Fig. 9.1
(a) A preoperative film of a maxillary cuspid with a perforation on the distal aspect of the coronal one-third. (b) The off-angle radiograph shows better the perforation. (c) The perforation has been repaired with MTA. (d) Postoperative radiograph
Figure 9.2 shows a case that had previously been surgically treated; the retreatment of this maxillary molar includes nonsurgical cleaning, shaping, and obturating the root canal system. This case, too, must be considered a retreatment, even though there was no previous filling material to remove from the canals. Figure 9.3 shows a maxillary first molar treated with a missed second mesiobuccal (MB2) canal. The tooth was nonsurgically retreated, but no filling materials were removed from the missed canal.
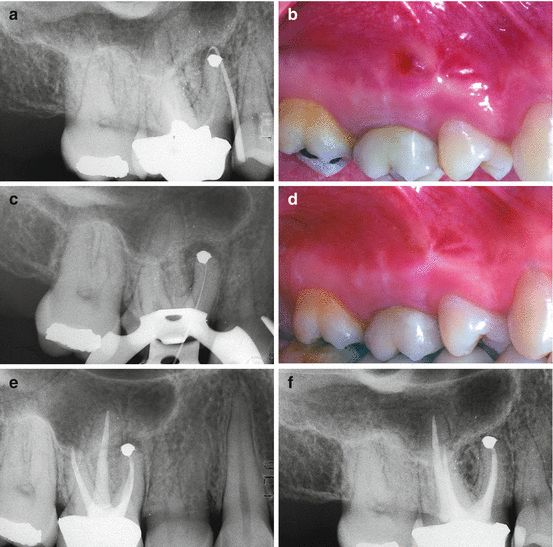
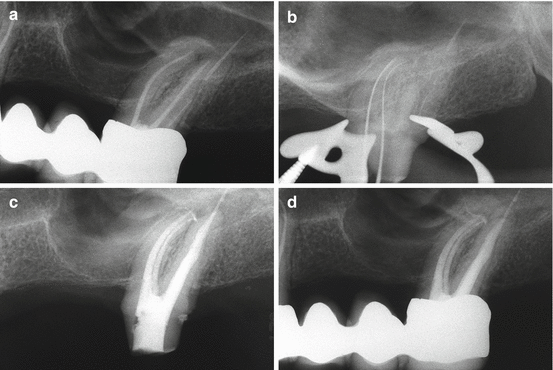

Fig. 9.2
(a) Preoperative film of the maxillary right first molar. The apical surgery has been performed on contaminated and empty root canals. The surgical failure must be retreated nonsurgically. The gutta-percha cone traces the sinus tract. (b) A sinus tract is evident clinically. (c) Working length radiograph of MB1. (d) After cleaning and shaping four canals, the sinus tract disappeared. (e) Postoperative film. (f) Two-year recall

Fig. 9.3
(a) The patient was referred for the retreatment of the palatal canal, thinking that the cause of pain was the overfilling. (b) During the retreatment, a missed MB2 was negotiated and then cleaned and shaped. Immediately after that, the pain disappeared, even though it was not possible to remove the gutta-percha protruding through the foramen of the palatal root. (c) Postoperative film. Note the independent foramen of MB2. (d) Follow-up at 2 years
The following definition is offered according to Carr [2] as an alternative that more closely reflects the actual clinical practice of retreatment: Endodontic retreatment is a procedure performed on teeth that received failed prior attempts at definitive root canal treatment, requiring further endodontic therapy to achieve a successful result.
9.2.1 The Rationale for Retreatment
The clinical practice of root canal treatment has changed markedly over the last 20 years. The introduction of rotary instrumentation, of various new obturation systems, of ultrasonically powered devices, and of magnification systems (in particular operating microscopes) has significantly increased the success rate of primary endodontic treatment and endodontic surgery [3, 4].
Perhaps, the most important difference today is that an endodontist’s manual dexterity is no longer the prime determinant for success. Obviously, individual skill always makes a difference, but with the use of modern endodontic techniques, levels of excellence are seen that were unheard of in the past [5, 6]. Nevertheless, a significant portion of the workload of endodontic specialists continues to be dedicated to redoing failed endodontic treatments.
Implantology can deliver high success rates [7] that might make extraction and replacement by implants seem a valid alternative to endodontic retreatment. However, it should be stressed that the two types of treatment have different goals: endodontic treatment aims to prevent or treat apical periodontitis, whereas implants are used to replace missing teeth [8]. This means that retreatment is the approach of choice for cases with endodontic failure, in which the tooth can be salvaged, both from restorative and periodontal standpoints.
In a recent US epidemiological study by Salehrabi and coworkers on a population of 4744 teeth that had undergone orthograde retreatment by endodontists, the success rate after 5 years was 89 % [9]. Earlier, Fristad and coworkers analyzed the success rate in 112 roots retreated by undergraduate students after 10–17 years, and after 20–27 years. The success rate at 10–17 years was 85.7 %, but 10 years later this had risen to 95.5 %, equaling the success rate found in cases of first treatment [10]. The study authors conclude that the persistence of asymptomatic periapical radiolucencies, especially those with overfill, should generally not be classified as failures, as many of them will heal after an extended observation period. This statement is of particular interest in increasingly easy access to cone beam computed tomography (CBCT). It has been shown that considerably more (asymptomatic) lesions are detected on CBCT scans rather than on periapical radiographs of endodontically treated teeth [11]. Likewise, in a systematic review, Torabinejad reports that endodontic surgery appears to offer more favorable initial success, whereas nonsurgical retreatment leads to a more favorable long-term outcome [12].
Planning endodontic retreatment requires a correct diagnosis using clinical and radiographic findings (see Chap. 2 in this book). It is necessary to understand the cause or causes that have led to the failure of the prior treatment and determine the feasibility of salvaging the tooth restoratively and periodontally. Prognostic factors of individual cases must be combined with a diagnosis to formulate a correct treatment plan.
The secret of achieving high success rates in retreatment undoubtedly lies in understanding typical causes of failure of the original endodontic treatment and will be discussed in the following section.
9.2.2 Incomplete Treatment of the Root Canal System
A root canal system may be highly complex, especially that of molar teeth (see Chap. 1). In many cases, complete mechanical treatment of such root canal systems is virtually impossible. Two different types of incomplete treatment of the root canal system exist:
- 1.
The working length stops short of the canal end, due to anatomical problems (curvature, bifurcations, etc.), preparation errors, or pathological problems (mineralizations; see Fig. 9.4)
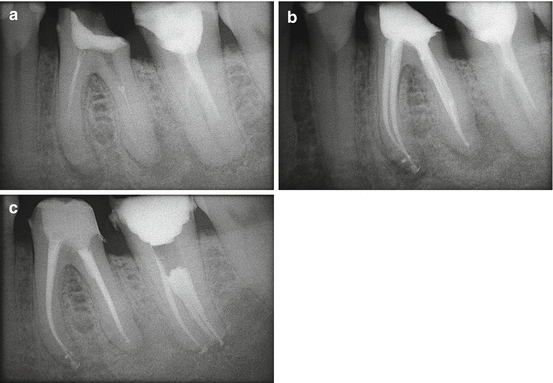 Fig. 9.4(a) Preoperative radiograph. Left mandibular first molar with insufficient endodontic treatment and apical, mesial, and distal radiolucent areas, indicative of asymptomatic apical periodontitis. (b) Postoperative radiograph. Retreatment. (c) Follow-up at 6 months
Fig. 9.4(a) Preoperative radiograph. Left mandibular first molar with insufficient endodontic treatment and apical, mesial, and distal radiolucent areas, indicative of asymptomatic apical periodontitis. (b) Postoperative radiograph. Retreatment. (c) Follow-up at 6 months - 2.
Overlooked anatomy (MB2 in maxillary molars, for middle mesial root canal of a mandibular molar, and other variants of molar anatomy, see Fig. 9.5)
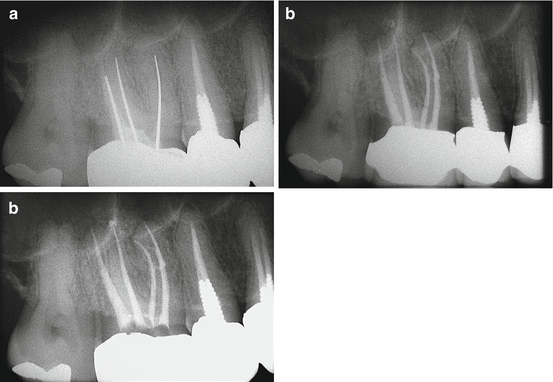 Fig. 9.5(a) Preoperative radiograph. Right maxillary first molar with insufficient endodontic treatment. (b) Postoperative radiograph after retreatment. The mesiobuccal root has two independent canals: MB1 and MB2. (c) Radiographic follow-up after 6 months
Fig. 9.5(a) Preoperative radiograph. Right maxillary first molar with insufficient endodontic treatment. (b) Postoperative radiograph after retreatment. The mesiobuccal root has two independent canals: MB1 and MB2. (c) Radiographic follow-up after 6 months
9.2.3 Inadequate Root Canal Filling
Historically, it has been held that inadequate apical seal may be a cause of failure in nonsurgical endodontic treatment [13]. It is indeed impossible to remove all the bacteria, toxins, and pulp tissue from the root canal system [14], and therefore tissue fluid (via the apical foramen and other foramina) may reach an incompletely filled canal space so that bacterial contamination persists and apical periodontitis is the consequence. Thus, to achieve long-term success, the root canal system should be filled as completely as possible.
Inadequate seal may occur in four cases:
- 1.
Canal filling in the presence of exudate
- 2.
Canal straightening with transportation of the apical foramen
- 3.
Ineffective filling techniques
- 4.
Filling procedure executed incorrectly
9.2.4 Vertical Fractures
According to clinical studies, vertical root fractures account for approximately 3 % of failures in teeth treated endodontically [15] and for 11 % of failures in fixed prostheses after 18 years [16]; of teeth requiring extraction, up to 32 % displayed vertical root fractures [17]. The extracted, fractured teeth were mostly root canal treated and associated with posts and screws. Diagnosis may be straightforward if the fracture can be identified in the coronal portion of the tooth in question: typically probing reveals a very narrow periodontal pocket along the fracture line (Fig. 9.6).
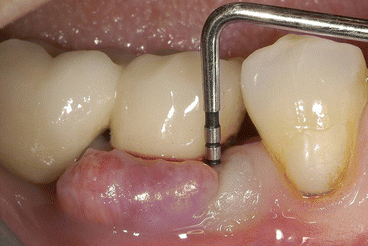

Fig. 9.6
Right mandibular first molar with vertical fracture of the mesial root. Very narrow periodontal probing is present at the fracture
Conversely, diagnosis is far from simple for a vertical root fracture that starts from the apical portion of the root. In these cases, there is initially no periodontal probing; however, a radiograph may show a radiolucent area along the lateral aspect of the root, or it is visible in a small field of view CBCT. In cases of a confirmed fracture connecting periodontal and pulpal spaces, nonsurgical retreatment is not recommended [18]. Endodontic surgery (see Chap. 10) may confirm or deny root fracture and provide means to improve the apical seal of the root canals (Fig. 9.7).
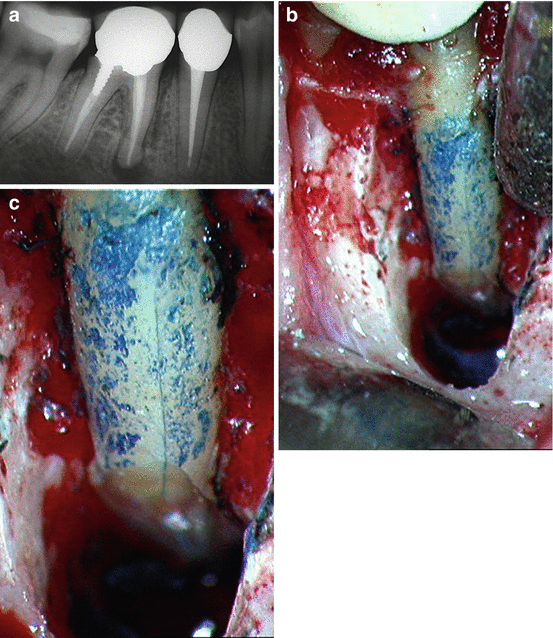

Fig. 9.7
(a) Preoperative radiograph. Right mandibular molar responsible for repeated abscesses. Note the good quality of the endodontic therapy and the radiolucent area surrounding the mesial root. Periodontal probing is noncontributory. Suspected vertical fracture starting from the apex suggests surgery is the best option. (b) View of surgical field. Note the loss of buccal bone in the mesial root area. The root was stained with methylene blue. Clearly visible fracture line originating apically and extending to the boundary between the medial and the coronal thirds of the root. (c) Enlarged view of surgical field
9.2.5 Loss of Coronal Seal
Loss of coronal seal is a frequent cause of failure some years after endodontic treatment. Magura and coworkers state that canals that have been obturated completely and exposed to the oral environment for 3 months or longer may need retreatment; if the root canal space had been prepared for a post, and if the root canal filling was incomplete, then the time lapse before clinically significant leakage occurs could be shorter [19].
In generating a treatment plan, the endodontist must next analyze the prognostic factors that may influence the treatment plan (Box 9.1).
Box 9.1. Prognostic Factors in Retreatment Decision-Making
-
Specific cause of failure
-
Presence of periradicular radiolucency
-
Satisfactory quality of prior treatment
-
Altered root canal morphology
-
Periodontal involvement
-
Suspected vertical fracture
-
Lack of coronal seal
-
Endodontist’s experience
-
Availability of technologies (operative microscope, ultrasound, etc.)
-
Patient’s expectations
9.2.6 Unclear Cause of Failure
To undertake retreatment without having clearly understood the causes responsible for failure of the original treatment is a serious mistake. While persisting or newly introduced microorganisms are the main cause of apical periodontitis [20], it is impossible to improve a situation without knowing where it went wrong in the technical aspects of treatment [21]. In difficult situations, it is not uncommon to think of the most complex and unusual causes (unsealed lateral canals, extra canals, etc.) and fail to see the obvious. The four causes of failure are listed above, and the specific cause or causes responsible for failure in individual cases must be determined. Naturally, an endodontist must have an in-depth knowledge of root canal anatomy for each molar, including possible anatomic variables, and he or she must perform a complete and in-depth clinical and radiographic assessment (see Chaps. 1 and 2 in this book).
9.2.7 Presence of a Periradicular Radiolucency
As with primary endodontic treatment, the presence of a preoperatively detected periradicular radiolucency in retreatment cases markedly reduces the success rate [21, 22]. In a critical review of literature published between 1970 and 2004 that sought to explore the level of evidence relating to the outcome of endodontic retreatment, Paik and coworkers [23] found that all included studies agreed in that the success rate was inferior in the presence of a periradicular lesion prior to retreatment; they also found that this difference varied greatly:
-
Presence of preoperative periradicular lesion – success rate ranged from 97 to 40 %
-
Absence of preoperative periradicular lesion – success rate ranged from 100 to 84.4 %
9.2.8 Satisfactory Quality of Previous Treatment
This prognostic factor is certainly one of the most problematic one. When dealing with the endodontic failure of a molar that has been treated satisfactorily from the endodontic standpoint (correct working length, appropriate shape, density of filling material), the most common error is to embark upon retreatment in the hope of improving the quality without taking into account that a possible cause may be a vertical fracture as discussed before. Chevigny and coworkers report an 88 % success rate for retreatment in cases where prior treatment was unsatisfactory, but only 66 % where prior treatment was adequate [22].
9.2.9 Altered Root Canal Morphology
The presence of ledges, perforations, false pathways, stripping, internal or external transportation of the foramen, mineralizations, broken instruments, apical resorption, or internal resorption are all factors that complicate retreatment and may jeopardize its success (Fig. 9.8). In a study on 452 teeth retreated after 2 years, Gorni and coworkers [21] found a significant difference in terms of success rate in cases in which the root canal morphology was altered, and in the presence of a periradicular lesion: they report 84.4 % success in the absence of iatrogenic alterations versus only 40 % in the presence of alterations of the root canal system.
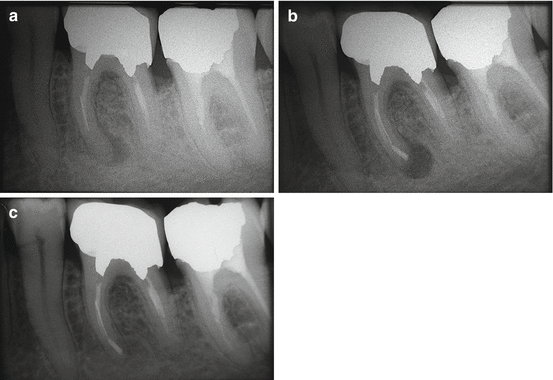

Fig. 9.8
(a) Preoperative radiograph. Left mandibular first molar with insufficient endodontic treatment and apical radiolucency at the level of the mesial root. Note the presence of a fragment of broken endodontic instrument in the middle third of one mesial root canal. Owing to the position of the broken instrument and the root anatomy, surgery is without doubt the least invasive treatment option. (b) Postoperative radiograph. (c) Radiographic follow-up at 6 months
9.2.10 Periodontal Involvement
It is important to distinguish between two different periodontal problems. One is primary: the patient is affected by periodontal disease of some degree of severity; he or she has numerous affected sites, and one of these is the molar scheduled for retreatment. As was already seen, in this case, a careful periodontal evaluation is necessary to evaluate whether the tooth can be salvaged, or whether it would be better to extract it and place an implant. The second eventuality is that in which there is a primary endodontic lesion with secondary periodontal issues, often as a consequence of iatrogenic damage (perforation, stripping, etc.; see Fig. 9.9). In these cases, the success rate is significantly reduced [24].
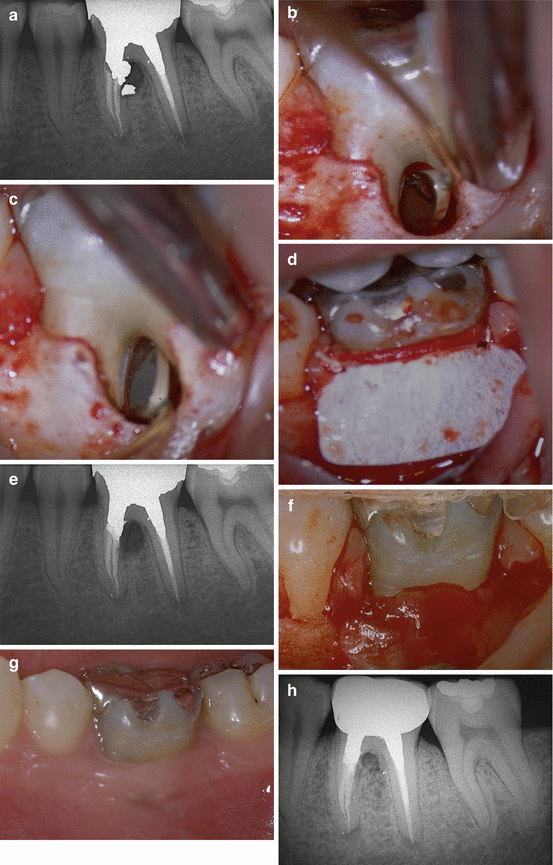

Fig. 9.9
(a) Preoperative radiograph. Left mandibular first molar with stripping at the level of the mesial root; repair has been attempted with amalgam. There is now an endo-perio lesion with wide buccal periodontal probing. (b) View of the surgical field. The amalgam obturation may be seen in the micro-mirror inserted into the furcation. (c) View of the surgical field. Repair of the perforation with Super EBA (Bosworth). (d) View of the surgical field. A Gore-Tex membrane is placed at the level of the periodontal lesion of the furcation. (e) Postoperative radiograph. (f) View of the surgical field, reopened after 4 weeks. Note the new-formed tissue. (g) Clinical checkup after 6 months. Note the healthy periodontal tissues. (h) Radiographic follow-up at 10 years
9.2.11 Suspected Vertical Fracture
As stated above, an evaluation of epithelial attachment must be made, even before radiography. Narrow probing reaching the apical third is very probably the consequence of a vertical root fracture. The presence of a single periodontal pocket, possibly in the furcation of a molar retreatment tooth, casts serious doubt on the possibility of salvaging the tooth for a long term. Another sign that points toward a vertical fracture is the presence of sinus tracts in unusual locations, for example, closer to the marginal gingival or on both the buccal and lingual aspects [25].
