(1)
Dept. of Oral and Maxillofacial Surgery/Oral Pathology of the VU University Medical center/ACTA, Amsterdam, The Netherlands
7.1 Introduction
In this chapter lesions and disorders are dealt with that may occur in the jaw bones. A distinction can be made between osseous lesions and lesions that are of odontogenic origin, such as odontogenic infections, cysts, and tumors. Furthermore, the jaw bones may be involved in a number of systemic diseases and syndromes.
7.2 Cysts of the Jaw Bones
The nasopalatine duct cyst has been dealt with in the chapter of diseases of the palate (Chap. 6), since the clinical presentation, if applicable, is almost invariably a swelling of the palate. Because of its extremely rare occurrence, the intraosseous dermoid cyst is not discussed here.
7.2.1 Aneurysmal Bone Cyst
Definition
Entity of which occurrence in the jaw bones is somewhat disputed. An aneurysmal bone cyst of the jaw bones may actually represent cyst formation in a preexistent osseous lesion such as a central giant cell lesion.
Etiology
The etiology is unknown.
Clinical Aspects
Usually located in the lower jaw; presents itself as a swelling.
Radiographic Aspects
Uni- or multilobular well-defined radiolucent lesion (Fig. 7.1).
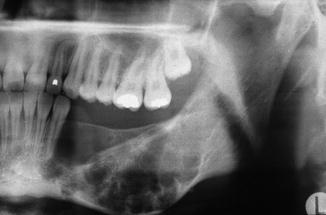

Fig. 7.1
Radiographic aspect of a possible aneurysmal bone cyst of the mandible
Histopathology
The histopathology shows connective tissue with lacunae and clefts filled with blood. Occasional multinucleated giant cells and osteoid formation are observed (Fig. 7.2).
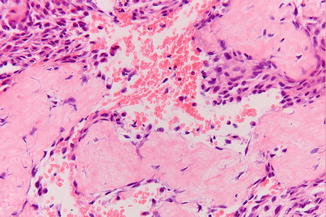

Fig. 7.2
Histopathologic aspect compatible with a diagnosis of aneurysmal bone cyst
Treatment
Enucleation. Because of the scarcity of reported cases, no information is available about possible recurrences.
7.2.2 Simple Bone Cyst
Definition
Intraosseous cavitation of unknown origin. May also occur elsewhere in the skeleton.
Synonyms are hemorrhagic bone cyst, traumatic bone cyst, and solitary bone cyst.
Due to the absence of cyst epithelium, it is in fact incorrect to use the term “cyst.”
Epidemiology
Only occurs in young people.
Clinical Aspects
When occurring in the jaw only, the mandible is affected. Usually an incidental finding on a radiograph without any symptoms. There is no swelling. The teeth in the affected area of the jaw remain vital.
Radiographic Aspects
Well-defined (“corticated”), often lobulated radiolucency around and between the roots of the teeth (Fig. 7.3). The nondistinctive radiographic aspect gives room for an extensive differential diagnosis such as keratocystic odontogenic tumor, ameloblastoma, and giant cell lesion.
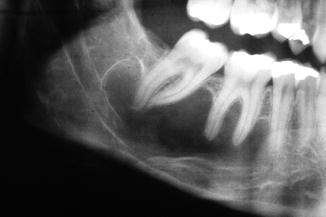

Fig. 7.3
Radiographic aspect compatible with, but not diagnostic of a simple bone cyst
Diagnosis
The diagnosis “simple bone cyst” is based on the finding of an empty cavity on exploration, occasionally being filled with some fluid and being lined by delicate fibrous tissue without epithelial lining (Fig. 7.4).
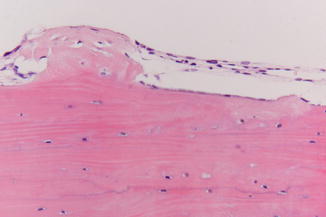

Fig. 7.4
Delicate fibrous lining of a simple bone cyst; no epithelial lining
Treatment
The surgical exploration that is required to obtain a diagnosis at the same time represents the treatment. There is no need to insert any type of implant material in the empty cavity. Recurrence (persistence) is rare. In such event one may choose just to follow the patient instead of repeating an exploration.
7.2.3 Latent Bone Cyst (Stafne’s Bone Cyst)
Definition
The latent bone cyst is actually based on an impression of the lingual cortex of the mandible, usually in the region of the angle (Fig. 7.5). In fact the term “cyst” is incorrect as there is no cavity lined with epithelium. Some prefer the term “lingual cortical mandibular defect.”
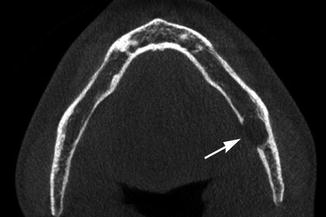

