Introduction
The use of miniscrews as anchorage has become increasingly popular, but there is no consensus on the best insertion angle. The purpose of this study was to determine the impact of insertion angle on implant primary stability.
Methods
Sixty-four miniscrews, 6 × 1.6 mm, were placed in 64 fresh bone segments from 32 sheep mandibles. The miniscrews were inserted into the bone surface at 4 angles: 30°, 45°, 60°, and 90°. The maximum resistance forces of miniscrews in pullout and shear tests were determined as primary stability using a universal testing machine.
Results
In the pullout tests, the 90° insertion angle had the highest primary stability. Oblique angulations of the miniscrews resulted in lower resistance. In the shear tests, angulations of the miniscrews from 90° to 45° led to increased primary stability. A more oblique insertion (30°) resulted in reduced primary stability.
Conclusions
The direction of the applied force had a significant impact on the primary stability of miniscrews at various insertion angles. The highest primary stability values were achieved at 45° when the miniscrews were loaded by shear force and at 90° when pullout force was applied.
Highlights
- •
Screw angulation was in occlusogingival direction (orthogonal to shear force).
- •
The impact of insertion angle on miniscrew primary stability depends on axial load direction.
- •
In the pullout test, insertion at 90° into the buccal surface has the greatest primary stability.
- •
In the shear test, a 45° insertion angle has the greatest primary stability.
Anchorage is an important part of successful orthodontic therapy. In some cases, absolute anchorage is necessary for treatment. The use of miniscrews has been recognized as an alternative method for anchorage control. Miniscrews have several advantages over conventional implants (ie, dental implants), including smaller size, relatively simple implantation and removal procedures, lower costs, and less pain after placement. Therefore, miniscrews have become frequently used. However, their success rates are lower than those of conventional implants.
Implant stability immediately after insertion is called primary stability. Primary stability has also been defined as the mechanical interlock between bone and implant. Primary stability is an important factor in the success rate of implants.
Establishment of good primary stability is a pivotal factor in the immediate loading of implants. The primary stability of miniscrews is determined by several factors, including thickness, volume, and density of cortical bone; the patient’s age; operational techniques; diameter of the implant and angle of insertion; insertion location; predrilling (depth and diameter); and implant design.
Primary instability may lead to weakening of the screw-bone interface and failure. This failure necessitates reinsertion of a screw that is associated with adverse effects such as tissue damage, inflammation, and pain and discomfort. As a result, use of an insertion method to achieve the highest primary stability is an important goal in contemporary orthodontics. The alveolar ridge is the most frequently used site for miniscrews. However, the risk of root injury should not be underestimated. Oblique rather than perpendicular insertion is recommended to prevent root contact. Some studies have shown that the insertion angle had no significant influence on miniscrew survival.
But other studies have demonstrated the impact of the insertion angle on the primary stability of miniscrews. Some investigators have suggested that oblique placement reduces primary stability and have recommended perpendicular insertion. However, others have argued that the angulation of the miniscrew increases cortical bone support and thereby better primary stability.
Therefore, there is no consensus on miniscrew insertion angle.
The authors of some studies have applied various techniques: resonance frequency and placement insertion torque to measure the primary stability of the miniscrews. However, pullout and shear tests have recently been used for this purpose. To the best of our knowledge, most previous investigations have applied mesiodistal angulation and not assessed the occlusogingival direction.
In this study, we aimed to determine the impact of 4 clinically advocated insertion angles on miniscrew primary stability.
Material and methods
Thirty-two fresh sheep mandibles were collected for miniscrew insertion. All sheep were adult males about the same size. None had any remarkable diseases. All were obtained from a slaughterhouse in Tehran, Iran. The review board of the School of Dentistry of Shahed University approved this study plan.
The mandibles were denuded from the soft tissues and stored in a solution containing equal amounts of normal saline solution and 70% ethanol at 4°C. This is a suitable method for preserving the mechanical and elastic properties of bones. The tests were done within the first 24 hours after the animals’ deaths. The edentulous segment between the incisors and the premolars was selected for implant insertions. Segments with similar shape and morphology of the buccal surfaces were selected. Then 64 segments of bone were cut with at least a length of 20 mm. One implant was inserted per segment. These segments were embedded in resin (ProBase; Ivoclar Vivadent, Schaan, Liechtenstein) except for the buccal surface. Resin blocks with dimensions of 2 × 5 × 2.8 cm were prepared. To avoid overheating the bone, resin block curing was done under water. Eight blocks were assigned for each insertion angle: half for the pullout tests and the other half for the shear tests. A custom holder was built for grabbing the blocks. The walls of the blocks were trimmed to be parallel and flat. A custom x-y table was mounted on the custom holder. For precise insertion, 4 metal plates were made with 4 guiding-canal angles (30°, 45°, 60°, and 90°). The width of the metal plate guiding canals was constructed almost equal to the width of the handhold screwdriver head, and the length was 10 mm.
Pilot drillings were carried out at a depth of 1 mm in the center of the buccal cortex with the predetermined angle for each group test. The miniscrews underwent only 1 test. A total of 64 miniscrews (16-G2-006, Dual-Top G2; Jeil Medical, Seoul, Korea) with the same size (1.6 × 6 mm) were placed in the prepared bone segments at angles of 30°, 45°, 60°, and 90° to the buccal surface. The design test matrix consisted of 8 groups of 8 implants each: 4 groups for pullout tests and 4 groups for shear tests. Using the metal plates, we placed the implants with a handhold screwdriver (111-010; Jeil Medical) and a driver shaft (113-GD-I0l; Jeil Medical). The miniscrews were driven in until the soft tissue cap reached the bone surface. Upon completion of the insertion process, a conventional dental radiograph was taken to (1) measure the cortical bone thickness and (2) evaluate the insertion angle to the buccal cortex and confirm that the implant did not contact the lingual cortex. The thickest part of the buccal cortical plate on each radiograph was considered an indicator of the quantity of bone. It was necessary to compensate for enlargement of the cortical thickness. This was done by measuring the length of the miniscrew in the radiograph and its actual size (8 mm). A simple proportional relationship was then set up:
apparent thickness of bone ( radiograph ) true thickness of bone = apparent length of miniscrew ( radiograph ) true length of the miniscrew
The insertion angle was measured at the intersection of 2 lines: the longitudinal axis of the miniscrew and another line tangential to the buccal surface.
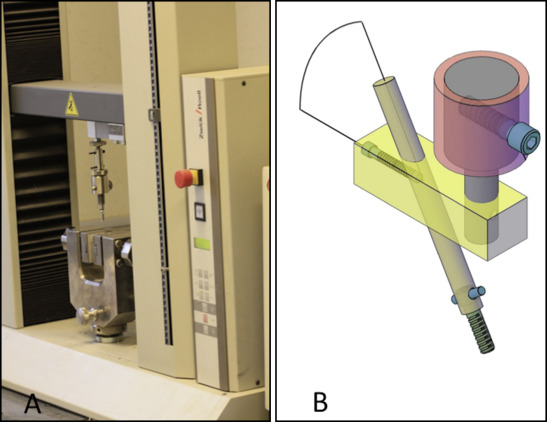
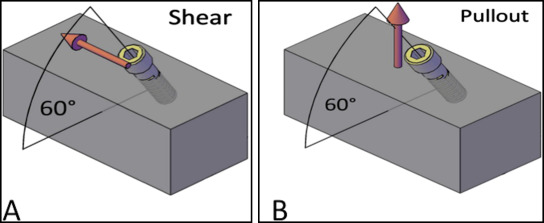
The pullout (tensile) and shear tests were done on the inserted implants using a universal testing machine (Z020; Zwick/Roell, Ulm, Germany). To apply the desired load to the screws, 4 custom miniscrew holders were designed (1 for each insertion angle) to grab the miniscrews. These holders comprised 2 parts. The upper parts were attached to the load cell, and the lower parts were integrated with miniscrews ( Fig 1 , A ). The lower part was a cylinder with an internal diameter of 2.91 mm (maximum width of miniscrew head, 2.90 mm). An 0.85-mm hole was drilled in the lower part at 0.5 mm from the base ( Fig 1 , B ). The angle between the upper and lower parts was similar to the predetermined test (ie, when the insertion angle was 30°, the angle between the upper and lower parts was 30°). So the directions of loading were parallel to the alveolar surface in the shear tests and perpendicular in the pullout tests ( Fig 2 ). The implant heads were placed in the custom miniscrew holder and secured by passing an 0.8-mm hard stainless steel wire (Dentarum, Ispringen, Germany) through the implant head hole and the lower part hole. All tests were done with a 2-N preload to minimize any play between the implant and the holder. A custom x-y-z table was mounted on the lower jaw of the testing machine to check the accuracy and to recognize any deviation during testing. All tests were done at room temperature (22°C). During testing, the bone blocks were kept moist with a wet paper wrapped around them.
The tests began with a crosshead speed of 0.05 mm per second. The tests were discontinued when the implant failed. Full pullout of a miniscrew was considered the failure point. For each test, the maximum force before the failure point was recorded as the primary stability. The test results were collected digitally for all samples. The second author (A.G.) prepared the samples and performed the tests.
Statistical analysis
Statistical analysis was performed with SPSS software (version 16; SPSS, Chicago Ill). The Shapiro-Wilk test was used to clarify whether the variables were normally distributed. If the variables’ distribution was normal, 1-way analysis of variance (ANOVA) with post hoc Tukey tests was applied for comparison of the pullout maximum force, the shear maximum force, and the bone thickness. Correlations between the insertion angles and the mechanical tests were analyzed using the Pearson correlation test. The level of significance of 0.05 was used for the comparisons.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