9.2.12 Lack of Coronal Seal
Lack of coronal seal at the time of retreatment undoubtedly complicates the already complex RCS infection. Kwang and Abbott [26] state that “The restoration-tooth interface is a potential pathway for bacteria to enter teeth and infect the root canal systems.” Complete removal of an existing restoration insertion of a leakage-proof temporary buildup is often the only way to ascertain that no new infection will occur during endodontic retreatment. Infection in retreatment cases may or may not be more difficult to eradicate, because it is sustained by streptococci, enterococci (e.g., Enterococcus faecalis) and yeasts [20, 27] existing in a biofilm, enabling them to develop effective protection against disinfectants [27, 28]. More recently, however, evidence has emerged that the microbial flora at the apicalmost portion of the root canal is similar in retreatment cases and initial treatment; this suggests that the inability to disinfect all canal space rather than specific microorganisms plays a role in failing endodontic treatment [29].
9.2.13 The Importance of Professional Experience
Because retreatment procedures frequently involve thinned root walls and altered anatomy, the endodontist’s level of experience is important, both in the initial phases of evaluating the case and formulating the treatment plan, and in the subsequent technical phases of executing the endodontic retreatment [30]. An experienced endodontist will be able to remember 15–20 other cases similar to the one being tackled, the difficulties encountered, how they were overcome, the end result, and the long-term outcome. A beginner in the specialty has the advantage of open-mindedness, but will require additional time to prepare to avoid irreparable damage of compromised teeth. Chapter 8 of this book provides a detailed discussion of decision-making in endodontics.
9.2.14 Available Technology
Whether in nonsurgical or surgical retreatment, both the operating microscope and ultrasonic tips are irreplaceable devices that can make a difference, significantly raising the treatment’s success rate. Setzer reported a success rate at 1 year of 88 % in surgical endodontic treatments performed with modern techniques, but without the help of enlargement, or only with magnifying loupes. The success rate rose to 94 % if surgery was performed under the operating microscope [31].
9.2.15 Patient Expectations
It is very important to have a consultation appointment with the patient, during which the endodontist illustrates costs and benefits together with any mishaps that could occur during treatment. The various phases of the procedure should be briefly explained and an estimate of costs given. The endodontist is under the obligation to list any alternative treatments, pointing out their advantages and disadvantages. It is imperative to understand the value of the tooth for the patient. A patient must never be urged into a decision: he or she must be sure that retreatment is the right choice and a good economic investment. To undertake retreatment in a nonmotivated patient is very stressful for the endodontist, and in consequence, it will be difficult to achieve a satisfactory outcome.
9.2.16 Nonsurgical Versus Surgical Retreatment
Nonsurgical retreatment is in principle considered the treatment of first choice, in particular, if this better addresses the cause of the treatment failure. Only when attempted nonsurgical retreatment is not feasible or was performed with no satisfactory result, should one select surgical treatment (see Chap. 10 in this book).
The clinical strategy in root canal treatment is to shape, clean, and fill the root canal system. Thus, it seems reasonable to assume that when nonsurgical retreatment addresses the entire canal space, cleaning it and densely filling it, success rates comparable to those possible with the primary endodontic treatment may be achieved. Studies point out better outcomes of surgical retreatment if it is preceded by nonsurgical retreatment that disinfects and seals the canal system successfully [32].
With this premise in mind, there are some cases in which surgical retreatment is indicated as first choice:
-
Presence of an obstacle that hinders complete treatment of the root canal space
-
Failure of an apparently well done endodontic treatment
-
Perforation in the apical third
-
Diagnosis of a suspected vertical fracture
-
Presence of recent, adequate prosthetic restoration
-
Less invasive compared to removal of restorations or posts
We may conclude that retreatment is indicated when there is a periradicular lesion that developed after the first endodontic treatment, when the lesion is enlarged or appears unchanged for more than 4 years, when the tooth is symptomatic, when the coronal seal has been lost for longer than 3 months, and when prosthetic restoration is necessary in the presence of an inadequate endodontic treatment, even without periradicular lesions and/or symptoms.
9.3 Clinical Practice of Root Canal Retreatment
9.3.1 Removal of Filling Material
The methods applied during nonsurgical retreatment vary according to the type of filling material to be removed or the obstacle to be overcome.
The degree of difficulty also varies, depending on whether the preceding obturation was performed with paste, sealer, gutta-percha, carrier-based obturators, or silver points, whether ledges were created in the root canal, whether an instrument had fractured, and whether preparation errors exist.
A preoperative radiograph can provide much useful information in this respect, but for molar retreatment, a cone beam CT (CBCT) scan should be obtained [33]. On the other hand, certainty about the nature of the material, its consistency, its ease of removal, as well as the presence of ledges and the likelihood of bypassing a broken instrument cannot be assessed by radiographic means alone, but can only be tested clinically, that is, by accessing the root canal space.
9.3.2 Pastes
The removal of root canal filling paste is in general easy, since, by definition, pastes do not set completely within the root canal; they can therefore be penetrated and removed by hand endodontic instruments and irrigating solutions. The most widely used paste is perhaps iodoform paste, which typically shows intense radiopacity and scattered areas of resorption.
9.3.3 Sealers
The removal of sealer is often also relatively simple; sometimes, however, it can be extremely complicated. Zinc oxide-eugenol sealers are dissolved by orange solvent [34], which is used as an irrigating solution, flooding the pulp chamber of the tooth in question. After creating the access cavity, an endodontic explorer is introduced into the orifice of the root canal to allow a deeper penetration of the solvent. After this, K-type endodontic instruments (e.g., .08 C + File, Dentsply Maillefer, Ballaigues, Switzerland) are introduced to probe apically with delicate movements. Special attention must be paid to not forcing the dissolved sealer beyond the apex and irritate periapical tissues. To prevent this, sealer should be removed as much as possible before taking instruments to the radiographic terminus of the canal and checking the working length.
If a sealer cannot be dissolved by orange or eucalyptic oil (whitish colored sealer, oftentimes used in Russia, and the reddish-brown resin paste, commonly utilized in Eastern Europe and the Pacific Rim), the coronal portion can be removed using ultrasonic instruments in conjunction with a microscope [35–37].
Once the preexisting sealer is eliminated and the canal has been negotiated to full length, the case can be completed using traditional methods (Fig. 9.10).
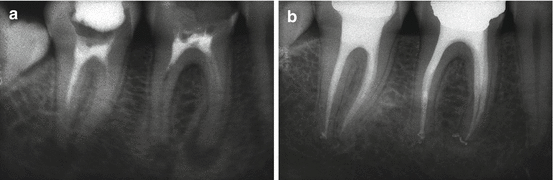

Fig. 9.10
(a) Preoperative radiograph. The first and second lower molars were treated using just sealer as a root-filling material. (b) Two years follow-up
9.3.4 Silver Point Removal
A silver point that conforms closely to the canal walls can be difficult to take out; in contrast, a point that fits loosely in a canal does not present great problems, especially if it extends into the pulp chamber. If zinc oxide-eugenol sealer, zinc phosphate cement, or composite were used to cover the coronal portion of the silver point within the pulp chamber, they can be removed with ultrasonics.
Once the coronal end of the cone is freed of surrounding materials, it can be grasped with hemostatic forceps (Stieglitz Forceps, Hu-Friedy; Chicago, IL, USA) and extracted from the root canal. If the pulp chamber was filled with amalgam, the silver point cannot be distinguished from the surrounding metal, and the cone will inevitably be sectioned at the orifice of the root canal unless one is able to dislodge the amalgam and remove it in one single piece. If one succeeds in doing so, the silver points will also be removed from the root canals [38]. Obviously, cutting the silver point seriously complicates the removal of the point itself and makes subsequent retrieval efforts difficult, if not impossible.
Dislodging a silver cone can be facilitated by the use of solvents to soften surrounding sealer or by ultrasonics [39, 40]. The latter is particularly effective in dislodging and removing silver cones after hand instruments have created paths alongside the points [38–41]. Ultrasonics has also been shown to be effective in removing fragments of silver cones when they break off within the canal as a consequence of corrosion [42]. Ultrasonics may be used indirectly, transmitting ultrasonic energy on grasping pliers to synergistically enhance the retrieval efforts. This form of “indirect” ultrasonics advantageously transfers energy along the silver point, breaks up material deep within the canal, and enhances removal efforts [42].
Some authors suggest several microtube removal methods, for example, Lasso & Anchor [43], the Cancellier Extractor kit (Sybron Endo; Orange, CA, USA) [2, 43], the Instrument Removal System (iRS) (Dentsply Maillefer) [43], the use of an injection needle with a wire loop at the end [44], and the use of specific instruments such as Masserann kit (Micromega; Besançon, France) [45] the Endo Extractor System kit (Roydent; Rochester Hills, MI, USA) [46] the Post Removal System kit (SybronEndo) [46]. However, the rigidity and size of the listed devices limit the use of these instruments to relatively wide and straight roots; any intracanal work with these tools requires the use of high magnifications, ideally an operating microscope. They cannot be safely used in the apical portions of curved roots.
9.3.5 Bypassing Ledges
One of the most frequent complications that can occur during root canal shaping is straightening the curvature of a canal, without communication with the periodontium; this is known as a ledge. The usual cause of ledges is using an incorrect, shorter working length. The canal is immediately blocked, due both to the accumulation of debris and the ledge that is formed. If the endodontist then applies force to the instruments in an attempt to bypass the blockage, he or she may create a “false canal,” tangential to the original pathway (Fig. 9.11). The result of ledge formation is that it becomes impossible to shape, cleanse, and fill the entire root canal; this frequently leads to treatment failure [47, 48].
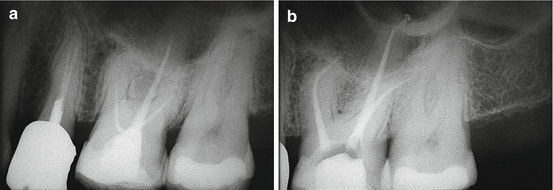

Fig. 9.11




(a) Left maxillary first molar. Endodontic treatment is insufficient and the patient complains of slight pain on mastication. (b) Postoperative radiograph showing retreatment. Note the palatal perforation in correspondence to the apical ledge
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