Fig. 7.5
CT scan shows the lingual depression in the mandible; not a true cyst
Epidemiology
The estimated prevalence is less than 0.1 %. The defect rarely becomes visible under the age of 40 years and is more common in men than in women. Bilateral occurrence is extremely rare.
Radiographic Aspects
Well-circumscribed round or oval radiolucency near the angle of the mandible, below the level of the mandibular canal (Fig. 7.6). The absence of symptoms, the localization, and the radiographic image usually allow to make a final diagnosis. In case of doubt, a CT scan can be performed in order to demonstrate the mandibular lingual defect.
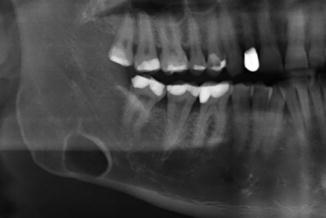

Fig. 7.6
Latent bone cyst below the mandibular canal; incidental finding
Treatment
Exploration is only indicated in case of doubt. It is interesting to mention that after having made a window in the intact buccal cortical bone, one, sometimes somewhat confusing, immediately enters the floor of the mouth and not an intraosseous cavity.
7.3 Cysts and Tumors of Odontogenic Origin
General Aspects
Cysts lined by odontogenic epithelium. Some cysts are caused by an inflammatory stimulus (inflammatory cysts), while for other cysts such a stimulus is unknown, being referred to as developmental cysts (Table 7.1). Odontogenic cysts may become symptomatic but may also be detected as an incidental finding on a radiograph. Malignant changes in the epithelium of odontogenic cysts are exceedingly rare. Odontogenic cysts are treated by enucleation or, occasionally, by marsupialization (see for explanation Chap. 2).
Table 7.1
Classification of odontogenic cysts
|
1 Developmental cysts
|
|
1.1 Dental lamina cyst (gingival cyst) in the newborn
|
|
1.2 Gingival cyst in the adult
|
|
1.3 Primordial cyst
|
|
1.4 Eruption cyst
|
|
1.5 Follicular (dentigerous) cyst
|
|
1.6 Lateral periodontal cyst
|
|
1.7 Keratinizing odontogenic cyst
|
|
1.8 Sialo-odontogenic cyst (“glandular odontogenic cyst”)
|
|
2 Inflammatory cysts
|
|
2.1 Radicular cyst
|
|
2.2 Residual (radicular) cyst
|
|
2.3 Paradental cyst (including the mandibular buccal infected cyst)
|
7.3.1 Odontogenic Cysts
7.3.1.1 Developmental Odontogenic Cysts
The dental lamina cyst of the newborn, the gingival cyst in adults, and the eruption cyst are located in the soft tissues and are discussed in Chap. 5.
Primordial Cyst
Definition
Cystic change in a developing tooth germ before formation of dentin or enamel matrix. Can, theoretically, also arise in a supernumerary tooth germ. It is a somewhat debatable entity, by many considered to always be based histopathologically on a keratocystic odontogenic tumor.
Epidemiology
Extremely rare odontogenic cyst.
Clinical Aspects
Incidental finding on a radiograph. Rarely, if ever, causes symptoms.
Radiographic Aspects
Well-defined radiolucency in an area of a missing tooth (and a negative history of a previous tooth extraction) (Fig. 7.7).
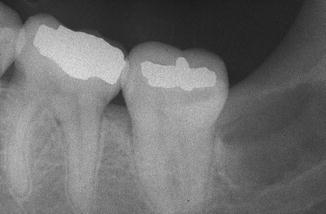

Fig. 7.7
Radiographic aspect distally of 37 compatible with a primordial cyst; no history of removal of 38
Histopathology
Often, according to some authors, always lined by epithelium that shows the characteristic features of a keratocystic odontogenic tumor.
Treatment
Enucleation.
Follicular (Dentigerous) Cyst
Definition
Cyst development in a follicle of an unerupted tooth.
Epidemiology
Quite common odontogenic cyst that almost exclusively occurs in the permanent dentition.
Clinical Aspects
Incidental finding on a radiograph, mainly related to mandibular and maxillary wisdom teeth and upper canines.
Radiographic Aspects
Well-defined radiolucency around the crown of an impacted tooth (Fig. 7.8). The differential diagnosis includes, among others, a keratocystic odontogenic tumor and an ameloblastoma. When the radiolucency surrounding the crown measures more than 2–3 mm, somewhat arbitrarily chosen, the term follicular cyst is used instead of “enlarged” tooth follicle.
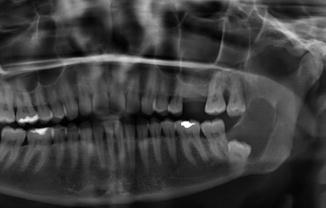

Fig. 7.8
Radiographic aspect compatible with the diagnosis of follicular cyst of 38
Histopathology
The lining of a follicular cyst consists of two or more layers of squamous epithelium without characteristic features (Fig. 7.9). Occasional “goblet cells” may be observed (Fig. 7.10).
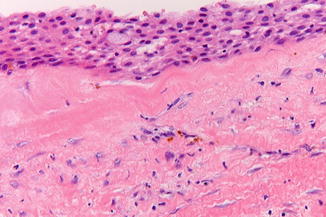
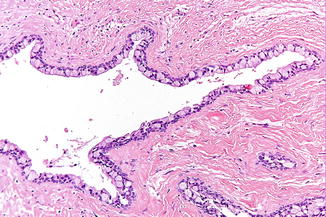

Fig. 7.9
Histopathologic aspect compatible with but not diagnostic of a follicular cyst

Fig. 7.10
Goblet cells in the lining of a follicular cyst
Histopathologically, no distinction can be made between the lining of a follicular cyst and the lining of an (enlarged) tooth follicle. In tooth follicles embryonal rests of odontogenic epithelium may be encountered, sometimes mimicking ameloblastomatous cells. Furthermore, myxoid changes in the stroma can be observed, mimicking to some extent the features of an odontogenic myxoma.
Treatment
Enucleation and removal of the associated tooth. Recurrences are extremely rare.
Lateral Periodontal Cyst (Incl. Botryoid Odontogenic Cyst)
Definition
In the past, a lateral periodontal cyst has been defined clinicoradiographically as a cyst located between the roots of two vital teeth. At present, the definition has been extended by certain histopathological characteristics. A botryoid odontogenic cyst shows the same histopathological characteristics as a lateral periodontal cyst but extends over an area of several teeth.
Clinical Aspects
The lateral periodontal cyst is almost exclusively found in the premolar area of the mandible, usually being an accidental finding on a radiograph.
Radiographic Aspects
Well-defined radiolucency between the roots of two vital teeth (Fig. 7.11a). In case of a lobular radiolucency, extending over an area of several teeth, the term “botryoid odontogenic cyst” is applied. The differential diagnosis includes, among others:
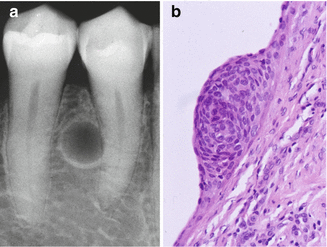

Fig. 7.11
(a) The radiographic aspect is compatible with a diagnosis of a lateral periodontal cyst. (b) Epithelial “plaque”, more or less diagnostic of the diagnosis lateral periodontal cyst
-
Ameloblastoma
-
Keratocystic odontogenic tumor
-
Central giant cell lesion
-
Ossifying fibroma
-
Langerhans cell histiocytosis
-
Simple bone cyst
Histopathology
The histopathology shows an epithelial lining of just a few cell layers thick with characteristic epithelial plaques (Fig. 7.11b). In fact, a more or less similar lining is seen in the gingival cyst of the adult. The latter cyst is by many authors regarded as the extraosseous counterpart of the intraosseous lateral periodontal cyst.
Treatment
Enucleation; especially the botryoid odontogenic cyst has a tendency to recur.
Keratinizing Odontogenic Cyst
Definition
The keratinizing odontogenic cyst (KOC) is a developmental odontogenic cyst, presenting clinicoradiographically as a follicular cyst (Fig. 7.12). The diagnosis is based on histopathologic features only. These features consist of an epithelial cyst lining showing hyperkeratosis without the characteristic epithelial architecture of a keratocystic odontogenic tumor (KCOT) (Fig. 7.13). In the past this cyst was for many years regarded as the orthokeratotic variant of a KCOT, that, in contrast to the parakeratotic variant of a KCOT, rarely recurred after removal.
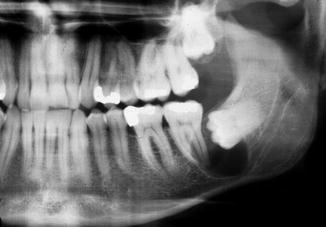
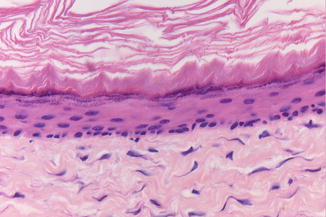

Fig. 7.12
Non-characteristic radiograph of a keratinizing odontogenic cyst

Fig. 7.13
Keratinizing odontogenic cyst somewhat mimicking a keratocystic odontogenic tumor
Radiographic Aspects
There are no specific radiographic features.
Treatment
The diagnosis KOC is always a postsurgical, histopathologic diagnosis. There is no tendency for recurrences and follow-up is not indicated.
Sialo-odontogenic Cyst
Definition
Rare developmental cyst with tubular-like structures in the epithelial lining which resemble salivary gland tissue.
Epidemiology
Usually in middle-aged persons.
Clinical Aspects
Usually located in the anterior part of the lower jaw.
Radiographic Aspects
Unilobular or multilobular radiolucency, indistinguishable from a keratocystic odontogenic tumor or ameloblastoma (Fig. 7.14).
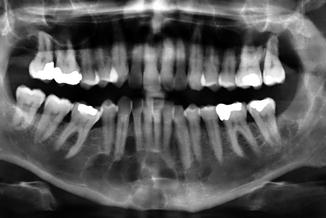

Fig. 7.14
Non-characteristic radiograph of a sialo-odontogenic cyst in the 43–44 region
Histopathology
Apart from squamous epithelium also tubular structures and mucous producing cells are encountered (Fig. 7.15); can somewhat resemble mucoepidermoid carcinoma.
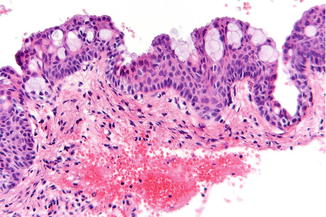

Fig. 7.15
Low-power view of the epithelial lining of the wall of a sialo-odontogenic cyst
Treatment
Enucleation; recurrences have been reported.
7.3.1.2 Inflammatory Odontogenic Cysts
Radicular Cyst
Definition
Cyst around the apex of a root of a non-vital tooth.
Clinical Aspects
Rarely occurs in the temporary dentition. Occasionally causes a swelling or an abscess.
Radiographic Aspects
Well-defined radiolucency around the apex of a root (Fig. 7.16a). Occasionally root resorption may be observed. Cannot be distinguished radiologically from a periapical granuloma, although the presence of a surrounding cortical line and large size are indicative of a radicular cyst. The radiographic aspect of a nasopalatine duct cyst may somewhat mimic a radicular cyst (Fig. 7.16b). However, in a nasopalatine duct cyst, the vitality of the teeth remains intact.
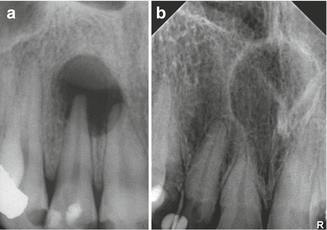

Fig. 7.16
(a) Radiolucency at the apex of the non-vital 12. (b) A nasopalatine duct cyst may somewhat resemble a radicular cyst of an upper central incisor
Histopathology
Non-characteristic lining with stratified squamous epithelium (Fig. 7.17).
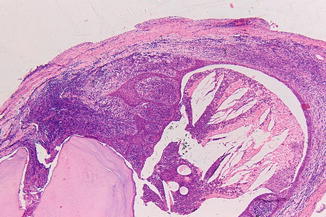

Fig. 7.17
Radicular cyst at the apex of a non-vital tooth
Treatment
Endodontic treatment, sometimes in combination with apicoectomy. If necessary extraction of the tooth and enucleation of the cyst may be considered.
Residual (Radicular) Cyst
Definition
(Radicular) cyst left behind after a tooth extraction.
Clinical Aspects
A residual may give rise to a swelling of the bone.
Radiographic Aspects
Well-defined radiolucent lesion in an edentulous part of lower or upper jaw (Fig. 7.18a, b). The differential diagnosis includes, a.o., ameloblastoma, keratocystic odontogenic tumor, and other non-odontogenic tumors. In an edentulous part of the dorsal part of the maxilla, it might be difficult to distinguish a residual cyst from an extension of the maxillary sinus (Fig. 7.19).
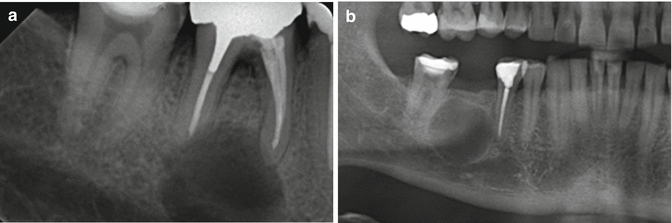
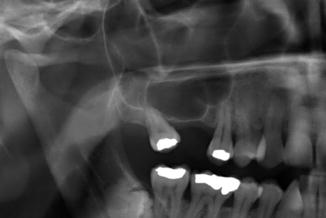

Fig. 7.18
(a) The radiographic aspect is suggestive of a radicular cyst. (b) After extraction of 46 two years ago, the cyst has apparently persisted (residual cyst)

Fig. 7.19
Expansion of the maxillary sinus may mimic a residual cyst
Histopathology
Non-characteristic lining with squamous epithelium (Fig. 7.20). Occasional presence of calcifications in the lining epithelial cells, called “Rushton bodies” (Fig. 7.21). Rushton bodies may be misinterpreted as part of a cystic calcifying odontogenic tumor, a rare odontogenic tumor that will not be discussed here any further.
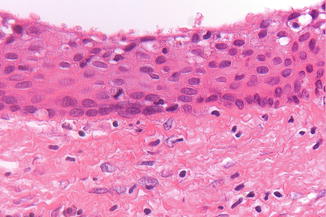
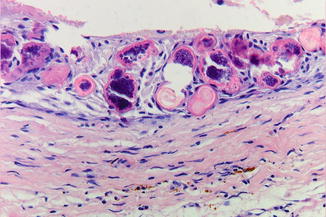

