Introduction
Cervical vertebral maturation (CVM) methods have been criticized because of their subjective nature. The aims of this study were (1) to analyze the morphometric changes in the outline of the second to fourth cervical vertebrae with growth and (2) to test the validity of the CVM method for determining the mandibular growth peak.
Methods
Lateral cephalograms of 25 participants from ages 10 to 16 years were acquired from the Burlington Growth Study, and the CVM stage was qualitatively determined. Mandibular and cervical vertebral semilandmarks were then digitized, and point distribution models were used to describe the morphometric templates of the vertebrae in relation to chronologic age and the timing of peak mandibular growth. Mixed model analysis was used to determine the relationship between mandibular length, sex, CVM stage, and chronologic age.
Results
Morphometric changes of the second to fourth cervical vertebrae during growth were consistent with the CVM descriptions. However, mandibular length changes were not significantly associated with CVM stages after adjusting for chronologic age. Morphometric templates of vertebral shapes before and during the mandibular growth peak were similar, with changes detectable only after the growth peak had passed. Morphometric vertebral shape changes varied between the sexes.
Conclusions
Morphometric changes of the cervical vertebrae and the CVM method could not accurately identify the mandibular growth peak.
Highlights
- •
Morphometric changes of cervical vertebrae are consistent with the CVM descriptions.
- •
Morphometric vertebral changes do not accurately identify the mandibular growth peak.
- •
Morphometric vertebral changes can be detected only after the mandibular growth peak.
The importance of the determination of periods of accelerated growth to the timing of dentofacial orthopedics has been often advocated. To date, evaluations of secondary sex characteristics, height and weight, hand-wrist maturation, and dental development have been used as alternatives to chronologic age. The usefulness of the evaluation of skeletal maturity using the second (C2), third (C3), and fourth (C4) cervical vertebrae has also been widely investigated, since the vertebrae can be seen on conventional lateral cephalometric radiographs even when a protective collar is worn. Despite controversy surrounding the specific radiation dose, a major advantage of the cervical vertebral maturation (CVM) methods over other maturation methods, such as the hand-wrist method, is that they eliminate the need for additional radiation exposure. The so-called CVM methods are based on the shape and size of changes of the cervical vertebrae with growth.
It has often been suggested that concavities in the inferior borders of C2 through C4 increase with age, and that C3 and C4 increase in height and become less trapezoid and more rectangular with time. However, these reported changes in vertebral shapes are mostly based on subjective evaluations. Hence, there has been criticism over the reproducibility and qualitative nature of maturational assessments from current cervical maturation methods.
Quantitative analytical methods are more useful than qualitative methods because they are accurate, allow numeric comparisons between groups, and do not rely on individual interpretations. Point distribution models have been shown to be a useful way of quantitatively describing shape for a variety of purposes. Point distribution models are a type of active shape model that derives the statistics of a set of labeled points or “semilandmarks.” After scaling and aligning all sets of data points, we can find the typical semilandmark position using an assigned weighting. After this, the shape template of an object can be determined in a quantitative way.
The aim of this study was to analyze and quantitatively describe the morphometric changes in the outlines of C2, C3, and C4 between the ages of 10 and 16 years, as seen on lateral cephalograms. Furthermore, we tested the validity of the assumptions underlying the CVM method and its relationship to observed changes in the mandibular length during growth.
Material and methods
Participants were selected from the records of the Burlington Growth Study, housed in the American Association of Orthodontists Foundation Craniofacial Growth Legacy Collection. At the time of data collection, 67 participants were available for downloading. Subjects were selected for inclusion if they had at least 5 of 6 lateral cephalograms available in the collection taken at ages 10, 11, 12, 13, 14, and 16 years, and if C2 through C4 were visible on all films. Exclusion criteria were incomplete records, radiographs of poor diagnostic quality, subjects with known craniofacial (or other) conditions or syndromes, and subjects treated orthodontically. Twenty-five participants (13 boys, 12 girls) fulfilled these criteria and were included in the study. The mean ANB angle for them was 3.9° (standard deviation, 1.9°). Images were scaled according to the American Association of Orthodontists guidelines. One principal investigator (S.G.) performed all data collection and the initial analysis after training and calibration.
Qualitative visual analysis was conducted for each head film to determine the CVM stage; this method has been previously described. Semilandmarks were digitized and then converted to Cartesian coordinates using MATLAB software (R21012; MathWorks, Natick, Mass). A total of 63 mandibular and cervical semilandmarks were identified and analyzed per radiograph.
The reliability of the 4 mandibular semilandmarks was assessed ( Fig 1 , A ). Mandibular length was measured using the distance between articulare and gnathion for each year-long time period. The distance was preferred to the distance from condylion to gnathion because of greater reliability.

Fifty-five semilandmarks were used to trace the inferior border of C2 and the outlines of C3 and C4 ( Fig 1 , B ). One point was placed on each corner of the vertebra, and 5 equally spaced points were placed between each corner along the x-axis for the superior and inferior borders, or the y-axis for the anterior and posterior borders. When a semilandmark was to be placed on the corner of a vertebra with a curvature, 2 lines of best fit were taken along the adjacent edges, and the angle was bisected so that the semilandmark was placed on the midpoint of the curvature. The assumptions of the CVM methods were tested in a separate study.
Intraobserver reliability of cervical and mandibular semilandmarks and CVM stage was evaluated by duplicate assessments of 25 cephalograms over a 4-week period. One image was randomly selected from each participant. The assessor (S.G.) was blinded to the chronologic age and sex of the participants. Agreement for the CVM staging was determined using the percentage of agreement, as well as unweighted and weighted kappa statistics.
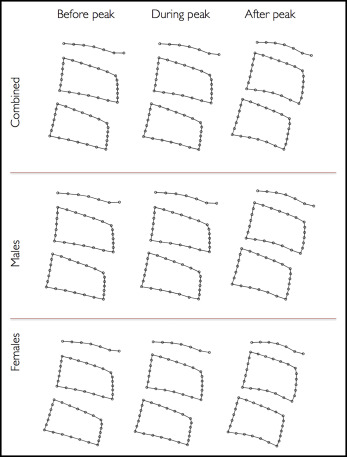
Data were clustered according to chronologic age. In addition, 3 more clusters were formed with regard to mandibular growth: before peak, during peak, and after peak. In each cluster, each shape was defined by “n” points (semilandmarks) in 2-dimensional space. Using Procrustes analysis, which finds the minimum of the least-squared error of all shapes in the same cluster subject to scale, rotation, and translation, we constructed a point distribution model as described by Cootes et al. After this, a vertebral template was made for each vertebra by finding the mean semilandmark point after aligning the shapes in each cluster ( Fig 1 , C ). All morphometric analyses were carried out for the sexes together and separately.
Mixed model analyses were used to determine the relationships between mandibular length, sex, CVM stage, and chronologic age. Mandibular length represented the response variable, and sex and CVM stage were entered as covariates. A term for subject was included as a random effect. An interaction term between CVM stage and sex was also entered into the model. A diagonal correlation matrix was used when implementing the mixed model.
The data were analyzed with the Statistical Packaging for the Social Sciences (version 19; IBM, Armonk, NY), and we set type I error at 0.05 (2-tailed).
Results
Cervical semilandmarks could be reliably identified over duplicate measurements; the standard deviations ranged from 0.2 to 0.3 mm for the x-axis and from 0.3 to 0.4 mm for the y-axis. Mandibular semilandmark reliability for articulare was 0.6 mm for the x- and y-coordinates; for gnathion, reliability was 0.4 mm for the x- and y-coordinates, compared. Condylion had poor reproducibility, at 1.4 and 2.1 mm for the x- and y-coordinates, respectively. The overall percentage of agreement for the CVM scores was 84%. The unweighted kappa value was 0.80 (95% CI, 0.61-0.97), and the weighted kappa value was 0.89 (95% CI, 0.78-0.99).
Point distribution models were used to find the morphometric templates of C2 through C4 according to chronologic age ( Fig 2 ) and mandibular growth peak ( Fig 3 ). In relation to mandibular growth, the morphometric templates were remarkably similar before and during the peak growth, whereas more distinct differences could be identified after the peak.

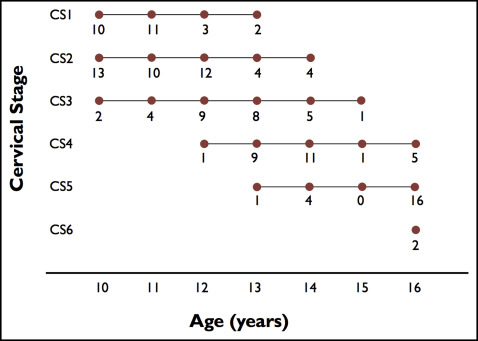
CVM stage was assessed for each cephalogram, and the distribution of all the CVM stages was plotted as a function of chronologic age ( Fig 4 ). As expected, there was a general increase in chronologic age as cervical stage (CS) increased, but the age spans corresponding to the CVM stages were broad: up to 6 years for CS3.

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


