The aims of this article are to introduce mandibular condylar pseudocysts to orthodontists, present 2 relevant case reports, and discuss possible differential diagnoses. Condylar pseudocyst is a radiologic variant of pterygoid fovea, which is the site of insertion of the lateral pterygoid muscle to the head of the mandibular condyle. A pathognomonic picture of a solitary well-defined radiolucency with radiopaque borders, located on the anterior aspect of the condyle in an asymptomatic orthodontic patient, is characteristic.
A panoramic radiograph is frequently used during evaluation of orthodontic patients. This radiograph gives a broad view of the jaws with relatively low radiation exposure. This wide view enables the clinician to identify aberrant tooth numbers and impactions, to estimate the patient’s dental age, and to exclude pathologic lesions of the jaws. The mandibular condyles are visualized in the panoramic radiograph and should be screened by the orthodontist for structure and symmetry.
Radiolucent cystic findings are not uncommon in mandibular radiography. True cysts, of odontogenic or nonodontogenic origin with inflammatory or developmental pathophysiology, must be differentiated from pseudocysts. Radiographically, pseudocysts are radiolucent and well circumscribed, and mostly appear in specific locations of the mandible. With the exception of an aneurysmal bone cyst, which requires resection, the management of other pseudocysts, such as a Stafne static bone cyst or a traumatic (simple) bone cyst, is conservative and includes either observation only or minimal surgical intervention.
Another location for pseudocystic appearance is the anterior aspect of the mandibular condyle. The aims of this article are to introduce this common phenomenon to orthodontists, present 2 relevant case reports, and discuss possible differential diagnoses.
Case reports
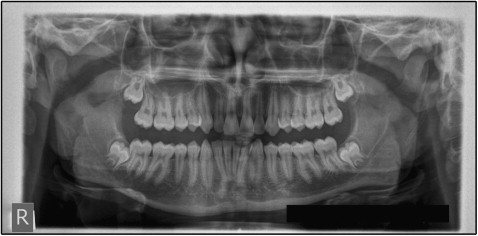
A 14-year-old boy came for an orthodontic consultation with the complaint that his anterior teeth were “not straight.” A full orthodontic evaluation was conducted. A panoramic radiograph showed an ovoid radiolucency with well-circumscribed sclerotic margins in the anterior aspect of the right mandibular condyle, with no apparent degenerative changes ( Fig 1 ). The lesion’s location and appearance were consistent with a condylar pseudocyst. An orthodontic treatment was planned and offered. The condylar finding was recorded and will be observed.
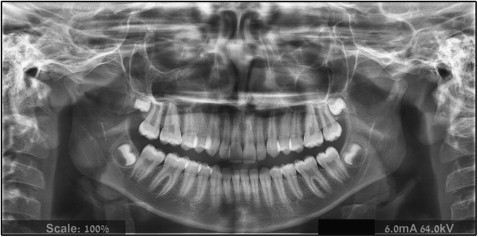
An 11-year-old girl came for an orthodontic consultation complaining about protruding maxillary incisors. A full orthodontic evaluation was conducted. Evaluation of the panoramic radiograph showed a radiolucent lesion on the anterior aspect of the right condyle. In its posterior border, the lesion was well defined with a radiopaque margin. A radiopaque area, with central radiolucency, was observed on the left condyle. No degenerative changes of the condyles were observed ( Fig 2 ). The radiolucency was only partially defined by the radiopaque border. The lesion’s location and appearance were consistent with the diagnosis of condylar pseudocyst. An orthodontic treatment was planned and offered. The condylar findings were recorded and will be observed.
Discussion
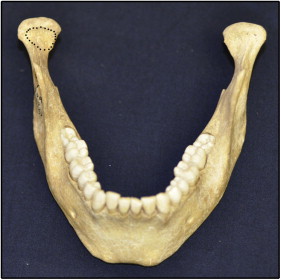
A condylar pseudocyst is a radiologic variant of a pterygoid fovea, which is the site of insertion of the lateral pterygoid muscle to the head of the mandibular condyle ( Fig 3 ). The image of the fovea is magnified and distorted in a panoramic radiograph because of the angle of the x-ray beam, which passes obliquely through the condylar head. Friedlander et al first described this phenomenon in 1992. Obviously, after the diagnosis of a condylar pseudocyst, no invasive treatment is needed; the diagnosis, however, can be a challenge for the clinician. On the one hand, surgical exploration of the condyle to obtain a speciman for histopathologic examination can result in unnecessary functional and esthetic damage. On the other hand, misdiagnosis of a “true” pathologic lesion can lead to a deleterious result.
The prevalences of condylar pseudocysts were found to be 1.8% and 1.5% in adult and young patients, respectively. Friedlander et al and Collins et al confirmed the diagnosis by sequential panoramic radiographs after 4 to 6 months or by computed tomography imaging. The differential diagnosis suggested by these authors includes osteochondroma, multiple myeloma, central giant cell lesion, simple bone cyst, aneurysmal bone cyst, and eosinophilic granuloma. However, a solitary radiolucent corticated cystic lesion, restricted to the anterior aspect of the condyle in the panoramic radiograph, is not a match with the radiographic appearance of osteochondroma and multiple myeloma, which are lytic lesions with undefined ragged borders, or multiple small defined lesions with no sclerotic borders, respectively. Central giant cell lesions, eosinophilic granulomas, aneurysmal bone cysts, and simple bone cysts are extremely rare in this location, with only 4, 10, 11, and 13 cases, respectively, documented so far in the English literature. Moreover, it seems that a simple bone cyst is a self-limited pathology; thus, surgical intervention might not be needed.
In our opinion, a clinician should also consider degenerative changes of the condyle (eg, osteoarthritis) in the differential diagnosis. However, even when radiologic degenerative changes of the condyle are observed in an asymptomatic patient (a condition defined as “osteoarthrosis” according the Research Diagnostic Criteria for Temporomandibular Disorders ), no medical intervention is usually needed. Friedlander et al and Collins et al further studied all the condylar cystic lesions; in all cases, the cystic lesions were the radiologic images of the pterygoid fovea; no true pathology was found.
The condylar pseudocyst has never been described in the orthodontic literature and, apparently, is not known to orthodontists. Since true cystic lesions in the mandibular condyle are extremely rare and mostly manifest as external swelling or asymmetry accompanied by pain or tenderness, we suggest that what appears to be a solitary radiolucent corticated cystic lesion, restricted to the anterior aspect of the condylar image seen on the panoramic radiograph of an asymptomatic orthodontic patient, is sufficient for a diagnosis of condylar pseudocyst. This eliminates the need for further imaging with unacceptable and unnecessary radiation exposure, especially in young patients. However, comparison with previous panoramic radiographs and clinical (and during routine orthodontic radiographic) follow-ups are strongly recommended.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


