(1)
Department of Endodontics, Nova Southeastern University College of Dental Medicine, Fort Lauderdale, FL, USA
Digital Radiographs
Dental radiographs created by x-rays are used to visualize the internal structures of the teeth, bones, and soft tissues to help diagnose pathology. Dental radiographs can show hidden dental structures such as cavities, anomalies, malignant or benign masses, impacted wisdom teeth, periapical lesions, and bone resorption that cannot be seen during a visual examination. Dental radiographs are an important diagnostic aid and are routinely taken preoperatively and postoperatively to monitor the outcome of endodontic treatment. Radiographs should only be taken when they are necessary for diagnosis and treatment. The amount of radiographs that should be taken of patients should be as few as reasonably achievable to limit their exposure to radiation.
Radiation Dosage and Avoiding Incidental Radiation Exposure
The dosage of x-ray radiation received by a dental patient is typically 0.150 mSv for a full mouth series of radiographs [1]. The dental radiation dose is equivalent to a few days’ worth of background environmental radiation exposure. Newer technology has reduced the amount of radiation needed to obtain radiographs by increasing the speed of the x-ray film. It is recommended to always use the fastest radiographic film (E or F film speed) and to reduce incidental patient radiation exposure by using lead protective aprons to shield the abdomen and thyroid when taking radiographs. Before a radiograph is being taken, all personnel should leave the room or stand behind lead shielding to limit their incidental radiation exposure.
A fundamental principle for diagnostic radiology is to limit the patient exposure to radiation using ALARA, as low as reasonably achievable by FOOD:
1.
Following appropriate radiograph selection criteria after taking a history from the patient and then a clinical evaluation.
2.
Only properly trained and credentialed personnel should take radiographs.
3.
Optimal radiographic techniques should be used, including beam projection geometry, beam energy, collimation, and filtration.
4.
Detector must be the fastest available to obtain a radiographic image of adequate diagnostic quality.
X-Rays and Radiographs
X-rays were first called invisible rays and were discovered by W. Conrad Roentgen in 1895 [2]. X-rays are a form of high-energy electromagnetic radiation. A radiographic image is formed by a controlled burst of x-ray radiation which penetrates oral structures at different levels, depending on varying anatomical densities, before striking the film or sensor. The teeth appear lighter because less radiation penetrates their dense structure to reach the film. If some of the structure of the teeth or bone is missing because of dental caries, infections, resorption, and lesions, these areas of pathology appear darker because the x-rays more readily penetrate these structures.
Dental materials for tooth restoration with filings and crowns or root canal obturation and sealing can appear lighter or darker depending on the density of the material. Most dental materials contain a radiopaque material such as barium sulfate to help visualize the material in radiographs.
The ability to accurately interpret radiographs is essential to identify and diagnose oral diseases. Reaching an accurate diagnosis takes training, skill, and good-quality imaging. Poor angulation and poor geometric configuration of the tooth onto the x-ray sensor can lead to poor-quality images which can cause substantial errors in interpretation. Most routine endodontic radiographs display sufficient resolution and image details to allow the diagnosis of problems and for treatment procedures to be planned.
Dental radiographs are commonly taken by placing the radiographic film or electronic sensor inside the patient’s mouth. A decision-making flow chart for taking radiographs is shown in Fig. 4.1.
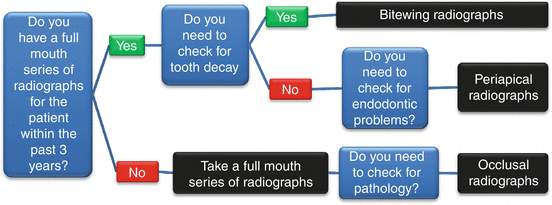

Fig. 4.1
Flow chart for taking radiographs
Types of Radiographs
The following types of dental radiographs are common.
Bitewing Radiographs
The name bitewing refers to a small tab of plastic situated in the center of the x-ray film. The patient bites on the tab which holds the x-ray film in a position to visualize the crowns of the posterior teeth and the height of the alveolar bone in relation to the cement-enamel junctions, which are the demarcation lines on the teeth which separate the tooth crown from the tooth root. The bitewing radiographs are routinely used to detect tooth decay and recurrent caries under existing restorations. When there is extensive bone loss, the films may be situated with their longer dimension in the vertical axis so as to better visualize their levels in relation to the teeth. Because bitewing views are taken from a more or less perpendicular angle to the buccal surface of the teeth, they more accurately exhibit the bone levels than do periapical views. Bitewings of the anterior teeth are not routinely taken.
Periapical Radiographs
The periapical radiograph is taken to visualize the root apex, periapical tissues, and bone surrounding the teeth that a patient is complaining of being painful and/or has swelling and/or the symptoms of infection. The periapical radiograph is the most common type for determining the need for endodontic therapy as well as to monitor the outcome of endodontic therapy. Periapical radiographs are useful in detecting impacted teeth and hyperdontia or presence or absence of supernumerary teeth.
