Diagnosis
1990–1999 N = 941
2000–2008 N = 2357
Number (%)
Number (%)
Asthma/respiratory issues
86 (9.1 %)
207 (8.8 %)
Autism
44 (4.7 %)
123 (5.2 %)
Attention deficit/hyperactivity disorder (ADHD)
25 (2.7 %)
75 (3.2 %)
Cardiac anomalies
47 (5.0 %)
108 (4.6 %)
Coagulation disorders/anemia
22 (2.3 %)
33 (1.4 %)
Craniofacial anomalies
34 (3.6 %)
73 (3.1 %)
Developmental delays/mental retardation
77 (8.2 %)
163 (6.9 %)
Genetic syndromes/chromosomal disorders
80 (8.5 %)
177 (7.5 %)
Neurological disorders (e.g., cerebral palsy, seizure disorders)
87 (9.2 %)
170 (7.2 %)
Well child/acute situational anxiety
439 (46.7 %)
1228 (52.1 %)
Children with chronic health conditions are more likely than those without such conditions to receive GA for dental treatment. In a survey of almost 63,000 Iowa Medicaid-enrolled children <15 years old Chi et al. compared the frequency with which children with and without chronic health conditions received GA for dentistry. Overall, less than 1 % of children received GA; however, for children under 6 years of age, the rate was twice as high for those with chronic conditions as demographically similar children without conditions. Age also appeared to be a factor. In this same study, children between 6 and 14 years were three times as likely to require GA if they had a chronic health condition when compared to similarly aged children without a chronic condition [8].
Many different subgroups of patients offer challenges for GA. There is no question that patients with congenital heart disease (particularly those with cyanosis, congestive heart failure, or pulmonary hypertension) [9, 10] or lower respiratory tract disease (such as cystic fibrosis or persistent asthma) represent high-risk subgroups for anesthesia and should only be cared for in setting that have backup capability to manage their possible complications. Additionally, patients with craniofacial abnormalities, who may have difficult to manage airways, should only be anesthetized in full service pediatric care facilities (e.g., Crouzon’s or Pierre Robin sequence).
More recently the anesthesia literature has highlighted the risks associated with anesthesia for patients with obstructive sleep apnea (OSA) [11]. In particular, there are multiple reports concerning the sensitivity of these patients to opiate medications and a higher rate of perioperative mortality in this subgroup [12]. With this in mind, dentists should question patients about symptoms of severe sleep apnea and be aware of any specific testing that may have been done to categorize a given patient concerning this problem. Dental providers should also be aware that these patients deserve special consideration when scheduled for GA and may require prolonged observation or even overnight observation following GA for dental procedures.
Quality of Care
General anesthesia can change the nature of the dental care that is possible for children with medical or behavioral problems. Multiple studies have documented the high quality of dental treatment that is possible under GA. In one study, Drummond et al. documented the outcomes of dental treatments in 292 children under GA. Ninety-five percent of the treated children were followed up. Fifty-five percent had new caries recorded. For the treatments provided, amalgam had a mean success of 57.1 %, composite 73.4 %, compomer 85.2 %, stainless steel crowns 92.8 %, and pulpotomies 84.6 % [13]. In another study, Eidelman and colleagues evaluated 34 patients with dental restoration performed under GA and compared them to 31 had restorations completed with conscious sedation. The group who underwent treatment with GA had a better success rate for marginal adaptation (93 versus 78 %), better success for anatomic form (92 % versus 79 %), a better rate of preventing secondary caries (97 % versus 90 %) [13, 14]. While these studies lack controlled or randomized comparative data with those who did not receive GA, there is no question that the quality of dental care provided with GA is high.
Quality of Life Measures
In considering the cost-effectiveness of GA for dental care, the effect of this care on longer-term outcomes such as the impact on general quality of life should be considered. These issues have been addressed by Jankauskiene and colleagues [15]. The authors carried out a literature search to identify relevant studies examining children’s oral health-related quality of life following dental treatment under GA. Their review included 11 journal articles that had relevant results of clinical trials. The studies outcomes were measured by various questionnaires measuring children’s oral health-related quality of life and parental satisfaction. They concluded that rehabilitation under GA results in the immediate improvement of children’s oral health and corresponding improvement in physical, emotional, and social quality of life. The result was a corresponding positive impact on the family. While the authors recognize the difficulties in measuring quality of life given the different measures that were included, they suggest the trend toward immediate improvement is clear and advocate for further studies in the future. Similarly White et al. [16] found that GA was widely accepted by parents primarily because they believed there was a positive social impact on their children. A majority of parents felt that their child smiled more often and performed better in school following major dental rehabilitation under GA.
Unfortunately, there remains little prospective, randomized, controlled data on the use of sedation versus GA for dental treatment in children in terms of either the immediate outcome of the dental treatment or the longer-term impact on quality of life. In fact, a recent Cochrane collaborative review concluded that there were no studies that met their inclusion criteria for controlled, randomized, high-quality studies and simply recommended that the issue be studied with randomized controlled trial (RCT) in the future [17].
Cost Considerations
The impact of cost and availability of GA for dental care cannot be ignored. Unfortunately, this is a complex issue that should take into account not only the immediate cost of the care, but the many associated costs (expenses) that can be impacted by one type of care versus another. As a general rule, the choice facing dental providers is not simply that of GA versus no intervention, but rather GA versus some form of sedation. Consideration of the cost of anesthesia versus sedation for dental interventions must take into account multiple issues related to the patient and the dental process that is being treated. Lee et al. examined this topic in detail and determined that using GA for dental interventions may be less expensive than sedation when all factors related to cost are considered [18]. These factors include (but are not limited to) transportation costs, time away from work for parents, and the fact that a child may need multiple conscious sedation appointments to complete a dental treatment that could be accomplished with one general anesthetic. “Cost” data are further complicated by the fact that they will vary from location to location depending on the nature of the health-care system. In spite of these limitations, Lee and colleagues provide a helpful roadmap for considering the many factors that go into calculating total cost of a dental intervention specifically contrasting sedation provision to GA.
Operating Room Issues
In many cases, the utilization of GA for dental interventions will require the care to take place in the operating room as opposed to the clinic setting. There are numerous problems inherent in utilizing operating rooms for dental procedures. These include long waiting lists for treatment and various scheduling issues and cancellations due to emergency operative needs. In 2002, the average waiting time for complex dental care in the OR with GA in the US pediatric dentistry programs was reported as an average of 28 days for children experiencing pain and 71 days for children without pain [19, 20]. A subsequent study in 2012 found an average wait list time of 90 days [20]. The long duration of these wait times is often cited as a factor in dental professionals not choosing GA for a given procedure.
Utilization of time in the OR is of great interest to hospital administrators. In particular, GA for dental procedures requires prolonged blocks of time, and the cases are not always easy to predict in terms of duration or level of intervention. Forsyth et al. carefully evaluated the operating room utilization time at the University of Washington for over 700 dentistry procedures performed in the OR. They found that dental procedures finished earlier than the scheduled time by an average of 14 min and overran the scheduled time in 27 % of cases. The average amount of dentist operator time was 76 min. In this same study, the average age of patients was 7.1 years and the American Society of Anesthesiologists (ASA) distribution included 77 % ASA I or II with the balance of patients considered ASA III. Contrary to expectations, the probability of overrunning the allotted time decreased significantly as the ASA status increased. The results of this study point out that (in this institution) dental cases were appropriately scheduled and did not pose an unpredictable burden on the management of the operating room case flow.
General Anesthesia Techniques for Dentistry
General anesthesia for dentistry follows the same general principles as that for other surgical procedures. There are a few caveats that should be kept in mind with respect to this particular clinical setting:
1.
Premedication with acetaminophen is common. Because of the presence of moderate pain (particularly after multiple extractions), many anesthesiologists will choose to premedicate children undergoing GA for dental interventions with acetaminophen. Generally, this is given as an oral solution at a dose of approximately 15 mg/kg, but it can also be given rectally (for age appropriate patients) at a dose of 30 mg/kg. The advantage of premedication is in the time it allows for an effective blood level to be established prior to emerging from anesthesia.
2.
Dental patients may also benefit from midazolam premedication to smooth the induction of anesthesia process. There are multiple studies documenting the improvement of behavior while undergoing induction of anesthesia after 0.5–0.75 mg/kg of oral midazolam [21, 22]. While the practice is not considered “standard,” it is not uncommon and can be particularly helpful in patients who have significant oppositional behaviors. The use of midazolam for premedication has been associated with a decrease in adverse behavior changes in the postoperative time frame [23]. On the other hand, the use of midazolam has also been associated with delayed awakening after GA and should be used with some caution for very short procedures [24].
-
Dexmedetomidine has also been used as an oral premedication for dental surgery. In one study, the use of oral dexmedetomidine was equally as effective as midazolam in decreasing anxiety preoperatively, and it was not associated with any cardiovascular adverse events [25].
3.
In most institutions in North America, inhaled induction with sevoflurane is preferred. This drug gives a smooth, rapid induction and is associated with very few adverse cardiac effects [26]. Bradycardia on induction (which was common with halothane anesthesia) is relatively uncommon with sevoflurane [27]. Induction of anesthesia with intravenous agents is certainly acceptable, but often considered challenging in the active, agitated patients that are not uncommon in the dental GA population.
4.
Adjunctive steroid administration with dexamethasone is common for dental GA. The addition of this drug has been shown to improve pain control and minimize postoperative nausea and vomiting (PONV) for pediatric patients undergoing oral or ears/nose/throat surgery [28–30].
-
Airway management for dental GA is chosen based on the expected duration of the procedure and the nature of the intervention itself. For full mouth rehabilitation, a nasotracheal tube is generally preferred as it is “out of the way” during the dental procedure and offers maximal access to the oral cavity (see Fig. 11.1). Most are placed under direct visualization after deepening the anesthetic with opiates, propofol, and (occasionally) muscle relaxants.
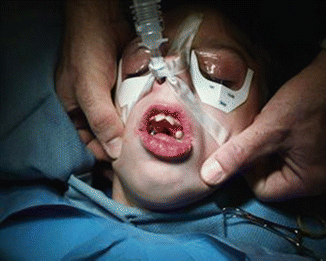 Fig. 11.1Special needs of patient with nasotracheal tube in place offering maximal access to the oral cavity
Fig. 11.1Special needs of patient with nasotracheal tube in place offering maximal access to the oral cavity
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


