Introduction
An increase in the number of adults seeking orthodontic treatment has given rise to new problems for orthodontists, one of which is the need to bond orthodontic brackets to teeth restored with temporary crowns. Many prefabricated temporary crowns are composed of polycarbonates or thermoplastic polymers; bonding to these surfaces is complex because of the composition, surface integrity, and resistance of the crowns. The bond must be sufficient to resist breakage from the forces of orthodontic biomechanics and oral functions including mastication. The purpose of this study was to test, in vitro, the effect of different surface treatments on the shear bond strength of metal and ceramic orthodontic brackets bonded to temporary polycarbonate crowns.
Methods
Eighty polycarbonate crowns for the maxillary right central incisor were evenly divided into 4 groups, and the facial surfaces were subjected to one of the following conditions: group A (control): no treatment; group B: the surface was sandblasted with 50 μm aluminum oxide particles; group C: the glazed surface was removed with a diamond bur; and group D: the surface was etched with 9.6% hydrofluoric acid. Precoated Victory metal brackets (3M Unitek, Monrovia, Calif) were bonded to the facial surface of half (n = 10) of the polycarbonate crowns in each group, and precoated Clarity ceramic brackets (3M Unitek) were bonded to the facial surface of the other half (n = 10). Each was debonded with a shear load in a universal testing machine at a crosshead speed of 0.254 mm per minute, and the adhesive remnant index (ARI) was used to analyze the sites of bond failure. Analysis of variance (ANOVA), post-hoc t test with the Bonferroni adjustment, Student t test, and chi-square test with the Yates correction were used for statistical analysis.
Results
There was a significant difference between group B (sandblasting) and all other ceramic and metal groups. In the metal groups, there was a slight difference between group C (diamond bur) and group A (control). According to the ARI, sandblasting was the only surface treatment to significantly affect the adhesion of metal and ceramic brackets to polycarbonate crowns. There was no statistically significant difference between the metal and ceramic brackets in group B (sandblasting). There was a statistically significant difference between metal and ceramic brackets in each group, with the exception of group C (diamond bur), which was just below statistical significance.
Conclusions
Metal and ceramic orthodontic brackets bonded to temporary polycarbonate crowns will most likely not withstand the forces of orthodontic biomechanics. However, sandblasting polycarbonate crowns consistently increased the shear bond strength of metal and ceramic brackets. A diamond bur effectively roughens the surface of a polycarbonate crown but with no gain in bond strength. Likewise, etching the surface of polycarbonate crowns with 9.6% hydrofluoric acid is ineffective. Ceramic brackets bonded to sandblasted polycarbonate crowns produced the highest mean shear bond strength (2.87 MPa), although this value is far below bond strengths with natural tooth surfaces.
An increase in the number of adults seeking orthodontic treatment has given rise to new problems for orthodontists. These patients often have restored teeth, creating a problem for the bonding of orthodontic brackets onto these teeth. In multidisciplinary treatments, teeth often have temporary crowns during orthodontic treatment because of the benefit of sequencing the placement of the final restorations until the teeth have been moved into more appropriate positions. Although bands can be placed on some teeth that have temporary crowns, particularly in the posterior region, this might not be an acceptable solution in the anterior areas because of esthetic considerations. In addition, bands are not possible on the abutment teeth of fixed bridges. Banded teeth have also been associated with plaque-control problems.
Many prefabricated temporary crowns are composed of polycarbonates, which are a type of thermoplastic polymer. The characteristics of polycarbonates are similar to those of polymethylmethacrylate, but polycarbonate is stronger and more costly. Bonding brackets to polycarbonate crowns is complex because of the composition, surface integrity, and resistance of the crowns. Due to the composition of polycarbonate crowns, they are fairly resistant to dilute acids and do not etch well. In addition, the surface integrity depends on the finishing procedure and whether the surface is glazed.
Although there have been numerous studies on increasing bond strength of orthodontic brackets to enamel and porcelain, no research has been done on the bond strength of orthodontic brackets bonded to polycarbonate. In general, acid etching, sandblasting, and roughening the surface with a diamond bur have been investigated as methods to increase bond strength. Although conventional acid etching with 37% phosphoric acid is effective for enamel, this is ineffective for the preparation of porcelain surfaces for bonding orthodontic brackets. Strong acids such as 9.6% hydrofluoric acid are commonly used to etch porcelain and increase bond strength. The action of hydrofluoric acid is to create surface pits by preferential dissolution of the glass phase from the ceramic matrix. However, hydrofluoric acid must be used carefully, since it is extremely corrosive and can cause severe trauma to soft tissues and tooth substance.
Orthodontic brackets need to be retained either mechanically or chemically to the polycarbonate crown. The bond strength should be sufficient to resist failure from the forces of orthodontic biomechanics and oral functions including mastication. The materials and techniques used in bonding should keep the brackets bonded for the duration of treatment and not damage the crown’s surface during debonding. The purpose of this research was to examine, in vitro, the effect of different surface treatments on the shear bond strength of metal and ceramic orthodontic brackets onto temporary polycarbonate crowns.
Material and methods
Polycarbonate crowns (Henry Schein, Melville, NY) for the maxillary right central incisor (n = 80) were used in this study. The facial surface of each crown was pumiced with a rubber prophylaxis cup in a low-speed electric hand piece. The surfaces were then rinsed with a steady stream of water for 20 seconds and dried with a mild continuous stream of oil-free and humidity-free compressed air. The specimens were evenly divided into 4 groups, and the facial surface was subjected to one of the following conditions: group A (control): no treatment, with the glaze maintained; group B: the surface was sandblasted with 50 μm aluminum oxide particles under 90 psi of air pressure with the nozzle held 10 mm from the surface until the surface was completely frosted; group C: the glaze was removed with a diamond bur (850-014, Axis Dental, Coppell, Tex); group D: the surface was etched with 9.6% hydrofluoric acid for 4 minutes (Pulpdent,Watertown, Mass). Specimens representative of each group were coated with a conductive layer of gold and examined with a scanning electron microscope (JSM-5600, JEOL, Tokyo, Japan).
The specimens of groups B, C, and D were rinsed again with a steady stream of water for 30 seconds and dried with oil-free and humidity-free compressed air. Three coats of the primer (Scotchprime Ceramic Primer, 3M Unitek, Monrovia, Calif) were painted onto the facial surfaces of the polycarbonate crowns in every group with a disposable brush and lightly dried with oil-free and humidity-free compressed air. Precoated Victory metal brackets (3M Unitek) were bonded to the facial surface of half (n = 10) of the polycarbonate crowns in each group, and precoated Clarity ceramic brackets (3M Unitek) were bonded to the facial surface of the other half (n = 10) in each group ( Fig 1 ). The adhesive used for all precoated brackets was Transbond XT light-curing adhesive (3M Unitek). Each bracket was positioned with a scaler, and excess adhesive was removed from the surface. All brackets were light cured with a Blue Ray light-emitting diode lamp (American Orthodontics, Sheboygan, Wis) for 40 seconds.

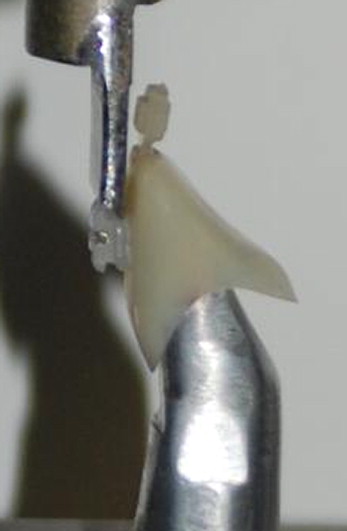
A specimen fixture was designed and fabricated from aluminum. Each sample was mounted on the specimen fixture. A small portion of dental wax was placed inside the polycarbonate crowns to secure it to the fixture. Each sample was subjected to a shear load with a universal testing machine (model SSTM-1, United, Huntington Beach, Calif) fitted with 5000-lb and 50-lb load cells. The readings were taken from the 50-lb load cell. A knife-edged blade from the upper fixture was fitted into the groove between the outer edge of the bracket and the polycarbonate crown ( Fig 2 ). The tests were run by using the testing machine software, DATUM 4.0 (United). The crosshead speed was set to 0.254 mm per minute. The machine recorded the results in newtons. The force per unit of area required to dislodge the bracket was then calculated and reported as the shear bond strength in megapascals (MPa). The bracket base areas for the Victory metal brackets and the Clarity ceramic brackets were 11.9 mm 2 and 14.6 mm 2 , respectively.
After debonding, an optic microscope with 10-times magnification was used to examine all bonding sites and classify them according to the adhesive remnant index (ARI). The ARI was used to analyze the sites of bond failure between the polycarbonate crown surface, the adhesive, and the bracket base.
Statistical analysis
Descriptive statistics including means, standard deviations, and minimum and maximum values were calculated for every group. Analysis of variance (ANOVA) was used to determine whether there were significant differences in the shear bond strength between the groups. If there were significant differences, a post-hoc t test with the Bonferroni adjustment was used to determine which means were significantly different from each other. The Student t test was used to determine significant differences between metal and ceramic brackets. The chi-square test with the Yates correction was used to determine the statistical significance of the ARI scores. The level of significance for all statistical tests was established as P ≤0.05.
Results
The mean shear bond strengths, standard deviations, and ranges of all groups are given in Table I .
| Group | Bracket-surface treatment | n | Mean | SD | Range |
|---|---|---|---|---|---|
| A | Metal-control | 10 | 0.012 | 0.010 | 0.036-0.003 |
| Ceramic-control | 10 | 0.070 | 0.040 | 0.296-0.037 | |
| B | Metal-sandblasting | 10 | 1.330 | 0.170 | 1.515-1.107 |
| Ceramic-sandblasting | 10 | 2.870 | 0.360 | 3.534-2.331 | |
| C | Metal-diamond bur | 10 | 0.134 | 0.064 | 0.217-0.065 |
| Ceramic-diamond bur | 10 | 0.090 | 0.020 | 0.117-0.051 | |
| D | Metal-etch (HF acid) | 10 | 0.099 | 0.030 | 0.137-0.044 |
| Ceramic-etch (HF acid) | 10 | 0.030 | 0.020 | 0.065-0.009 |
ANOVA was used on the ceramic brackets bonded to the facial surface of the polycarbonate crowns in the 4 groups. Since the test produced a Fisher F value of 596.96 ( P = 0.000), it was determined that there was a statistically significant difference among the groups. The post-hoc t test with the Bonferroni adjustment determined that a significant difference existed between group B (sandblasting) and all other ceramic groups.
ANOVA was also used on the metal brackets bonded to the crowns in the 4 groups. It was also determined that a statistically significant difference existed among the groups, since the test produced a Fisher F value of 461.484 ( P = 0.000). When the post-hoc t test with the Bonferroni adjustment was performed, it was determined that a significant difference existed between group B (sandblasting) and all other metal groups, and a slight difference existed between group C (diamond bur) and group A (control).
The ARI results ( Table II ) showed that all groups bonded with ceramic or metal brackets scored 0, since no adhesive was left on the polycarbonate crowns, except for some specimens in group B (sandblasting) for ceramic and metal brackets. Some specimens in this group scored 1 and had less than half of the adhesive left on the crown. The chi-square test with the Yates correction was done to determine whether the ARI scores between the ceramic and metal brackets in group B (sandblasting) were statistically significant. The results showed no statistically significant difference (chi-square = 0.202 with 1 degree of freedom and P = 0.6531) between the metal and ceramic brackets in group B.
| Group | Bracket-surface treatment | n | 0 | 1 | 2 | 3 |
|---|---|---|---|---|---|---|
| A | Metal-control | 10 | 10 | 0 | 0 | 0 |
| Ceramic-control | 10 | 10 | 0 | 0 | 0 | |
| B | Metal-sandblasting | 10 | 5 | 5 | 0 | 0 |
| Ceramic-sandblasting | 10 | 6 | 4 | 0 | 0 | |
| C | Metal-diamond bur | 10 | 10 | 0 | 0 | 0 |
| Ceramic-diamond bur | 10 | 10 | 0 | 0 | 0 | |
| D | Metal-etch (HF acid) | 10 | 10 | 0 | 0 | 0 |
| Ceramic-etch (HF acid) | 10 | 10 | 0 | 0 | 0 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


