(1)
Dept. of Oral and Maxillofacial Surgery/Oral Pathology of thr VU University Medical Center/ACTA, Amsterdam, The Netherlands
3.1 Introduction
Many diseases that affect the oral mucosa may occur on the lips as well. However, there are a number of lesions that exclusively or preferably affect the lips. Both types of lesions will be discussed in this chapter.
3.2 Acanthosis Nigricans
Definition
Pigmented papillomatous cutaneous lesion that occasionally involves the lips. Acanthosis nigricans may be a manifestation of a gastrointestinal malignant tumor.
Etiology
The etiopathogenesis is unknown.
Epidemiology
Rare phenomenon.
Clinical Aspects
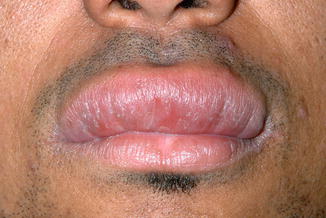
Multiple papillomatous lesions of the labial mucosa; in contrast to the cutaneous lesions, pigmentation of the labial lesions is rare (Fig. 3.1).
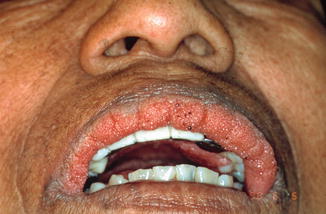

Fig. 3.1
Acanthosis nigricans of the upper lip
Treatment
It is not feasible to remove the numerous papillomatous lesions.
3.3 Cheilitis
3.3.1 Cheilitis Actinica
Definition
Inflammatory-like, premalignant disease of the lips caused by excessive exposure to sunlight. Some pathologists only report a diagnosis of cheilitis actinica when there is epithelial dysplasia.
Etiology
Apart from excessive exposure to sunlight, smoking may play a role in the etiology.
Epidemiology
Mainly in men; usually above the age of 50–60 years.
Clinical Aspects
Solitary or multiple, often recurrent but otherwise asymptomatic crusts on the vermillion border of the lower lip (Fig. 3.2); the upper lip is, indeed, rarely involved.
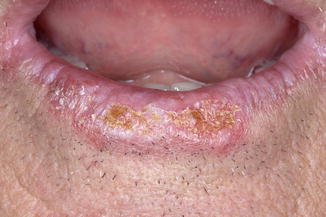

Fig. 3.2
Clinical aspect of actinic cheilitis
Clinical Differential Diagnosis
The main clinical differential diagnosis relates to a squamous cell carcinoma; in case of doubt, a biopsy should be taken.
Histopathology
Various degrees of hyperkeratosis with or without the presence of epithelial dysplasia may be observed (Fig. 3.3). In the subepithelial connective tissue, basophilic amorphic changes can be observed, referred to as actinic elastosis.
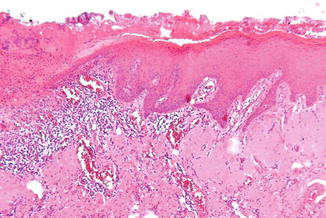

Fig. 3.3
Low-power view of actinic cheilitis
Occasionally, it may be difficult for the pathologist to render a firm diagnosis of actinic cheilitis based on a biopsy, particularly with regard to the distinction of a squamous cell carcinoma (“…most likely actinic cheilitis, but a squamous cell carcinoma cannot be ruled out”). As has been mentioned before, some pathologists use the diagnosis of actinic cheilitis only in the presence of epithelial dysplasia. In this respect, proper communication between the clinician and pathologist is essential in order to prevent any misunderstanding.
Treatment
In the absence of epithelial dysplasia, follow-up may be advised, e.g., twice a year.
In case of epithelial dysplasia or because of esthetic reasons, treatment may be instituted, e.g., by superficial surgical removal of the vermillion border (“lip shave”); also laser evaporation may be applied provided the biopsy has not shown signs of malignancy. Other treatment modalities include the topical use of trichloracetic acid and other ointments such as 5-fluorouracil.
3.3.2 Cheilitis Angularis
Definition
Inflammatory-like lesion of the commissures of the lips (“perlèches”).
Etiology
The etiology is unclear; several factors may play a role, such as decreased vertical dimension of the jaws in denture wearers. Apparently, C. albicans may play a role as well. Also, the possibility of an underlying disorder, such as vitamin B deficiency or folic acid deficiency, has been mentioned as possible causative factors. In some patients, none of the aforementioned causes can be identified.
Epidemiology
Angular cheilitis occurs only in adults and elderly persons; mainly in women.
Clinical Aspects
Cracked, reddish, and atrophic changes of the mucosa of the commissures, painful; usually bilateral distribution (Fig. 3.4).
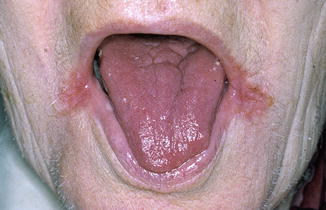

Fig. 3.4
Bilateral angularis cheilitis in an elderly woman
Treatment
Adjustment of the vertical height of the jaws, if applicable. Local application of antifungals may be helpful. Some advise to prescribe a mixture of antifungals and antibiotics, such as neomycin sulfate.
3.3.3 Cheilitis Exfoliativa
Definition
Inflammatory-like condition of the lips due to epithelial exfoliation.
Etiology
Habitual biting (“morsicatio”) on the lips, occasionally driven by automutilation. In most instances, such habits are denied by the patient.
Clinical Aspects
Crust formation on the lower or upper lip; usually not painful (Fig. 3.5).
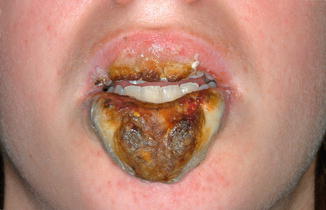

Fig. 3.5
Rather severe manifestation of exfoliative cheilitis, probably caused by automutilation
Treatment
It is often difficult for the patient to discontinue the habit, in spite of the often unpleasant cosmetic appearance.
3.3.4 Cheilitis Fissurata (Fissured Lip)
Definition
Fissuring of the mucosa of the vermillion border of the upper or lower lip.
Etiology
The cause of the fissuring is actually unknown.
Epidemiology
Rare phenomenon, almost exclusively occurring in adults.
Clinical Aspects
Superficial, often painful fissuring of the mucosa, usually in the midline (Fig. 3.6). Absence of induration.
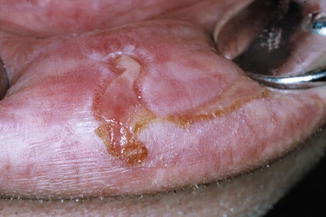

Fig. 3.6
Cheilitis fissurata of the lower lip
Histopathology
There are no pathognomic histopathological features.
Treatment
Since there is hardly any tendency for spontaneous healing, surgical correction may be considered.
3.3.5 Cheilitis Glandularis
Definition
Inflammation of the minor, intraoral salivary glands (see also Chap. 2).
Etiology
Most likely caused by a retrograde infection from the oral cavity.
Epidemiology
Mainly in adults.
Clinical Aspects
The clinical manifestation consists of often painful solitary or multiple painful nodules, being firm elastic on palpation. Sites of preference are the lips and the buccal mucosa. When solitary, the differential diagnosis includes a sialolith, a salivary gland neoplasm or, rarely, a foreign body reaction to cosmetic fillers (Fig. 3.7).
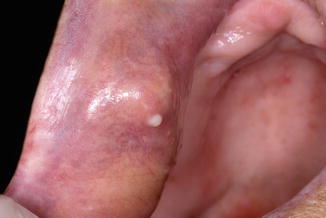

Fig. 3.7
Nodule in the upper lip caused by glandular cheilitis
Histopathology
Nonspecific chronic inflammation of the salivary glands.
Treatment
In general, conservative surgical excision suffices.
3.3.6 Cheilitis Granulomatosa
Definition
Inflammatory-like swelling of the upper or lower lip. Can be a manifestation of Melkersson-Rosenthal syndrome (a combination of cheilitis granulomatosa, fissured tongue, and transient facial paralysis; this triad does not necessarily occurs simultaneously).
Etiology
Unknown; in rare instances, granulomatous cheilitis is a manifestation of an underlying disease such as Crohn’s disease or sarcoidosis.
Epidemiology
Mainly in adolescents and adults.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses