(9.1) CONSTANTIN VÂRLAN, BOGDAN DIMITRIU, IONUŢ BRÂNZAN
(9.2) CAMELIA ALB, FLORIN ALB, IONUŢ BRÂNZAN
(9.3/9.4) SMARANDA BUDURU, RAREŞ BUDURU
Chapter IX
ESTHETIC RESTORATION OF ANTERIOR TEETH
Direct adhesive techniques using materials based on composite resins are an excellent modality for the minimally invasive esthetic restoration of anterior teeth. They can be applied and finalized in a single chairside appointment, without the participation of the dental technician’s laboratory in most cases. Esthetic direct adhesive composite restorations allow the replacement of hard dental structures in the following cases:
•Where they are irreversibly altered.
•Where they have been lost, or show structural defects.
•In disorders of carious etiology (simple caries lesions in vital teeth).
•Non-carious etiology.
•Wear lesions (such as attrition/abrasion/abfraction/erosion).
•Traumatic lesions (in coronal location, without the irreversible involvement of the dental pulp).
•Dystrophic enamel/dentin lesions.2,3,5,10
The treatment of tooth discoloration (related to its etiology) using direct laminate veneers represents a specific issue. Moreover, the reshaping of the coronal morphology (shape, size, 3D-positioning) of intact teeth, unaffected by the aforementioned lesions, can be achieved under correct functional conditions.6–8,10
9.1.1 Restorative materials
The achievement of the expected esthetic results is undoubtedly related to the right choice and correct use of the restorative dental materials, according to the indications and techniques specific to each clinical situation. For that purpose, the value of such material is related1,4 to its physical and chemical properties, particularly its optical properties (multiple color shades, opacity/translucency, color stability); to its user-friendly handling; and to the final quality of the surface finishing and polishing. The technique must allow the acquisition of the shape and size, as well as the selection, establishment, and reproduction of the natural chromatic appearance of the restored tooth.2,3,5–10 This is why the currently used techniques are mainly based on various modalities of composite resins layering.5– 8,10
Enamel and dentin adhesive systems are components with a decisive role in the final result of these restorations. Regarding the therapeutic approach of the substrate, their current development and variability offer high bonding forces, increased fracture and wear strength, and optimal marginal sealing, which will accord an increased longevity to the restorations.7,10
The first composite resins available for current use in practice were macrofill composite resins. They have a high degree of loading with irregularly shaped macroparticles, with a nonhomogeneous distribution and uneven sizes. Although they are mechanically strong, they have reduced esthetic qualities because of their optical properties and the surface texture obtained after finishing and polishing. For this reason they are not a convenient solution for this purpose.1,4,10
From an esthetic point of view, in order to reproduce the physical optical properties of enamel and the biological qualities of its surface, microfill composite resins are the highest performance composite materials that can be used for the direct restoration of anterior teeth. These materials contain a dense load of homogeneously distributed, uniform-sized spherical particles, which allow a long-duration polishing of the restored surface, together with a good wear resistance (particularly by abrasion/erosion) under normal functional conditions.1,4 Thus, such restorations do not support the formation of dental microbial plaque, and allow effective cleaning. Regarding their optical properties, microfill composite materials have reflection and refraction properties that are extremely similar to those of the dental enamel surface. This is why, after processing, finishing, and polishing, they reproduce this surface best in terms of smooth texture and lack of roughness, light reflection and refraction, color density, and translucency, conferring the natural vitality of the esthetic appearance, which can be observed immediately and in the short term, as well as maintained in the long term.6,8,10
The main problem related to the properties of microfill composite resins is the low resistance to fracture and high or excessive wear (particularly by attrition), which limits their use in locations where they are exposed to increased strain due to high occlusal forces.2,3,7,10
The first composite materials used to solve this problem (due to their good resistance to mechanical strain), and to replace microfill composite resins in the aforementioned situations, were microhybrid composite materials. Their physical properties include high resistance to compression and fracture, but their esthetic qualities do not equal those of micro- or nanofill composite materials. The mean size of small-size particles in microhybrid composite materials is 0.4 to 0.7 µm; large size particles reach 35 µm, conferring resistance and good handling properties to the material. However, they do not allow finishing and polishing of the surface in order to obtain a texture and a gloss similar to natural enamel, both immediately and in the short term, and particularly in the long term.1,4,10 This is why the final esthetic appearance of microhybrid composite resin restorations, although clearly superior to that of restorations with conventional macrofill materials, cannot reach the level of micro- or nanofill composite resins. Due to their increased strength and opacity, these materials are extremely useful for stratified restorative techniques in anterior teeth, in order to reproduce the qualities of dentin (as a support for enamel) or, frequently, for masking darker or discolored areas.6,8,10
•Very good handling properties.
•Low polymerization shrinkage.
•Fracture resistance.
•Favorable optical properties with a color and a translucency close to that of natural teeth.
•Good final polishing that results in a surface texture that reproduces the enamel.
Apart from the above, they can also be used as a support for microfill composite resins, in which case the quality of translucency allows for the reproduction of the vital tooth appearance. However, compared to microfill composite resins, their final surface characteristics are not either quasi-identical or extremely similar to those of the dental enamel surface; nor do they perfectly mimic the natural vitality of the esthetic appearance.6,8,10
To summarize the adequate and appropriate selection of materials for direct esthetic restorations in anterior teeth: microhybrid composite resins are optimal to reproduce the properties of dentin (resistance, color, opacity), and to replace it. Nanofill composite resins (based on nanotechnology) and nanohybrid composite resins are the most frequently indicated as universal materials for most ordinary situations (with above-average esthetic requirements). Microfill composite resins can reproduce enamel characteristics (surface texture and gloss, translucency, light reflection and refraction) extremely well, and are therefore esthetically optimal for its replacement in restorations with exceptional requirements. These statements, supported by the theoretical and practical data presented by the current literature, lead to the conclusion that in most cases, the handling technique should be based on layering. This is due to the need to replace different hard dental structures and to reproduce the properties of each one in the best way possible to obtain optimal strength and esthetic appearance, as well as for the longevity of the restorations.2,3,5–8,10
9.1.2 Auxiliary components: opacifiers and tints
An extremely important aspect – unfortunately underestimated or even disregarded and thus insufficiently and sporadically applied in current practice – is the use of opacifiers and/or tints to improve the quality of the final esthetic result of direct composite restorations in anterior teeth.8,10 This is mainly due to incomplete and superficial information regarding the advantages that can be obtained from using them.
Opacifiers are used to reduce the visibility of and mask discolored (most frequently, dark) areas inside the preparation, or to eliminate areas of unesthetic light refraction through the composite material. Really “invisible” restorations, which completely reproduce the “natural” appearance of the teeth, frequently require the adequate use of a kit of opacifiers with multiple color shades, compatible with the composite resin used.10
Tints are used to increase the incisal translucency or the cervical (gingival) basic shade and/or intensity (pigment load) of the initially selected color for the restoration material, according to needs. In order to make this effect possible, tints should be translucent (unlike opacifiers) to allow the refracted light to cross and “carry” the augmented color to the overlying composite material layer.
The possibility of improving the final result is another reason why this type of resin is indicated as a first option for direct restorations for the replacement of enamel in anterior teeth.10
Taking all of this into consideration, it appears that the most advantageous solution for direct esthetic restoration techniques in anterior teeth is the use of a complex set of components (each of which can be necessary at a certain step), where microhybrid, nanofill, nanohybrid, or microfill composites present different color shades in accordance with their different components and with the shade guide (color determination method) used; furthermore, for each shade there are various degrees of intensity (pigment “loading”),5,6,8,10 besides the opacifiers and the tints.
Ideally, all these components (including the adhesive system used) should be perfectly compatible in terms of composition and structure, physical and chemical properties, technical fabrication characteristics, and working modality (including optimal handling).
9.1.3 Clinical indications
Direct esthetic restorations of anterior teeth using resin composite materials and adhesive techniques are currently widely used. Their current indications are extensive, ranging from ordinary (routine) restorations of caries lesions in class III, IV, and V cavities, to single or multiple (including complex, extensive) incisal/proximal/vestibular defects due to wear, trauma, or dystrophic lesions. A particular situation, with characteristic aspects, is the treatment of tooth discoloration (depending on etiology) using direct laminate veneers. Intact teeth, unaffected by the aforementioned lesions, can also be approached for coronal reshaping, in cases of diastema, microdontia, and atypical shapes, or for repositioning/realignment, as part of the complex reconstruction of the dental component of the dentolabial appearance (restoring/changing the smile design).5–10
In some of these cases, the indication of direct composite restoration can be discussed in relation to the degree of expertise, as well as the experience, of a particular practitioner, with a specific composite material and the working technique required for that material. However, apart from these situations (representing exceptions rather than the rule), the idea that these types of restorations should not be currently approached and performed because they are too difficult and do not have an adequate longevity is erroneous: if they are rigorously performed, and all clinical and technical indications are respected, direct esthetic restorations (including extensive, complex ones) with composite resins maintain their qualities and last for at least 8 to 10 years, while the number of reported and documented cases for which this period extends to 15 or even 20 years is constantly increasing.5–8,10
There are some opinions (coming from practitioners with vast experience) regarding these types of restorations that relate to the laborious and rigorous techniques and multiple procedures involved, some of which are delicate and require a fastidious approach. Furthermore, they require a significant extension of the time required for restoration and also increase the practitioner’s stress levels, as well as the risk of failure. These opinions cannot be considered relevant or decisive in light of the important advantages conferred by direct composite restorations in anterior teeth, which include the following:8,10
• Enamel and dentin adhesion (if correctly and efficiently performed) confers the retention of the restoration and the marginal integrity. It prevents microleakage and subsequent deterioration at this level.
• Temporary restoration is no longer necessary.
• The patient can benefit from the final esthetic result being obtained in a single appointment.
• The dentist is in complete control of the final esthetic result and can continuously collaborate with the patient during the restoration.
• Correction, reconditioning, or repair is much easier and faster to perform, with much better and more immediate results compared to other restoration modalities.
For these reasons, due to current materials and techniques, these types of direct restorations can provide excellent chairside and single-appointment results that are highly esthetic, with a remarkable longevity. Furthermore, these types of restorations are examples of the application of minimally invasive principles in common practice.8,10
9.1.4 Specific aspects of dental preparations for direct composite resin restorations in anterior teeth
The characteristics of dental preparation for these types of restorations in anterior teeth are determined by the performance of the adhesive bonding of the material to enamel and dentin. Clinically, this involves a number of aspects that correlate with the location and the surface area and depth of the defect that needs to be restored.6,8
Class III and IV preparations of small and medium size located only in the enamel require for the adhesive cavity (in addition to the concave regularization of the walls, after the removal of the irreversibly altered hard dental tissue) only a reduced circular marginal, beveled with a maximum 0.5 mm width. If the restoration of the incisal angle is involved, the shape, size, and modality of preparing the bevel should be correlated with the esthetic appearance and the extension of the restoration: extended preparations justify a bevel width of at least 1 mm. The surface of adhesion to the enamel should be larger, while the forces to which the restoration may be exposed will be higher.6
In order to mask the contour of the restoration on the buccal surface, the edges of the bevel will be slightly finished and polished, so as to be continuous, without clear delineation, with the unprepared dental surface. At the initial preparation of a class III cavity, it is frequently possible to avoid the suppression of the buccal marginal crest and the involvement of the buccal surface in the restoration, which permits the achievement of a better esthetic result; in the case of an extended restoration, it will be difficult to avoid the implication of the buccal surface in the preparation. In this case, the most indicated solution is a fine circular bevel with a small flare.
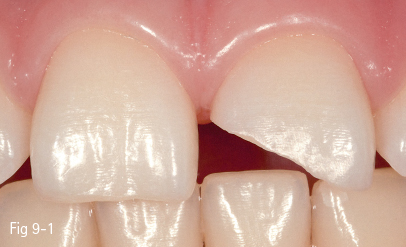
Fig 9-1 Nonpenetrating fracture 21.
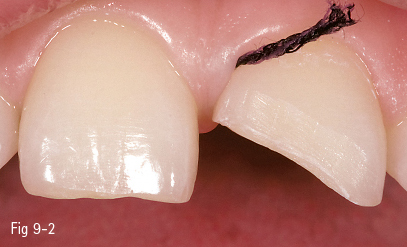
Fig 9-2 Preparation with a bevel and a retraction cord.
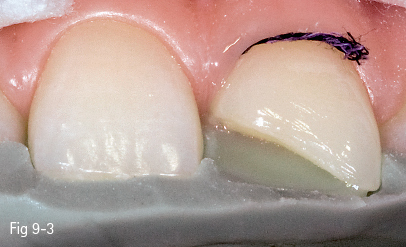
Fig 9-3 Silicone key.
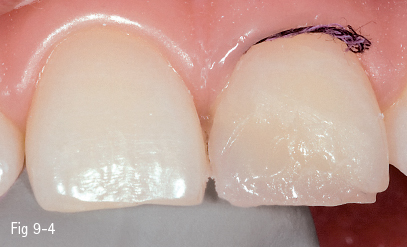
Fig 9-4 Composite layering.
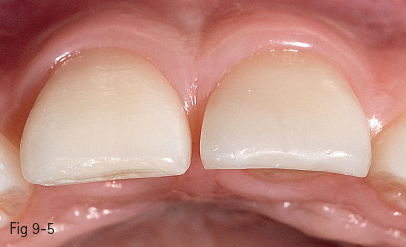
Fig 9-5 Final aspect – incisal view.
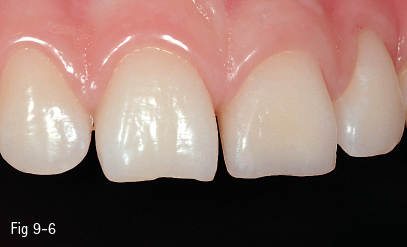
Fig 9-6 Final aspect – buccal view.
In class V buccal cavities, the bevel requires a reduced slope and less width, particularly in order to create a less visible progressive transition from the appearance of the restoration to that of the dental surface. In the case of lesions such as erosions/abrasions, preparation is often unnecessary, the finishing of the margins being sufficient (Figs 9-1 to 9-6).6,8
In principle, besides checking for the complete removal of the irreversibly altered hard dental tissue, any fragile or unsupported marginal enamel portion should be finally removed, because it will have an unfavorable effect on the adhesion at the enamel interface. On the other hand, the maintenance of these thin, irregular enamel margins will cause (after the placing of the composite resin) the so-called “prism effect,” due to light refraction through that enamel layer. The refracted light will create an obvious delineation between the restoration and the hard dental structure.6
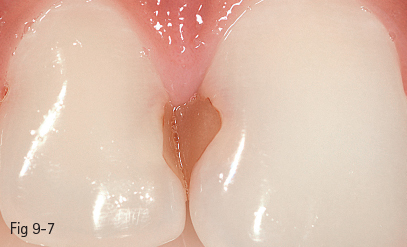
Fig 9-7 Old discolored fillings 11, 12.
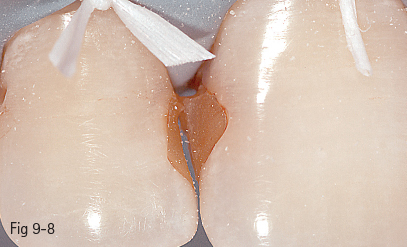
Fig 9-8 Placing of the rubber dam.
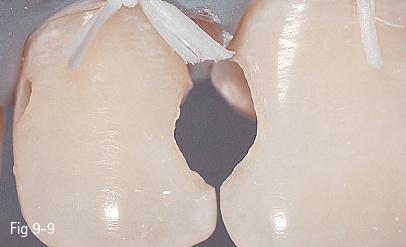
Fig 9-9 Cavity preparation.
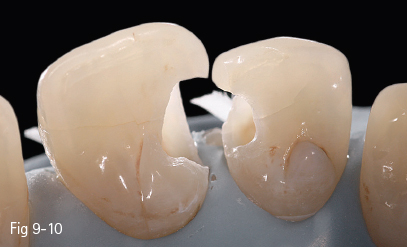
Fig 9-10 Beveled preparation – palatal view.
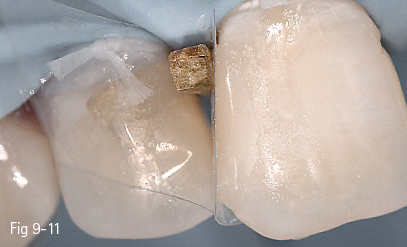
Fig 9-11 Placing of celluloid matrix and wedge.

Fig 9-12 Removal of excess material with no. 15 blade.
Certain clinical situations allow the placing of composite resins for restoration without a preparation: most frequently, direct veneers or tooth reshaping (in cases of interdental spaces, or at the end of orthodontic treatments). Unlike indirect composite or ceramic laminate veneers, which require a well-defined thickness according to a preparation algorithm, there is no mandatory thickness for the material layer regarding the direct composite veneer technique without a preparation.6,8
A modified shape or discoloration may require coronal recontouring through selective buccal and incisal reduction, usually limited to the enamel layer (“enamel sculpting”).6
A special preparation form (“subs-tractive method”) consists of the selective reduction from the proximal area through interdental slicing. This is used, for example, for restoration cases presenting asymmetrically distributed interdental spaces, where it would be impossible to obtain equal widths in homologous teeth, or proportional widths in an anterior group of teeth, by using only the “additive method”.6
Fig 9-13 Finishing.
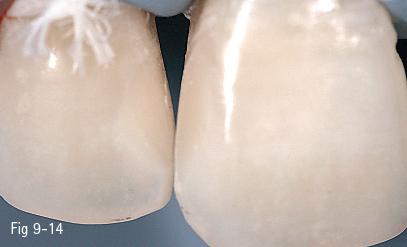
Fig 9-14 Final aspect after finishing and polishing.
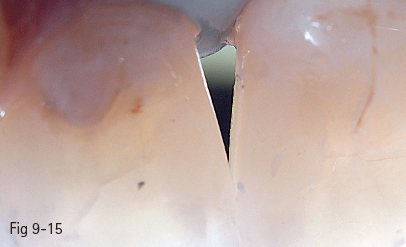
Fig 9-15 Final aspect – palatal view.
Extended preparations are necessary for restorations that correct important position changes, dystrophic enamel lesions, or intense discoloration. The sequence of the preparation steps includes the initial stage of the main external contour, followed by the buccal surface; the thickness of the material layer at this level may vary between 0.3 and 1 mm, depending on the desired correction regarding the position, shape, or color of the tooth.6,8
9.1.5 Composite layering – the multiple morphological layering technique
The reproduction of the natural appearance of the color, translucency, and texture of the surface is determined by the propagation of light through the restoration (starting from the surface), through the composite mass applied over the residual enamel and dentin. In order to produce a natural three-dimensional effect, the composite mass should have optical properties identical or very similar to those of the enamel and dentin.2,3,6–8,10 However, it should be taken into consideration that microfill composite resins have a different light refraction index in comparison with natural prismatic enamel, and the placing of an “enamel composite” layer with the same thickness as that of natural enamel would result in a marked gray shade of the final restoration (Figs 9-7 to 9-15).6,8
This is why the artificial enamel layer should have approximately half the thickness of natural enamel, ie, about 0.5 mm. So, in contrast with the natural tooth, the multiple morphological layering of composite materials for the restoration of anterior teeth can be described as “dominated by dentin”, because the dentin mass core will have a greater volume than in the case of natural teeth.6,8
To achieve an optical appearance similar to that of the natural tooth, all restorations should present an “enamel composite” layer on their buccal, oral, or proximal surface. In order to avoid the undesired excessive marginal translucency effects (the so-called “halo effect”) in the areas of transition from the restoration limit to the natural enamel surface, the dentin composite layer with a basic (more opaque) shade must partially extend over the beveled enamel margin of the preparation. In that area, the enamel composite covering the dentin mass must be very thin.6
Usually, the working steps for this layering technique will be as follows:6
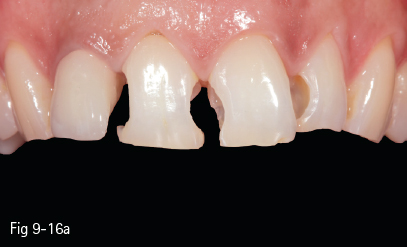
Fig 9-16 a Proximal cavity preparations in 11, 21, and 22.
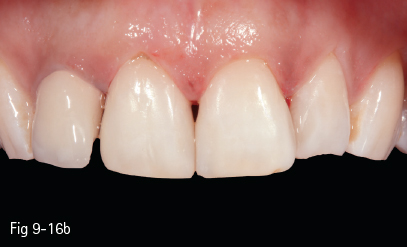
Fig 9-16 b Final aspect of the restorations – buccal view.
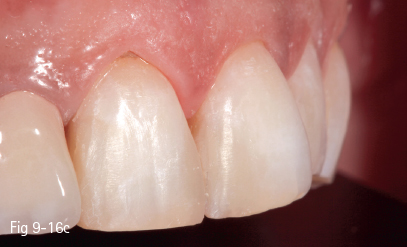
Fig 9-16 c Final aspect – anterolateral view.
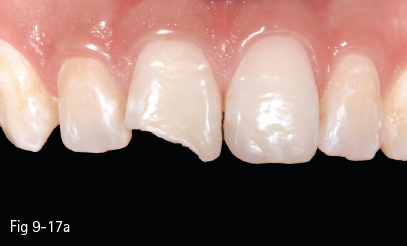
Fig 9-17 a Incisal fracture on 11.
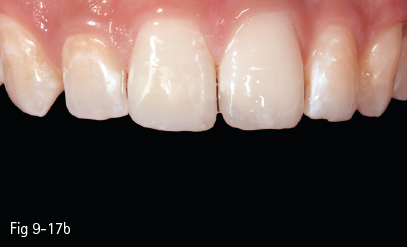
Fig 9-17 b Final aspect.
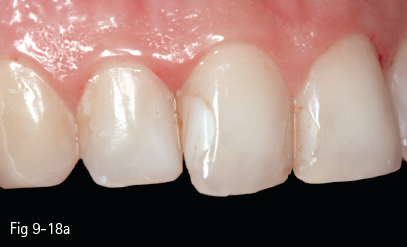
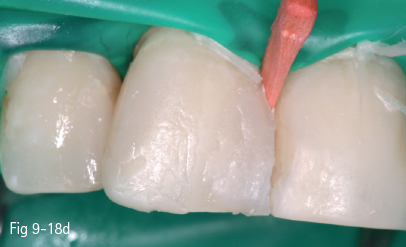
Fig 9-18 a Old discolored fillings on 11.
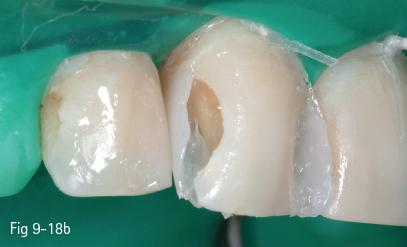
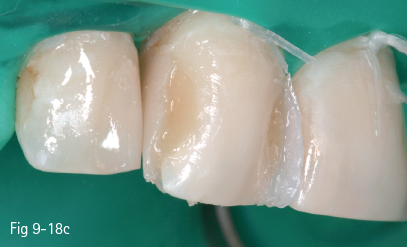
Fig 9-18 b, c, d Restoration steps.
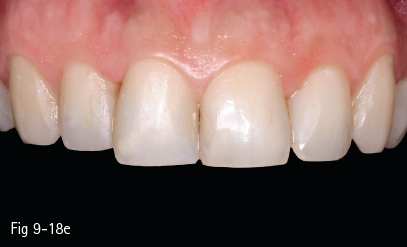
Fig 9-18 e Final aspect. (Images courtesy of Dr Stefan Arion.)
•Determination of the color (“chromatic map”) for the restoration of the tooth.
•Construction of the dentin core (with several shades of dentin mass).
•Use of opacifiers/tints (optional).
•Selection of the basic shade for the enamel mass.
•Specific “characterization” of the enamel layer (optional).
9.1.6 Matrices for the direct esthetic restoration of anterior teeth
The current techniques for these restorations, depending on the clinical situation and the need to restore the of coronal contour and the interdental proximal contact area, can use several types of matrices:2,3,5–8,10
•Transparent matrix bands (with interdental wedges).
•Prefabricated anatoform copings.
•Silicone guides – by the impression of the oral surface.
•Special matrices: cervical/proximal (individualized matrices).
A special mention should be made of the increasing frequency of the recommendation and use of proximal matrices “open” towards the vestibular and oral surfaces, which allow a much more convenient access for layering and modeling.6–8
For the majority of authors who recommend and use direct composite restorations, in addition to using matrices (considered to be mandatory in proximal restorations), the use of freehand sculpting of coronal morphology is essential. This is because it allows for creativity and adds to the quality of the final result (Figs 9-16a to 9-18e).6–8,10
REFERENCES
1. Powers JM, Sakaguchi RL. Craig’s Restorative Dental Materials, ed 12. St Louis: Mosby Elsevier, 2006:189–212.
2. Hilton TJ, Ferracane JL, Broome JC. Summit’s Fundamentals of Operative Dentistry. A Contemporary Approach, ed 4. Chicago: Quintessence, 2013.
3. Heymann HO, Swift Jr EJ, Ritter VA. Sturdevant’s Art and Science of Operative Dentistry, ed 6. St Louis: Mosby Elsevier, 2013.
4. O’Brien WJ. Dental Materials and their Selection, ed 4. Chicago: Quintessence, 2008.
5. Brenna F, Breschi L, Cavalli G, et al. Restorative Dentistry: Treatment Procedures and Future Prospects. St Louis: Elsevier Mosby, 2009.
6. Hugo B. Esthetics with Resin Composite. Basics and Techniques. Chicago: Quintessence, 2009.
7. Mangani F, Putignano A, Cerutti A. Guidelines for Adhesive Dentistry. The Key to Success. Chicago: Quintessence, 2009.
8. Terry DA, Leinfelder KF, Geller W. Aesthetic and Restorative Dentistry: Material Selection and Technique. Stillwater: Everest Publishing Media, 2011.
9. Ricketts D, Bartlett D. Advanced Operative Dentistry: A Practical Approach. London: Churchill Livingstone, 2011.
10. Freedman G. Contemporary Esthetic Dentistry. St Louis: Elsevier Mosby, 2012.
9.2 PORCELAIN LAMINATE VENEERS
9.2.1 Motivation
Porcelain laminate veneers (PLVs) are currently the treatment most in demand in esthetic dentistry: patients request them daily; dentists recommend them whenever possible, depending on the particular clinical case; and, for dental technicians who fabricate them, they represent the highest technical expertise of their laboratories. This is a highly elective dental treatment, so everybody involved in it – patient, dentist, dental technician – is very motivated to achieve a beautiful smile that is as close as possible to perfection. In the 21st century, beauty and physical attractiveness are considered to be directly correlated with social, professional, or personal success. Social and psychological studies have unequivocally shown that people perceived as beautiful by their peers earn higher salaries, are more easily employed, receive more favorable decisions in court, and have a better chance at finding a life partner than ordinary-looking people. The face is the most important aspect of the entire physical appearance, and with the smile at its center, it is easy to understand why it induces a reaction from those who perceive it.
Porcelain laminate veneers have become so popular because they meet several important requirements:
• Biological: they are very conservative with the dental tissues and, in most cases, do not require subgingival preparations.
• Functional: even though PLVs are extremely thin and breakable, due to the low flexural strength of the ceramic, the tooth-veneer complex is extremely resistant over time.
• Esthetic: they reproduce the natural teeth almost perfectly, due to the optical properties of sintered ceramic.
• Reliability: PLVs provide very stable results over time, without chromatic changes;1
• Economic: the most frequently used veneers (feldspathic and pressed veneers) do not require expensive investments in the laboratory or the dental office, so theoretically they can be made by any dentist and any ceramist who has the knowledge and can master the procedures.
Veneers started their journey in 1928, with the first acrylic resin veneers made by Charles Pincus for Hollywood actors, who only wore them for several hours while shooting a movie. Then Pincus started to apply porcelain veneers onto teeth without special preparation. This was followed by today’s modern concept of veneers. The use of veneers would not have been possible without the discovery of adhesion through the acid etching technique introduced for the first time by Buonocore in 1955, as well as the etching treatment of the porcelain surface discovered by Rochette in 1973. PLVs were introduced by Horn in 19832 under the name of porcelain labial veneers, and were developed by authors such as Ronald Goldstein, Pascal Magne, Urs Belser, Galip Gürel, Eduard McLaren, Michel Magne, David Garber, and Horn, who have done extensive work and research in this field, and published many books and articles.
A review by Della Bona of over 400 articles published between 1993 and 2008 on the longevity of ceramic veneers concludes that their success rate is over 90% in all single-tooth restorations in the anterior area, regardless of the ceramic system used.3–5 Many studies were carried out on certain types of ceramics: Fradeani, in his study on 83 Empresspressed veneers, reported a 6-year success rate of 98.8%,6,7 while other studies have reported a 12-year success rate of 91%.8,9
9.2.2 Clinical indications for PLVs
When introduced in the 1980s, PLVs had very few clinical indications because of the poor physical properties of the ceramic masses. Today, the indications for PLVs have been considerably extended and they are successfully used in many clinical situations:
•Minor malpositions (rotations, lingual tilting).
•Shape and size abnormalities (undersized or conical teeth), enamel dysplasia or dystrophia.
•Mild or moderate changes in the shape of dental arches.
•Closure of interdental spaces, physiological or pathological abrasion.
•Fractures of anterior teeth in the incisal and middle thirds.
•Single-tooth discoloration (non-vital teeth) or generalized discoloration, most frequently found in relation to antibiotic treatment, that is resistant to oxidative whitening procedures or have relapsed after such treatments (Figs 9-19a and 9-19b).10
Absolute contraindications include:
•Non-vital teeth with extended class III or class V composite restorations.
•Teeth with severe position changes (severe rotation, inclination, translation) that cannot be corrected through preparation and veneers but only with orthodontic treatment.
•Occlusal disorders that cannot be corrected by prosthetic rehabilitation.
The following can be considered as relative contraindications:
•Severe discoloration that cannot be masked by veneers.
•Bruxism (in certain cases).
•Teeth with old composite restorations on more than two dental surfaces.
•Teeth with advanced enamel abrasion, particularly on the buccal surface.11,12
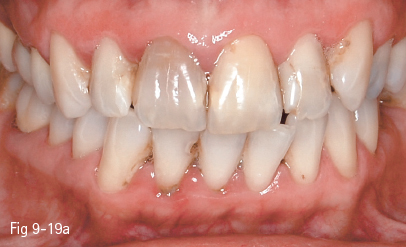
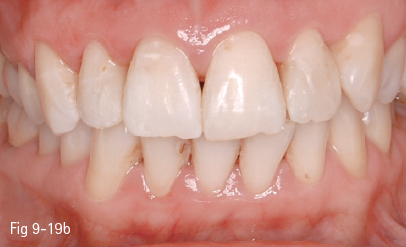
Fig 9-19 a,b. Single-tooth discoloration of endogenous cause – clinical case before and after internal bleaching with Opalescence Endo (Ultradent). Although immediate results are good, internal discoloration will relapse within 2 to 4 years.
9.2.3 Case selection and treatment planning
Restoration of teeth using ceramic veneers is a reliable and long-lasting treatment option when applied correctly for the right indication, with a good treatment plan, if all the details and techniques are strictly followed in the office and in the dental laboratory.13 Even the most experienced cosmetic dentist will not always obtain a 100% success rate. Most frequently, failures occur because of inadequate clinical indication, insufficient case analysis, or lack of communication between dentist, patient, and ceramist, which results in the general dissatisfaction of all parties concerned. This is why the authors strongly recommend that any esthetic case should start with several preliminary sessions involving the documentation of the case, initial discussions with the patient in order to understand his/her expectations, an esthetic analysis with the team of specialists, and, finally, the detailed presentation of the treatment plan to the patient.
Esthetic case documentation
The documentation of esthetic cases includes:
•Complete medical records.
•An esthetic questionnaire for self-evaluation.
•A complete set of intraoral and facial photos.
•Study or diagnostic casts.
•The record of the occlusal relations using high-performance methods.
•The use of the facebow to mount the study cast in the articulator.
•Full-mouth radiograph.
•Lateral cephalometric and/or CT scans (in more complex cases).
Esthetic analysis of the clinical case
The esthetic analysis of the clinical case should be done before offering any treatment plan to the patient. For complex cases, we should involve a team of specialists: an orthodontist, a periodontologist, an oral surgeon, and, of course, one or more highly trained dental ceramists.
The esthetic analysis will include: examination of the dental proportions; the dental arches; the gingival esthetic criteria; the dentofacial aspect; the facial esthetics; and analysis of the occlusion. These aspects are detailed in Chapter II.1,10
After this analysis, a complex and well-documented esthetic treatment plan can be presented to the patient in a second appointment. As Dr Elliot Mechanic pointed out, “our patients did not go to dental school”, so it is generally difficult to explain to patients the proposed treatment plan and esthetic procedures using only words. In most cases, dentists need to add other modern means of communication to correctly convey the message to patients, and also to increase treatment acceptance.
Generally, when we restore a patient’s smile with porcelain veneers, we perform a treatment of choice. Precisely because of this, it is absolutely necessary to establish a perfect communication with the patient (described in detail in Chapter IV) before starting any irreversible procedure, such as the preparation on those teeth that the patient wishes to change. We strongly advise against dentists starting from the first appointment directly with the preparation, impression, cast and fabrication of ceramic veneers in the laboratory simply because the patient is eager to change his/her appearance. By so doing, we can end up in the unpleasant situation of being at the final stages of try-in or cementation, with the dentist not having completely understood the patient’s expectations, or the patient not having been able to see what could have been achieved at the end of the prosthetic treatment.
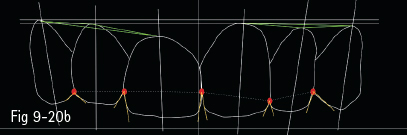
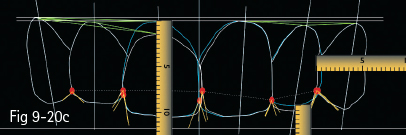
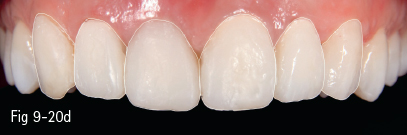
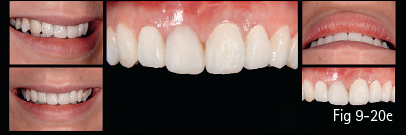
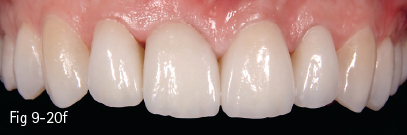
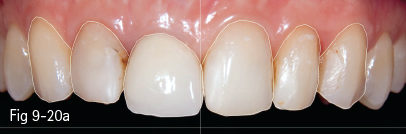
Fig 9-20 a. Clinical case analyzed by Digital Smile Design: analysis of dental arches in buccal view, with the outline of the contour of maxillary anterior teeth. b. Contours and initial analysis, on which the possible changes proposed by the dentist are based, and then discussed with the patient. c. Measurements of the changes proposed for the dental technician. d. Provisional work according to the mock-up. e. Checking the temporary restorations in the patient’s mouth for the validation of the DSD project. f. Final esthetic solution using e.max Press crowns on the four maxillary incisors and e. max Press veneers on the canines. (Images courtesy of Dr Dan Lazăr.)
< div class='tao-gold-member'>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses