The objective of this article was to report a clinical case of a patient with solitary median maxillary central incisor syndrome. He was treated with rapid maxillary expansion and evaluated with computed tomography. The boy, aged 6 years 7 months, had a single maxillary central incisor in the midline, posterior crossbite, prominent midpalatal ridge, indistinct philtrum, no incisive papilla, and no labial frenulum. No other systemic anomalies were found. Posteroanterior cephalometric radiography showed skeletal atresia of the maxilla that was corrected with rapid maxillary expansion. A Haas expander was used and activated twice per day (quarter turn per activation) for 15 days. The procedure was monitored with computed tomography to evaluate any effect on the intermaxillary suture and tooth. Although the crossbite was clinically corrected after the expansion, radiographs and tomographs showed no opening of the midpalatal suture. Rapid maxillary expansion resulted in neither midpalatal suture opening nor transverse increase of the maxillary skeletal base in this patient.
Solitary median maxillary central incisor (SMMCI) syndrome is a rare disorder affecting about 1 in 50,000 newborns. This anomaly is characterized by a symmetric central incisor of normal size located exactly in the midline of the maxilla. Other midline structures of the body, including the skull bones, the nasal cavity, and even the brain can be involved.
The etiology of this condition is unknown. Some authors suggest that the formation of 1 central incisor might be the result of a change in the cell mitotic potential of this group of teeth, interfering with genetic or environmental factors. In addition, lack of space in the dental arch or deficiency of transverse growth might result in early fusion of the right and left dental lamina, thus impeding the formation of 2 central incisors.
SMMCI syndrome is seen in both the deciduous and permanent dentitions. It is characterized by high labial position, malformation in the palatal suture, V-shaped palate with prominent midpalatal ridge, and absence of labial frenulum and incisive papilla. Moreover, other systemic characteristics can be associated with SMMCI syndrome, such as choanal atresia, nasal stenosis, nasal pyriform aperture stenosis, short stature, growth-hormone deficiency, and learning deficits. In severe cases, in addition to those characteristics cited above, there can be holoprosencephaly or chromosomal anomalies.
In terms of dental treatment, there are few reports on SMMCI syndrome in the literature. In general, the treatment approach differs depending on the characteristics of the malocclusion. Basically, however, the treatment suggestion consists of either closing the spaces or opening them for prosthetic rehabilitation with implants.
This article reports on a child with SMMCI syndrome who had rapid maxillary expansion (RME) that was evaluated with cone-beam computed tomography (CT).
Case report
A boy, aged 6 years 7 months, was brought to the Paediatric Dentistry Clinic of the Federal University of Santa Catarina in Brazil by his caregiver, who was concerned about his appearance.
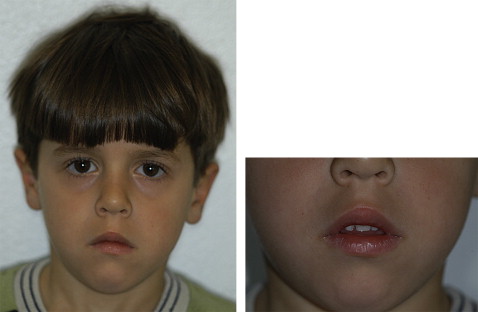
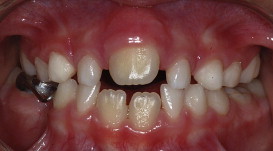
Clinical examination showed only 1 maxillary central incisor situated exactly in the midline as well no labial frenulum and incisive papilla, and an indistinct philtrum. The patient also had a posterior crossbite and a prominent midpalatal ridge ( Figs 1 and 2 ). He was in the mixed dentition phase and had no history of tooth loss from trauma or extraction in the anterior region; this ruled out early loss of 1 incisor.

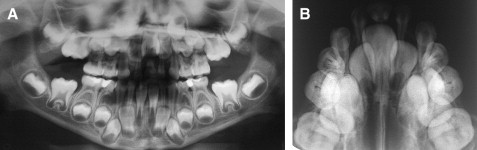
A periapical radiographic examination showed a central incisor having only 1 root canal, a finding also confirmed by CT. Panoramic radiography showed normal development of all permanent teeth ( Fig 3 , A ). Presence of the intermaxillary suture in the premaxilla, which was mistaken for the root canal of permanent incisor, was observed on the occlusal radiograph ( Fig 3 , B ). Sella turcica was found to be anatomically normal on profile radiography.
Posteroanterior radiography showed skeletal atresia of the maxilla. The distance between the jugal point and the frontal facial line was of 12 mm on both right and left sides; this meant a maxillary atresia of 4 mm according to Ricketts. Therefore, the RME with a modified Haas expander was the treatment of choice. The appliance was cemented to the maxillary second deciduous molars and attached buccally to the deciduous canines and palatally to the first deciduous molar. The clinical protocol for its activation was a half-turn of the screw when it was placed and quarter-turns twice a day for 2 weeks.
CT scans were taken three times: before treatment, 7 days after the start of RME, and after stabilization of the expander screw.
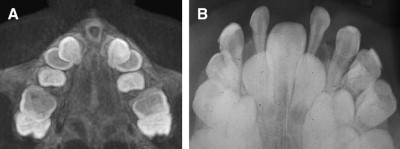
Both the CT and occlusal radiography images showed no suture opening after activation of expander screw ( Fig 4 ), and posteroanterior radiography and CT images showed no increase in the maxillary base. The initial intermolar widths were 36.88 and 22.36 mm at the canine and cervical levels, respectively. After expansion ( Fig 5 ), these measurements were 41.57 and 26.53 mm, respectively. Consequently, one can conclude that only dental movement with bone remodeling had occurred.