In order to create a high-quality periapical radiograph, the central x-ray beam must pass through the alveolar crest or root apex. There are two projection techniques for taking periapical radiographs:
-
The paralleling technique, also called the long-cone technique: The periapical film is stood parallel to the long axis of the teeth, and the central is aimed at the right angles of the teeth and the film (Fig. 4.2a).
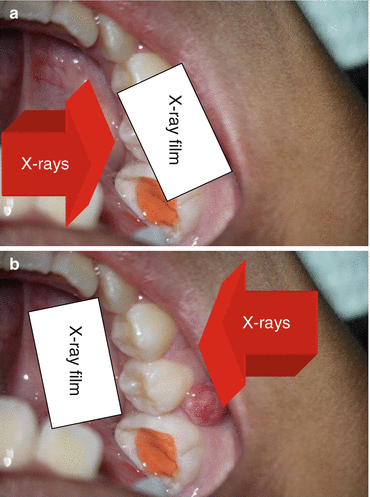 Fig. 4.2(a) The paralleling technique; (b) the bisecting-angle technique
Fig. 4.2(a) The paralleling technique; (b) the bisecting-angle technique
Occlusal Radiographs
The occlusal radiograph is taken to visualize the skeletal or pathologic anatomy of either the floor of the mouth or the palate. Sometimes, the occlusal film is used to detect soft tissue anomalies and conditions. The occlusal view is not included in the routine full mouth series of radiographs.
Full Mouth Series of Radiographs
A new dental patient may need to have a complete set of radiographs taken of their mouth. The full mouth series (FMS or FMX) or complete mouth radiographic series (CMRS) is discouraged because it involves taking 18 radiographs, many of which may not be necessary for the patient’s treatment. The full mouth series comprises of:
Four bitewings:
-
Left and right molar bitewings
-
Left and right premolar bitewings
Eight posterior periapicals:
-
Left and right maxillary molar periapicals
-
Left and right maxillary premolar periapicals
-
Left and right mandibular molar periapicals
-
Left and right mandibular premolar periapicals
Six anterior periapicals:
-
Left and right maxillary canine-lateral incisor periapicals
-
Left and right mandibular canine-lateral incisor periapicals
-
Maxillary and mandibular central incisor periapicals
Panoramic Radiographs
Panoramic radiographs are occasionally taken using extraoral films and show a broad view of the jaws, teeth, sinuses, nasal area, and temporomandibular joints and anatomic structures (Fig. 4.3).
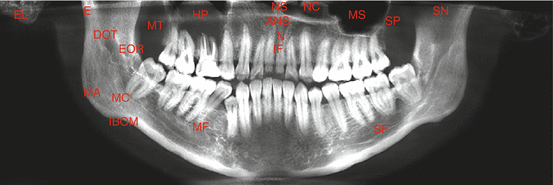

Fig. 4.3
Panoramic radiograph with marked anatomic structures. ANS anterior nasal spine, DOT dorsum of tongue (shadow), EL ear lobe, E epipharynx, EOR external oblique ridge, HP hard palate, IF incisive foramen, IBOM inferior border of mandible, MA mandibular angle, MC mandibular canal, MC mandibular condyle, MS maxillary sinus, MT maxillary tuberosity, MF mental foramen, NS nasal septum, NC nasal cavity, N nasopalatine canal, SN sigmoid notch, SP soft palate, SF submandibular fossa
Panoramic radiographs are useful in detecting impacted teeth, bone abnormalities, cysts, solid growths (tumors), infections, and fractures but have limitations for assessing periodontal bone loss and tooth decay. Panoramic radiographs of children are useful in detecting developing teeth (Fig. 4.4).
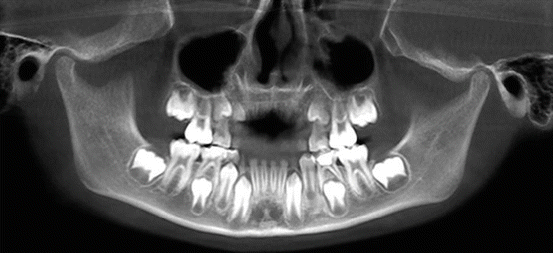

Fig. 4.4
Panoramic radiograph of a child with developing teeth
Cone Beam Computed Tomography
Digital radiographs are an acceptable first choice for the diagnosis and treatment of dental pathology. Cone beam computed tomography (CBCT) imaging is becoming a complementary technology and in many instances can provide 3-dimensional oral pathology information that might have been overlooked on 2-D images. CBCT avoids the superimposition seen on 2-dimensional radiographs and avoids the geometric distortion of radiographic structures. CBCT must not be used routinely for endodontic diagnosis or for screening purposes in the absence of clinical signs and symptoms that require imaging. A patient’s history and clinical examination must justify the use of CBCT in addition to routine radiographs. Several different views are possible of patients with CBCTs as shown in Fig. 4.5.
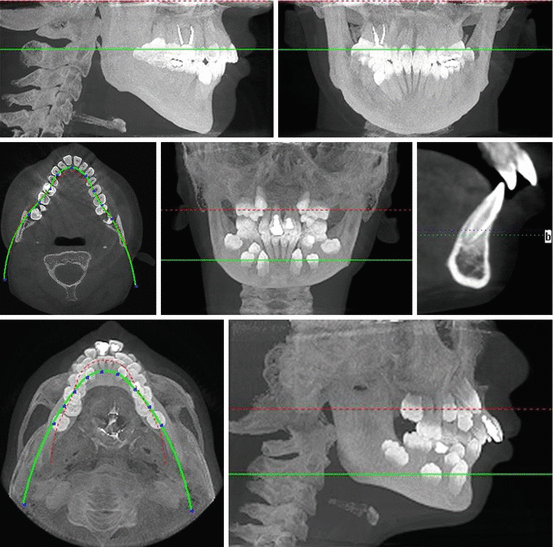

Fig. 4.5
A selection of CBCTs showing the different views which are possible
Computed tomography was invented by Hounsfield in 1974 [4]. The first CBCT unit was approved in the USA in 2001 [5]. Since then, the technology has become standard in dental schools and hospitals. CBCT uses a rotating gantry with an x-ray source and detector. A divergent pyramidal or cone-shaped source of ionizing radiation is directed through the middle of the area of interest onto an area x-ray detector on the opposite side of the patient. The x-ray source and detector rotate around a fixed fulcrum within the region to be imaged. During the exposure sequence, hundreds of planar projection images are acquired of the field of view (FOV) in an arc of 180°. In a single rotation, the CBCT can generate accurate 3-D radiographic images. The limitation of CBCT is the artifacts caused by scatter and beam hardening around high-density structures including enamel, metal posts, restorations, and root obturation materials. Another common problem is artifacts caused by patient movement during the CBCT scan. Dentists must be responsible for interpreting the entire CBCT image and can be liable for missed diagnosis, even if it is outside of endodontics; thus, specialist referral of CBCT or routine checking of CBCTs in universities and hospitals by specialists is recommended.
CBCT Field of View
The CBDT dimensions of the field of view (FOV) also known as the scan volume are dependent on the detector size and shape, the beam projection geometry, and the ability to collimate the beam. Collimation of the primary x-ray beam limits x-radiation exposure. The field size limitation ensures that an optimal FOV can be selected for each patient based on disease presentation and the tissues to be imaged. In general, the smaller the scan volume, the higher the resolution of the image and the lower the effective radiation dose to the patient. As the earliest sign of a periapical radiographic finding suggestive of pathosis is discontinuity in the lamina dura and widening of the periodontal ligament space, it is desirable that the optimal resolution of any CBCT imaging system used in endodontics does not exceed 200 μm—the average width of the periodontal ligament space [5]. The principal limitation of large FOV cone beam imaging is the size of the field irradiated. Unless the smallest voxel (volumetric pixel) size is selected in these larger FOV machines, there will be reduced resolution compared to intraoral radiographs or limited-volume CBCT machines. For endodontic use, limited or focused FOV CBCT is preferred over large volume CBCT. There is often an extra charge to patients for CBCT images, but the advantages of CBCT over other types of radiographs are:
1.
Images of tissues which are located on axial, coronal sagittal planes can be seen more easily. The anatomical area of interest is focused and it reduces the area of responsibility.
2.
No magnification or distortion problems, and saves some time, because of the smaller volume to be interpreted.
3.
Superimposition of tissues is eliminated.
4.
Easy planning of the placement of dental implants.
5.
Cyst and tumor density can be measured.
6.
Tissues with different densities can be more easily distinguished. Resolution is increased to improve the visualization of calcified/accessory canals, root canal curvature, missed canals, root fractures, luxation, and tooth displacement and differentiate odontogenic from nonodontogenic pathology, discontinuity in the lamina dura, widening of the periodontal ligament space, root resorption, and periapical lesions.
The disadvantages of CBCT over other types of radiographs are:
1.
Higher radiation exposure.
2.
A contrast agent is necessary to image soft tissue.
3.
Degradation of images by metallic objects, dental crowns, and fillings.
CBCT Diagnosis
The pathology in and around the individual teeth can be more easily diagnosed by the high-resolution images of CBCT. The periodontal ligament is approximately 0.2 mm in diameter; the high resolution allows the assessment of periodontal disruptions from apical periodontitis, periapical pathology, fractures, and other pathology. CBCT has fewer limitations for identifying periapical pathology, which can only be seen on standard radiographs if the bone loss is more than 35 % and it perforates the cortex [5
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


