Given the myriad of reconstructive options available, it seems easy to theoretically reconstruct even the most complex ablative or traumatic defects, especially since the introduction of microvascular free flaps. The head and neck reconstructive surgeon is faced with the task of conceptualizing a defect, often before it even exists. The challenge arises in choosing the appropriate reconstructive modality for each patient, which begins with the identification of functional goals. Although facial harmony and esthetics are factors in reconstruction of the maxillofacial region, the maintenance of function closely correlates with quality of life outcomes. Considerations in flap design and flap choice are largely based on the characteristics of the anatomic defect. Multiple flap classification systems have been described, and such stratification can be used to direct clinician decision-making. Additionally, flap evolution has closely mirrored the progress of continuing flap reclassification in the literature. This chapter will focus on the classification of flaps and treatment planning with an emphasis on flap choice and free flap design in the reconstruction of oral cavity defects.
Etiopathogenesis and Causative Factors
Reconstruction of the oral cavity is complicated by its anatomic and functional complexity. As the site of entry to the aerodigestive tract, it contains several specialized tissues: the mandible, dentition, tongue, and soft palate. Furthermore it is microbially rich and continuously exposed to saliva. Functional and esthetic reconstruction of major maxillofacial defects requires an in-depth comprehension of the intrinsic anatomy or anatomic subunits to be reconstructed. A guiding principle of reconstruction is to replace absent tissue with qualitatively and quantitatively similar tissue. Ablative defects from both benign and malignant disease are predictable for preoperative planning. Good communication between the ablative and reconstructive surgeons may prevent intraoperative changes to the treatment plan that would potentially affect the outcome. Factors including previous radiotherapy or surgery involving the neck and general medical condition should be incorporated into a reconstructive plan. Elective ablative surgery affords the surgeon ample time to conceptualize and plan a reconstruction, whereas traumatic defects are less predictable and often require temporization to ensure the wound bed is suitable for reconstruction. Historically, reconstruction was typically delayed to permit wound stabilization, facilitate reconstruction, and monitor for disease recurrence. This paradigm has been abandoned by most practitioners and immediate reconstruction is advocated when feasible.
Pathologic Anatomy and Flap Classification
An ideal classification system aids in communication, treatment planning, and outcome assessment. By definition, a flap is a unit of tissue that is transferred from a donor site to a recipient site while maintaining its blood supply. There are several approaches to the classification of flaps, including donor site or destination, type or types of tissue to be transferred, and blood supply. There is no perfect classification system; however, multiple efforts have been made to standardize terminology in the literature. The evolution of flaps has been mirrored by scientific endeavors to reclassify them.
The most basic means of flap classification is by tissue type. Tolhurst devised the “atomic” system of flap classification, in part based on tissue type. Flaps of any tissue type can be devised, provided there is an underlying reliable vascular supply to maintain physiologic homeostasis in the recipient bed. Single-source tissue flaps typically include skin, fascia, muscle, or bone. Composite tissue flaps include more than one type of tissue, such as osteocutaneous or fasciocutaneous.
Flaps may also be described in terms of their proximity to the recipient site (local, regional, distant). Local flaps involve transfer of tissue from the immediate adjacent anatomic subsite. They are descriptively stratified by the basic geometric movement required to facilitate wound closure: advancement, rotation, or transposition. A tongue flap is considered a local/random flap, whereas a facial artery myomucosal flap is considered a local/axial pattern flap. The majority of local flaps for head and neck reconstruction are used for cutaneous defects ( Fig. 3-1 ).
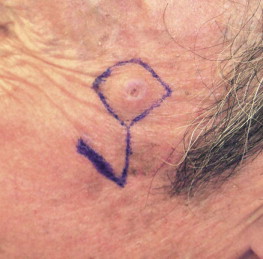
Regional flaps involve the transposition of tissue from a neighboring anatomic site. They too can be further described by their blood supply; however, the majority have an axial pattern of vascularization. Regional cutaneous flaps including the bipedicled forehead flap with a random pattern of blood supply are not commonly used. Distinction should be drawn between the bipedicled forehead flap and the paramedian forehead. The latter differs from a bipedicle forehead flap in that a vascular pedicle is included in the flap design. The deltopectoral flap, a prototypical regional/cutaneous flap, has an axial pattern blood supply from the second, third, and fourth perforators of the internal mammary artery. The distal one third of the flap, however, has a random pattern. The majority of regional flaps used in contemporary reconstruction of head and neck defects are myocutaneous or muscle-only flaps. The pectoralis major myocutaneous flap (PMMC), introduced by Ariyan in 1979, was quickly adopted as the first-choice reconstructive option, and is still considered a versatile and robust choice. The main advantages of the PMMC are that the surgery is easy, a large amount of soft tissue can be obtained, and morbidity at the donor site is low. Although the versatility of free flaps has supplanted the broad use of regional flaps in developed countries, regional flaps are widely used in developed and developing countries alike. Other common and useful regional flaps are derived from the latissimus dorsi muscle, the temporalis muscle, and the temporoparietal fascia; all are reliable for head and neck reconstruction.
Distant flaps may be either free or pedicled. Pedicled distant flaps are infrequently used in head and neck reconstruction, although they do occasionally appear in the contemporary medical literature. Tagliacozzi theorized the use of a distant/pedicled arm flap, the so-called Italian flap, for nasal reconstruction. Free flaps entail transfer of tissue from a remote site with accompanied vascular supply to a recipient bed. Blood flow is reestablished by microvascular anastomosis. Widely adopted after the introduction of the radial forearm free flap (RFFF) in the early 1980s, free flaps have revolutionized head and neck surgery. Innumerable flaps have been described, and their versatility, reliability, and utility for reconstruction are unmatched choices for reconstruction in the head and neck.
Contemporary flap nomenclature and classification is based upon blood supply. Knowledge of the intrinsic blood supply to the skin is recognized as a critical factor in flap success. The recognition that the skin receives its blood supply mainly from vessels that traverse the deep fascia through muscle spawned the evolution of musculocutaneous flaps. Axial pattern flaps are based on a reliable, well-defined vascular pedicle, oriented longitudinally within the flap. The work by Mathes and Nahai helped elucidate the different patterns of blood distribution within muscle flaps; five different patterns were identified based on the principle that muscular blood supply is derived from specific series of arteries and accompanying veins ( Box 3-1 ). The corresponding skin territory of each superficial muscle extends from the insertion to the origin and courses along its borders and may even extend beyond. The skin overlying muscle is perfused by perforating arteries from the muscle. The Mathes and Nahai classification led to a greater understanding of flaps such as the PMMC, in which a reliable skin paddle overlying the muscle is perfused from a specific source vessel. Their work aided surgeons in designing flaps for particular uses based on the pattern of vascularization. Cormack and Lamberty elucidated three vessel subtypes that accounted for many of the cutaneous flaps of the time ( Box 3-2 ). Though the concept was not new, they coined the term fasciocutaneous to describe a flap where the skin is supplied by vessels that pass along intermuscular and intercompartmental fascia to reach the skin. Type A fasciocutaneous flaps contain multiple, unnamed fascial perforators. Type B fasciocutaneous flaps contain a single perforator. Type C fasciocutaneous flaps contain multiple small fascial perforators, but all are fed from a single subfascial vessel that must be transferred with the flap. Nakajima and colleagues expanded on this concept and identified six types of fasciocutaneous perforators, distinguishing between direct and indirect perforators ( Box 3-3 ). The angiosome concept illustrated that arteries closely follow the connective tissue framework of the body. Injection studies by Taylor and Palmer showed that the blood supply to the skin and deep tissues corresponded to a consistent source vessel. The vascular supply to the skin was supplied by direct cutaneous arteries with reinforcement by smaller indirect vessels. Controversy surrounding the use of the term perforator was largely ameliorated following the Fifth International Course on Perforator Flaps in Ghent, Belgium, in 2001. According to Wei and colleagues, a true perforator must pass through a muscle en route to the skin. The nomenclature born from the Ghent conference includes the source artery and the muscle that is traversed by the vessel supplying the skin paddle. The anterior lateral thigh flap would hence be named the lateral circumflex femoral artery perforator flap, with the addition of the vastus lateralis muscle in the notation.
-
Type I: Single vascular pedicle (e.g., vastus lateralis)
-
Type II: Dominant vascular pedicle(s) and minor vascular pedicle(s) (e.g., trapezius)
-
Type III: Dominant pedicles (e.g., rectus abdominis)
-
Type IV: Segmental vascular pedicles (e.g., flexor hallucis longus)
-
Type V: Dominant vascular pedicle and secondary segmental vascular pedicles (e.g., latissimus dorsi)
-
Type A: Contains multiple, unnamed fascial perforators
-
Type B: Contains a single perforator
-
Type C: Contains multiple small fascial perforators
-
Type A: Direct cutaneous
-
Type B: Direct septocutaneous
-
Type C: Direct cutaneous branch of a muscular vessel
-
Type D: Perforating cutaneous branch of a muscular vessel
-
Type E: Septocutaneous perforator
-
Type F: Musculocutaneous perforator
To date, there is no consensus on the classification of flaps. The current trend is to classify free flaps by source vessel. There is little doubt that the classification will continue to evolve with our expanding interest and knowledge of the anatomy and physiology of flaps.
Pathologic Anatomy and Flap Classification
An ideal classification system aids in communication, treatment planning, and outcome assessment. By definition, a flap is a unit of tissue that is transferred from a donor site to a recipient site while maintaining its blood supply. There are several approaches to the classification of flaps, including donor site or destination, type or types of tissue to be transferred, and blood supply. There is no perfect classification system; however, multiple efforts have been made to standardize terminology in the literature. The evolution of flaps has been mirrored by scientific endeavors to reclassify them.
The most basic means of flap classification is by tissue type. Tolhurst devised the “atomic” system of flap classification, in part based on tissue type. Flaps of any tissue type can be devised, provided there is an underlying reliable vascular supply to maintain physiologic homeostasis in the recipient bed. Single-source tissue flaps typically include skin, fascia, muscle, or bone. Composite tissue flaps include more than one type of tissue, such as osteocutaneous or fasciocutaneous.
Flaps may also be described in terms of their proximity to the recipient site (local, regional, distant). Local flaps involve transfer of tissue from the immediate adjacent anatomic subsite. They are descriptively stratified by the basic geometric movement required to facilitate wound closure: advancement, rotation, or transposition. A tongue flap is considered a local/random flap, whereas a facial artery myomucosal flap is considered a local/axial pattern flap. The majority of local flaps for head and neck reconstruction are used for cutaneous defects ( Fig. 3-1 ).
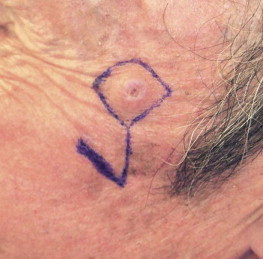
Regional flaps involve the transposition of tissue from a neighboring anatomic site. They too can be further described by their blood supply; however, the majority have an axial pattern of vascularization. Regional cutaneous flaps including the bipedicled forehead flap with a random pattern of blood supply are not commonly used. Distinction should be drawn between the bipedicled forehead flap and the paramedian forehead. The latter differs from a bipedicle forehead flap in that a vascular pedicle is included in the flap design. The deltopectoral flap, a prototypical regional/cutaneous flap, has an axial pattern blood supply from the second, third, and fourth perforators of the internal mammary artery. The distal one third of the flap, however, has a random pattern. The majority of regional flaps used in contemporary reconstruction of head and neck defects are myocutaneous or muscle-only flaps. The pectoralis major myocutaneous flap (PMMC), introduced by Ariyan in 1979, was quickly adopted as the first-choice reconstructive option, and is still considered a versatile and robust choice. The main advantages of the PMMC are that the surgery is easy, a large amount of soft tissue can be obtained, and morbidity at the donor site is low. Although the versatility of free flaps has supplanted the broad use of regional flaps in developed countries, regional flaps are widely used in developed and developing countries alike. Other common and useful regional flaps are derived from the latissimus dorsi muscle, the temporalis muscle, and the temporoparietal fascia; all are reliable for head and neck reconstruction.
Distant flaps may be either free or pedicled. Pedicled distant flaps are infrequently used in head and neck reconstruction, although they do occasionally appear in the contemporary medical literature. Tagliacozzi theorized the use of a distant/pedicled arm flap, the so-called Italian flap, for nasal reconstruction. Free flaps entail transfer of tissue from a remote site with accompanied vascular supply to a recipient bed. Blood flow is reestablished by microvascular anastomosis. Widely adopted after the introduction of the radial forearm free flap (RFFF) in the early 1980s, free flaps have revolutionized head and neck surgery. Innumerable flaps have been described, and their versatility, reliability, and utility for reconstruction are unmatched choices for reconstruction in the head and neck.
Contemporary flap nomenclature and classification is based upon blood supply. Knowledge of the intrinsic blood supply to the skin is recognized as a critical factor in flap success. The recognition that the skin receives its blood supply mainly from vessels that traverse the deep fascia through muscle spawned the evolution of musculocutaneous flaps. Axial pattern flaps are based on a reliable, well-defined vascular pedicle, oriented longitudinally within the flap. The work by Mathes and Nahai helped elucidate the different patterns of blood distribution within muscle flaps; five different patterns were identified based on the principle that muscular blood supply is derived from specific series of arteries and accompanying veins ( Box 3-1 ). The corresponding skin territory of each superficial muscle extends from the insertion to the origin and courses along its borders and may even extend beyond. The skin overlying muscle is perfused by perforating arteries from the muscle. The Mathes and Nahai classification led to a greater understanding of flaps such as the PMMC, in which a reliable skin paddle overlying the muscle is perfused from a specific source vessel. Their work aided surgeons in designing flaps for particular uses based on the pattern of vascularization. Cormack and Lamberty elucidated three vessel subtypes that accounted for many of the cutaneous flaps of the time ( Box 3-2 ). Though the concept was not new, they coined the term fasciocutaneous to describe a flap where the skin is supplied by vessels that pass along intermuscular and intercompartmental fascia to reach the skin. Type A fasciocutaneous flaps contain multiple, unnamed fascial perforators. Type B fasciocutaneous flaps contain a single perforator. Type C fasciocutaneous flaps contain multiple small fascial perforators, but all are fed from a single subfascial vessel that must be transferred with the flap. Nakajima and colleagues expanded on this concept and identified six types of fasciocutaneous perforators, distinguishing between direct and indirect perforators ( Box 3-3 ). The angiosome concept illustrated that arteries closely follow the connective tissue framework of the body. Injection studies by Taylor and Palmer showed that the blood supply to the skin and deep tissues corresponded to a consistent source vessel. The vascular supply to the skin was supplied by direct cutaneous arteries with reinforcement by smaller indirect vessels. Controversy surrounding the use of the term perforator was largely ameliorated following the Fifth International Course on Perforator Flaps in Ghent, Belgium, in 2001. According to Wei and colleagues, a true perforator must pass through a muscle en route to the skin. The nomenclature born from the Ghent conference includes the source artery and the muscle that is traversed by the vessel supplying the skin paddle. The anterior lateral thigh flap would hence be named the lateral circumflex femoral artery perforator flap, with the addition of the vastus lateralis muscle in the notation.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


