Because the nose is a prominent facial structure, nasal fractures are the most common facial fractures. Compared to any other facial bone, less energy is required to fracture the nasal complex. These fractures frequently occur in conjunction with other facial fractures. The prevalence of nasal fractures is high and often unnoticed by both physicians and patients. Patients with nasal fractures usually present with some combination of deformity, tenderness, hemorrhage, edema, ecchymosis, instability, and crepitation ( Figure 16-1 ). However, these features may not be present or may be transient. Edema can mask underlying nasal deformity, crepitation, and instability; thus many physicians and patients fail to pursue further diagnosis and appropriate treatment. If left untreated, a nasal fracture can result both in unfavorable appearance and in unfavorable function, especially when the underlying structural integrity of bone and cartilage is lost. Nasal fractures are more common in males. Nasal fractures are seen in all age groups, but this condition is seen mostly in young males, probably as a result of increased interpersonal violence in this age group.
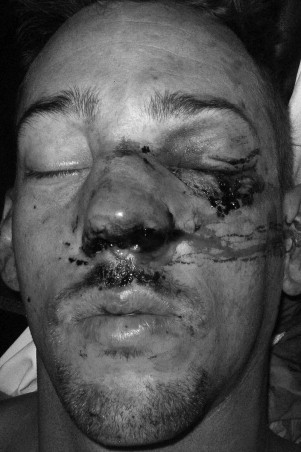
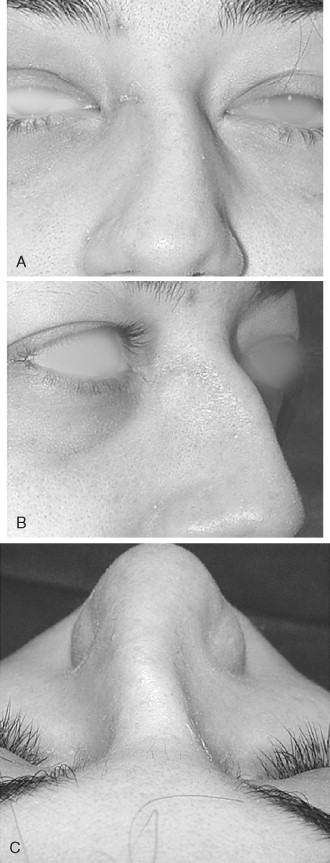
Nasal fractures can occur by a variety of insults such as interpersonal violence, sports, motor vehicle accidents, and industrial injuries. Significant controversy exists about the treatment of nasal fractures. This is mainly in the timing of repair and the method employed—closed versus open approach. Untreated nasal fractures account for the high percentage of rhinoplasty and septoplasty procedures performed months to years after the initial trauma occurs. Nasal trauma can also cause a dorsal hump deformity ( Figure 16-2 ). Thus appropriate treatment should be rendered in a timely manner, before scarring and soft tissue changes occur. The incidence of post-traumatic nasal deformity requiring revision rhinoplasty ranges from 14% to 50%. This is an indication that the initial approach to management of nasal fractures is suboptimal. Acute treatment of nasal fractures minimizes the amount of deformity, but the likelihood of additional treatment procedures should be considered.
APPLIED ANATOMY AND PATHOGENESIS
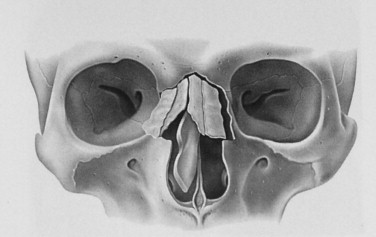
The nasal apparatus has a complex anatomy. Knowledge of this anatomy is of utmost importance in evaluation and management of nasal fractures. The nose occupies the middle third of the face and is attached at the top to the forehead; the free lower end of the nose is called the apex or tip. The upper part of the nose that is supported by the nasal bones is the bridge. The nasal bones and underlying cartilage are susceptible to fractures because the nose maintains a prominent position and central location on the face and because it has a low breaking strength. Patterns of fracture are known to vary with the momentum of the striking object and the density of the underlying bone. As with other facial bones, younger patients tend to have larger nasoseptal fracture segments, whereas older patients are more likely to present with more comminuted fracture patterns ( Figure 16-3 ).
SKIN AND SOFT TISSUES
The skin of the nose can be divided into vertical thirds. It is generally thicker in males than in females, and major racial differences also exist. The upper third is fairly thick but tapers into a thinner mid-dorsal region. The inferior third regains the thickness of the upper third as a result of the more sebaceous nature of the skin in the nasal tip. The dorsal skin is usually the thinnest of the three sections of the nose. The difference in the skin thickness must be appreciated during dorsal reduction because minor imperfections or fractures would make this area visible and perceptible. This would also make the dorsal area more susceptible to ecchymosis and lacerations with laterally directed forces on the nose.