Fig. 7.20
Non-characteristic squamous epithelium lining of a residual cyst

Fig. 7.21
Rushton bodies in the lining of a residual cyst
Treatment
Enucleation or, if indicated, marsupialization (Fig. 7.22a–d).
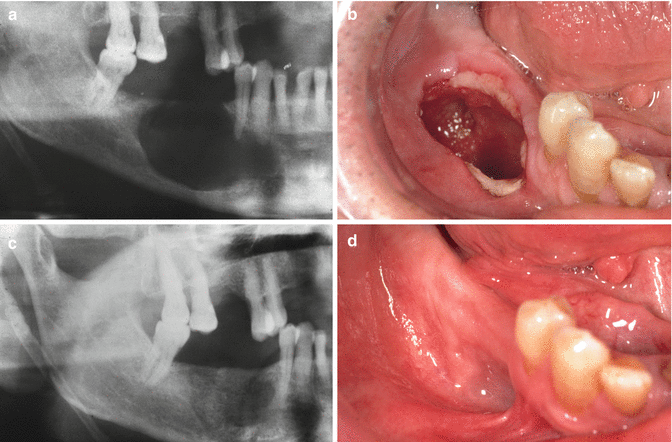

Fig. 7.22
(a) Radiographic aspect compatible with a diagnosis of a residual cyst. (b) Clinical aspect immediately after marsupialization. (c) Radiographic aspect one year postoperatively. (d) Clinical aspect one year postoperatively
Paradental Cyst (Incl. Mandibular Buccal Infected Cyst)
Definition
Cyst formation in a persisting follicle of an erupted tooth; the mandibular buccal infected cyst is a rare subtype.
Clinical Aspects
Usually incidental finding on a radiograph. Occasionally pocket formation and mild symptoms of gingival discharge of fluid.
Radiographic Aspects
The paradental cyst presents as a circumscribed radiolucency, distally of an erupted tooth, often a lower wisdom tooth. The mandibular buccal infected cyst may be accompanied by a periapical radiolucency around a vital tooth (Fig. 7.23).
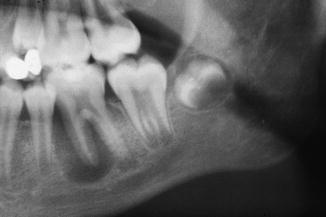

Fig. 7.23
Paradental cyst (“mandibular buccal infected cyst”) of a vital 36 in a young patient
Histopathology
Non-characteristic epithelial lining of the cyst wall.
Treatment
Enucleation (Fig. 7.24a–d). In some cases the tooth is lost due to periodontal problems.
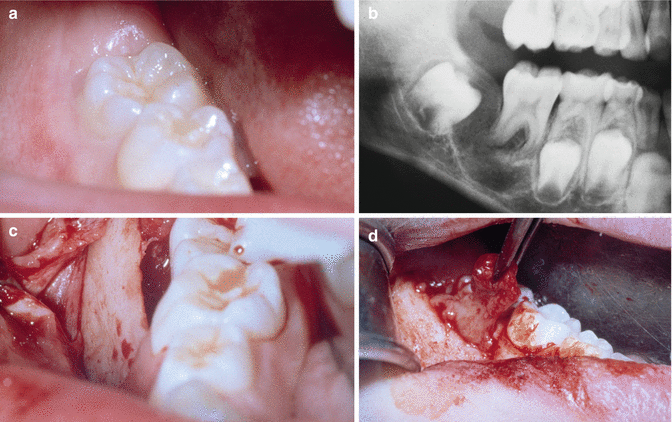

Fig. 7.24
(a) Mild periodontal complaints of vital 46; buccal pocket at probing. (b) Radiolucency around 46, compatible with a diagnosis of mandibular buccal infected cyst. (c) After reflecting a mucoperiosteal flap, a gap is observed between the alveolar bone and 46. (d) Removal of the cyst at the buccal aspect of 46
7.3.2 Odontogenic Tumors
Introduction
Odontogenic tumors are made up of one or more dental tissues, such as enamel, dentin, and cementum. Some of these tumors are to be regarded as developmental disorders; others do have neoplastic properties. The 2005 classification by the World Health Organization distinguishes benign and some extremely rare malignant tumors. Here we will limit our discussion to the most common benign odontogenic tumors, being:
-
Ameloblastoma and ameloblastoma-like tumors
-
Cementoblastoma
-
Keratocystic odontogenic tumor
-
Myxoma
-
Odontoma
7.3.2.1 Ameloblastoma
Definition
Nearly always histologically benign tumor consisting of ameloblast-like epithelial cells.
Is characterized by a high rate of recurrence. An ameloblastoma with histopathological malignant characteristics such as cellular or nuclear polymorphism, mitotic activity, and invasive growth is extremely rare. A histologically benign ameloblastoma may in rare instances metastasize to the cervical lymph nodes or to sites elsewhere in the body, being referred to as metastasizing ameloblastoma.
Etiology
There are no known etiologic factors.
Epidemiology
The estimated incidence is one per million population per year. Sometimes diagnosed at a young age. The average age at the time of diagnosis is around 30 years.
Clinical Aspects
The tumor nearly always develops in the jaw bone (intraosseous ameloblastoma), probably from residual epithelium of the dental lamina. Occasionally the tumor arises from odontogenic epithelium of the alveolar mucosa (peripheral ameloblastoma).
An ameloblastoma is often diagnosed after histopathological evaluation of a lesion that clinicoradiographically looked like a cyst. Sometimes an ameloblastoma presents as an intraoral or extraoral swelling (Fig. 7.25a, b). Occasionally causes disturbed tooth eruption.
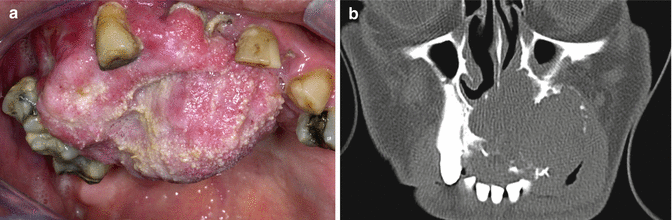

Fig. 7.25
(a) Example of a neglected ameloblastoma in the anterior part of the mandible. (b) A CT scan shows the extent of the tumor
Radiographic Aspects
Unilobular or multilobular radiolucency, sometimes surrounded by a cortical line. May cause resorption of teeth (Fig. 7.26). Often expansion of the jaw bone. May mimic, a.o., a residual cyst, a follicular cyst, or a keratocystic odontogenic tumor (Fig. 7.27). Particularly in the upper jaw but also in the mandible, additional CT scans are required in order to get better information about the extent of the lesion and the integrity of the cortical plates of the jaw bones.
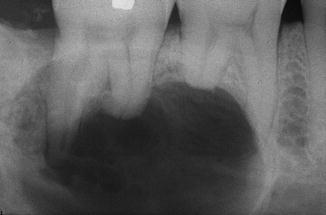
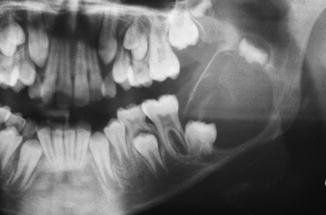

Fig. 7.26
Resorption of the roots of 46 and 47 caused by an ameloblastoma

Fig. 7.27
Non-diagnostic radiograph of a radiolucency caused by an ameloblastoma
Histopathology
Almost all ameloblastomas are histopathologically benign. The diagnosis “malignant” ameloblastoma is justified only in case of cellular and nuclear polymorphism and/or mitotic activity. Most ameloblastomas are histopathologically easy to diagnose, especially in case of the common follicular type (Fig. 7.28). However, some histopathologic subtypes, such as the plexiform type and the granular cell type, may be difficult to recognize as such (Fig. 7.29). Furthermore, it may be difficult to distinguish an acanthomatous ameloblastoma from a squamous odontogenic tumor, another extremely rare but less aggressive odontogenic tumor.
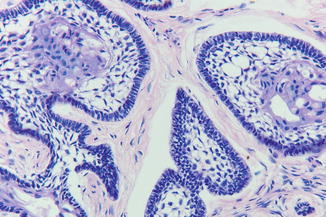
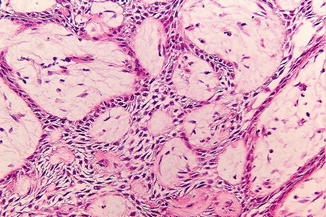

Fig. 7.28
Histopathologic aspect of ameloblastoma, follicular type

Fig. 7.29
Ameloblastoma, plexiform type. This subtype can be misinterpreted as epithelial proliferation
The unicystic ameloblastoma is a rare variant, being characterized macroscopically as a cystic lesion and microscopically by a lining with ameloblastomatous epithelial cells (Fig. 7.30). The diagnosis “unicystic ameloblastoma” cannot be made on the basis of radiographic aspects.
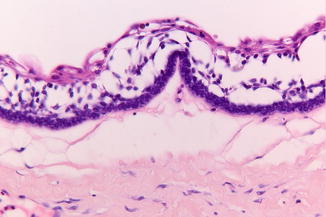

Fig. 7.30
Low-power view of an ameloblastomatous lining in a unicystic ameloblastoma
The histopathological differential diagnosis of an ameloblastoma may include a number of other odontogenic, somewhat ameloblastoma-like tumors, such as the already mentioned squamous odontogenic tumor, the ameloblastic fibroma (Fig. 7.31), the ameloblastic fibrodentinoma, and the ameloblastic fibro-odontoma, having generally a less aggressive behavior than an ameloblastoma.
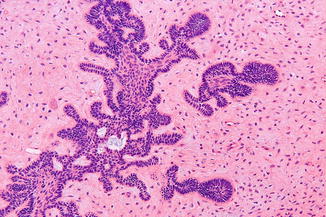

Fig. 7.31
Ameloblastic fibroma; the stroma resembles pulpal tissue
Note: in follicular tissue of impacted teeth, epithelial proliferations may occur that might be misdiagnosed histopathologically as part of an ameloblastoma (Fig. 7.32).
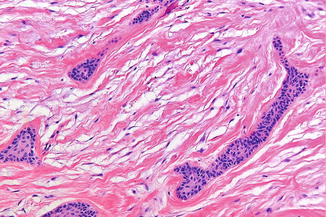

Fig. 7.32
Epithelial nests in a tooth follicle resembling ameloblastomatous proliferations
Treatment
Preferably wide surgical excision with a margin of surrounding clinically normal bone, if necessary sacrificing the continuity of the mandible. In children a more conservative approach is perhaps justified; this possibly also applies to ameloblastomas that are located in the anterior part of the mandible or maxilla. Especially when located in the dorsal part of the mandible and the maxilla, radical removal has to be pursued, since a recurrence in that location will be difficult to treat successfully. Most recurrences after enucleation do so within a few years. Therefore, strict annual follow-up is indicated for, e.g., 10 years.
7.3.2.2 Cementoblastoma
Definition
A benign tumor consisting of cementum.
Epidemiology
Rare tumor; the estimated incidence is less than one per million population per year. Is usually diagnosed before the age of 25 years.
Clinical Aspects
Usually relates to the mandibular molars. Fast-growing swelling, painful.
Radiographic Aspects
Well-circumscribed opacity attached to the root of a tooth (Fig. 7.33).
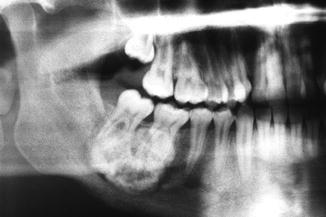

Fig. 7.33
Radiographic aspect of cementoblastoma of 46 in a 22-year-old man
Histopathology
Cementum and cementum-like tissue attached to the root of a tooth (Fig. 7.34a, b).
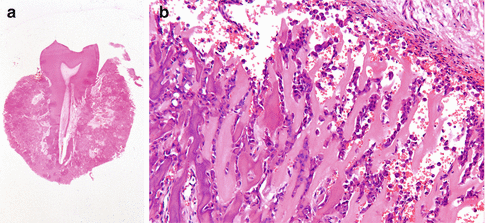

Fig. 7.34
(a) Gross specimen of a cementoblastoma attached to the roots. (b) Histopathologic aspect of cementoblastoma; viewed “in isolation” the differential diagnosis includes an osteosarcoma
Treatment
Extraction or surgical removal of the tooth together with the attached cementoblastoma. Recurrences are not uncommon.
7.3.2.3 Keratocystic Odontogenic Tumor (“Keratocyst”)
Definition
The diagnosis keratocystic odontogenic tumor (KCOT) is based exclusively on histopathologic criteria. In the past, the lesion was classified as an odontogenic cyst. Worldwide there is a debate among (oral) pathologists about the correctness of “upgrading” the odontogenic keratocyst to a keratocystic odontogenic tumor.
Clinical Aspects
Intraoral or extraoral swelling; sometimes an incidental finding on a radiograph.
Radiographic Aspects
Unilobular or multilobular well-defined radiolucency (Fig. 7.35); sometimes expansion of the bone (Fig. 7.36). A KCOT rarely causes tooth resorption. The radiographic aspect is not pathognomonic and may resemble, a.o., a residual cyst, an ameloblastoma, a central giant cell lesion, and other odontogenic and non-odontogenic lesions.
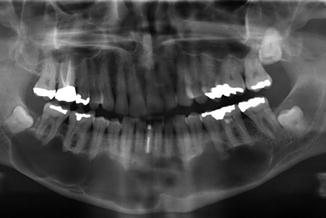
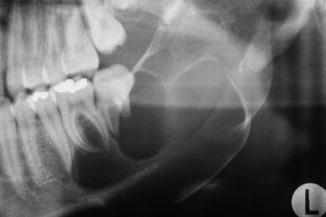

Fig. 7.35
Multilobular radiolucency extending bilaterally in the mandible; keratocystic odontogenic tumor

Fig. 7.36
Multilobular radiolucency; keratocystic odontogenic tumor
Multiple KCOTs, not necessarily present simultaneously, are indicative of the hereditary basal cell nevus syndrome (Gorlin syndrome); the other aspects of this syndrome are, a.o., the presence of one or more bifid ribs, pits in the skin of the hand palms, calcifications of the falx cerebri, and, most important, multiple basal cell carcinomas of the skin, often located in the head and neck area and occurring already at an early age (Figs. 7.37, 7.38, and 7.39).
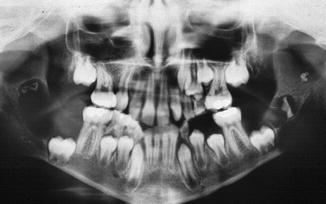
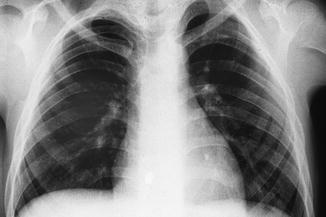
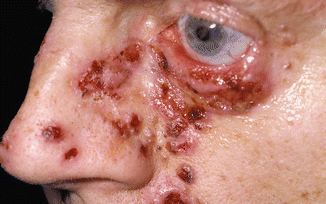

Fig. 7.37
Keratocystic odontogenic tumor bilateral in the mandible in a patient suffering from the basal cell nevus syndrome

Fig. 7.38
The chest X-ray shows two bifid ribs on the left side

Fig. 7.39
Multiple basal cell carcinomas immediately after treatment in a patient with basal cell nevus syndrome
Histopathology
KCOT has characteristic histopathologic aspects consisting among others of an epithelial lining of 6–8 cell layers thick, palisade arrangement of the basal cells, corrugated surface of the epithelium, and a parakeratotic, often corrugated surface (Fig. 7.40a, b). The characteristic features may partly disappear when the cyst becomes secondary inflamed. In case of distinct hyperkeratosis, one is most likely dealing with a keratinizing odontogenic cyst (see before).
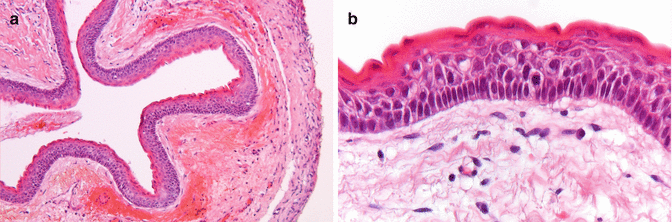

Fig. 7.40
(a) Rather typical folding of the wall of a keratocystic odontogenic tumor (KCOT). (b) Characteristic epithelial lining of a KCOT; notice the palisade arrangement of the basal cell layer
Treatment
Enucleation and, if possible, removal of the overlying mucosa. In some cases marsupialization or decompression is to be preferred, usually requiring enucleation at a later stage. Some clinicians use the “fixation before and/or after enucleation technique,” applying Carnoy’s fixative solution before and/or after enucleation.
The recurrence rate of KCOTs depends on the extent of the surgical removal and may be up to 25 % or more during a follow-up period of five years after just enucleation. Because of the risk of recurrence, annual follow-up is advised for at least five years. Although the recurrence rate after enucleation is lower than in ameloblastomas, one may consider to perform radical surgery for KCOTs located in the posterior part of the jaws, particularly when located in the ascending ramus of the mandible since recurrences at that side may be difficult to treat successfully.
In case of suspicion of the basal cell nevus syndrome, referral to a department of clinical genetics is indicated.
7.3.2.4 Odontogenic Myxoma
Definition
Odontogenic tumor of mesenchymal tissue of the tooth bud.
Epidemiology
The estimated incidence is less than one per million population per year. The tumor is usually diagnosed at the age of 20–30 years.
Clinical Aspects
The odontogenic myxoma almost exclusively occurs within the bone of the upper or the lower jaw. Sometimes, the tumor gives rise to an intraoral or extraoral swelling, usually being asymptomatic otherwise.
Radiographic Aspects
Unilobular or multilobular radiolucency with sometimes a “honeycomb” aspect (Fig. 7.41); sometimes associated with an impacted tooth. The radiographic differential diagnosis includes, among others, ameloblastoma, keratocystic odontogenic tumor, central giant cell lesion, and a central arteriovenous malformation.
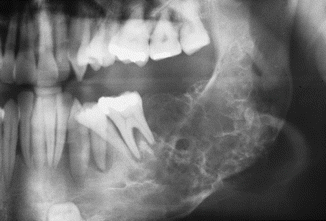

Fig. 7.41
Honeycomb radiolucency compatible with a diagnosis of odontogenic myxoma
Histopathology
Circumscribed loose, fibromyxoid tissue containing stellate or sometimes rounded cells (Fig. 7.42). Cellular and nuclear polymorphism or mitotic activity is rarely observed. Sometimes the presence of nests of odontogenic epithelium, but this is not a requirement for the diagnosis of odontogenic myxoma.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses