Introduction
The objective of this prospective trial was to compare the clinical effectiveness of bonded retainers with vacuum-formed retainers, in terms of maintaining the results of orthodontic treatment in the lower arch up to 18 months post debond.
Methods
This was a hospital-based, prospective randomized controlled clinical trial in which a total of 82 subjects were randomly allocated using a computer-generated number sequence to 1 of 2 groups, receiving either a vacuum-formed retainer (Essix Ace plastic (120 mm; DENTSPLY Raintree Essix, Sarasota, Fla) or a bonded retainer (0.0175 coaxial archwire (Ortho-Care, UK, Shipley, United Kingdom) bonded in place with Transbond LR (3M United Kingdom, Brachnell, United Kingdom) for the mandibular arch. Each number was placed in an opaque, concealed envelope and chosen randomly by the study subject; this determined the allocation group. Eligibility criteria included patients nearing debond after treatment with 0.022 × 0.028-in slot size preadjusted edgewise fixed orthodontic appliances whose pretreatment records and study models were available to confirm pretreatment labial segment crowding or spacing and who had clinically acceptable alignment at the end of treatment. The main outcome was to investigate the clinical effectiveness of the 2 types of retainers in terms of changes in incisor irregularity at 6 months of retention. The following measurements were recorded at each time point (6, 12, and 18 months) with a digital caliper: Little’s irregularity index, intercanine width, intermolar width, arch length, and extraction site opening. Blinding was applicable only at debond because of the permanence of 1 intervention.
Results
The 2 groups were well matched with respect to age, sex, clinical characteristics, and treatment plans. There was a statistically significant difference between the groups for changes in Little’s irregularity index at 6 months, with the vacuum-formed retainer group showing greater changes than the bonded retainer group ( P = 0.008). There was no statistically significant difference between the groups for changes in Little’s irregularity index at 12 and 18 months.There were also no statistically significant changes at any time for intercanine width, intermolar width, arch length, or extraction site opening.
Conclusions
Some relapse is likely after fixed appliance therapy irrespective of retainer choice, and this is minimal in most patients at 6 months after debond. Bonded retainers have a better ability to hold the mandibular incisor alignment in the first 6 months after treatment than do vacuum-formed retainers.
Registration
Not applicable.
Protocol
The protocol was not published before trial commencement.
Funding
There is no funding or conflict of interest to be declared.
Highlights
- •
The clinical effectiveness of bonded and vacuum-formed retainers was compared.
- •
Bonded retainers maintained better mandibular incisor alignment in the first 6 months.
- •
Changes in the first 18 months were minimal in both groups.
The goal of orthodontic treatment is to produce an ideal occlusion that is morphologically stable, esthetic, and functional. Despite proper diagnosis and carefully rendered treatment mechanics, the results achieved at the end of active treatment are not necessarily stable over the long term.
Posttreatment relapse is perhaps the most common risk of orthodontic treatment, and planning for postretention stability should be part of the initial treatment plan and discussed with the patient during the informed consent process before treatment, so that any relapse is not a disappointment for either the clinician or patient.
Stability and relapse, in both treated and untreated malocclusions, have been studied intently over many years, and the long-term results have been similar and not hugely optimistic. Sadowsky and Sakols followed patients on average for 20 years postretention and found that 9% had an increase in mandibular crowding when compared with pretreatment, and 73% had dental relationships “outside the norm.” Similarly, Little et al noted that only 10% of patients had maintained satisfactory mandibular incisor alignment at 20 years postretention.
This previous research demonstrates that the only apparent guarantee of long-term stability is long-term retention. This is due to the variety of factors that are reported to affect tooth positions in both treated and untreated malocclusions. These include skeletal and soft tissue growth ; dental factors ; treatment mechanics such as changes in arch form, length, width, and treatment plan ; final interdigitation ; and functional occlusion, as well as elements of the pretreatment malocclusion.
Retention is necessary to allow reorganization of the gingival and periodontal tissues affected by orthodontic tooth movement, to prevent unwanted movement as a result from growth changes, and to prevent the relapse tendency of teeth that have been moved to an inherently unstable position.
In the United Kingdom, the most common types of retention appliances are vacuum-formed retainers, Hawley retainers, and bonded retainers, with the latter the most frequently used by private practitioners; the former are more commonly prescribed by the National Health Service. A similar study in the United States found that a maxillary Hawley and a mandibular bonded retainer were the most popular. In a trial carried out in a specialist practice in the National Health Service, Hichens et al reported that a vacuum-formed retainer was preferred by the patients over Hawley retainers. Cerny eta al identified a patient preference for bonded retainers in private practice. More recently, social perceptions of intellectual ability and attractiveness have also been found to be influenced by retainer design and appearance.
Previous prospective research evaluating the clinical effectiveness of removable retention is limited. In a trial reported by Rowland et al, a statistically significant difference was found between the clinical effectiveness of vacuum-formed retainers and Hawley retainers, with the vacuum-formed group more successful in maintaining posttreatment alignment of the anterior teeth after 6 months.
Previous research involving bonded retention has been mainly retrospective, and the few available prospective studies have investigated failure rates and dental health associated with fixed retainer types as opposed to their clinical effectiveness. It was noted in 1 study that thin multistranded wires were superior for maintaining mandibular incisor positions compared with a thicker wire and a prefabricated wire.
There is 1 prospectively designed trial comparing bonded and vacuum-formed retainers up to 24 months after debond. In these studies, it was reported that a prefabricated positioner used as a retainer showed a statistically significant difference in its inability to maintain incisor positions after treatment (measured with Little’s irregularity index) compared with a vacuum-formed retainer or a bonded retainer after 6 months, but no statistically significant difference was found after 2 years.
Retention type and duration of wear are also ongoing contentious issues in the specialty. Two Cochrane reviews have been published on relapse; the latest reviewed the management of relapse and found no study to include in the review. The former review identified limitations to previous research on retention type including short follow-up periods, inappropriate or no controls, retrospective designs, and insufficient or irrelevant data. Thus, both highlighted the need for randomized controlled trails in this area to aid in determining the most effective and safe method for managing the relapse of alignment of the mandibular front teeth.
The purposes of this study were to quantify and compare the changes in a number of intra-arch variables with vacuum-formed retainers and bonded retainers from debond to 6, 12, and 18 months and to determine whether 1 type of retainer is superior to the other in terms of maintaining the orthodontic results. These particular retainers have to date not been directly compared in a randomized controlled trial.
Specific objectives and hypotheses
The main aim of this randomized controlled trial was to compare the clinical effectiveness of 2 types of orthodontic retainers in the mandibular arch in terms of retention of the treated results at 6 months after debond. More specifically, our aim was to determine whether there are any differences in the clinical effectiveness of vacuum-formed retainers compared with bonded retainers in maintaining alignment in the mandibular labial segment (Little’s irregularity index) at 6 months after debond. Also, we aimed to investigate whether there are any differences in the clinical effectiveness of vacuum-formed retainers compared with bonded retainers in maintaining arch width (intercanine width) and intermolar width, arch length, and extraction site closure. In addition to the 6-month time point, 12 and 18 months were also considered because previous retrospective studies have shown that most relapse after orthodontic treatment occurs within the first 12 months after debonding of the appliances.
The null hypothesis tested in this study was that there is no difference in the ability of both types of retainers to retain the treated result in the short and medium terms.
Material and methods
Trial design
This was a hospital-based parallel design randomized controlled clinical trial.
Participants, eligibility criteria, and setting
Ethical approval was granted by the National Research Ethics Services Committee (reference number, 10/H0713/57).
The study population was drawn from patients nearing debond after treatment with 0.022 × 0.028-in slot size preadjusted edgewise fixed orthodontic appliances who fulfilled the following inclusion criteria: (1) patients nearing debond of fixed orthodontic appliances, (2) records and study models available to confirm the pretreatment labial segment crowding or spacing, and (3) clinically acceptable alignment at the end of treatment (no clinically detectable contact point displacement).
The exclusion criteria were the following: (1) patients who completed treatment early or had repeated breakages during treatment, (2) patients with poor oral hygiene during treatment, (3) patients with prosthodontic needs in the mandibular arch after treatment, (4) patients with a history of periodontal disease, and (5) patients with a learning difficulty.
Subjects who fulfilled the selection criteria were identified and invited to take part in this study. Informed consent and assent were obtained on the day of debond.
Enrollment started in January 2011 and was completed by February 2012. Eighty-five subjects were entered into the trial, but during recruitment 1 declined to take part and 2 more subjects did not meet the inclusion criteria. Therefore, 82 subjects were recruited in total. At the debond appointment after appliance removal (T0), a set of alginate impressions was taken for study models, and an additional polysilicone impression of the mandibular arch was taken to obtain measurements for this study. The polysilicone impression was then cast in hard stone (type III) in the laboratory on the same day. All subjects were then randomized into the intervention groups.
Interventions
The vacuum-formed retainer was constructed from Essix Ace plastic (120 mm in diameter, 0.03 in thick; DENTSPLY Raintree Essix, Sarasota, Fla). This was fabricated by a qualified orthodontic technician under standardized conditions, using the same technique and the same machine for each retainer made for this study. This was fitted within 7 days with instructions for full-time wear for the first 6 months followed by 6 months of nighttime wear and a further 6 months of alternate-night wear, which was the department protocol after delivery of retainers.
For the bonded retainer group, the teeth were polished with pumice, and scaling (Cavitron; DENTSPLY International, York, Pa) was used if deemed necessary. A 0.0175-in stainless steel coaxial archwire (Ortho-Care UK, Shipley, United Kingdom) was formed at chairside to fit passively against the mandibular labial segment from canine to canine, using a 37% phosphoric acid etch followed by copious washing, drying, and application of an adhesive primer (OrthoSolo bonding agent; Ormco, Orange, Calif), which was subsequently cured. The wire was then bonded with Transbond LR composite material (3M United Kingdom, Bracknell, United Kingdom).
All subjects were reviewed by a member of the research team (N.O’R. or H.A.), and a mandibular arch dental impression was taken with polysilicone at 6 months (T1), 12 months (T2), and 18 months (T3) to obtain stone models for measurement purposes.
When patients lost their retainers, new impressions and retainers were provided. When there was appliance breakage or loss, the patients were advised to attend the daily emergency clinic, where a new appliance was made; bonded retainers were repaired.
Outcomes (primary and secondary and any changes after trial commencement)
All measurements were made manually with a digital caliper (150 mm DIN 862, ABSOLUTE Digimatic caliper, model 500-191U; Mitutoyo, Andover, Hampshire, United Kingdom) with a resolution of ±0.01 mm. The arch was viewed from above, the caliper was held parallel to the occlusal plane, and the distance between the contact points of the caliper was recorded.
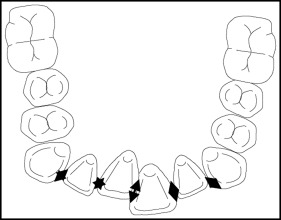
Irregularities of the mandibular incisors were measured on the study models at T0, T1, T2, and T3 using the method described by Little ( Fig 1 ).
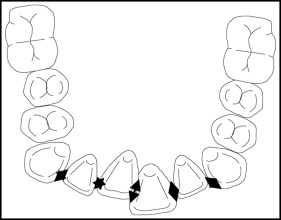
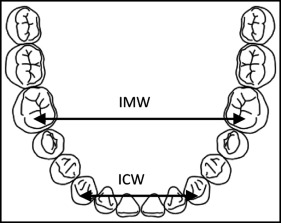
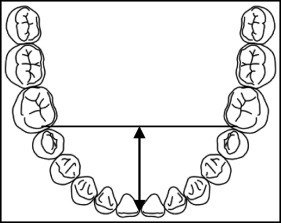
Intra-arch measurements included intercanine width, which was measured as the distance between the 2 canine cusp tips; in case of cuspal wear, an estimation of the middle of the surface was made ( Fig 2 ). Intermolar width was measured as the distance between the mesiobuccal cusp tips of both mandibular first molars; similarly, if the cusps tips were worn, an estimation of the middle of the surface was made ( Fig 2 ). Arch length was measured at a point midway between the incisal edges of the central incisors, bisecting the line connecting the mesial marginal ridges of the left and right permanent molars ( Fig 3 ). The extraction space opening was measured as the sum of contact point displacements in the anteroposterior plane where the extractions were carried out.
All model measurements were collected by 1 investigator (N.O’R.). Random errors and intraoperator reliability were assessed by reproducing 2 sets of measurements on 25 randomly selected study models 2 weeks later.
No harm was observed as a result of either intervention. Unlike previous data in the literature, there was a low failure rate associated with the bonded retainer group over 18 months, with only 3 subjects returning with 1 pad that had debonded. This may have been because most (39 of 42) of the bonded retainers were placed by 1 operator (N.O’R.) under a standardized protocol.
Sample size calculation
The main outcome measure in this study was change in incisor irregularity in the groups after 6 months of retention. Sample size estimation, using PASS 11, showed that a total of 72 participants, 36 in each treatment arm, were required to demonstrate a clinically significant difference in the primary outcome of 0.5 mm between the groups, with 90% power, a standard deviation of 0.79, and an alpha of 0.05, using the Mann-Whitney U test, and with the null hypothesis of equal effect. This calculation was based on a previous randomized controlled trial that identified a treatment effect of 0.5 mm at the 6-month follow-up. In addition, to allow for a potential 15% dropout rate, the sample size was increased to 82 subjects.
Interim analyses and stopping guidelines
No interim analysis was performed during the study. During the protocol stage, we decided that the trial would be stopped if it became obvious that 1 intervention was clinically superior to the other or if any harm came as a result of the interventions.
Randomization
An electronic randomization program was used, whereby a subject allocation sequence was generated using an online computer program ( www.random.org ). The numbers were assigned by the computer to 2 groups that corresponded to 1 of the 2 treatment options to be studied. The random numbers were then placed in opaque envelopes that were identical, tamper-proof, and prepared in advance. One envelope was then selected randomly by the patient and opened. Forty subjects were randomized to the vacuum-formed retainer group and 42 subjects to the bonded retainer group, and all subjects received their allocated intervention.
Blinding
It was not possible to be blinded to the randomization allocation after T0 because of the permanence of a bonded retainer. However, measuring the models in a random order and blinding during data analysis were aimed to minimize bias.
Statistical analysis
Mann-Whitney U tests were performed to allow comparison of the vacuum-formed retainer and bonded retainer groups in relation to the different variables at all time periods. A P value of 0.05 was taken to be statistically significant. Statistical analyses were performed on the available data set. No missing data imputation was carried out.
Intraobserver reliability was assessed by performing measurements for Little’s irregulatiry index at a 2-week interval on 25 casts with intraclass correlation coefficients, which confirmed excellent agreement between the measurements, with 95% of the sample demonstrating an intraclass correlation coefficient between 0.92 and 0.98.
Material and methods
Trial design
This was a hospital-based parallel design randomized controlled clinical trial.
Participants, eligibility criteria, and setting
Ethical approval was granted by the National Research Ethics Services Committee (reference number, 10/H0713/57).
The study population was drawn from patients nearing debond after treatment with 0.022 × 0.028-in slot size preadjusted edgewise fixed orthodontic appliances who fulfilled the following inclusion criteria: (1) patients nearing debond of fixed orthodontic appliances, (2) records and study models available to confirm the pretreatment labial segment crowding or spacing, and (3) clinically acceptable alignment at the end of treatment (no clinically detectable contact point displacement).
The exclusion criteria were the following: (1) patients who completed treatment early or had repeated breakages during treatment, (2) patients with poor oral hygiene during treatment, (3) patients with prosthodontic needs in the mandibular arch after treatment, (4) patients with a history of periodontal disease, and (5) patients with a learning difficulty.
Subjects who fulfilled the selection criteria were identified and invited to take part in this study. Informed consent and assent were obtained on the day of debond.
Enrollment started in January 2011 and was completed by February 2012. Eighty-five subjects were entered into the trial, but during recruitment 1 declined to take part and 2 more subjects did not meet the inclusion criteria. Therefore, 82 subjects were recruited in total. At the debond appointment after appliance removal (T0), a set of alginate impressions was taken for study models, and an additional polysilicone impression of the mandibular arch was taken to obtain measurements for this study. The polysilicone impression was then cast in hard stone (type III) in the laboratory on the same day. All subjects were then randomized into the intervention groups.
Interventions
The vacuum-formed retainer was constructed from Essix Ace plastic (120 mm in diameter, 0.03 in thick; DENTSPLY Raintree Essix, Sarasota, Fla). This was fabricated by a qualified orthodontic technician under standardized conditions, using the same technique and the same machine for each retainer made for this study. This was fitted within 7 days with instructions for full-time wear for the first 6 months followed by 6 months of nighttime wear and a further 6 months of alternate-night wear, which was the department protocol after delivery of retainers.
For the bonded retainer group, the teeth were polished with pumice, and scaling (Cavitron; DENTSPLY International, York, Pa) was used if deemed necessary. A 0.0175-in stainless steel coaxial archwire (Ortho-Care UK, Shipley, United Kingdom) was formed at chairside to fit passively against the mandibular labial segment from canine to canine, using a 37% phosphoric acid etch followed by copious washing, drying, and application of an adhesive primer (OrthoSolo bonding agent; Ormco, Orange, Calif), which was subsequently cured. The wire was then bonded with Transbond LR composite material (3M United Kingdom, Bracknell, United Kingdom).
All subjects were reviewed by a member of the research team (N.O’R. or H.A.), and a mandibular arch dental impression was taken with polysilicone at 6 months (T1), 12 months (T2), and 18 months (T3) to obtain stone models for measurement purposes.
When patients lost their retainers, new impressions and retainers were provided. When there was appliance breakage or loss, the patients were advised to attend the daily emergency clinic, where a new appliance was made; bonded retainers were repaired.
Outcomes (primary and secondary and any changes after trial commencement)
All measurements were made manually with a digital caliper (150 mm DIN 862, ABSOLUTE Digimatic caliper, model 500-191U; Mitutoyo, Andover, Hampshire, United Kingdom) with a resolution of ±0.01 mm. The arch was viewed from above, the caliper was held parallel to the occlusal plane, and the distance between the contact points of the caliper was recorded.
Irregularities of the mandibular incisors were measured on the study models at T0, T1, T2, and T3 using the method described by Little ( Fig 1 ).