recurrence rate following treatment.
Management
When diagnosed early, basal cell carcinoma can be removed by one of several methods. Surgical excision is the most common treatment, although electrodessication and curettage or cryosurgery may also be used. Radiation therapy and topical agents like imiquimod and fluorouracil are used in some cases. Mohs micrographic surgery is the most effective therapy and has a recurrence rate of less than 1% after 5 years, compared with 5% for surgical excision. However, Mohs is usually reserved for more invasive subtypes (micronodular, infiltrative, and morpheaform); high-risk locations, such as the nose, eyelids, and ear; as well as for recurrences given its cost. Regardless of the treatment used, all patients with basal cell carcinomas require follow-up to monitor for the development of new tumors and for recurrence at the treated site.
Labial melanotic macule
Introduction
A labial melanotic macule is a benign pigmented lesion on the lip that arises secondary to increased melanin within basal layer keratinocytes and melanocytes.
Cause
Labial melanotic macules may result from racial pigmentation or they may be idiopathic.
Epidemiology
Females present more commonly than males, and the highest incidence is reported during the fifth decade.
Prognosis
Unlike ephelides (freckles), melanotic macules do not darken with exposure to solar radiation. Multiple lesions are rare unless associated with systemic syndromes, such as Peutz-Jeghers and Laugier-Hunziker syndromes, or endocrine disorders such as Addison disease, McCune-Albright syndrome, hyperthyroidism, and Nelson syndrome.
Clinical Features
A labial melanotic macule is characterized as a tan-brown, irregular macule with well-defined borders on the cutaneous or mucosal lip that usually measures less than 1 cm ( Fig. 2 ). Labial lesions almost exclusively affect the lower lip. The central lip is the most common site, and some cases may involve the vermilion border. Although often darkly pigmented, labial melanotic macules are evenly pigmented with a uniform pigment network. Furthermore, they tend to remain stable over time. Although a labial melanotic macule may occasionally be difficult to differentiate from melanoma clinically, the former does not show any significant increase in melanocytes histologically.
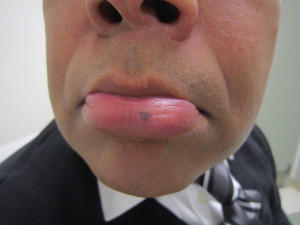
Management
Treatment is unnecessary because this lesion is without malignant potential. For elective removal, cryotherapy, laser therapy, and surgical excision may be used.
Nevi
Introduction
A nevus is a benign proliferation of melanocytes. Nevi are divided according to their histology—junctional, compound or intradermal proliferation of melanocytes—or by their appearance—halo or blue.
Cause
Nevi may be congenital (present at birth or acquired in the first year of life) or acquired. Nevi arise from the neural crest and migrate during embryonic development to their final location in the brain, eyes, and skin.
Epidemiology
Common acquired melanocytic nevi are the most frequent neoplasms in Caucasians. They develop in children even in the first years of life, and their number increases continually into adulthood. Melanocytic nevi develop predominantly in childhood and adolescence. Studies demonstrate that sun exposure at a young age promotes the development of melanocytic nevi. When children grow up in sunny climates, the number of nevi on sun-exposed skin is increased. High, intermittent UV exposure also promotes the development of a greater number of melanocytic nevi, along with sunburn. Genetic factors also play a role, including somatic mutations of the RAS and RAF genes.
Prognosis
The number of common melanocytic nevi represents an independent risk factor for the development of melanoma. With greater than 50 nevi, the melanoma risk is increased by about a factor of 4 to 5. Because the number of nevi impacts the risk of melanoma, this indicates the importance of UV light for the development of melanoma. Freckles are associated with a greater number of nevi. Children with fair skin (Fitzpatrick types I and II, which are defined as skin that “always burns, does not tan” and “burns easily, tans with difficulty,” respectively) have significantly more nevi than those with darker skin.
Clinical Features
Junctional melanocytic nevi are round or oval macules with brown pigmentation, regular in color and contour. Compound nevi are round to oval, flat papules with light to dark brown pigmentation ( Fig. 3 ). Dermal melanocytic nevi usually present as flesh-colored nodules with a smooth surface, usually dome shaped, but papillomatous and pedunculated forms also exist.
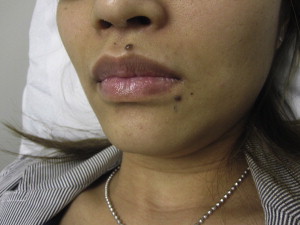
Histologically, nests of melanocytic cells are found at the dermoepidermal junction for junctional nevi. Compound nevi have additional nests and cordlike nevus cell formations in the dermis, whereas intradermal nevi no longer have melanocytes along the dermoepidermal junction.
A congenital melanocytic nevus is a melanocytic nevus that is present at birth or within the newborn period. It is a hamartoma of melanocytes derived from the neural crest. It is categorized as either small (<1.5 cm), medium (1.5 to <20 cm), or giant (>20 cm). Giant congenital melanocytic nevi affect a substantial portion of an anatomic region and do have an increased risk of developing melanoma. Congenital melanocytic nevi present as homogeneous light to dark brown pigmented macules or plaques with sharp borders, a smooth surface, and increased hair. They increase in size proportionally as the skin grows. As lesions age, they may have an irregular surface or have their pigment lighten. Some larger lesions may display color variations with darker areas.
Atypical or dysplastic nevi are those that are larger, have irregular borders, and variable pigmentation. Originally described in association with familial melanomas, it was later recognized that these nevi appear in individuals from nonmelanoma families. The clinical criteria for atypia in melanocytic nevi overlap with the ABCD rule for early melanoma (A, asymmetry; B, border; C, color; D, diameter). Dermoscopy, a noninvasive examination of the skin with a magnifier and a nonpolarized light source, can play an important role in identifying atypical melanocytic lesions and assist in differentiating benign versus malignant lesions. Additionally, the ugly duckling sign has gained importance in the differentiation from melanoma. In this instance, a pigmented lesion is suspicious for melanoma if that lesion is distinctive and dissimilar relative to the patient’s other nevi.
Management
The most important goal of surgical treatment of melanocytic nevi is the histologic differentiation from melanoma. Whether or not to excise melanocytic lesions depends on the risk of developing into melanoma. Because this may be difficult clinically at times, an excision is indicated for diagnostic purposes.
Melanoma
Introduction
Melanoma, a malignancy that develops from melanocytes either de novo or from within a nevus, is an important public health issue throughout the world, including the United States. A melanoma may present as a changing mole or a new dark brown or black macule, papule, or nodule. Diagnosing melanoma early is of utmost importance because the primary treatment modality is surgical excision.
Cause
The causes of malignant melanoma have not been fully elucidated; however, multiple risk factors have been identified, including brief, intense exposure to UV light (UVA 315–400 nm), environmental exposures, skin type, the presence of nevi, and genetic mutations.
Exposure to the sun is the most important environmental cause of melanoma, with the UV radiation being most associated with development of the disease. There is a documented role for UVA radiation inducing carcinogenesis. In light-skinned populations, tanning beds have become the main nonsolar source of exposure to UV light. Multiple studies over the past 30 years show that the risk of melanoma is increased by 20% for those who ever used indoor tanning.
Acquired melanocytic nevi are important markers for the risk of melanoma development, with the total number of melanocytic nevi on the whole body being the most important independent risk factor. Additionally, the presence of dysplastic nevi is an additional independent risk factor for the development of melanoma. The development of potential precursors to melanoma, such as dysplastic nevi, is inhibited by the regular use of sunscreen. Sun protection at an early age may lower the subsequent risk of melanoma.
Approximately 10% of melanomas occur in familial clusters. There is a relationship between a prior personal or family history and melanoma risk. Mutations have been identified in 2 high-penetrance susceptibility genes, the cyclin-dependent kinase inhibitor 2A (CDKN2A) on chromosome 19p21 and cyclindependent kinase 4 (CDK4) on chromosome 12q14. Mutations in CDKN2A account for approximately 20% to 40% of hereditary melanoma and 0.2% to 1.0% of all melanomas. In a more recent study, the melanocortin 1 receptor gene, which encodes the melanocyte-stimulating hormone receptor and determines pigment development, has been identified as a low penetrance melanoma susceptibility gene. Thus, the inability to tan is also associated with an increased risk of melanoma.
Epidemiology
The incidence of melanoma has been increasing faster than that of any other cancer in the United States. Each year, melanoma is diagnosed in more than 70,000 Americans. At current rates, the lifetime risk of developing invasive melanoma is 1 in 52 overall, 1 in 38 for Caucasian men, and 1 in 56 in Caucasian women. In the United States, melanoma is more common in men than in women overall; however, more recently, incidence seems to be increasing in younger women possibly because of increased tanning bed use. The incidence of melanoma also differs between races, with a lower incidence in nonwhite populations.
Prognosis
The prognosis is usually good for thin melanomas; however, greater thickness and advanced-staged melanomas have a much lower 5-year survival. Metastatic melanoma has a well-known predilection for distant spread, with a median survival time of 6 to 9 months. In advanced regional disease, it commonly metastasizes hematogenously to other skin regions, soft tissues, the lung, the liver, and the brain. Lungs are the second most common sites of metastatic disease, after lymph node involvement.
Clinical Features
Cutaneous melanoma can have a variety of clinical appearances, either occurring de novo or within preexisting melanocytic nevi, often with a change in clinical appearance. Early lesions are often characterized by a macule or plaque with different hues (brown, black, blue, red, or white) or occasionally as an ulceration that does not heal. Pigmented cutaneous lesions can be initially evaluated using the ABCDE acronym (asymmetry, border irregularity, color variegation, diameter, and evolving lesions). Not all melanomas present with all 5 features, and it is the combination of the different ABCDE parameters that makes a cutaneous lesion suspect for melanoma.
The anatomic distribution differs by sex and age. In men, they are commonly located on the trunk (55%), especially the back (39%). In women, 42% of melanoma lesions were localized to the lower extremities, with 24% on the lower leg. Lentigo maligna melanoma, a variant more common in the elderly, has a predilection for the head and neck.
Melanoma is diagnosed by skin biopsy. Excisional biopsy with a 1- to 2-mm margin of adjacent normal-appearing skin is the preferred technique for cutaneous lesions suspicious for melanoma. This technique allows the entire lesion to be removed while providing important prognostic information for staging.
Four major clinical subtypes of melanoma have been described: superficial spreading melanoma, nodular melanoma, lentigo maligna melanoma, and acral lentiginous melanoma. Superficial spreading melanoma is the most common subtype, accounting for 50% to 80% of all melanoma diagnoses. Although they can arise from a precursor nevus, most occur de novo. Clinically, a superficial spreading melanoma appears variegated with a sharply marginated, irregular border. Multiple hues and shades are often noted. Histopathologically, there are pagetoid and nested epithelioid melanocytes cells in the intraepidermal portion with poor circumscription.
Nodular melanoma composes 20% to 30% of cases and is more common in men. Typically, they are found on the trunk and are thickened dark brown or black papules.
Lentigo maligna melanoma commonly occurs in older individuals with sun-damaged skin. It has a predilection for sun-exposed areas, such as the nose, malar region, temple, forehead, neck, and forearms. It presents as a slowly enlarging patch that is flat and variably pigmented with tan, brown, and black colors. It is typically asymmetrical with irregular borders. Transformation is slow, often taking 10 to 50 years before invasive growth becomes apparent.
Acral lentiginous melanoma, the least common subtype, accounts for less than 5% of all melanomas. This subtype accounts for 70% of melanomas seen in African Americans and occurs on hairless areas like the subungual, palmar, and plantar regions. Clinically, a variably colored macule develops irregular borders and variegated pigment, usually brown or black, and increases in size over time.
Staging of melanoma is based on the tumor, node, metastasis (TNM) staging criteria. The TNM categories described by the American Joint Committee on Cancer consider histopathologic factors, such as primary tumor thickness, ulceration status, and rate of mitosis.
Because the current research suggests that UV light exposure contributes to the development of nonmelanoma skin cancers and possibly melanoma, limiting exposure may prevent the development of skin cancers. The United States Preventive Services Task Force currently recommends that primary care physicians counsel patients on sunprotective strategies, including regular application of sunscreen and avoidance of indoor tanning.
Management
Surgical excision is the primary treatment modality. Wide excision is recommended; but the recommended surgical margin varies, depending on the depth of the tumor. Mohs micrographic surgery has emerged as a surgical option in cases in which tissue preservation is important, such as on the head and neck, particularly in cases of lentigo maligna.
Sentinel lymph node biopsy is important in melanoma staging. The results from sentinel lymph node biopsy may provide important prognostic information. It is often recommended for melanomas that are more than 1 mm in depth. Adjuvant systemic therapies have limited success in the treatment of advanced-stage melanoma. IFN-a is an adjuvant treatment approved by the US Food and Drug Administration (FDA) for stage III melanoma; however, there is very limited efficacy.
High-dose IL-2, another immunotherapeutic recently been approved by the FDA for the treatment of metastatic melanoma, has been found to induce remission in 6% of cases of metastatic melanoma. In 2011, ipilimumab, a monoclonal antibody against cytotoxic T-lymphocyte antigen 4 that induces a T-cell–mediated response against the tumor, was approved for metastatic disease. Bevacizumab, an endothelial growth factor antibody, and vemurafenib, a BRAF cellular pathway inhibitor, have also shown some efficacy in advanced melanoma. Radiotherapy plays a limited role since melanoma is radioresistant compared with other cancers.
Trichoepithelioma
Introduction
Trichoepitheliomas are benign follicular neoplasms, 2- to 3-mm dome-shaped papules on the nasolabial folds and upper lip.
Cause
Multiple familial trichoepithelioma is a disseminated autosomal dominant form of this disease characterized by numerous papules on the central face. Another heritable condition, known as Brooke-Spiegler syndrome, consists of trichoepitheliomas accompanied by other neoplasms, cylindromas and spiradenomas, as a result of mutations in the CYLD tumor suppressor gene.
Epidemiology
They are increasingly probable with advancing age, though inherited forms can be seen in children.
Prognosis
Trichoepitheliomas are characterized by slow growth. Recurrence may occur with partial removal of lesions. The familial variant may have an aggressive, recurrent course with numerous tumors.
Clinical Features
A solitary lesion presents as a small 2- to 3-mm, smooth, firm, dome-shaped, skin-colored papule that is commonly seen on the nasolabial folds, nose, upper cutaneous lip, and scalp. Trichoepitheliomas can be clinically suspicious for a malignancy. A certain phenotype, known as desmoplastic trichoepithelioma, may resemble basal cell carcinoma and presents as firm papules with raised annular borders and a slightly indented center. Such lesions are found most commonly among young women, and familial solitary and multiple lesions have been described. Shave or small punch biopsies allow a histologic diagnosis of trichoepithelioma, which shows nodules of basaloid cells in a fibrous stroma with prominent follicular germs and papillae and small horn cysts.
Management
Treatment is primarily surgical excision. Multiple lesions can be resurfaced with laser surgery, dermabrasion, or electrosurgery ; but the results of these procedures vary and tend to be repeated because of the gradual regrowth of elevated papules or nodules.
Sebaceous hyperplasia
Introduction
Sebaceous hyperplasia is characterized by yellowish or skin-colored papules with a predilection for the face.
Cause
The risk of development of sebaceous hyperplasia is dramatically increased by chronic immunosuppression with cyclopsporin A or infection with HIV. Although the cause is unclear, murine experiments have suggested that topical irritants and carcinogens may be implicated in the pathogenesis of sebaceous hyperplasia. Growth factors or other cytokines produced by young fibrocytes may explain why some sebaceous hyperplasias overly other lesions, including neurofibromas, melanocytic nevi, verruca vulgaris, and acrochordons.
Epidemiology
Lesions may be seen at any age, although prevalence is highest in the fifth decade and increases over time. Sebaceous hyperplasia is more common in men.
Prognosis
Although sebaceous hyperplasia does not have malignant potential, it is associated with an increased risk of nonmelanoma skin cancer in patients undergoing a renal transplant. Additionally, an association with Muir-Torre syndrome, an autosomal dominant genodermatosis characterized by at least a single sebaceous gland tumor and one or more internal malignancies, has been postulated, although this is controversial because the high prevalence of sebaceous hyperplasia renders it essentially nonspecific for the syndrome.
Clinical Features
Several rare forms of sebaceous hyperplasia exist, which are classified as giant, linear, diffuse, functional familial, and juxtaclavicular beaded lines. The most common variant, however, is senile sebaceous hyperplasia, which is recognized by its yellow color, dome-shaped morphology, and ductal opening. The diagnosis of sebaceous hyperplasia can be made clinically, but biopsy is confirmatory when there is uncertainty. Lesions may clinically resemble basal cell carcinoma, making histologic examination necessary.
Management
Treatment is usually for cosmetic purposes and may elicit the use of photodynamic therapy, chemical peeling, isotretinoin, bichloracetic acid, cryosurgery, electrodessication, and laser therapy.
Milia
Introduction
Milia are small, white, benign, superficial cysts that generally measure less than 4 mm.
Cause
Milia are classified as either primary or secondary. Primary milia arise spontaneously and include the following subtypes: congenital milia, benign primary milia of children and adults, milia en plaque, nodular grouped milia, multiple eruptive milia, nevus depigmentosus with milia, and genodermatosis-associated milia. Secondary milia are associated with blistering disease, medication, or trauma.
Epidemiology
Milia are noted to occur in those of all ages. Primary milia are seen in newborns. Multiple eruptive milia, although rare, are more common in women.
Prognosis
Milia in infancy tend to spontaneously disappear within the first few weeks of life. When they occur in adults or older children, they often persist.
Clinical Features
Milia have walls of stratified squamous epithelium that resemble the epidermis or the follicular infundiblulum, and they have a granular cell layer adjacent to the keratinous cyst lumen. They are white to yellow cystic-appearing papules, dome shaped, and asymptomatic. Overwhelmingly, the most common type encountered in clinical practice is benign primary milia of children and adults, with lesions of the head commonly seen on the cheeks, eyelids, forehead, and, rarely, the nasal crease.
Management
Milia can be safely left alone; but if treatment is desired, the contents of the cyst may be extruded by making a small incision with a needle, scalpel blade, or even a paper clip and applying tangential pressure with a comedone extractor or curette. Topical retinoids and mild electrocautery or electrodesiccation are other therapeutic options for multiple milia.
Acne vulgaris
Introduction
Acne vulgaris is a common, inflammatory disease of the pilosebaceous units affecting adolescents and young adults, characterized by the development of comedones (keratin and sebum-plugged pilosebaceous units), inflammatory papules, and pustules.
Cause
The formation of acne depends on 4 primary factors: increased sebum production from the sebaceous glands, hyperkeratinization of the follicle that leads to an enlarged comedo, colonization of the follicle by the anaerobe Propionibacterium acnes , and an inflammatory reaction.
Epidemiology
Acne is the most common skin disorder in the United States, affecting 40 to 50 million people of all ages and races. Acne usually begins in adolescence and often resolves by the mid 20s, with girls peaking in prevalence at a younger age than boys. Males are usually more frequently and more severely affected than females on account of greater androgen levels, which correlate with greater sebaceous gland activity.
Prognosis
Acne is generally self-limited, lasting from months to a few years. Adult woman with chronic acne can be an exception to this rule and may be affected by acne for several years. Cystic acne variants, seen most commonly in young men, may persist from adolescence to the fifth decade of life and can be complicated by profound scarring despite treatment.
Clinical Features
The main features of acne range from noninflammatory open (blackheads) or closed (whiteheads) comedones to inflammatory papules, pustules, nodules, and cysts. Lesions occur in areas with the highest concentration of sebaceous glands, such as the face, neck, chest, and back. Inflammatory lesions may be superficial or deep, and deeper lesions may be complicated by scarring. In patients with darker skin types, postinflammatory hyperpigmentation is commonly observed.
The presence of comedones can help distinguish acne from the following conditions: folliculitis, rosacea, or perioral dermatitis.
Management
The goals of treating acne include acute control of flare-ups; long-term maintenance therapy; scar prevention; and reduction of accompanying psychologic sequelae, such as embarrassment and anxiety. Accordingly, the severity of the condition and patients’ motivation dictate aggressiveness and risk of the therapy to be undertaken. Current therapies are aimed at the aforementioned 4 major factors of acne development. Topical retinoids are effective in the reduction and prevention of comedones, making them suitable for the treatment of inflammatory and noninflammatory lesions. Benzoyl peroxide is an over-the-counter bactericidal agent that does not lead to bacterial resistance. Topical and oral antibiotics are especially effective in combination with topical retinoids and benzoyl peroxide but may be used as monotherapy. Systemic hormonal therapy may be useful in adult women with chronic acne. Severe, recalcitrant acne, especially if associated with scarring, may warrant the use of oral isotretinoin. Finally, patients should be counseled to avoid picking or squeezing acne lesions, which may prolong healing.
Gram-negative folliculitis
Introduction
Gram-negative folliculitis is an uncommon superficial or deep bacterial infection of the hair follicle.
Cause
The normal gram-positive flora of the facial skin and mucous membranes of the nose are replaced and invaded by gram-negative bacteria, which include Escherischia coli , Pseudomonas aeruginosa , Serratia marescens , Klebsiella , and Proteus mirabilis . The infection is considered to be a complication of long-term antibacterial treatment in patients with acne and rosacea.
Epidemiology
Anyone using antibiotics for a prolonged period of time may be affected, with a greater likelihood among older men with severe seborrhea.
Prognosis
The prognosis for cure is excellent once the diagnosis is accurately established and appropriate therapy is rendered.
Clinical Features
Typical features include perioral and perinasal erythematous papules and pustules or, less commonly, a deep, nodular, and cystic lesion. Gram-negative folliculitis should be suspected in patients with acne with flare of these characteristic lesions, who are being treated with chronic, oral tetracycline antibiotics. The differential diagnosis includes acne, rosacea, and pseudofolliculitis barbae. Diagnosis is confirmed by swabbing a lesion for gram stain, culture, and sensitivities.
Management
Gram-negative folliculitis may be treated with oral antibiotics selected based on the sensitivity and resistance pattern of the culture. Isotretinoin, a systemic retinoid, is also effective.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


