(10.1) CONSTANTIN VÂRLAN, BOGDAN DIMITRIU, IONUŢ BRÂNZAN
(10.2) CAMELIA ALB, FLORIN ALB
(10.3) SMARANDA BUDURU, RAREŞ BUDURU
Chapter X
ESTHETIC RESTORATION OF POSTERIOR TEETH
In their most recent variants, ie, based on microhybrid, submicrohybrid, nanofilled, and nanotechnology, composite resins are extremely widely used for restoring posterior teeth, due to their adequate biomechanical and esthetic properties.2–9
For these restorations, composite resins can be used by means of several techniques based on enamel-dentin adhesion:2,7
• Direct.
• Semi-direct.
• Direct – Indirect.
• Indirect.
Direct techniques are the best known and most widely used. Improved and diversified enamel-dentin adhesive systems, along with compensated polymerization shrinkage to counteract and balance undesired side effects, may currently provide a high-quality marginal adaptation, with good longevity, without microleakage.2,3,6,7
Current composite resins have superior physical and chemical properties that have increased their fracture and wear resistance, so that this problem is practically solved, at least for restorations of cavities with small and medium extension.4,5,8,9
The result of these improvements is that direct esthetic restorations with composite materials have proved to have a higher survival rate.4,5,7–9
The problems concerning the quality of direct restorations are related to their use in large and deep cavities, or in cavities that are difficult to access in order to apply the appropriate handling technique. These problems are related to the maintenance of the marginal adaptation to cavity contour areas located at the limit of the cementoenamel junction (CEJ), or beyond it, or to the presence of excessively undermined or fragile enamel crown walls.
In such situations, restoration possibilities other than direct adhesive composite techniques should be considered.1,2,4,5,7–9
In 1998, the American Dental Association defined a series of indications regarding the esthetic restorations of posterior teeth using direct adhesive techniques:4,5,7
• Sealing, even extended sealing, of pits and fissures.
• Preventive resin restorations in pits and fissure areas.
• Treatment of primary class I and class II caries lesions.
• Treatment of secondary caries lesions in class I and class II restorations, when the buccal-oral extension of the cavity is smaller than half the distance between the buccal and the oral cusps.
• Treatment of class V cervical lesions.
• Patients allergic to metal alloy restorative dental materials.
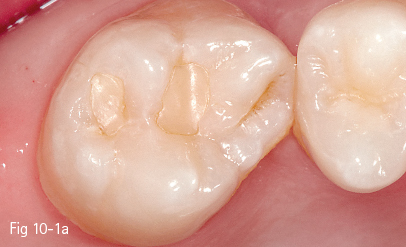
Fig 10-1 a Preoperative situation of 17. Old restoration with incorrect marginal adaptation.
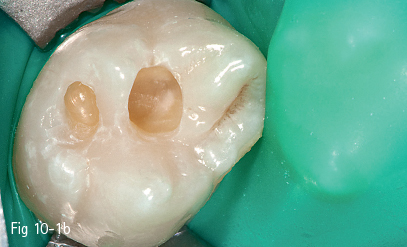
Fig 10-1 b A class I occlusal cavity on 17 (beveled preparation).
10.1.1 Adhesive preparation
The adhesive preparation7 is indicated in primary cavitated caries lesions, the size of which is exclusively determined by the extent of the missing hard dental tissues.
The specific aspects of an adhesive restoration in such cases consist of rounded internal angles of the cavity and a chamfer preparation of its enamel margins. It should be noted that due to the orientation of the enamel prisms at the external margins of the cavity, their finishing by using adequate rotary cutting instruments (straight fissure, tapered fissure, or flame finishing burs) perpendicular to the occlusal surface results in sectioning of the prisms, and in exposing the cut surface under a favorable angle for acid etching. Therefore, there is no longer the need for conventional beveling at this level.3,6,8
10.1.2 Conventional preparation with beveled margins
In clinical situations characterized by the existence of a previous metal alloy restoration, a conventional preparation with beveled margins becomes necessary. After the removal of the metal alloy restoration and of the irreversibly altered hard dental tissues, this preparation of the cavity consists of adjusting by rounding the internal angles and finishing the beveled external margins, most preferred as a chamfer. These changes to the initial preparation result in a cavity (Figs 10-1a and 10-1b) with adhesive characteristics.2,7,8
10.1.3 Restorative materials
In most cases, the restorative materials indicated for the posterior teeth are the microhybrid composite materials, having an average microparticle size of 0.5 to 1 µm, and pyrolytic silica particles of 0.04 µm. Flowable composite materials are frequently applied, as a first increment, on the floor or on the pulpal walls of occlusal or proximal cavities.
The continuing evolution of direct restoration materials has determined the development and use of composite materials intended for lesions located in posterior teeth, including nanoparticles with sizes generally smaller than 100 nm (most frequently ranging between 5 and 20 nm). These materials are characterized not only by the nanometric size of the particles they are loaded with, but also by specific nanotechnological modalities, which allow the stable grouping of nanoparticles in clusters with sizes similar to those of microparticles: 1 to 5 µm, up to 10 µm. Thus, the mineral filling of such a composite material consists of both separate nanoparticles and nanoclusters.
At the same time, these technological improvements have allowed the production of materials with a higher degree of particle loading, both in weight (70% to 80%) and in volume (60% to 65%). Due to all these changes, current composite materials recommended for posterior teeth have very good physical (particularly mechanical) properties. These translate into the obtaining of a wear resistance similar to enamel and silver amalgam (10 to 50 µm/year).3,6,9 The presence of an elasticity modulus close to that of dentin results in mechanical strain responses similar to those of dentin and significantly contributes to the integration of the direct restoration in the stress behavior of the tooth concerned.
The esthetic result is also remarkable. This is due, first of all, to the special finishing and polishing possibilities resulting from the optimal surface characteristics of the latest generation of composite materials. Furthermore, there are currently not only many different shades available, but also different degrees of translucency. These are the result of the mixture of particles with different optical properties, both in the material mass (as separate nanoparticles) and inside the nanoclusters.
The protocol for a composite restoration of the posterior teeth recommends the use of flowable resin composites, with a lower elasticity modulus, of maximum 5 GPa, applied to the cavity floor, over the enamel-dentin adhesive. These belong to microhybrid composites with a higher internal flowability, and show a higher elasticity in comparison with dentin (18 GPa). They are applied in a thin layer, as the first increment, between the adhesive system and the composite material that will represent the bulk of the final restoration.
The use of flowable composite materials is indicated for:
• Improving the interface between the adhesive system layer found on the cavity floor and the composite material that forms the main mass of the restoration.
• Compensating internal stress that occurs during polymerization and is manifest by the shrinkage of the material, consequently by tension exerted on the internal walls of the cavity.
• Diminishing the risk of postoperative sensitivity, which manifests particularly in the case of an unfavorable configuration of the cavity.
From this point of view, the cavity is evaluated by assessing the C factor.4,5,7,8 This permits the estimation of the ratio between the elements that define the configuration of the cavity and the value of stress developed due to the polymerization shrinkage. The C factor takes into consideration the number of cavity surfaces with or without adhesion, thus describing the relationship between the number of the cavity walls, the number of adhesive interfaces, and the polymerization shrinkage. Thus, the risk of the weakening of adhesion is determined by the increase of the polymerization shrinkage values, the condition of a higher number of cavity surfaces, and the use of a composite resin material with a higher consistency. It is estimated that the polymerization shrinkage value is minimum in the case of a freely flowing material, and consequently, the number of free surfaces without an adhesive interface is higher than that of the adhesion surfaces involved in the restoration.7
Thus, it becomes obvious that the composite material has a limited flow in the case of class I and V cavities, which are characterized by an unfavorable C factor, due to the existence of five surfaces presenting adhesive interfaces and only one free surface. In these situations, the direct consequence is an increase of internal stress occurring during the polymerization shrinkage, and consequently, a lowering of the chances for the maintenance of adhesion between the composite restoration material and the hard dental tissues. Thus, the use of flowable composite materials as an intermediate layer between the adhesive system found on the cavity floor and the restoration material becomes a necessity because of the possibility offered by the intrinsic characteristics and the behavior of these materials, which counteract the internal tensions caused by the polymerization shrinkage.3–7
10.1.4 Placement and shaping of the material – layering
The placement techniques for composite materials are aimed both at compensating the subsequent tendency of detachment from the cavity walls, caused by polymerization shrinkage, and facilitating the shaping and obtaining of the desired shades in the chromatic context of the teeth concerned.
The chromatic characteristics specific for posterior teeth generally make the selection of the colors of the composite material easier than for anterior teeth,2,10 and many manufacturers reduce the number of basic shades in the composite material kits concerned. A tendency to consider a single shade for dentin and a few shades for enamel can be observed.7–9
Establishing the color and shade details of the dental surfaces to be restored is recommended by assessing these aspects before isolation with a rubber dam, both at the level of the tooth concerned and of the neighboring and the contralateral tooth.
It should be noted that the shade of the material layer that will replace the dentin must be evaluated not only regarding the type of tooth, but also the age of the patient, which can significantly contribute to the alteration of tooth color.
The chromatic appearance of the material layer intended for the replacement of the enamel should take into consideration the characteristics of natural enamel, with a higher opalescence and brightness, obviously also depending on its thickness at the level of the different anatomy elements of the tooth-crown surfaces. Taking this into account, whiter shades are recommended for the restoration of enamel crests, and the use of pigments to evidence occlusal fissures and pits.7–9
Regarding the modalities of placement of the composite material for direct restorations of posterior teeth, there are several techniques depending on the size of the cavities to be restored, represented by the bulk application of the composite material, the horizontal layering technique, the oblique layering technique, the three-increment technique, and the four-increment technique.
10.1.4.1 The bulk placement of composite resin material
This is a modality recommended for small-size cavities, the so-called “preventive cavities”. In these situations, the reduced thickness of the composite material required for the restoration allows the curing shrinkage value to be assessed as being practically insignificant,2,7 and consequently, it permits the placement and polymerization of the material inside the entire cavity from the start.
10.1.4.2 The horizontal layering technique
The layer replacing the dentin is placed first, while respecting the shade and thickness of the dentin mass, as well as the cusp slopes and the appearance and depth of occlusal pits and fissures. Allowing enough space for the placement of the enamel-replacing layer, 0.5 to 1 mm thick, should be considered. Its placement and shaping should be according to the specific aspects for the tooth anatomy.
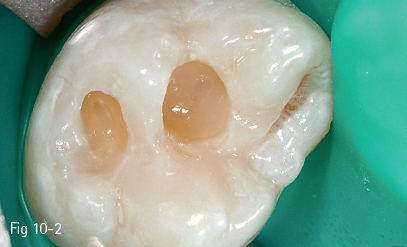
Fig 10-2 Horizontal layering on 27.
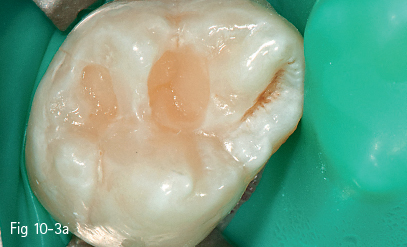
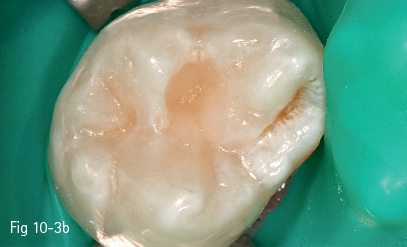
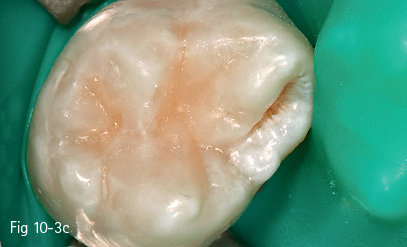
Fig 10-3 a–c Oblique layering on 27.
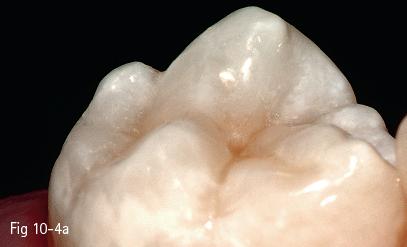
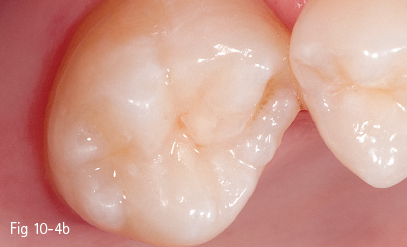
Fig 10-4 a, b Final appearance of the restoration.
Horizontal layering (Fig 10-2) with light curing from the direction of the cavity access opening is an adequate technique for deeper cavities with a smaller surface extension.2,7
10.1.4.3 The oblique layering technique
Larger-size cavities, with an extended surface and a depth estimated as medium to high, require placement and light curing in successive layers, due to a higher amount of composite material that will be applied, which increases the risk of internal tensions caused by the polymerization shrinkage. The use of horizontal layering techniques in these cases would allow for the development of important tensions, exerted on the opposite walls of that cavity.2,7–9
Although it is considered that the positioning of the light beam can affect the action direction of vectors according to which the polymerization shrinkage manifests, the elements that decisively influence the behavior of the restoration material during polymerization are the shape of the cavity and the value of adhesion. Therefore, the guidance of the light beam for curing through the cusp thickness can contribute to the orientation of shrinkage vectors towards the walls, not to the center of the cavity (although this is not an essential factor).
However, the shaping of the composite material can be facilitated by its placement using the oblique layering technique (Figs 10-3a, 10-3b, 10-3c, 10-4a, and 10-b), and trans-cusp light curing can be progressive (soft-start), which can contribute to the lowering of the polymerization shrinkage value of the resin composite and, implicitly, of the internal stress acting upon the cavity walls.
10.1.4.4 The three-increment technique
This modality of placing resin composite materials has been more recently indicated by some authors7–9 for small- and medium-size class I cavities.
The three increments are represented by:
• The application of a flowable composite layer to cover the dentin adhesive system found on the cavity floor.
• The placement of the composite material replacing the dentin in one layer.
• The placement of the composite material replacing the enamel in one layer, and its shaping at occlusal level.
10.1.4.5 The four-increment technique
This technique, even more recently indicated by a number of authors,7–9 for small- and medium-size class II cavities, is performed as follows:
• Placement of an enamel layer adjacent to the matrix, which will restore the missing proximal wall and the marginal ridge (conversion of a class II cavity into a class I cavity: the centripetal technique).
• Placement of the flowable composite for the covering of dentin on the cavity floor.
• Placement of the dentin mass in one layer.
• Placement of the enamel mass in one layer and occlusal shaping.
10.1.5 Finishing and polishing
By following the principles and the technical steps of the layering and occlusal shaping of the resin composite, a restoration that does not require occlusal adjustments can be achieved. Taking into consideration the occlusal anatomy (pits and fissures, cuspal slopes) during the placement steps, practitioners can avoid marginal gaps or material overhangs beyond the limits of the cavity. The need for post-curing contouring on the visible surfaces of the restoration is thus significantly reduced, which results in the absence of special finishing and polishing problems, particularly in class I cavities. Potential intervention areas are usually found at the tooth-restoration interface. The rest of the exposed surface of the restoration is only polished with rubber points with little or no abrasion, with the brushes impregnated with polishing paste. In this way, the finishing and polishing steps take very little time and are also aided by the high esthetic qualities of current composite resin materials.2,4,5,7–9
10.1.6 Clinical technique step-by-step
10.1.6.1 Isolation of the operating field
• Recording of occlusal contacts, anesthesia, and placement of the rubber dam.
• Cleaning of dental surfaces by using powder jet devices (bicarbonate, pumice stone powder, etc), with small-size prophylactic cups.
10.1.6.2 Cavity preparation and finishing
• Removal of pre-existing (metal or metal-free) restorations with adequate rotary instruments, at high speed.
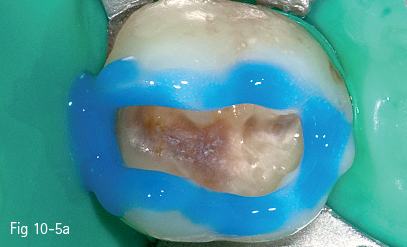
Fig 10-5 a Enamel etching.

Fig 10-5 b Dentin etching.
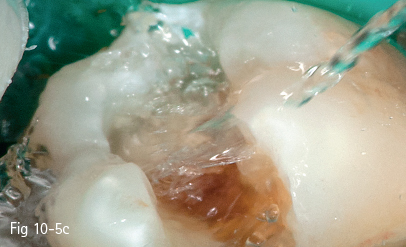
Fig 10-5 c Rinsing for 30 to 60 seconds.
• Preparation of the cavity with cylindrical or spherical fine diamond burs, mounted in the reduction contra-angle handpiece – red ring.
• Removal of the infected dentin with steel or carbide burs, mounted in the contra-angle handpiece – blue ring.
• Finishing of margins: beveling and finishing of the enamel with cylindrical fine burs or flame burs, mounted in the reduction contra-angle handpiece – red ring.
10.1.6.3 Enamel and dentin adhesion procedures
• Enamel and dentin etching (total etch), with 35% to 37% phosphoric acid (20 to 40 seconds for enamel, 10 to 20 seconds for dentin) (Figs 10-5a and 10-5b).
• Rinsing with water up to 30 to 60 seconds (Fig 10-5c) and gentle air drying to remove all humidity traces from the rubber dam sheet and the neighboring teeth, avoiding the penetration of the air jet straight inside the cavity in order to prevent tissue dehydration; after etching and rinsing and before the primer application, the application inside the cavity for 1 to 2 minutes of a 0.2% to 2% chlorhexidine solution, with antimicrobial and protease (MMPs) inhibitor role, has also been suggested.5
• Abundant application of the primer, by persistent rubbing against the dentinal walls for 30 to 60 seconds, with the frequent addition of new amounts of primer.
• Gentle air drying for 5 to 10 seconds; after drying, the surface should be glossy and bright.
• Application of the bonding resin on the enamel and dentin walls by rubbing for several seconds, forming a layer that is subsequently extended and reduced in thickness, using a gentle air jet.
• Light curing of the adhesive for 20 to 40 seconds.
• Application and light curing of a flowable resin composite layer on the cavity floor.
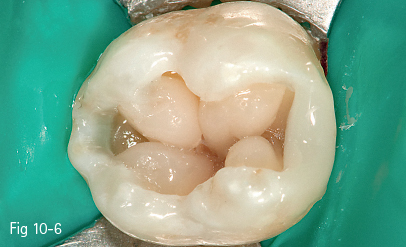
Fig 10-6 View during dentin layering for an occlusal restoration on tooth 37.
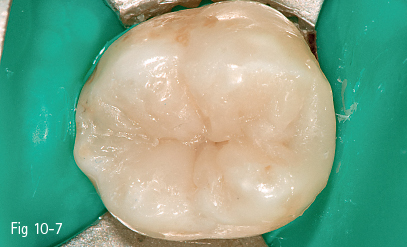
Fig 10-7 View after enamel layering for an occlusal restoration on tooth 37.
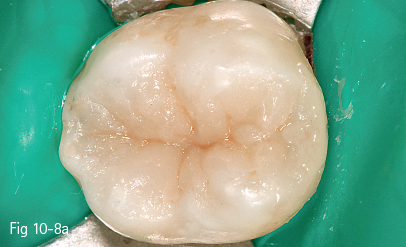
Fig 10-8 a View after tint application on tooth 37.
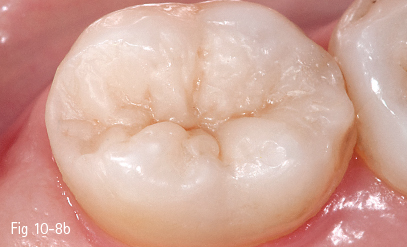
Fig 10-8 b Final view after finishing and polishing of the occlusal restoration.
10.1.6.4 Layering of the dentin composite mass
• Horizontal layering in narrow and deep cavities and progressive (soft-start) direct or usual light curing.
• Oblique layering and trans-cusp light curing (with additional occlusal light beam) in large cavities.
• Multiple increment layering according to anatomical principles, and shaping of cusp slopes and occlusal pits and fissures (Fig 10-6).
• Light curing of each composite increment.7
10.1.6.5 Layering of the enamel composite mass
• The bulk technique is applied for small-size cavities.
• Horizontal and oblique anatomical layering is used for larger cavities.
• The characterization of pits and fissures is performed.
• The different composite layers are light cured; at the last activation, the application of a fine glycerin gel layer in order to block the inhibitory effect of atmospheric oxygen and to allow the complete polymerization of the composite restoration surface is recommended.
• Mild finishing with fine and extra-fine diamond burs mounted in the reduction contra-angle handpiece – red ring.
• Polishing with medium and fine rubber points/cups and silicone polishers.
• Polishing with nylon and silicone brushes, together with polishing pastes.
• Removal of the rubber dam isolation, checking of occlusal contacts, and final control of the restoration (Figs 10-7, 10-8a, and 10-8b).
10.1.7 Characteristic aspects of direct restorations of posterior teeth in class II cavities
There are a number of characteristic aspects of direct restorations in class II cavities, which influence the indications, the techniques for the compensation of the polymerization shrinkage, the instruments and materials required for a correct restoration, and the sequence of operations used for the restoration.2,4,5,7–9 Some of these aspects will be outlined briefly, as follows.
These are the main indications for cavities with a small to medium extension, with the maintenance of an adequate enamel layer at the level of the cervical wall of the proximal cavity.2,4,5,7–9
Class II restorations should meet two essential clinical requirements:2,4,5,7–9
• Counteracting the effects of the polymerization shrinkage.
• The esthetic anatomical restoration of the concerned teeth.
The effects of the polymerization shrinkage, related to consecutive internal stress developed in the tooth-restoration unit, are mainly evidenced by two aspects:
• At the level of the cavity walls, through the tendency to deformation by tension, with the possible appearance of microfissures, followed by the partial or total fracture of some walls.
• At the level of the adhesive interface, in two areas:
– The external margins of the restoration, with the possible appearance of microleakage.
– The internal dentinal surfaces, with the possible appearance of postoperative hypersensitivity, by hydrodynamic mechanisms.4,5
The possible effects of the polymerization shrinkage are not immediately clinically evidenced in all cases, but can appear subsequently, after a latency period of several days or weeks (postoperative sensitivity), or even months (fissures or fractures).
The polymerization shrinkage is inherent and is correlated with three main factors:2,3,6–8
• The physical and chemical properties of composite resins.
• The adhesion force developed at the tooth-restoration adhesive interface.
• The three-dimensional configuration of the cavity and the consecutive C factor.
For the compensation of the polymerization shrinkage and the counteracting of its effects, different clinical approaches of direct composite restoration have been proposed:
• Application of special tips (Light-tip), with a condensation-polymerization role, at the end of the optical fiber guide of the curing unit.2,7
• The use of prefabricated ceramic inserts, incorporated in the composite resin mass, before polymerization, in order to reduce the volume of material subjected to shrinkage.2,7
NOTE: The two above-mentioned methods have a number of drawbacks:
•It is difficult to avoid the placement of excess material at the level of the marginal ridge, with real problems in correctly obtaining the interproximal contact point.
•It is difficult to obtain the correct natural shape and color of the restored tooth.
•The finishing and polishing procedures become more complicated.
•The total working time is prolonged.
It is for the above reasons that these methods are practically impossible to use in current practice and are used only in exceptional situations.
The use of multiple layer placement and polymerization techniques, various application sequences, various three-dimensional spatial positioning, and various orientations of the light beam (horizontal technique, three-direction polymerization technique, oblique technique, three-increment technique, four-increment technique – centripetal technique) seems to be the most adequate approach, according to most opinions.2,4,5,7–9
For the esthetic anatomical restoration of posterior teeth by direct techniques in class II cavities, another important aspect is represented by the necessary instruments and accessories.
In addition to adequate instruments for the placement and shaping of composite resin, a decisive role for the quality of these restorations is played by dental matrices, along with interdental wedges, through their correct use.4,5,7,8
For the restoration of the proximal contour and obtaining the proximal interdental contact, partial matrices (half-matrices) with the double convexity of the matrix band in buccal-oral and occlusal-cervical direction are recommended. They are accompanied by an elastic metal ring which accomplishes a double role: maintaining the matrix in position (similarly to classical matrix holders) and minimally separating the teeth (within physiological limits of the marginal periodontium), in order to obtain the contact point.
These types of matrices were specifically designed for direct adhesive composite restorations. The best known and most widely used matrices are:17
• The Palodent matrix system, with Bi-Tine rings.
• Silver Plus G rings; the rings of this system have two variants: with long or short interdental arms.
• The Composi-Tight GDS 3D matrix system, with Soft Face 3D rings; the rings of this system have three-dimensionally modeled extremities of the interdental arms, following the morphology of the interdental embrasure, by means of attached elastic silicone tips).
• The V-Ring matrix system with attached rings.
Mesio-occlusodistal cavities require circular (circumferential) matrices, starting from the classical Tofflemire type. The AutoMatrix type is widely used for these types of cavities. It can be introduced, adapted, and maintained in position with optimal results for the final quality of the restoration.
REFERENCES
1. Garber DA, Goldstein RE. Porcelain and Composite Inlays and Onlays: Esthetic Posterior Restorations. Chicago: Quintessence, 1994.
< div class='tao-gold-member'>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses