Introduction
The aim of this study was to see the effect of a single dose of low-level laser therapy on spontaneous and chewing pain after the placement of elastomeric separators.
Methods
Eighty-eight patients were randomly selected for this single-blind study. Elastomeric separators were placed mesial and distal to the permanent first molars in all quadrants. Both arches were divided into experimental and control sides. The experimental sides were treated with low-level laser therapy on 3 points on the buccal mucosa for 20 seconds each, with a 940-nm gallium-aluminum-arsenic diode laser on continuous mode and power set at 200 mW. The other side received placebo laser therapy without turning on the laser. A numeric rating scale was used to assess the intensity of spontaneous and chewing pain for the next 7 days. The independent sample t test and repeated-measures analysis of variance with the post hoc Tukey test was used to analyze the results.
Results
Significant differences were found in spontaneous and chewing pain among both groups ( P <0.05).
Conclusions
A single dose of low-level laser therapy can be an efficient modality to reduce the postoperative pain associated with the placement of elastomeric separators.
Highlights
- •
Placement of separators causes postoperative spontaneous and chewing pain.
- •
In the literature, multiple applications of low-level laser therapy reduced pain.
- •
The effect of low-level laser therapy on chewing pain has not been studied.
- •
We assessed a single dose of low-level laser therapy on spontaneous and chewing pain.
- •
One dose of low-level laser therapy reduces both types of pain.
Orthodontic treatment with fixed appliance improves dentofacial esthetics as well as masticatory function, but it is also associated with discomfort and pain. It has been reported that more than 90% of orthodontic patients experience varying degrees of pain after the placement of elastomeric separators, initial wire insertions, and activations. The pain usually begins within 4 hours after the procedure, has its peak at 24 hours approximately, and dissipates by day 7. The intensity of the pain is sometimes perceived as even greater than the pain related to extractions and thereby becomes a major deterrent to treatment or a reason for premature discontinuation of orthodontic treatment.
The placement of elastomeric separators is a part of routine fixed appliance therapy to create space for molar bands. This process causes displacement of teeth and the immediate release of biochemicals in the gingival fluid, followed by an increase in the level of prostaglandins E2 and interleukin-1 the next day. Therefore, the intensity of pain is at its highest after 24 hours, remains bothersome for the next 3 days, and diminishes over the next 6 to 8 days. Most patients report pain on chewing for which they have to change their dietary pattern during the separation period. Since this pain is inflammatory, nonsteroidal anti-inflammatory drugs are the gold standard in reducing the discomfort. However, the systemic effects of these drugs, including their deceleration effect on the rate of tooth movement and the necessity for the patient’s compliance in taking the medications, should be considered. Other methods such as bite wafers, vibratory stimulation, transcutaneous electrical nerve stimulation, and chewing gum have achieved pain reduction to some degree, but the effects are highly variable.
Low-level laser therapy (LLLT) has also been reported to have analgesic effects in many clinical applications. Although the mode of action of LLLT is still not clear, investigators relate its analgesia with anti-inflammatory and neuronal effects. It has been reported that LLLT not only excites neural cells and lymphocytes, resulting in the release of neurotransmitters into inflammatory tissues, but also inhibits neural signaling that further reduces the pain perception. It also increases local blood circulation that removes the pain-inducing inflammatory mediators and enhances the cellular activities (biostimulation).
Some investigators have reported significant results in pain reduction after applying multiple and frequent doses of LLLT. Considering the convenience of patients, a few researchers have attempted a single dose of LLLT and found significant results. Lim et al applied a single dose of LLLT to reduce separation pain with the split-mouth design, but only postoperative spontaneous pain for 5 days was recorded, and no consideration was given to pain on chewing.
Only a few studies have been conducted to observe the effects of LLLT on the reduction of chewing pain associated with separator placement. Therefore, the purpose of this research was to evaluate the effect of a single dose of LLLT on not only the spontaneous pain but also the chewing pain caused by the placement of separators.
Material and methods
This single blind, placebo-controlled, split-mouth study was conducted at the Orthodontic Department of Baqai Dental College, Baqai Medical University, in Karachi, Pakistan. The study was approved by the ethics committee of Baqai Medical University. The sample comprised 88 Pakistani patients (60 female, 28 male; age range, 13-30 years). The inclusion criteria were patients with no history of orthodontic treatment, healthy and complete dentition including permanent second molars, good periodontal health, and tight proximal contacts of all permanent first molars (both mesially and distally). Patients with multiple fillings, root canal treatments, gingivitis, multiple missing teeth, or spacing between molars and premolars were excluded from the sample. We explained the procedures verbally to the patients, and voluntary participation was ensured by obtaining signatures on the informed consent form. Consent forms of participants less than 18 years of age were signed by a parent. Subjects who refused to participate in the clinical trial received the standard treatment.
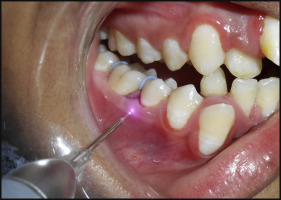
The sample size was calculated using power analysis with an anticipated mean difference of 2 points in pain on the numeric rating scale between the experimental and the placebo groups with a standard deviation of 2. The sample had at least a 90% power at α of 0.05. The total number of patients included in this study was higher than the number calculated. In all selected patients, elastomeric separators (3M Unitek, Monrovia, Calif) were placed using dental floss (Oral B; Procter & Gamble, Cincinnati, Ohio) interproximally across the permanent first molars (both mesially and distally) in all quadrants. Both arches in each patient were divided into experimental and placebo sides (groups) randomly by flipping a coin. Immediately after placement of the separators, LLLT was applied on the experimental side using a 940-nm gallium-aluminum-arsenic diode laser (iLase; Biolase, Irvine, Calif) on continuous mode with power set at 200 mW. The laser was applied buccally on 3 points: mesial, distal, and middle of the root of the permanent first molar for 20 seconds each. The vertical level of application was approximately at the center of the root with the fiber tip of the laser placed nearly perpendicular in close contact with the gingival tissue ( Fig 1 ). The energy dose (200 × 20) was 4 J per square centimeter at each point and 12 J per square centimeter on the whole. We made sure that while working on the intervention side, the emitted light was not allowed to affect the placebo side. On the placebo side, the laser was held the same way and for the same duration but without turning it on. The operator, assistant, and patient all wore protective glasses, and the procedure was carried out in an isolated room.
A questionnaire was formulated using the numeric rating scale and was given to all the patients to record their pain daily and for 7 days. The patients were advised that 0 indicated no pain and 10 indicated unbearable pain. The patients were asked to record spontaneous pain as well as pain on chewing after every 24 hours for the entire week. Analgesics were discouraged, but if they were taken, the patients were advised to note it. All patients were reminded by daily phone calls to record their entries as advised.
Statistical analysis
The data were analyzed using SPSS software (version 20.0; IBM, Armonk, NY). Independent sample t tests were applied to compare the mean pain scores between the experimental and the placebo sides for spontaneous and chewing pain. Repeated measures analysis of variance was used to evaluate the differences in the levels of pain during the week.
Results
The duration of this study was 5 months (January-May 2014). Initially, 90 patients were recruited, but 2 did not comply. One patient did not fill out the questionnaire, and the other took analgesics for pain. Both were excluded from the study. Therefore, the sample comprised 88 patients with a mean age of 18.56 years.
There was a significant difference ( P <0.05) between the LLLT and the placebo groups on spontaneous pain perceived by the patients for all 7 days ( Table I ). Table II shows a statistically significant difference in pain on chewing between the 2 groups for all 7 days. The maximum intensity of discomfort was associated with chewing pain in the placebo group. Although the LLLT reduced the pain perception on chewing in the LLLT group, it was still greater than the spontaneous pain in that group ( Fig 2 ). The patients had maximum pain at 24 hours after the placement of the separators, and it declined significantly on the third day in almost all groups; however, the spontaneous pain in the LLLT group reduced more gradually. Figure 2 shows that some pain was still there in all groups even on day 7.
| Day | Group | Mean | SD | Mean difference | P value |
|---|---|---|---|---|---|
| 1 | LLLT | 1.86 | 2.50 | 3.18 | 0.000 ∗ |
| Placebo | 5.04 | 3.24 | |||
| 2 | LLLT | 1.54 | 2.37 | 3.00 | 0.000 ∗ |
| Placebo | 4.54 | 3.27 | |||
| 3 | LLLT | 1.18 | 1.83 | 2.31 | 0.000 ∗ |
| Placebo | 3.50 | 3.48 | |||
| 4 | LLLT | 0.72 | 1.39 | 0.86 | 0.015 ∗ |
| Placebo | 1.59 | 2.98 | |||
| 5 | LLLT | 0.59 | 1.56 | 1.31 | 0.001 ∗ |
| Placebo | 1.90 | 3.23 | |||
| 6 | LLLT | 0.36 | 0.88 | 1 | 0.003 ∗ |
| Placebo | 1.36 | 2.97 | |||
| 7 | LLLT | 0.31 | 0.87 | 1.13 | 0.001 ∗ |
| Placebo | 1.45 | 3.02 |
| Day | Group | Mean | SD | Mean difference | P value |
|---|---|---|---|---|---|
| 1 | LLLT | 2.50 | 3.48 | 3.18 | 0.000 ∗ |
| Placebo | 5.68 | 3.54 | |||
| 2 | LLLT | 2.45 | 3.24 | 2.68 | 0.000 ∗ |
| Placebo | 5.13 | 3.47 | |||
| 3 | LLLT | 1.22 | 2.22 | 2.27 | 0.000 ∗ |
| Placebo | 3.50 | 3.74 | |||
| 4 | LLLT | 0.59 | 1.59 | 1.22 | 0.001 ∗ |
| Placebo | 1.81 | 3.16 | |||
| 5 | LLLT | 0.50 | 1.31 | 1.31 | 0.000 ∗ |
| Placebo | 1.81 | 3.07 | |||
| 6 | LLLT | 0.50 | 1.31 | 0.90 | 0.011 ∗ |
| Placebo | 1.40 | 3.02 | |||
| 7 | LLLT | 0.48 | 1.38 | 0.98 | 0.007 ∗ |
| Placebo | 1.47 | 3.07 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