The nasal muscles are encountered deep to the skin and comprise four principal groups: the elevators, the depressors, the compressor, and the dilators. The elevators include the procerus and levator labii superioris alaeque nasi. The depressors are the alar nasalis and depressor septi nasi. The compressor of the nose is the transverse nasalis, whereas the dilators are the dilator nares anterior and posterior. The muscles are interconnected by an aponeurosis termed the nasal superficial musculoaponeurotic system (SMAS). The internal nasal lining consists of squamous epithelium in the vestibule that transitions to pseudostratified ciliated columnar respiratory epithelium with abundant seromucous glands.
Hard Tissue Anatomy
Superiorly, the bony framework consists of the paired nasal bones attached to the frontal bone. Superolaterally, the nasal bones are connected to the lacrimal bones, and inferolaterally, they are attached to the ascending processes of the maxilla. Posterosuperiorly, the bony nasal septum is composed of the perpendicular plate of the ethmoid. Posteroinferiorly lies the vomer, which in part forms the choanal opening into the nasopharynx. The floor consists of the premaxilla and the palatine bones. The lateral nasal walls contain three pairs each of small, thin, shell-like bones: the superior, middle, and inferior conchae, which form the bony framework of the turbinates. Lateral to these curved structures lies the medial wall of the maxillary sinus. Inferior to the turbinates lies a space called a meatus, with names corresponding to the above turbinate (e.g., superior turbinate, superior meatus). The roof of the nose internally is formed by the cribriform plate of the ethmoid; posteroinferiorly to this structure, sloping down at an angle, is the bony face of the sphenoid sinus.
The nasal cartilages are paired upper lateral cartilages and lower lateral cartilages. These cartilages form the lower part of the internal skeleton of the nose. The nasal bones articulate with the upper lateral cartilages in a “lap” joint. The internal area or angle formed by the junction of the upper lateral cartilage with the nasal septum forms the internal nasal valve. This valve regulates nasal respiration. The upper lateral cartilages are triangular in shape. The internal nasal valve comprises the narrowest portion of the nasal airway. This valve regulates nasal respiration, and an angle wider than 15 degrees is needed in this area. They are connected to the maxilla laterally and to the septum medially. Beneath the upper lateral cartilages lie the lower lateral cartilages. The paired lower lateral cartilages swing out from medial attachments to the caudal septum in the midline, called the medial crura, and then to an intermediate crus area. They finally flare out superolaterally as the lateral crura. These cartilages are frequently mobile, in contradistinction to the upper lateral cartilages. The two medial crura of the lower lateral cartilage curve inferiorly down the midline to support the columella. The lateral crus of the lower lateral cartilage supports the ala during respiration. Adjacent sesamoid cartilages are variably found lateral to the lower lateral cartilages in the fibroareolar connective tissue.
The nasal septum forms the main vertical support of the nasal complex. It acts like a strut to support the nasal bones and upper and lower lateral cartilages in the midline. The nasal septum is made up of a bony component and a cartilaginous component. The vomer and perpendicular plate of the ethmoid form the bony component. The cartilaginous component is quadrangular in shape. The inferior aspect of the septum articulates with the crest or maxillary groove of the maxilla. This allows mobility of the septum but is also a common location for dislocation of the nasal septum during trauma. The septum articulates posteriorly with the sphenoid bone through the vomer.
Weak areas are noted in the cartilage framework and in the junctions of the upper lateral cartilages with the nasal bones and the septal cartilage at the maxillary crest. The weak areas account for an increase in the rate of fracture/dislocation after nasal trauma. A lateral force of only 16 to 66 kilopascals (kPa) and a greater frontal force of 114 to 312 kPa can displace the bony dorsum. A large force in any direction can cause comminution of the nasal bones with an associated C-shaped deformity of the nasal septum. Murray et al reported that almost any deviation of the fractured nasal bones involves a concomitant fracture of the septal cartilage. Cartilage fracture lines are often oriented vertically in the caudal septum and horizontally in the posterior portions.
Lateral impact injuries are the most common type of nasal injury leading to fracture. Lateral injury produces a depression of the ipsilateral nasal bone that usually involves the lower half of the bone, the nasal process of the maxilla, and a variable portion of the pyriform margin. Nasal fracture and displacement without septal fracture usually occur with weaker applied forces; however, with increased force, displacement of the bilateral nasal bones can be noted, and the septum is usually dislocated and fractured as well.
