http://evolve.elsevier.com/Hatrick/materials.
Few materials in dentistry are used as frequently or with as much variation as dental cements. There are an impressive number of dental cements available, and each may have specific or multiple uses. No single cement is universally acceptable and fulfills all applications; rather, various cements are available whose properties and manipulation lead them to be an appropriate choice for a given application. In most cases, cements have inferior strength and high solubility when compared with other restorative materials and, with the exception of resin and glass ionomer cements, have little or no adhesive properties. Even with these limitations, the use of cements in a wide variety of dental procedures is extensive. The influx of different types of prosthetic restorative materials to choose from, ranging from gold crowns, PFM (porcelain-fused-to-metal) crowns, all-ceramic crowns, indirect composite resins, and CAD/CAM (computer-assisted design/computer-assisted machining) milled products, has dramatically changed the way cements are chosen. Adding to this, there are cements specifically targeted for specialization in orthodontics, endodontics, surgery, and implants. Today’s adhesive dentistry, using the acid-etch bonding technique, has been shown to be the most effective method of ensuring retention and reducing microleakage. With the multitude of available cements and their applications, it is easy to become confused as to which cement should be selected for a given situation. In most cases, the dentist will select the cement for the procedure on the basis of mechanical as well as biological considerations. It becomes the dental assistant’s responsibility to manipulate the cement to the proper consistency within a specific time frame. Many expanded function auxiliaries are also placing the cement and removing it at the end of a procedure. The dental hygienist may be placing and removing cements and instrumenting against their surface during periodontal procedures. It is important that the allied oral health practitioner have a thorough understanding of cement uses, properties, limitations, and manipulation to effectively use these materials. Although there is no single cement that serves all purposes, the cement you chose should strike the right balance between performance and handling characteristics.
Uses of Dental Cements
Pulpal Protection
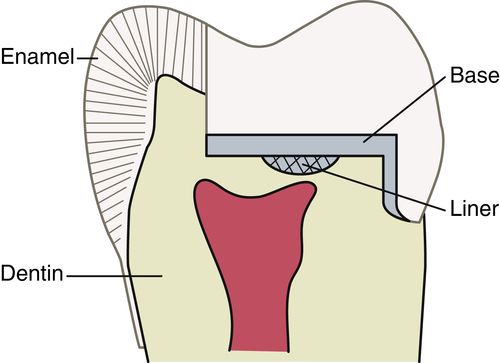
The bacterial effects of caries, the biological response to chemicals contained in restorative materials, and even the cutting of tooth structure may cause pulpal irritation. Pulpal irritation can also occur as the result of thermal conductivity of metal restorations placed near the pulp, and when the dentin remaining over the pulp is too thin to withstand compressive, tensile, and shearing stresses. Many of the chemicals contained within the materials used to restore teeth have the potential to cause irritation. Older amalgam formulations were prone to more corrosive products leaking into the tubules of the tooth structure, causing discoloration. Cavity varnishes, liners, and bases act as protective layers between the dentin and the restorative material (Figure 14-1). There has been a dramatic reduction in the use of pulpal protection materials as resin bonding technologies and high-copper amalgams have replaced these older types of restorations.
Cavity Varnish
Cavity varnish acts as a protective barrier between preparation and restoration. Varnish formulations are solutions of natural resins (copal) or synthetic resins dissolved in a solvent such as alcohol or chloroform. The varnish is applied in two or three layers over the surface of the preparation. The solution is placed in a thin film, allowing evaporation of the solvent to occur for 5 to 15 seconds before application of the second layer. The remaining resin protects the pulp by sealing the tubules from the penetration of irritating chemicals found in some restorative materials and luting agents. This resin varnish is thought to reduce the amount of microleakage and staining at the restoration/tooth interface. Copal varnishes, although popular for many years, are no longer widely used today. They were used extensively under amalgam restorations, but studies showed that they washed out, leaving a microscopic gap between the amalgam and the cavity preparation. Today’s dentin bonding agents, which also seal enamel and dentinal tubules, have largely replaced the use of varnish.
Low-Strength Base/Liner
Calcium hydroxide is used as a low-strength base/liner in cavity preparations in which dentin no longer covers the pulp. When close or very small exposures of the pulp are suspected, this material is used as an indirect or direct pulp-capping agent or as a dressing after vital pulpotomy procedures on primary teeth. The two-paste system involves the use of calcium hydroxide, zinc oxide, and glycol salicylate. Equal amounts of catalyst and base pastes are incorporated to a creamy consistency.
Calcium hydroxide has an alkaline pH between 9 and 11. This alkali stimulates secondary dentin when in direct contact with the pulp, providing a barrier between pulp and restoration. It has some antimicrobial and thermal insulating properties and provides minimal strength to support the forces of condensation. Under amalgam restorations calcium hydroxide paste slowly leaches out over time.
High-Strength Base/Liner
High-strength base/liners provide thermal insulation and support for restorations. Cements used as bases are mixed to secondary consistency—a thick putty-like consistency that is condensable and can be rolled into a ball or rope. Bases placed at a thickness of 0.75 mm or greater provide protection from the thermal conduction of metallic restorations and galvanic shock. When the cavity preparation is so deep that there is 2 mm or less of remaining dentin over the pulp, many clinicians will choose to provide mechanical support for the restoration by first placing a cement base. The restorative material is placed after the initial set of the base has occurred.
Buildup
A buildup, much like a high-strength base/liner, provides mechanical support for a restorative material when an excessive amount of tooth structure is removed. The remaining tooth structure may first need to be rebuilt to better support the restorative material or to act as a foundation before crown preparation. With placement of a cement buildup, the compromised tooth is reinforced (Figure 14-2). Resin-modified glass ionomer and resin cement are the strongest of the cements. Typically, resin cement is not used in thick layers as a buildup, but composite resin serves well for this purpose. Resin-modified glass ionomer cement is frequently used as a buildup material when only a portion of the coronal tooth structure is missing so that there is still remaining sound tooth structure to support the crown. Its desirable features are its strength (compared to the conventional cements), chemical bond to the mineral component of enamel and dentin, and good seal to the tooth and fluoride release.
Luting, Bonding, Cementation
Retention of restorations through luting/bonding/cementation has been a challenge to dentistry. Adhesive dentistry involves the application of an adhesive at the interface between the tooth surface and the restorative material. Good adhesion requires physical, chemical, and/or mechanical mechanisms that bind the tooth structure (substrate) to the restoration. A good adhesive provides resistance to separation and seals the interface of the substrate and restoration. Cements can be placed into two categories:
Luting cements: Luting cements achieve retention by filling the interface between the restoration and the tooth substrate, much like household cements.
Bonding (or adhesive) cements: Stronger than luting cements, bonding (or adhesive) cements fill the interface and provide micromechanical retention between the tooth substrate and the resin-based cement and restorative materials.
Mechanical luting with traditional cements was the only means of accomplishing cementation until dentin bonding with acid-etch systems was developed in the mid-1960s, leading to today’s adhesive dentistry. Successful cementation ensures predictable retention for the indirect restoration. The restorative material itself may be the primary determinant for the cement selection. When choosing a luting/bonding agent, the clinician must consider which of the following indirect restorations are being used:
• Metal and metal-based restorations—crowns, bridges, inlays, or onlays
• Glass-ceramic restorations
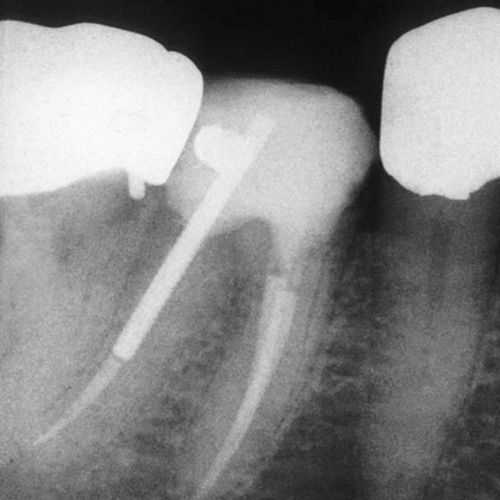
FIGURE 14-2 Radiograph of a cement buildup over endodontically treated tooth #30, to reinforce the remains of the tooth in preparation for crown placement. (Courtesy of Steve Eakle, University of California, San Francisco [San Francisco, CA].)
• High-strength ceramic restorations
• Indirect composite restorations
Other considerations include the amount of mechanical retention from the form of the preparation and the patient’s parafunctional habits (i.e., bruxing). In order for the cement to be successful, the tooth preparation must have adequate retention and resistance form. While bonding cements can enhance retention of the restoration, they cannot overcome the negative influence of an over-tapered, non-retentive preparation.
A luting agent is a material with low viscosity that, placed between tooth structure and a prosthesis, sets and firmly attaches the prosthesis to the tooth structure. New-generation luting cements with adhesive capability are now successfully used to improve the clinical success of fixed prosthodontics.
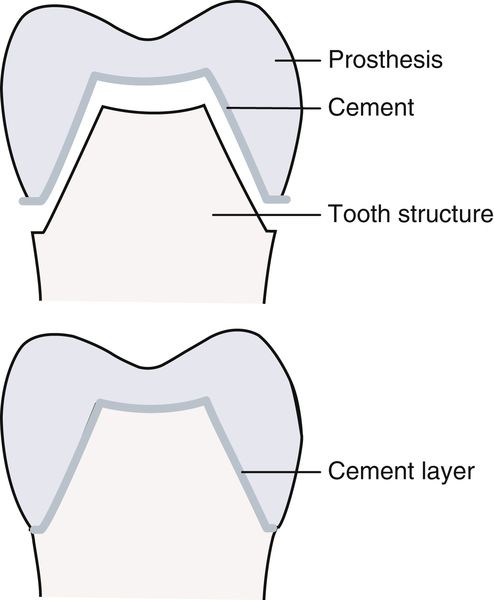
Cements used for permanent or temporary luting (i.e., the cementing together of two components) of fixed prostheses, orthodontic bands and brackets, and pins and posts must have good wettability and flow to provide a thin film thickness. When the tooth structure and the fixed prostheses are in intimate contact, a microscopic space exists—the tooth/restoration interface. This space is often created in the dental laboratory to allow room for the cement. Without this interface and because of the thickness of the cement, the restoration may be prevented from seating completely. CAD/CAM restorations allow the cement space to be milled into the restoration. The primary purpose of both luting and bonding cements is to fill this space (Figure 14-3). Cements mixed to primary consistency must have low-enough viscosity to be able to flow into a film thickness of 25 μm (micrometer, or micron) or less. If the viscosity of the cement is such that the prosthesis fails to regain intimate contact with the tooth, a thick layer of cement will be exposed at the margin. This may also occur if the margins do not fit precisely before luting. Exposure of cement to oral fluids at the margins results in dissolution of the cement. As cement is lost at the margins, bacterial plaque can accumulate beneath the crown where the patient cannot clean, resulting in tooth sensitivity and/or recurrent caries. Bonding cements have the ability to chemically bond the prosthesis to the tooth. The chemical bond enhances retention by reducing the separation created by the tooth/prosthesis interface.
Orthodontic Bands and Brackets
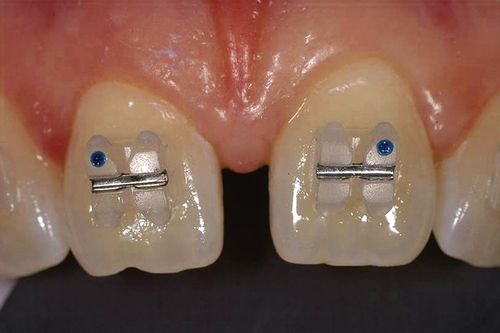
Orthodontic bands and brackets are retained on teeth for several months or even years. Brackets are usually bonded directly to the tooth structure (see Chapter 5 [Principles of Bonding] Procedure 5-3), whereas bands are luted with a dental cement. The cement must adhere tenaciously to the enamel and the orthodontic appliance to provide leverage for tooth movement and when the bond is removed have minimal effect on the tooth surface. Demineralization of the tooth surface due to solubility of cements and resultant leakage of bacteria between the bands and the tooth surface has been problematic for many patients. This concern has been minimized to some extent with fluoride-releasing, anticariogenic glass ionomer cements (Figure 14-4).
Restorations
Permanent, Intermediate, and Temporary/Provisional
Because of their lower strength and wear resistance and higher solubility, cements are not frequently chosen as permanent restorations. The exception is glass ionomer cement (GIC), which, because of its release of fluoride, is used for class V restorations of root caries in adults and for restoration of primary teeth (see Chapter 6 [Composites, Glass Ionomers, and Compomers]). The formulation of Glass Ionomer Cement (GIC) as a restorative material is different than the GIC luting cement. GIC luting cement must achieve a low film thickness for successful cementation.
As temporary/provisional and intermediate restorations, dental cements are mixed to secondary consistency. The choice of cement for this type of restoration is largely based on the particular clinical situation. Provisional restorations are used for emergency situations when appointment scheduling does not allow sufficient time to place a permanent restoration. Provisional restorations are placed when a tooth is symptomatic or when deep caries removal is required. By placing a sedative provisional restoration, the dentist is able to evaluate the response of the pulp before reappointment for a permanent restoration. Provisional and intermediate restorations are used to restore teeth awaiting treatment such as inlays, between endodontic appointments, or when extensive treatment plans require several weeks or months of coverage before treatment can be completed.
See Chapter 18 (Provisional Restorations) for a discussion of provisional luting and intracoronal cement provisionals.
Surgical Dressings
As surgical dressings, cements are used to provide protection and support for the surgical site, to provide patient comfort, and to help in the control of bleeding. Most clinicians prefer a noneugenol dressing, which may be dispensed in both light-cure and chemical-cure formulas. These materials are mixed to a soft putty-like consistency; they harden when placed over the tissue, forming a rigid covering. They are mechanically retained in place by gently forcing the material into the embrasure space and under the contact. For removal a blunt instrument is used under the edge of the dressing with gentle lateral pressure to loosen the pack. The clinician must be very aware of the location of sutures and avoid breaking the sutures away with the dressing. Large pieces of the dressing are lifted with cotton forceps and the surgical site is cleaned with a dilute solution of hydrogen peroxide or sterile water (Figures 14-5 and 14-6; and Table 14-1).
Properties of Dental Cements
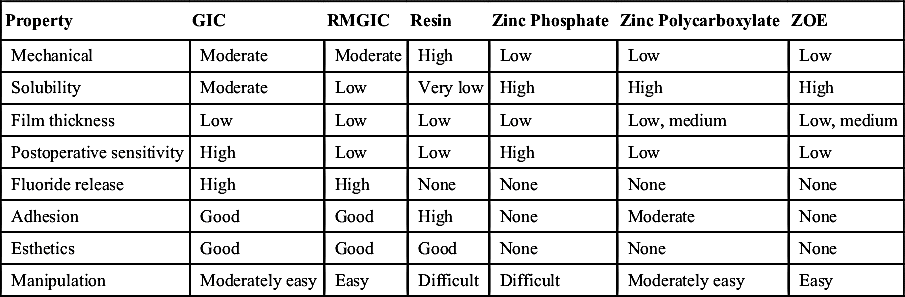
Properties of dental cements differ from one type of cement to another. No cement is ideal for every clinical situation. Although one type of cement may be appropriate for a single crown, it may not be ideal for a multiple-unit bridge; some cements work well on metal surfaces, but others are more appropriate for ceramic or porcelain surfaces. Ideally, the cement should adhere to the tooth structure as well as the restorative material. The clinician must consider both physical and biological properties when selecting cement for a specific dental procedure. The most important properties are as follows: strength, solubility, viscosity (affecting film thickness), biocompatibility, anticariogenic properties, retention, esthetics, radiopacity, and ease of manipulation (Table 14-2).
TABLE 14-1
| Uses of Cements | Cement |
| Low-strength base/liner | Calcium hydroxide, RMGIC |
| High-strength bases, buildup | Reinforced zinc oxide eugenol, zinc phosphate, zinc polycarboxylate, GIC, RMGIC |
| Permanent cementation | |
| Cast crowns, inlays/onlays, and bridges | Zinc phosphate, zinc polycarboxylate, GIC, RMGIC, resin-based |
| Porcelain, ceramic or composite veneers, inlays, onlays, and metal-free crowns | Resin cements and self-adhesive resin cements |
| Endodontic posts | GIC, RMCIC , resin, and self-adhesive resin |
| Orthodontic bands | Fluoride-added zinc phosphate, GIC, RMGIC |
| Orthodontic brackets | GIC, RMGIC, resin-based |
| Provisional cementation | Zinc oxide eugenol, noneugenol, zinc polycarboxylate |
| Provisional restorations | Reinforced zinc oxide eugenol, polycarboxylate, zinc phosphate |
| Surgical dressing | Eugenol and noneugenol |
Strength
The cement’s resistance to deformation/fracture under an applied force is a measure of its mechanical properties. Cements must be strong enough to resist the forces of mastication and the dynamics of the patient’s mouth and occlusion. Compressive, tensile, and flexural strengths are important considerations for differing cement applications. Bond strength is important in high-stress areas. Adhesive failure is seen when the prosthesis comes off cleanly; the break occurred at the interface and is a test of the bond. If the failure occurred in the bonding agent itself, this is called cohesive failure and is a test of the strength of the bonding material. Failure that results because the bond is stronger than the tooth substrate may result in the tooth rather than the restoration breaking.
The strongest cements are resin cements, and the weakest is zinc oxide eugenol. Cements used for permanent luting and high-strength bases need good compressive, tensile and flexural strength. As can be seen in Table 14-2, resin-based cement is high in mechanical strength and fracture toughness, and polycarboxylate cement is low in both. Most cements consist of a combination of powder and liquid; their ratio determines many of their properties. The strength of cement is controlled primarily by the amount of powder used in the prepared mix. In general, an increase in the powder-to-liquid ratio increases the strength of the cement. However, excessive powder or liquid can weaken the cement.
Solubility
The tendency of cements to dissolve in the oral fluids, leading to marginal ditching, microleakage, recurrent caries, and failure of the restoration, is one of the greatest challenges for dental cements. Many of the cements used in dentistry will disintegrate in the oral environment over time. Solubility is important whenever the cement is expected to remain exposed to mouth fluids for prolonged periods. High resistance to oral solubility helps to maintain the marginal seal. Bonded, resin-containing cements are as close as possible to being insoluble. Again, the amount of powder incorporated into the final product will influence greatly the solubility of the resultant cement.
Viscosity and Film Thickness
The consistency, or viscosity, of mixed cement refers to its ability to flow under pressure. This is particularly important in the case of cement used for luting, because it determines the dentist’s ability to seat the indirect restoration properly and completely. If the film thickness is too thick the restoration will not seat and there will be excessive marginal cement exposed. This will result in excessive occlusal adjustment and the increased likelihood of recurrent decay and staining due to the washing away of cement at the margins.
For primary consistency, also known as luting consistency, cements should be able to be mixed thin—to about the consistency of honey.
The cement must be able to flow easily and completely throughout the interface between the restoration and preparation. For a cement to be considered an effective luting cement, American Dental Association (ADA) specifications require the cement to be able to flow into a film thickness of 25 μm or less. As a comparison, a human hair is about 20 to 50 μm. Resin-based cements and resin-modified glass ionomer cements are thixotropic, meaning they will flow under pressure. When cementing with any of these cements the patient should be instructed to bite down on a stick during initial set to force the material into all intracoronal areas.
Secondary consistency requires the addition of powder to increase strength and bring the cement to a thick, putty-like consistency. Cements mixed to secondary consistency are used as bases and restorations, temporary or permanent. The addition of powder increases the viscosity and strength and decreases the solubility of the cement.
Several factors influence the consistency of mixed cement. Temperature has a great effect; a lower temperature will slow the setting reaction, giving the clinician more working time and allowing incorporation of more powder into the liquid.
Biocompatibility and Anticariogenic Properties
Cements must be safe to use on patients; where a specific type of cement may be appropriate in one circumstance it may be inappropriate in another. A cement may be suitable for use in a conservative preparation while causing sensitivity and even pulpal necrosis in a deep preparation or where there is an extensive amount of dentin surface coverage. Many cements represent a combination of a powder of zinc oxide or powdered glass and an acid. The pH of the acid both at placement and after complete setting is a matter of concern. Postoperative pulpal sensitivity is also related to the pH and manipulation variables of the cement. Other causes include unsealed dentinal tubules, trauma to the pulp during preparation, and bacterial leakage under the provisional restoration. Careful attention to powder-to-liquid ratios, dispensing technique, and mixing recommendations can minimize this concern. A cement with low risk for postoperative sensitivity should be selected when the susceptibility to sensitivity is a concern. Eugenol, found in the liquid of zinc oxide eugenol cements, has an obtundent (i.e., soothing, sedative) effect on the pulp.
Retention and Adhesion
Good adhesion is a critical component of both fixed prosthodontics and restorative dentistry, as good adhesion helps to increase strength and minimize microleakage. Adhesion is the bonding of dissimilar materials by the attractive forces of atoms or molecules.
Mechanical adhesion: Mechanical adhesion is based on the interlocking of one material with another; an excellent example is Velcro.
Chemical adhesion: Chemical adhesion occurs at the molecular level, when atoms of the two materials swap electrons (ionic bonding) or share outer electrons (covalent bonding).
In many dental applications, chemical adhesion and mechanical adhesion occur together. We now have a much better understanding of the surface characteristics of enamel and dentin and the requirements needed to obtain good bonds to them. The most recent dental cements, using resin adhesive technologies, strive to achieve a micromechanical and chemical bond between the tooth and the restoration. Several things may weaken the strength of the adhesion between two materials, including differences in the coefficient of thermal expansion of the two materials, dimensional changes that occur during setting of the adhesive agent, and contamination of the substrates by water and saliva or by residual enamel and dentin debris, known as the “smear layer.”
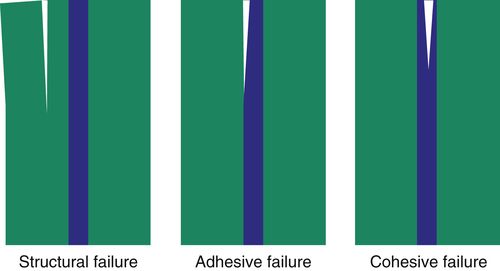
There are three possible reasons for failure of an adhesive. Structural failure occurs as a result of internal failure of the substrate material; the tooth itself breaks away from the restoration, leaving the restoration intact. Adhesive failure occurs when the substrate separates from the adhesive layer; the restoration is dislodged from the tooth and/or recurrent caries forms. Cohesive failure occurs when there is internal failure of the adhesive layer; this may also result in dislodging of the restoration with the cement layer still present in the restoration and on the tooth substrate (Figure 14-7).
Failure of the adhesive will result in failure of the restoration if the direct or indirect restoration breaks away from the tooth structure altogether, or if leakage occurring between the tooth structure and restoration or prosthesis, results in deterioration of the margins and the formation of secondary caries. The acid-etch bonding system is the basis of today’s adhesive dentistry. In this process hydroxyapatite is removed from the tooth structure with the etchant to create micropores, and the resin monomers of the cement fill the micropores to create resin tags that micromechanically lock the substrate to the restoration (Figure 14-8).
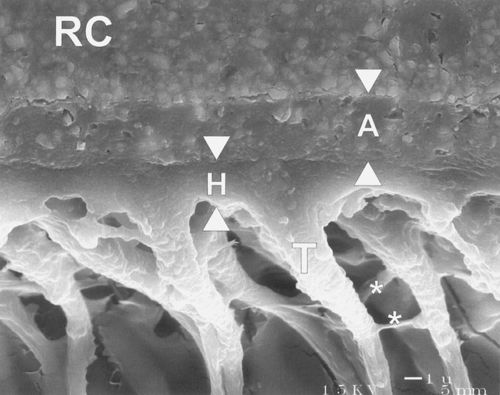
FIGURE 14-8 Scanning electron micrograph of interface bonded with dental adhesive. A, adhesive layer. H, hybrid layer with T, resin tags. RC, resin composite restoration. (From Frankenberger R, Perdigão J, Rosa BT, et al: “No-bottle” vs “multi-bottle” dentin adhesives—a microtensile bond strength and morphological study. Dent Mater 2001;17:373-380.)
Esthetics
Cements are available in a variety of shades and opacities. Typically, resin cements are used for bonding porcelain veneers, ceramic or composite inlays and onlays, and ceramic full crowns. Usually, a shade is chosen to approximate the shade of the restoration, so that the appearance of the restoration is not altered by the underlying cement as light passes through the restoration and reflects off the cement. On occasion, it is necessary to mask the color of the dentin, especially if it is discolored. In this situation, an opaque cement of the appropriate shade is selected. Many manufacturers provide try-in paste; this water-soluble paste is matched to the base shade of the cement and is used to temporarily tack the restoration in place to check the shade of the final product.
Radiopacity
Radiopacity is an important property in the measure of the success of a cement. High radiopacity will allow the cement to show when examined with x-rays so that it will not be mistaken for caries or a void. Good radiopacity will also make excess cement easier to see; this is particularly important in the case of implants and in restorations with deep subgingival margins.
Manipulation
Storage
Cements should not be stored in warm or humid areas of the dental office. If you are refrigerating your cement, it should be taken out of the refrigerator at least 1 hour before use so that it can reach room temperature.
Mixing
It is important that cements be mixed to their appropriate consistency in accordance with manufacturers’ recommendations, with meticulous attention to detail. Cements that are mishandled may lead to difficulties in seating, retaining the restoration, or even pulpal sensitivity. Cements may be hand mixed or may come in predosed capsules or automix syringes. Newer delivery techniques have eliminated the need to mix cements by hand. Hand mixing is thought to be responsible for porosity due to void or air bubble inclusion in the final product, compromising the bond between the restoration and tooth substrate. Cements delivered as a single component or via automix, light-cure, or dual-cure systems eliminate the need to hand mix.
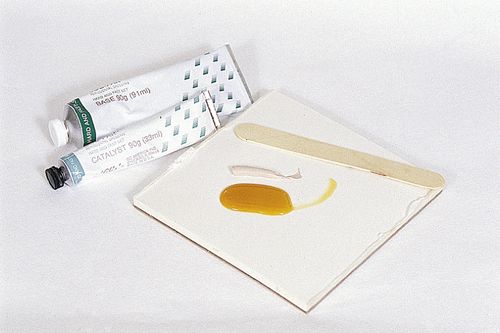
Even skilled hand mixing may incorporate air that is thought to lead to the reduction of bond strength between the restoration and the tooth substrate. If hand mixing is chosen, the amount of time taken to mix the cement must be carefully monitored: too much time and the cement may be too viscous; too little time and the cement may not be mixed thoroughly (Figure 14-9).
Cements, like composite restorative materials, come in self-cure, light-cure, and dual-cure delivery systems.
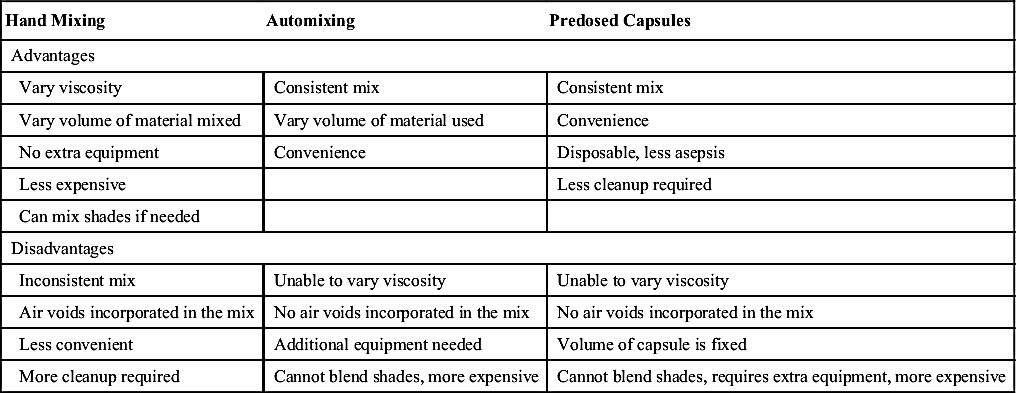
Advantages and disadvantages of each delivery system are listed in Table 14-3.
Working and Setting Times
The working time and the setting time are considerations in the choice of cement and mixing mechanism. A longer working time is needed for cementation of longer span bridges versus single crowns and a shorter setting time is required for difficult-to-isolate areas. Patient considerations and the dental team’s mixing and delivery skills play a part in the selection of an appropriate cement. The dental assistant is responsible for delivering the cement at the proper consistency within very definite time frames. A skilled assistant must be able to routinely mix cements rapidly to their proper consistency.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses