Introduction
Our objective was to investigate the effectiveness of debonding ceramic brackets with a diode laser.
Methods
Two types of ceramic brackets (monocrystalline and polycrystalline) were bonded to bovine maxillary central incisors. The diode laser was applied to brackets in the experimental groups for 3 seconds. Shear bond strength and thermal effects on the pulp chamber were assessed at 2 laser energy levels: 2 and 5 W per square centimeter. Analysis of variance (ANOVA) was used to determine significant differences in shear bond strength values.
Results
The diode laser was ineffective with polycrystalline brackets and effective with monocrystalline brackets in significantly ( P <0.05) lowering the shear bond strength. There were no significant adhesive remnant index score differences between any groups tested.
Conclusions
Diode laser use significantly decreased the debonding force required for monocrystalline brackets without increasing the pulp chamber temperature significantly. Diode lasers did not significantly decrease the debonding force required for polycrystalline brackets.
Ceramic brackets have been the preferred choice for esthetically conscious clinicians and patients since their introduction in the 1980s. Their popularity continues, as evidenced by the recent wave of ceramic self-ligating bracket systems introduced to the specialty. Discussion of the clinical challenges of ceramic bracket use remains an active topic of debate. A major concern is bracket debonding. The increased bond strength in attachment of ceramic brackets to enamel might increase the potential for enamel damage or bracket fractures at debonding.
Various methods have been developed to aid in debonding ceramic brackets. These methods use special pliers for mechanical debonding, degrading the bonding resin with electro-thermal debonding devices, and lasers. There are 4 major types of lasers. They are classified mostly by their lasing mediums, defined by their state: gas, liquid, solid, and semiconductor (or laser diode).
A laser diode, also known as an injection laser or a diode laser, is a semiconductor device that produces coherent radiation (in which the waves are all at the same frequency and phase) in the visible or infrared spectrum when current passes through it. Laser diodes are used in optical fiber systems, compact disk players, laser printers, and remote-control devices. Laser diodes differ from other laser types in several important ways: small size and low weight, current, voltage, intensity, and power requirements.
Previous studies have shown that use of carbon dioxide, neodymium: yttrium-aluminum garnet, or xenon chlorine excimer lasers can be effective in significantly lowering the shear bond strength (SBS) of ceramic brackets. The purpose of this study was to investigate the effect of diode laser use in debonding 2 types of ceramic brackets.
Material and methods
Two maxillary left central incisor ceramic brackets were used in this study: Inspire ICE (Ormco, Orange, Calif), a monocrystalline bracket; and Clarity (3M Unitek, Monrovia, Calif), a polycrystalline bracket. A single-paste visible light-cured orthodontic adhesive system, Transbond XT (3M Unitek), was used.
Sixty bovine incisors were obtained from a slaughterhouse. The teeth were stored in distilled water in a freezer at –20°C until used. When needed, the teeth were thawed in warm water and embedded in auto-polymerizing polymethyl methacrylate in molds (25 × 25 × 25 mm) so that the crown was exposed. After polymerization of the polymethyl methacrylate, the teeth were stored for 24 hours in distilled water to which crystals of thymol were added to inhibit bacterial growth. Before bonding, access cavities, 2 mm in diameter, were drilled into the pulp chamber by using a high-speed hand piece into the center of the cingulum on the lingual surfaces.
The middle third of the labial surface was flattened with sandpaper. The flattened enamel surface was dried with hot air, and Transbond Plus Self Etching Primer (3M Unitek) was prepared for application to the tooth surface according to the manufacturer’s instructions. A saturated applicator tip was rubbed on the tooth surface for 4 seconds followed by a gentle air burst. Transbond XT was then placed on the bracket base, and the bracket was placed on the prepared enamel surface so that the slot was parallel to the incisal edge of the incisor.
The guide pin of a nonadjustable Hanau articulator (Teledyne Water Pik, Fort Collins, Colo), with a stone cylinder of 600 g attached to its upper member, was positioned to engage the bracket slot. This ensured that the brackets were seated under constant pressure and allowed the investigator to remove, with a sharp dental explorer, any surplus cement extruded from the periphery of the base without compromising the onset of the polymerization process. The cement was then cured with a 75-W halogen curing light (3M ESPE, St Paul, Minn) for 40 seconds (10 seconds on each side of the bracket). The teeth were then stored for 24 hours in distilled water with thymol in an incubator at 37°C.
The embedded teeth and ceramic bracket were positioned in a universal testing machine (Instron, Canton, Mass) so that the bracket slot was parallel to the horizontal. The brackets were lased at this time according to the protocol of the group in which they were categorized ( Table I ). The laser was applied directly to the center of the Inspire ICE brackets and just superior to the stainless steel slot of the Clarity brackets. A type K thermocouple (Extech Instruments, Waltham, Mass) was placed in the pulp chamber, and temperatures were recorded before and after lasing.
| Group | Bracket type | Debonding method |
|---|---|---|
| 1 | Clarity | Force only |
| 2 | Inspire ICE | Force only |
| 3 | Clarity | Diode laser 2 W/cm 2 /3sec and force |
| 4 | Inspire ICE | Diode laser 2 W/cm 2 /3 sec and force |
| 5 | Clarity | Diode laser 5 W/cm 2 /3 sec and force |
| 6 | Inspire ICE | Diode laser 5 W/cm 2 /3 sec and force |
Immediately after lasing, a sharp chisel blade was placed at the bracket base-enamel interface, and, with a load cell of 1 kN and a crosshead speed of 0.5 mm per minute, the bracket was shear tested to failure. The force producing failure was recorded in newtons and converted to force per unit area (megapascals) by dividing the measured force values by the mean surface area of the brackets. Immediately after debonding, the bracket and tooth were examined with a light microscope under 10 times magnification to determine the adhesive remnant index (ARI) score : 0, all adhesive was removed with the bracket; 1, adhesive remnants covered less than 50% of the former bracket site; 2, adhesive remnants covered more than 50% of former bracket site; and 3, adhesive remained on tooth surface with a clear imprint of the bracket base.
Statisical analysis
Statistical analysis of the data was then carried out, including calculating the mean SBS values, ARI scores, and standard deviations for each group. A 1-way analysis of variance (ANOVA) established whether there were any differences in the mean SBS values for each bracket type. If there were differences, the Tukey honestly significant difference test was done to establish which groups differed significantly. A chi-square test was calculated to analyze the mean ARI score for each bracket group. Signed rank tests were used to compare each bracket group’s temperature change against standard increases of 1.8°C and 5.5°C.
Results
The mean SBS values and standard deviations are given in Table II . The data were then used to compare the means of the groups for each bracket type.
| Clarity | Inspire Ice | |||||
|---|---|---|---|---|---|---|
| Group 1 | Group 3 | Group 5 | Group 2 | Group 4 | Group 6 | |
| n | 10 | 10 | 10 | 10 | 10 | 10 |
| Mean | 9.79 | 9.68 | 7.24 | 15.99 | 9.27 | 8.88 |
| SD | 3.20 | 2.63 | 3.60 | 4.91 | 3.67 | 3.04 |
No statistically significant differences ( P <0.05) were found when comparing the mean SBS values of the 3 groups of Clarity brackets. There was a statistically significant difference in the mean SBS values of the 3 groups of Inspire ICE brackets. The means of the 2 lased groups were statistically significantly lower ( P <0.05) than those of the nonlased group. However, the difference in the means of the lased groups was not statistically significant ( P <0.05; Fig 1 ).
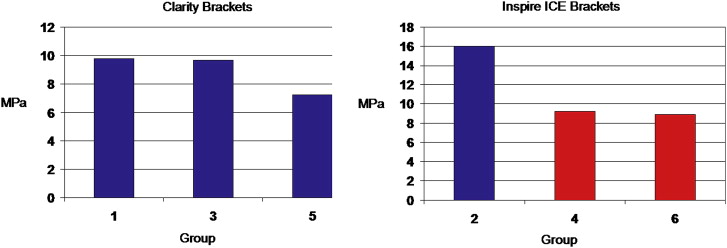
There were no significant differences in the ARI scores of 3 groups when either the Clarity (chi-square, P = 0.37) or the Inspire ICE (chi-square, P = 0.79) brackets were tested. All groups in the study had mean ARI scores of 3; this indicates that almost all adhesive was left behind on the tooth surfaces with a clear imprint of bracket base.
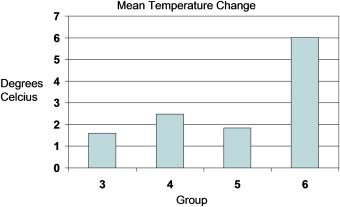
The mean increases in pulp chamber temperature for groups 3, 4, and 5 were statistically significantly less ( P <0.01) than the 5.5°C increase threshold and not significantly different ( P <0.01) from the 1.8°C standard. Group 6 had a mean pulp chamber increase significantly greater than the 1.8°C standard and not significantly different ( P <0.01) from the 5.5°C standard ( Fig 2 ).

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