The patient was also evaluated by a geneticist, a cardiologist, an otorhinolaryngologist, and a psychologist concomitantly with the dental treatment. A cranial CT ordered by the otorhinolaryngologist showed that all structures were normal with no brain malformation. Blood was collected for DNA analysis, which showed no mutation linked to the SMMCI syndrome. Therefore, according to the medical reports, the patient had no other clinical findings associated with the syndrome, except for those involving his oral cavity and perioral region. The patient is still under genetic, psychological, and dental follow-up.
Discussion
Early detection of SMMCI syndrome is crucial regarding the patient’s dental needs. Genetic counseling is often advised, since holoprosencephaly is a severe congenital malformation that affects daily life and is commonly associated with SMMCI syndrome.
In general, the dentist is responsible for the initial clinical diagnosis and then refers the patient for specialized evaluation before any dental intervention.
The lack of a maxillary central incisor is commonly caused by trauma. However, cases of anadontia are rarely found in the deciduous dentition, and the lateral incisor is often missing in the permanent deciduous. For this reason, further investigation on this tooth absence is an important differential diagnosis.
Lo et al reported that prenatal malformations involving palatal and facial midlines in patients with holoprosencephaly are associated with defects in the cerebral midline, malformation of sella turcica, and morphology of craniofacial structures. All these diagnoses are important in a differential diagnosis in patients with SMMCI syndrome.
However, changes in sella turcica morphology do not always mean pathophysiologic function, and dysfunction of the pituitary gland does not indicate alterations in sella turcica. In patients with holoprosencephaly, defects in the pituitary gland result in growth-hormone deficiency or short stature. Other cranial anomalies involving the facial and cerebral midlines, including SMMCI syndrome, might be hypothalamic-pituitary dysfunction.
In this case report, the radiographic image showed that sella turcica was within the normal morphology. In addition, the patient had a normal height for his age and no changes in the growth-hormone levels.
By analyzing occlusal photographs of patients with SMMCI syndrome, Kjaer et al classified the midpalatal ridge as complete or incomplete, with the former extending posteriorly from the central incisor to the soft palate, and the latter centrally situated at the palate. Similar to the cases reported by those authors, our patient had a complete midpalatal ridge.
We suggest that a morphologically altered midpalatal ridge might be the result of a tissue fusion during its embryologic formation.
Becktor et al analyzed radiographs from 11 patients with SMMCI syndrome and found that the vertical and horizontal growth of the maxilla was normal. However, they suspected that the transverse maxillary growth was deficient, and the internasal suture and parts of the intermaxillary suture were absent.
The lateral cephalometric analysis of our patient showed harmonious vertical and horizontal growth, although the posteroanterior radiograph showed maxillary atresia.
Several authors suggested that maxillary expansion can be a possible treatment for this cranial anomaly to obtain sufficient space to move the single incisor toward 1 side of the midline. This procedure would allow a dental implant or prosthesis to be placed next to the incisor.
On the other hand, Scott reported on a 6-year-old girl whose treatment of choice was to extract the incisor and move the lateral incisors toward the midline. McNamara et al also reported on a patient with SMMCI syndrome and a 10-mm overjet whose treatment might involve extraction to provide space enough for tooth alignment.
In this case report, the patient had maxillary atresia, and the treatment consisted of RME to correct the transverse skeletal discrepancy at the proper age. In esthetic and psychological terms, however, this procedure is not enough to rehabilitate the child, since the main complaint was not properly resolved.
Because there is no previous case report on patients with SMMCI syndrome having RME, it was decided to monitor the whole procedure with CT. The first scan was made before treatment; the second was 7 days after the initial activation of the expander so that both incisor positioning and any changes in the palatal midline could be evaluated. The second CT scan showed no midpalatal suture opening and no incisor movement or change in the alveolus. Clinically, the patient still had a posterior crossbite.
The expander screw was further activated for 7 days, and a third CT scan and occlusal radiograph were taken. It was observed that the posterior crossbite was uncrossed, and alveolar remodeling and dental movement had occurred despite the lack of midpalatal suture opening.
In 2006, Hall cited that in some cases the intermaxillary suture is absent in the anterior region of the incisive fossa, which was probably prematurely fused. In this case report, however, the intermaxillary suture was mistaken for the incisor root canal on the initial occlusal radiograph.
Podesser et al used CT scanning and RME to evaluate normal patients aged 8 years 1 month on average during their mixed dentition phase. All patients had midline palatal openings in the molar and canine regions measuring on average 1.6 and 1.52 mm, respectively. For these patients, the mean intermolar distance was 3.6 mm. Those authors emphasized that almost 50% of the occlusal changes resulted from dentoalveolar alterations, and skeletal involvement was relatively modest.
Because maxillary expansion in patients with no anomalies in their nasomaxillary complex is limited, at least skeletally, this implies that RME in patients with SMMCI syndrome will not open the intermaxillary suture because of the probable fusion of the anterior sutural region where the single tooth is located. Therefore, further studies are needed to verify whether it is an isolated case or whether SMMCI syndrome carriers cannot have their maxillary suture opened.
Another treatment option discussed by the authors was surgically assisted maxillary disjunction.
Our patient is being followed by a multidisciplinary team that includes an orthodontist, a pediatric dentist, a geneticist, and a psychologist.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


