Introduction
Placement of mini-implants carries with it the risk of iatrogenic damage to the adjacent root surfaces. The aims of this study were to assess the type of trauma incurred on tooth roots after contact or approximation with mini-implants during placement, and to observe and analyze the healing responses via histologic analysis.
Methods
Four male minipigs were used as experimental subjects. Twenty mini-implants (1.6 × 8 mm) were implanted in each minipig into the buccal sides of all 4 quadrants between the roots of teeth so that contact or approximation between the mini-implant and root surface occurred, with the aid of dental fluoroscopy. All mini-implants on the left side of the mouth were left in situ, and all mini-implants on the right side were removed immediately after placement. The minipigs were killed at 4-week intervals up to week 16, and histologic sections were made.
Results
When mini-implants were left in situ, the root surface was mostly resorbed away from the mini-implant thread. Partial repair started at 8 weeks. When the mini-implant thread was left touching the root, there was no normal healing response. If the mini-implant was placed less than 1 mm from the periodontal ligament, resorption was evident on the root surface. Abnormal healing responses were seen when the pulp tissue was ruptured, mostly through osteodentin formation. In all instances after mini-implant removal immediately after placement, varying degrees of cementum repair was observed.
Conclusions
Immediate removal of the mini-implant leads to cementum repair, whereas leaving the mini-implant in place will cause either a delay in repair or no repair. Placing mini-implants less than 1 mm from the root surface causes root-surface resorption.
Mini-implants are now being extensively used in orthodontic treatment. They have opened up a new field of possibilities for treatment that was nearly impossible before the concept of absolute anchorage became available to us in the form of mini-implants. The small size and ease of placement have made mini-implants user-friendly; they are also relatively comfortable for the patient. The main concerns with mini-implants are the failure rate and potential trauma to the surrounding structures and the consequences of the damage. Potential complications of root injury mentioned in the literature include loss of tooth vitality, osteosclerosis, and dentoalveolar ankylosis. Iatrogenic root damage from mini-implants is an important aspect but has had little attention until recently. Fabbroni et al investigated root contact after transalveolar screw placement for mandibular fractures in a clinical study. Although some implant and root contact occurred, they concluded that the incidence of clinically significant damage appeared to be low. Asscherickx et al found that, after accidental damage to tooth roots in beagles, almost complete repair of the cementum occurred in 18 weeks and started at the earliest 12 weeks after the screw was removed. In a recent study by Kadioglu et al, scanning electron microscopy was used to observe root surfaces after intentional contact between root and mini-implant. They found that most of the repair of root surfaces occurred 8 weeks after removal of the screw or the orthodontic force. Scientific evidence regarding these side effects, especially histologic evaluation of root surfaces, is still lacking in the literature.
Although mini-implants can be placed in various areas of the mouth, the interradicular spaces between adjacent teeth are the most common sites. These sites have an increased risk of causing iatrogenic root damage and require careful planning and consideration before mini-implant placement. In a recent study with computed tomography images, the greatest amount of mesiodistal bone between adjacent roots buccally was 3.5 mm between the first and second premolars. There is also evidence that mini-implants migrate up to 0.5 mm during treatment. This must be considered when choosing sites for placement. Liou et al stated that the minimum distance between the root surface and the mini-implant should be 2 mm to prevent root damage. Maino et al, on the other hand, recommended that a 1-mm clearance between mini-implant and root is sufficient to maintain periodontal health and mini-implant stability.
The extent of root damage from mini-implant contact can be well ascertained from histologic analysis. It is of special interest to observe the different types of responses when the mini-implant is left touching the root surface and when the stimulus has been removed. The aims of this study were to assess the type of trauma incurred on tooth roots after contact or approximation of mini-implants during placement and to observe and analyze the healing responses via histologic analysis.
Material and methods
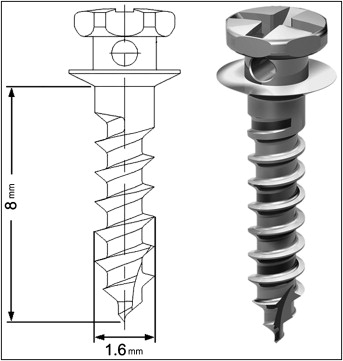
Four male minipigs (specific pathogen-free micropigs) weighing between 31 and 43 kg and aged over 12 months were used as the experimental subjects. A total of 20 mini-implants (16-JA-008H, JA type, Jeil Medical, Seoul, Korea) measuring 1.6 mm in diameter and 8 mm in length were placed in each minipig ( Fig 1 ).
