Diagnostic imaging of facial structures has advanced significantly in the past several decades. Although conventional radiography still has some utility, the majority of craniofacial diagnostic imaging is now done with computed tomography (CT) and magnetic resonance imaging (MRI). In the setting of trauma, CT is the most useful because of the rapid acquisition times, excellent bone detail, and ability to examine anatomy in multiple planes.
This chapter discusses facial anatomy pertinent to the evaluation of trauma patients, reviews the various imaging techniques useful in facial trauma, and discusses the imaging findings in common facial injuries.
ANATOMY
BUTTRESSES
One of the major functions of the midfacial skeleton is the transmission of masticatory forces to the cranium. This is accomplished through a series of vertical and horizontal buttresses. These buttresses form the basic vertical and horizontal framework for the facial skeleton. They give structural integrity to important facial structures, such as the orbits and paranasal sinuses. Thus, they directly or indirectly anchor to the skull base or cranium. Slight variations of the facial buttress systems exist. The described system is based primarily on that described by Manson et al. ( Figure 8-1 ).
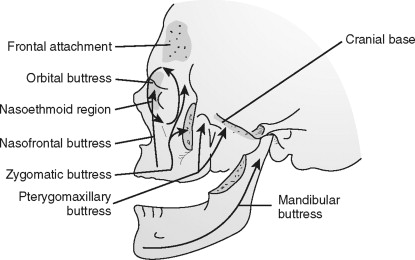
Transverse Buttresses
Three major buttresses of the face and two buttresses of the mandible give lateral stability to their respective surrounding structures. The superior transverse facial buttress is composed of the orbital plate of the frontal bone and the cribriform plate of the ethmoid. The middle transverse buttress consists of the zygomatic process of the temporal bone, the body and temporal process of the zygoma, the infraorbital process of the zygoma, the orbital surface of the maxilla, and segments of the frontal process of the maxilla. The inferior facial buttress consists of the superior alveolar ridge and hard palate. The superior mandibular transverse buttress runs along the inferior alveolar ridge. The inferior mandibular transverse buttress runs along the inferior edge of the mandible from one angle to the other.
Vertical Buttresses
Three paired peripheral buttresses and one central buttress exist. The nasofrontal buttresses comprise the frontal process of the maxilla, the nasal bones, the nasofrontal suture (nasion), and the medial walls of the maxillary sinuses and orbits. The zygomatic buttresses extend from the posterior maxillary molars vertically through the zygomaticomaxillary (ZMC) sutures, zygomatic bodies, and through the lateral orbital walls into the frontal bones. The pterygomaxillary buttresses consist of the pterygoid processes of the sphenoid bone and the posterolateral and posteromedial walls of the adjacent maxillary sinus. The central nasoethmoidal buttress is composed of the ethmoid and vomer bones.
IMAGING TECHNIQUES
RADIOGRAPHY
Before the introduction of CT, plain radiographic studies were the only imaging studies available for assessing complex osseous maxillofacial injuries. Although CT has supplanted plain radiographic imaging for the evaluation of complex facial fractures and soft tissue injuries, these studies are appropriate for the evaluation of uncomplicated injuries.
The facial bone series used in the evaluation for trauma typically consists of three to five projections. The three essential views are the lateral, Waters’, and Caldwell’s views. Lateral views can be used to evaluate the airway, retropharyngeal soft tissues, anterior and posterior maxillary antral walls, and alveolar ridge. The Waters’ view is useful to evaluate the zygomatic arches and anterior facial structures. Caldwell’s view provides the best demonstration of the orbits and posterior facial structures.
Additional submentovertical (SMV) and Towne’s views can also be obtained. These views can help delineate fractures not seen on the other views.
Basic Principles
Radiography shows four basic densities: air, bone, soft tissue, and fat. Identifying abnormalities in these overlapping densities requires a systematic approach. A general approach can be remembered by the four S’s: symmetry, sharpness, sinus, and soft tissue. Fortunately, the face is generally a symmetric structure, greatly simplifying identification of abnormal densities.
The normally sharp edge along a cortical margin of bone can be disturbed by fracture, hematoma, or even fat density (as in an orbital floor fracture with fat herniating into the maxillary sinus).
Air within sinuses typically results in a darker (less dense) structure than the orbits. Unfortunately, this “soft tissue” density within the sinuses can be due to sinusitis, hemorrhage, or even soft tissue tumors.
Soft tissues should be reviewed for air, foreign bodies, and loss of normal fat density.
COMPUTED TOMOGRAPHY
Multi-Detector CT
A basic understanding of the technical capabilities of CT is useful for this chapter. Modern multi-detector CT (MDCT) scanners are capable of acquiring sub-millimeter slices in a matter of seconds. These thin axial images are then used to create highly detailed reformatted images that can be created in virtually any orientation, greatly simplifying the evaluation of facial trauma. Usually these reformatted images are in the standard coronal and sagittal planes.
At our institution, a maxillofacial CT consists of thin-cut (2-3-mm) axial images with coronal reformations. Some typical indications for this series include (1) ZMC fracture, (2) suspicion of blow-out/blow-in fracture, or (3) any significant facial trauma. Sagittal reformations are useful in mandibular fractures. Bone and soft-tissue reconstruction algorithms are used; the former maximizing bony detail (highest fracture sensitivity), whereas the latter allows better evaluation of soft tissues (retrobulbar hematomas, inferior rectus entrapment in blow-out fractures).
CT Angiography
Vascular injury to the neck is a potential life-threatening complication. Approximately 25% of cervical penetrating injuries result in vascular injury. In addition, a rare (0.18%) complication of multiple facial fractures is blunt internal carotid artery injury. Penetrating trauma injuries most commonly involve the carotid arteries (80%) followed by the vertebral arteries (43%), whereas the opposite is true with blunt injury. Figure 8-2 demonstrates a potential pitfall of penetrating trauma: metallic artifact can obscure adjacent injury. In cases with metallic fragments, conventional angiography may be necessary.
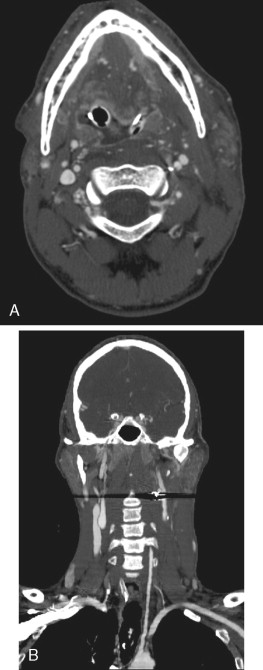
Traditionally, conventional angiography was used to evaluate stable patients with suspected cervical vascular injury. Multi-detector row CT now provides isotropic data acquisition, allowing multiplanar reformations with resolution comparable to the axial source images. This provides an excellent noninvasive evaluation of the major vascular structures of the head and neck. Recent studies have reported 100% sensitivity and 98% specificity in diagnosing vascular occlusion, pseudoaneurysm, fistulae, and partial thrombosis.
Patients may present with symptoms of stroke, palpable hematoma, or an enlarging arteriovenous fistula (bruit). Initially, many patients with such injuries are initially asymptomatic. Injuries to the vascular structures of the neck are listed in Table 8-1 .
| Vascular Injuries to the Neck | Findings on MDCT |
|---|---|
| Partial Occlusion | Vessel stenosis, marginal irregularities due to intramural hematoma, intravascular clot, and/or intimal flap (focal filling defect within the lumen that represents a partially injured vessel wall) |
| Complete Occlusion | |
| Dissection | |
| Pseudoaneurysm | Disruption of the vascular wall leading to hemorrhage within the adventitia or extravasating into the perivascular soft tissues |
| Arteriovenous Fistula | Partial transection of an adjacent artery and vein allows a fistula that becomes symptomatic (bruit) and enlarges over time |
IMAGING TECHNIQUES
RADIOGRAPHY
Before the introduction of CT, plain radiographic studies were the only imaging studies available for assessing complex osseous maxillofacial injuries. Although CT has supplanted plain radiographic imaging for the evaluation of complex facial fractures and soft tissue injuries, these studies are appropriate for the evaluation of uncomplicated injuries.
The facial bone series used in the evaluation for trauma typically consists of three to five projections. The three essential views are the lateral, Waters’, and Caldwell’s views. Lateral views can be used to evaluate the airway, retropharyngeal soft tissues, anterior and posterior maxillary antral walls, and alveolar ridge. The Waters’ view is useful to evaluate the zygomatic arches and anterior facial structures. Caldwell’s view provides the best demonstration of the orbits and posterior facial structures.
Additional submentovertical (SMV) and Towne’s views can also be obtained. These views can help delineate fractures not seen on the other views.
Basic Principles
Radiography shows four basic densities: air, bone, soft tissue, and fat. Identifying abnormalities in these overlapping densities requires a systematic approach. A general approach can be remembered by the four S’s: symmetry, sharpness, sinus, and soft tissue. Fortunately, the face is generally a symmetric structure, greatly simplifying identification of abnormal densities.
The normally sharp edge along a cortical margin of bone can be disturbed by fracture, hematoma, or even fat density (as in an orbital floor fracture with fat herniating into the maxillary sinus).
Air within sinuses typically results in a darker (less dense) structure than the orbits. Unfortunately, this “soft tissue” density within the sinuses can be due to sinusitis, hemorrhage, or even soft tissue tumors.
Soft tissues should be reviewed for air, foreign bodies, and loss of normal fat density.
COMPUTED TOMOGRAPHY
Multi-Detector CT
A basic understanding of the technical capabilities of CT is useful for this chapter. Modern multi-detector CT (MDCT) scanners are capable of acquiring sub-millimeter slices in a matter of seconds. These thin axial images are then used to create highly detailed reformatted images that can be created in virtually any orientation, greatly simplifying the evaluation of facial trauma. Usually these reformatted images are in the standard coronal and sagittal planes.
At our institution, a maxillofacial CT consists of thin-cut (2-3-mm) axial images with coronal reformations. Some typical indications for this series include (1) ZMC fracture, (2) suspicion of blow-out/blow-in fracture, or (3) any significant facial trauma. Sagittal reformations are useful in mandibular fractures. Bone and soft-tissue reconstruction algorithms are used; the former maximizing bony detail (highest fracture sensitivity), whereas the latter allows better evaluation of soft tissues (retrobulbar hematomas, inferior rectus entrapment in blow-out fractures).
CT Angiography
Vascular injury to the neck is a potential life-threatening complication. Approximately 25% of cervical penetrating injuries result in vascular injury. In addition, a rare (0.18%) complication of multiple facial fractures is blunt internal carotid artery injury. Penetrating trauma injuries most commonly involve the carotid arteries (80%) followed by the vertebral arteries (43%), whereas the opposite is true with blunt injury. Figure 8-2 demonstrates a potential pitfall of penetrating trauma: metallic artifact can obscure adjacent injury. In cases with metallic fragments, conventional angiography may be necessary.
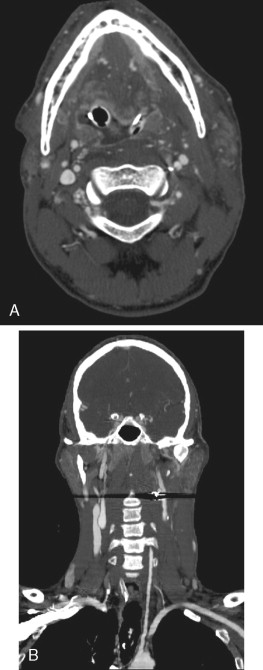
Traditionally, conventional angiography was used to evaluate stable patients with suspected cervical vascular injury. Multi-detector row CT now provides isotropic data acquisition, allowing multiplanar reformations with resolution comparable to the axial source images. This provides an excellent noninvasive evaluation of the major vascular structures of the head and neck. Recent studies have reported 100% sensitivity and 98% specificity in diagnosing vascular occlusion, pseudoaneurysm, fistulae, and partial thrombosis.
Patients may present with symptoms of stroke, palpable hematoma, or an enlarging arteriovenous fistula (bruit). Initially, many patients with such injuries are initially asymptomatic. Injuries to the vascular structures of the neck are listed in Table 8-1 .
| Vascular Injuries to the Neck | Findings on MDCT |
|---|---|
| Partial Occlusion | Vessel stenosis, marginal irregularities due to intramural hematoma, intravascular clot, and/or intimal flap (focal filling defect within the lumen that represents a partially injured vessel wall) |
| Complete Occlusion | |
| Dissection | |
| Pseudoaneurysm | Disruption of the vascular wall leading to hemorrhage within the adventitia or extravasating into the perivascular soft tissues |
| Arteriovenous Fistula | Partial transection of an adjacent artery and vein allows a fistula that becomes symptomatic (bruit) and enlarges over time |
RENDERING TECHNIQUES
3D IMAGING
Due to advances in software and computer processing, 3D imaging is widely available. There are two basic types of 3D imaging: shaded-surface display (SSD) and volume rendering (VR).
SSD uses a fixed threshold to determine which voxels will be displayed. The selected voxels are then displayed using established computer graphics algorithms for the rendering of solid objects, including control over lighting angle, shadow, and color. These images can be very realistic and provide excellent simulated images for surgical planning in facial trauma. However, since SSD relies on a fixed threshold, images are highly dependent on the threshold selection; some important features (particularly soft tissue) might be excluded from the image.
3D VR attempts to address this shortcoming by displaying tissue density in a range of transparency rather than using a single threshold. In addition, structures of varying densities can be artificially assigned different colors—better discriminating bone, soft tissue, and vasculature. Virtual fly-throughs within a lumen are possible, and some software allows real-time intra-operative guidance.
FACIAL FRACTURES
Efficient and accurate evaluation of the facial bones is a radiologic challenge. Familiarity with the pattern and typical location of such fractures greatly expedites their evaluation. Here we will discuss the typical patterns and locations for facial fractures.
Zygomaticomaxillary Fractures
This fracture, often referred to as ZMC or tripod fracture, is one of the most common facial fracture complexes. The zygoma is roughly triangular with three bony projections (hence the name “tripod”) and comprises the majority of the orbital floor and lateral orbital wall. It therefore plays a key role in maintaining orbital volume and serves as a reference for reduction of maxillary fractures.
The two major buttresses of the ZMC are the upper transverse maxillary (across the zygomaticomaxillary and zygomaticotemporal sutures) and the lateral vertical maxillary (across the zygomaticomaxillary and frontozygomatic sutures) ( Figure 8-3 ).
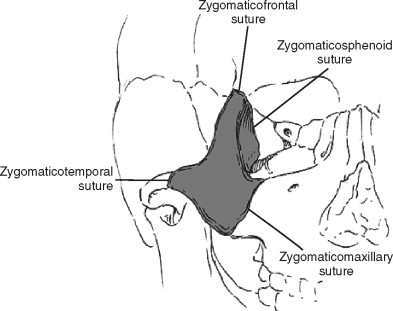
Since the zygoma is composed of fairly dense bone, it typically functions as a unit; therefore, fractures typically occur along sutures, rather than through the zygoma itself. Two fairly common exceptions are isolated fractures of the zygomatic arch (typically depressed) and the pneumatized inferior orbital rim/anterior maxillary sinus wall. Orbital floor fractures typically course through the inferior orbital foramen, potentially involving the inferior orbital nerve, leading to anesthesia of the cheek and upper portions of the lip.
For accurate evaluation of the zygoma, both axial and coronal images are needed. The lateral orbital wall is often interrupted or angulated on axial images. A common confounder is confusing the normal suture for fracture, and occasionally slight widening of the suture (diastasis) is the only clue. Comparison with the opposite side is helpful. Evaluation of the orbital floor is extremely difficult on axial images, and coronal and sagittal reformats are extremely useful. The curvilinear orbital floor should appear smooth and interrupted only by the interior orbital fissure.
Orbital Fractures
Orbital fracture can occur in isolation or as part of named fractures, most commonly the ZMC, naso-orbital-ethmoid (NOE), and Le Fort II. When seen in isolation, the mechanism of injury is likely due to a piston-like increase in intraorbital pressure resulting in “blow-out” or “blow-in,” referring to floor or medial wall fractures, respectively. It is important to identify these types of fractures since any change in orbital volume can severely impair vision. Rectus muscle injuries, commonly associated with these fractures, must be excluded as well.
On imaging, the orbits should appear smoothly rounded with interruption only at the location of expected sutures. In the setting of trauma, fat density (<-10 HU) within the maxillary or ethmoid air cells is related to fracture until proven otherwise. The same rule applies to the presence of intraorbital air. Rectus muscle injuries are common with this fracture type and usually detected as asymmetric thickening or a rounded appearance of the normally slit-like muscle. A bony fragment in close proximity implies entrapment, requiring surgical correction within 24-72 hours to minimize the potential of long-term motility problems ( Figure 8-4 ).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


