To make better and more engaged decisions about treatment, it is vitally important for patients to understand the terminology, type of specialists, and common procedures related to dental implant treatments.
Oral surgeons receive a minimum of four years of postdoctoral training in accredited residency programs. They receive hospital-based training in oral and facial surgical procedures and anesthesia, in addition to extensive medical training to care for medically-compromised patients.
With extensive surgical expertise, oral surgeons are the specialist of choice for the placement of dental implants and related bone grafting procedures. Additionally, oral surgeons specialize in:
•Extraction of teeth (wisdom teeth and others)
•Oral biopsies
•Corrective jaw surgery (orthognathic surgery)
•Oral and facial infections
•Oral and facial trauma
•IV sedation/anesthesia
Periodontists receive 2–3 years of post-graduate training for treatment of gum disease, various gingival procedures (functional and cosmetic), and dental implants for teeth replacement. Periodontists often work along with general dentists or prosthodontists for long term periodontal care of patients (bone and gum tissue surrounding teeth). They provide both preventive periodontal care as well as both surgical and non-surgical management of periodontal disease. While some procedures are performed by both periodontists and oral surgeons, they often work in collaboration on patients with complex needs requiring their expertise. Additionally, periodontists specialize in:
•Surgical and non-surgical treatment of gum disease
•Preventive periodontal procedures
•Treatment of gum recession via grafting procedures
•Cosmetic gingival procedures
•Minor bone grafting procedures for implants
The first type of restorative dentist is a prosthodontist who has received three additional years of postdoctoral training in dentistry, gaining advanced skills in both cosmetic and restorative procedures. Some may also perform common periodontal or oral surgery procedures, but most focus on treatment of patients with complex cosmetic and restorative needs. In a patient with multidisciplinary needs (e.g., a patient who needs crowns, implants, root canal treatment, and gum surgery), a prosthodontist will act as both the restorative dentist and the coordinator of the overall treatment and team of dentists.
The second type of restorative dentist is a general practitioner. A general dentist has graduated from a 4-year dental school with no additional formal post-doctorate residency. Some may have completed a 1-year general practice residency program following dental school, providing them additional clinical experience and expertise.
About ‘Implantologists’
Some dentists market themselves as implantologists signifying their specific interest in implant dentistry. However, It’s important to know that ‘implantology’ is not a recognized specialty by American Dental Association and does not reflect formal training in an accredited residency program like those in oral surgery or periodontics. Any dentist can self-prescribe this label with no specific requirements.
About ‘Mini-Residency’ Programs in Implant Dentistry
Some clinicians may have completed a ‘mini-residency’ program in the field of implant dentistry. Most mini-residencies are weekend programs given over six to eight sessions and consist of lectures and some hands-on classes on lab models. While such programs provide participants a greater insight and knowledge base in implant dentistry, they do not provide the necessary training as given during formal residencies that take three to four years to complete. When seeking the right dentist for implant therapy, patients should inquire about the clinician’s proficiency and experience.
CBCT (Cone Beam CT Scan)
CBCT (Cone Beam CT Scan) is an in-office dental scan imaging machine that provides an accurate 3-dimensional view of the jawbone and surrounding structures (Fig 28 a-b). CBCT is used for precision planning of dental implant placement and related bone grafting with maximal safety. It allows computer-assisted planning and fabrication of accurate surgical guides for precision placement of dental implants. Although, at the time this book was written, it is not considered a standard-of-care to use CBCT for dental implant planning, in our opinion it should be used in every patient as its benefits significantly outweigh its low cost and minor additional radiation. CBCT allows proper diagnosis and planning allowing the surgeon to augment bone when necessary and place the implants in proper position. Many cases of peri-implantitis can be effectively prevented by this approach.
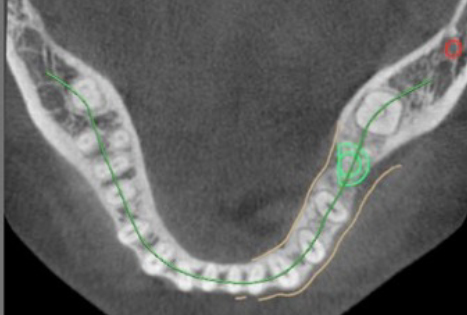
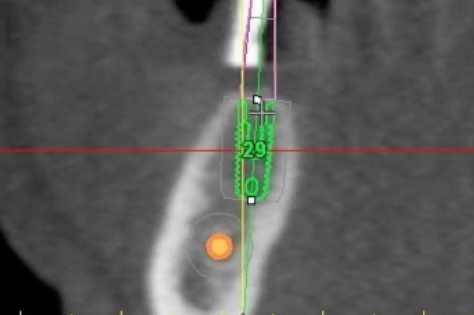
Fig 28 a-b CBCT images showing precise dimensions of the jaw bone and vital structures important during treatment planning
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