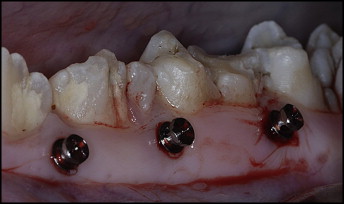
After administration of intramuscular preanesthetic medication, anesthesia was maintained through inhalation of isoflurane (2.0%, Terell isoflurane, Minrad, Orchard Park, NY). The mini-implants were placed into the buccal sides of all 4 quadrants, between the roots of teeth so that contact or close approximation between the mini-implant and root surface occurred ( Fig 2 ). The mini-implants were placed without making incisions in the mucosa and without a separate drilling procedure. If it was uncertain whether contact with the root surface were made or if adequate root approximation was unsuccessful due to thick mucosa, the mini-implants were excluded. To aid in visualizing the roots and the mini-implants, fluoroscopy was used during placement. Fluoroscopy is an imaging technique that uses an x-ray source passed to a monitor to view real-time images of moving structures (40F, Dreamray, Busan, Korea). Lead vests were worn, and exposure times were kept to a minimum. After placement of all mini-implants, 4 tattoo marks were made around each mini-implant in the maxilla and the mandible of the right side. The mini-implants on the right side were removed immediately after placement.
Three fluorochromatic dyes (Sigma, St Louis, Mo) were injected intramuscularly for fluorescent microscopy investigation. Tetracycline hydrogen chloride was administered (15 mg/kg) at 2 weeks and 14 weeks after placement, calcein (10 mg/kg) at 6 weeks after placement, and alizarin red (30 mg/kg) at 10 weeks after placement. The minipigs were killed one at a time at 4-week intervals, for a total experimental period of 16 weeks. After killing each minipig, the specimens of each mini-implant on the left side, and the areas where the mini-implants were removed on the right side, were prepared in the axial plane by using a cutting and grinding system (Exakt Apparatebau, Nordstedt, Germany) according to the method reported by Donath and Breuner. The thickness of the specimens was about 40 to 50 μm. The specimens were stained with hematoxylin and eosin. Each specimen was sectioned so that the contact area between the mini-implant and the root surface was well represented.
Results
Of the total number of mini-implants placed, only the specimens that best represented the contact area between root and implant were analyzed. This amounted to an average of 7 sections per animal for the mini-implants in-situ group, and 3 sections per animal for the mini-implant removed group. The small number of slides meant that statistical analysis was difficult to carry out. Only observational analysis was undertaken.
The observed results were separated into 2 groups: healing of the root surface when the mini-implants were left in situ, and changes in the root surface and surrounding structures after the mini-implants were removed.
A summary of the root healing observed when the mini-implants were left in situ is shown in the Table . The root-contact group was divided into 2 subgroups, the first containing those that made contact or were in close proximity with the dentin or the periodontal ligament (PDL), and the second subgroup included those that penetrated into the pulp. Overall, no teeth showed signs of ankylosis after contact with the mini-implant. A patent PDL space was maintained for all observed specimens throughout the 16-week experimental period. The samples in the root-contact group were further classified into 3 types, and the pulp penetration group into 2 types, according to the type of healing observed.
| Specimens (n) | Percentage of total specimens | |
|---|---|---|
| Root contact only | ||
| Resorption of root in proximity | 2 | 6% |
| Resorption away from thread | 13 | 41% |
| Thread touching root | 11 | 34% |
| Penetration through pulp | ||
| Dentin tissue rupture only | 1 | 3% |
| Dentin rupture + bone-like tissue overgrowth/osteodentin | 5 | 16% |
The root-contact only group included 3 types.
- 1.
Resorption of the root in proximity. Even though direct contact between the root and the implant was not made, resorption of the root surface was observed. The distance between the implant and the root surface was less than 1 mm. Even though there was bone between the implant and the root surface, resorption still occurred on the root surface ( Fig 3 ).
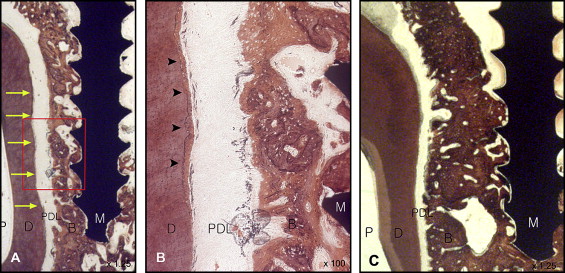
Fig 3 Resorption of the root in proximity (specimen from minipig killed at 4 weeks) and normal specimen. A, Even though direct contact between root and implant was not made, root resorption was observed ( yellow arrows ). The area in the red box shown in B . B, Higher magnification showing cementum deposition on resorbed root surface ( short black arrows ). C, Normal specimen showing implant placed more than 1 mm from the root. No root resorption is seen on the root surface. P , Pulp; D , dentin; PDL , periodontal ligament; B , bone; M , mini-implant. - 2.
Resorption away from the thread. After contact of the implant with the root surface and with time, resorption occurred away from the thread of the mini-implant. There was no bone between the thread and the root surface, just soft tissue resembling the PDL ( Fig 4 ).
Fig 4 Resorption away from the thread (specimen from minipig killed at 12 weeks). A, After contact of the mini-implant was made with the root surface, with time, resorption occurs away from the mini-implant threads. The area in the red box is shown in B and C . B, Higher magnification showing cementum deposition on root surface ( short black arrows ). C, Fluorescent microscopy examination shows repair through tetracycline ( yellow arrow ), calcein ( green arrow ), and alizarin red ( orange arrow ) deposition on root surface. P , Pulp; D , dentin; M , mini-implant. - 3.
Thread touching the root. After contact of the mini-implant thread with the root surface, it stayed in contact with no resorption of the root surface ( Fig 5 ).
Fig 5 Thread touching the root (specimen from minipig killed at 16 weeks). A, Lodging of the mini-implant between adjacent roots with severe force means that the threads of the implant stay in contact with the root surface. The increased force during placement caused slight bending of the mini-implant. B, Higher magnification showing the point of contact between the implant and the root surface ( short red arrows ). There is no evidence of cementum repair. P , Pulp; D , dentin; M , mini-implant.
The penetration through the pulp included 2 types.
- 1.
Dentin-tissue rupture only. No healing response was observed.
- 2.
Dentin-tissue rupture, with osteodentin. There was rapid formation of irregular reparative dentin with cellular inclusions ( Fig 6 ).
Fig 6 Root penetration of mini-implant (specimen from minipig killed at 4 weeks). A, Dentin tissue rupture with osteodentin formation. The area in the red box is shown in B . B, Higher magnification showing rapid formation of irregular reparative dentin ( short yellow arrows ) with cellular inclusions ( long red arrows ). P , Pulp; D , dentin; PDL , periodontal ligament; M , mini-implant; B , bone.
Resorption of the root in proximity was seen in specimens at 4 and 8 weeks. A small area of cementum healing was observed in 1 area of the specimen at 4 weeks with evidence of rapid resorption and repair ( Fig 3 ). The 8-week specimen showed no obvious signs of cementum deposition on the section stained with hematoxylin and eosin, but it did begin to indicate some hard-tissue formation through calcein deposition from week 6 on fluorescent microscopy.
For the sections that showed root resorption away from the thread, varying degrees of repair were seen. At 4 weeks, no sections showed a healing response, only resorption lacunae following the shape of the implant threads. On higher magnification, however, osteoblasts were seen arranged in a row in the PDL layer, ready to begin the repair process. By week 8, partial repair of the cementum was seen in 1 specimen of 3. At 12 weeks, 3 of 4 specimens showed cementum repair on the damaged root surface ( Fig 4 ).
When any part of the mini-implant thread was left touching the root surface, it was interesting to see that, during the entire observation period, no definite cementum repair was observed on the damaged root surface ( Fig 5 ). In 1 specimen of the 16-week group, an abnormal overproduction of cementum was seen around the thread of the implant.
The healing responses of the pulp-penetration group were mostly through osteodentin formation ( Fig 6 ). This was observed as early as week 4 and up to week 16. The dentin-tissue rupture only type was observed in the 4-week specimens only.
Healing in the group of specimens with the mini-implants removed showed that, in most cases, cementum repair occurred on the damaged root surface. At week 4, there was partial repair with cementum formation in some areas only. From weeks 8 to 16, all sections showed cementum repair ( Fig 7 ). At week 16, a specimen with dentin and pulp penetration damage demonstrated osteodentin formation, with maintenance of the PDL ( Fig 8 ).

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