Other injuries that are commonly associated with nasal fractures include midface injuries involving the frontal, ethmoid, and lacrimal bones; naso-orbital-ethmoid fractures; orbital wall fractures; cribriform plate fractures; frontal sinus fractures; and maxillary LeFort I, II, and III fractures.
Blood Supply
The arterial supply to the nose is by (1) branches from the internal carotid, namely, the branches of the anterior and posterior ethmoid arteries from the ophthalmic artery; and (2) branches from the external carotid, namely, the sphenopalatine, greater palatine, superior labial, and angular arteries.
The external nose is supplied by the facial artery, which becomes the angular artery coursing over the superomedial aspect of the nose. The sellar and dorsal regions of the nose are supplied by the infraorbital artery, branches of the internal maxillary artery and ophthalmic arteries, and branches from the internal carotid system.
Internally, the lateral nasal wall is supplied by the sphenopalatine artery posteroinferiorly and by the anterior and posterior ethmoid arteries superiorly. The nasal septum also derives its blood supply from the sphenopalatine and anterior and posterior ethmoid arteries with the added contribution of the superior labial artery (anteriorly) and the greater palatine artery (posteriorly). The Kiesselbach plexus, or the Little area, represents a region in the anteroinferior third of the nasal septum where all three of the primary blood supply to the internal nose converge ( Figure 16-4 ).
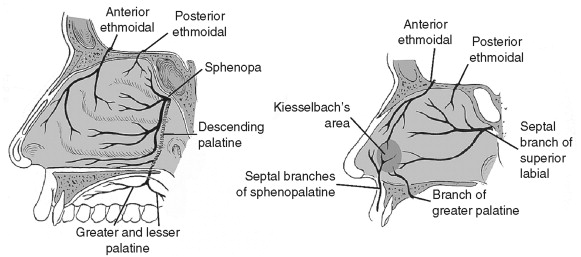
Veins in the nose essentially follow the arterial pattern. They are significant for their direct communication with the cavernous sinus and for their lack of valves; these features potentiate the intracranial spread of infection. Even with the abundant blood supply of the nose, smoking does compromise postoperative healing.
Lymphatics arise from the superficial mucosa and drain posteriorly to the retropharyngeal nodes and anteriorly to the upper deep cervical nodes and/or submandibular glands.
Nerves
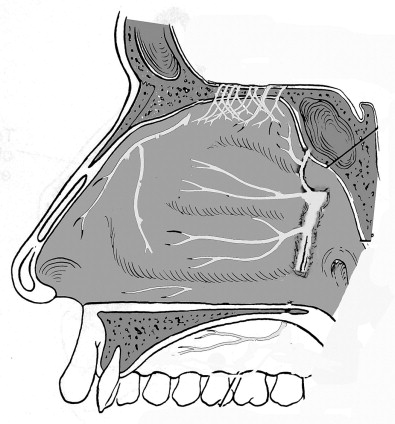
The sensory innervation to the nose is from the trigeminal nerve while the motor supply to the nasal muscles is from the facial nerve. Sensory branches are from both the first and second divisions of the trigeminal nerve. Branches of the first division of cranial nerve V are the infratrochlear and external nasal branches of the anterior ethmoidal nerve. The supratrochlear nerve contributes slightly to the bridge of the nose. The infraorbital nerve supplies the inferolateral regions and the tip. The nasal septum is innervated by the anterior ethmoidal, nasopalatine, and maxillary nerves ( Figure 16-5 ).
DIAGNOSIS AND EVALUATION OF NASAL FRACTURES
A thorough evaluation of nasal fractures is mandatory before embarking on any kind of treatment. Many of the post-traumatic nasal deformities are attributed to incomplete examination. History includes inquiring about the mechanism of injury, time elapsed, and previous nasal fractures or nasal surgery. Head injury must be ruled out first. Proper lighting, a nasal speculum, and a vasoconstrictor are required. History of epistaxis is important because it indicates mucosal injury. A complete examination of the naso-orbital-ethmoid (NOE) complex and visual acuity is mandatory. Increased intercanthal distance is a good indicator of a concomitant NOE complex fracture. Examination of other facial bones is undertaken to rule out other facial fractures. The nose is examined for gross deformity and external lacerations. Gentle palpation of the nasal bones provides an idea of the underlying mobility. Marked edema may mask an underlying nasal deformity. Review of old photographs or a driver’s license can be very helpful. Intranasal examinations require a minimum of a nasal speculum. Rhinorockets or Afrin-soaked pledgets may be used for vasoconstriction. The examiner should look for mucosal lacerations and septal hematoma ( Figure 16-6 ). A complete assessment of the nasal septum is the most important determinant of the outcome of nasal reduction. About 1% to 4% of the general population has some degree of septal deviation. The entire septum is evaluated including dislocation of septal cartilage from the maxillary groove, and deviation or mobility is noted. Rohrich describes the pattern of fracture-dislocation of the septum in low-velocity injuries to be along the vomerine groove.

High-velocity injuries tend to result in more extensive fractures of the quadrangular septal cartilage and perpendicular plate of the ethmoid. Following fracture, nasal bones unite in the direction of the deviated septum; therefore proper alignment of the septum is the key to adequate nasal reduction. Rohrich et al developed a nasal fracture data sheet that is comprehensive of all the pertinent points to consider for minimizing further nasal fracture deformities. They have also adopted a simple nasal fracture classification based on physical examination. They classify nasal fractures into simple, comminuted, complex (associated septal hematoma or open laceration), and associated NOE fractures. Haug and Prather designed a different classification of nasal fracture based on the specific bones fractured.
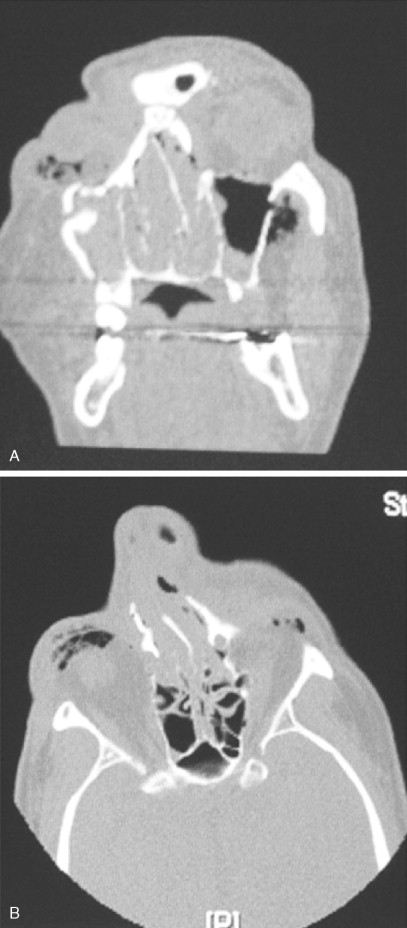
The use of plain images and, recently, computed tomography (CT) scans for the diagnosis and management of nasal fractures has been controversial; however, several small studies have shown that use of these modalities is neither cost-effective nor beneficial to the patient or physician. Nasal fractures are usually evident and can be verified by means of careful history-taking and physical examination. Rarely is the radiologic confirmation of these injuries needed. This is because old fractures with bony deformities are very common and can be confused with new fractures. Yabe and colleagues recommended routine preoperative and postoperative x-rays and CT scans, claiming that some slightly depressed nasal fractures are more easily diagnosed on lateral x-rays than on CT scans. Nonetheless, patients determined by x-rays to have displaced nasal fractures are at a higher risk for long-term nasal deformity. Routine radiographs, however, may be important from a medical/legal point of view, but the treatment is predicated on the basis of the physical examination alone. CT scans are indicated when a concomitant NOE or other facial fractures are suspected ( Figure 16-7 ).
Although the use of plain images is not suggested, the preferred examination includes the acquisition of Waters’ and lateral nasal views.
DIAGNOSIS AND EVALUATION OF NASAL FRACTURES
A thorough evaluation of nasal fractures is mandatory before embarking on any kind of treatment. Many of the post-traumatic nasal deformities are attributed to incomplete examination. History includes inquiring about the mechanism of injury, time elapsed, and previous nasal fractures or nasal surgery. Head injury must be ruled out first. Proper lighting, a nasal speculum, and a vasoconstrictor are required. History of epistaxis is important because it indicates mucosal injury. A complete examination of the naso-orbital-ethmoid (NOE) complex and visual acuity is mandatory. Increased intercanthal distance is a good indicator of a concomitant NOE complex fracture. Examination of other facial bones is undertaken to rule out other facial fractures. The nose is examined for gross deformity and external lacerations. Gentle palpation of the nasal bones provides an idea of the underlying mobility. Marked edema may mask an underlying nasal deformity. Review of old photographs or a driver’s license can be very helpful. Intranasal examinations require a minimum of a nasal speculum. Rhinorockets or Afrin-soaked pledgets may be used for vasoconstriction. The examiner should look for mucosal lacerations and septal hematoma ( Figure 16-6 ). A complete assessment of the nasal septum is the most important determinant of the outcome of nasal reduction. About 1% to 4% of the general population has some degree of septal deviation. The entire septum is evaluated including dislocation of septal cartilage from the maxillary groove, and deviation or mobility is noted. Rohrich describes the pattern of fracture-dislocation of the septum in low-velocity injuries to be along the vomerine groove.

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


