Fig. 7.1
Selection of clinical cases of molar endodontics with (a) a right mandibular first molar (46 FDI, #30 Universal) with inadequate root canal treatment, periapical lesions on both roots and a large amalgam restoration retained by two metal posts; (b) a long-span bridge restoration including three molars, with metal posts in multiple root canals; (c) tooth 36 (#19) with cast post and core in precious alloy before crown placement. Note the very thin remaining dentin layer toward the furcation of both roots indicated by arrows; (d) three-unit bridge placed 3 years ago with metal post and resin core in tooth 37 (#18). Note vertical root fracture indicated by the red arrow; (e) example of bridge restoration anchored by root canal posts, but with massive destruction of tooth structure due to recurrent caries; (f) left: inadequate root canal treatment with periapical radiolucent areas and resin composite restoration with two large metallic screw posts; center: same case after removal of the posts, endodontic retreatment; immediately after crown placement and 4-year follow-up showing periapical healing; (g) endodontically treated upper molar with large coronal tissue loss restored with bonded overlay composite restoration after preliminary margin relocation (Courtesy of Dr. T. Hollaert); (h) left: tooth 25 (#13) with vertical root fracture, 26 (#14) and 27 (#15) with mesial decay; right: same case after extraction of 25 (#13) and 27 (#15); crown preparation of 26 (#14) resulting in loss of tooth structure and pulpal inflammation requiring root canal treatment; the remaining composite material will have to be replaced; (i) left: tooth 26 (#14) with apical radiolucency on MB root, with a carrier-based fill in a pulp-floor perforation; right: tooth after endodontic retreatment, removal of the carrier, repair of the perforation, and lesion healing at the 1 year follow-up. The initial large composite restoration was maintained, and the access cavity filled by a direct composite
-
Are posts required for the restoration of endodontically treated molars? Which posts, for example, which type, shape, size, or diameter?
The placement of certain posts usually requires additional dentin removal, and may therefore result in a weakening of the tooth (Fig. 7.1c). The stiffness of metal posts materials could also generate inappropriate stresses on the thin remaining dentin walls, which may result in root fracture (Fig. 7.1d).
-
Do posts reinforce or weaken endodontically treated molars?
It must be kept in mind that retention of a restoration (survival) does not necessarily mean clinical success. In some instances, even if the retention provided by the post is sufficient to maintain the restoration in place, the loss of marginal seal should already be considered as a failure, and restoration repair or replacement should be performed. This is illustrated by a very extreme situation in Fig. 7.1e, but more moderate cases of this very situation are not uncommon. While reinforcement of thin, fragile root walls with a bonded fiber post is possible, posts often weaken teeth due to nonphysiological forces exerted and further loss of dentin to prepare the post space. This leads to a more general transition in modern dentistry, now giving more importance to the tooth survival than to the restoration survival, the former being certainly more important from a patient perspective.
-
Can an endodontically treated molar with extensive tissue loss be restored solely by a bonded restoration? Are posts required for root canal-treated molars?
Dental material technologies have evolved tremendously over the last decades. In particular, resin-based composites, which can be micromechanically and chemically bonded to the dental tissues, have become more and more reliable. By tradition, some dentists keep using metal posts to retain bonded composite restorations (Fig. 7.1f), while they accordingly should be replaced by fiber-reinforced resin-based posts, or possibly by no posts at all, either in case of a composite core covered by a full crown, or more recent adhesive strategies such as the so-called endocrowns or overlays in general (Fig. 7.1g).
-
Is adhesive technology sufficient to reinforce the tooth?
The preparation of a full crown frequently results in additional removal of sound tooth structure (Fig. 7.1h). Fiber posts rely on luting resin that fills discrepancies, so that additional widening of the space becomes unnecessary. This is supported by the fact that a ferrule should be obtained on endodontically treated teeth. If a 2 mm ferrule can be obtained, a post is not needed to retain the buildup.
-
Is a ferrule a must in endodontically treated molars or is tissue preservation more important? Is partial restoration a valid alternative to full crown? Should the cusps be covered?
A ferrule is generally admitted to be a must to prevent dislodging forces that will lead to coronal leakage. Cusps should be covered if structure loss is the size of an MOD preparation, or larger, and in undermined coronal walls. It should be considered in cases with loss of marginal ridges.
-
After endodontic (re-)treatment through an existing restoration, should the latter be replaced or repaired?
Very often, endodontic treatment is performed through an existing restoration, either a crown or a filling (Fig. 7.1i), which in some instances are still serviceable. Here preservation of the previous restoration and the direct restoration of the occlusal cavity may suffice.
-
Can endodontically treated molars be part of a multiunit restoration?
Despite the development of implant technology, endodontically treated teeth are still valid abutments in large-span restoration. This chapter focuses on single-tooth restoration for endodontically treated molars; detailed considerations for complex treatment plans likely require multispecialty discussion and are beyond the scope of this book.
-
Finally, how should a tooth with poor endodontic prognosis be restored?
Despite the high success rate of endodontic procedures, some teeth are compromised due to problems such as broken instruments, perforation, or stripping, which may result in a poorer prognosis of the endodontic treatment. A direct restoration for teeth with a poor prognosis may be an appropriate solution.
This list of question is not exhaustive, and the answers not comprehensive, but they illustrate part of the decision-making process of the dentist restoring a molar after root canal procedure, which offers specific challenges (Box 7.1). This chapter will provide considerations to help practitioners answer these questions, and make the best possible clinical decision.
Box 7.1. Specific Properties and Findings Regarding Endodontically Treated Molars
-
They differ from other tooth types, since they endure most of the vertical masticatory forces (100–300 N), and are protected from lateral forces by anterior teeth through anterolateral guidance.
-
Root canal therapy itself does not seem to weaken dental structures; increased susceptibility to fracture appears to be due in majority to coronal and pericervical hard tissue removal, not to local changes of dentin characteristics.
-
Three major technological developments are challenging the way endodontically treated molars have so far been restored:
-
Adhesive dentistry and the development of increasingly more reliable dental adhesives
-
The rise of digital technology, enabling the rapid and reliable design and manufacture of restoration in practice
-
The development of “Bio-”materials, with characteristics closer to the replaced tissues
-
7.3 Molar Restoration in an Era of Adhesive Dentistry, Digital Technology, and Biomaterials
Molar teeth endure the majority of the vertical masticatory forces, while most of the time, they are protected from lateral forces by anterior teeth through anterolateral guidance [10]. Occlusal loads sustained by molars during normal function range roughly between 100 and 300 N, while they do not exceed 50 N for premolars, and are lower yet for anteriors [11]. Higher values for maximum voluntary bite force have also been reported (500–800 N) [12], and can potentially reach even higher levels in case of parafunctions [10]. The variability is due to factors such as the type of food [13], age [12], or gender [14].
This underlines that restorative concepts should be specific to each tooth type, since each is submitted to very different challenges. Molar teeth are mostly submitted to axial forces of high intensity. Since root canal treatment weakens teeth due to loss of structure, there is a particular need to adequately protect endodontically treated molars against tooth fracture. In this regard, it is to some extent surprising that most reviews and guidelines dealing with restoration after endodontic treatment propose general concepts of restoration for all teeth, and not specific to each tooth type [15].
Tooth weakening following endodontic treatment seems to have little [10] or nothing to do [16] with local changes of dentin characteristics following endodontic treatment (e.g., loss of moisture, use of chelators, irrigants, or medicaments). The major cause for increased susceptibility to fracture of endodontically treated teeth appears to be the loss of hard tissue [10]. Endodontically treated teeth indeed very often undergo additional dentin removal in the process of the restoration, for example:
-
Creating post space
-
Preparation for full crowns
-
Occlusal reduction of thin dentin walls
In this regard, it is quite sobering that a major cause of further tissue damage is iatrogenic, especially given the efforts that are currently invested in developing strategies to regenerate dental tissues in order to strengthen tooth structure.
In light of this paradox, it is important to weigh the necessity or rationale of additional tissue sacrifice. The ultimate goal of dentistry is to retain a healthy complement of teeth for a lifetime; therefore, appropriate strategies should be “conservative” in order to control, rather than eliminate a condition, with existing tissues preserved as much as possible [17]. Indeed, it appears that habits, heritage, and/or traditions sometimes lead to a “conservative” dentistry in the sense of holding to traditional attitudes and values and cautious about change or innovation. In this regard, it is significant to consider certain advances and evolutions made over the past few decades that are of prime importance when considering the best way to restore endodontically treated molars: adhesive dentistry, digital technology, and biomimetics.
Adhesive dentistry started in 1955 with Buonocore, and bonding materials and strategies have since considerably evolved. Dental adhesives are now more and more reliable and predictable [18]. Specifically regarding restoration of endodontically treated molars, composite restorations enable us to do more and more without mechanical, nonadhesive, retention features such as cavity taper, grooves, or posts. Retention elements necessary in the era of silver amalgam are no longer needed, and this allows for more tissue preservation.
Another major breakthrough that is very likely to greatly affect tooth restoration is the advent of digital technology, specifically the CAD/CAM technology. Clearly, digital technology is changing dentistry and it is likely that the use of computers will replace manual tasks with the hope to get results faster and with fewer errors [19]. For endodontically treated teeth, with a likely further spread of CAD/CAM devices, clinicians may have the option of placing a permanent indirect restoration immediately after completion of endodontic treatment. As mentioned above, this approach is highly desirable in terms of endodontic success, as it limits or avoids temporary restoration failure.
Finally, another interesting evolution is the advent of “bio”-materials. Far more than just a buzzword, the addition of these three letters in front of the word “material” has a clear meaning, in that materials should not only be considered for their intrinsic qualities, but in the context of their integration in a living organism. Biomaterials are expected to behave and perform in a similar fashion as the tissue they replace. Therefore, their characteristics should be as close as possible to the tissues replaced. This should be kept in mind by clinicians when choosing the best strategy and most adapted material for tooth restoration. The current trend is to use materials whose mechanical properties are as close as possible to the dental tissues they replace [20], this is sometimes implied by the expression “biomimetics.”
For example, an important property to consider is the elastic modulus, which is the tendency of a material to be reversibly deformed when a force is applied to it. A significant difference of elastic modulus between the replacement material and the tissue replaced might result in inappropriate interfacial stress generation. The elastic modulus was determined to be about 19 GPa for dentin and 80–94 GPa for enamel [21]. In comparison, it is much higher in metals and other dental materials, for example, about 110 GPa for titanium, 200 GPa for stainless steel, 200 GPa for zirconium, and 300 GPa for aluminum oxide. This major difference in modulus suggests that metal posts in roots should be used with caution. In contrast, the elastic modulus of fiber posts ranges between 10 and 25 GPa, which is much closer to that of dentin [22].
The elastic moduli of currently available materials for coronal restoration are as follows: 10–15 GPa for hybrid resin-based composites [23], 10–17 GPa for glass ionomer [24], about 20 GPa for amalgam [25], 71 GPa for feldspathic porcelain, and 224 GPa for zirconia [26]. Interestingly, it has been shown that an increase in elastic modulus of the restoration from 5 to 20 GPa actually results in a 30 % reduction of stress at the tooth-restoration interface under occlusal load [27]. Hence, it seems to make sense that the deformation under load of the restorative materials should be as close as possible to that of the tooth, which according to the above values points to resin-based composites for dentin, and feldspathic porcelain for enamel. As illustrated, many clinical situations show that a lack of respect of these biomimetic concepts can result in a failure. Nevertheless, it is also possible to find other clinical cases where these concepts of integration are not respected, but where the restoration can still be considered a clinical success. In fact, clinical experience seems to illustrate that in dentistry, a treatment might be successful despite what we do, not because of what we do. Therefore, and given the lack of clear clinical evidence, risks pointed out by in vitro data need to be carefully appraised when restoring root canal-treated molar teeth.
7.4 Objectives of the Restoration of Endodontically Treated Teeth
Generally, goals of the restoration of teeth after endodontic treatments can be summarized in three main objectives: to restore tooth functions, to prevent infection or reinfection of the root canal space by providing a fluid-tight seal and to protect the remaining tooth structure against further tissue damage (Box 7.2).
Box 7.2. Objectives for the Restoration of Endodontically Treated Molars
-
To restore function
-
Mastication
-
Occlusal stability
-
Contact points with neighboring teeth to ensure protection of the marginal periodontal tissues
-
Aesthetics (to a lower extent in the posterior sector)
-
-
To prevent the infection or reinfection of the root canal space by providing a fluid-tight seal
-
An adequate tooth restoration increases the chances of healing when combined with an adequate root canal treatment and obturation
-
-
To protect the remaining tooth structure against further tissue damage, in particular tooth fracture
-
Increase of tooth longevity
-
Although these general objectives are not specific to molars, the latter appear to be the most commonly extracted teeth among endodontically treated teeth (81 %) compared to premolars (16 %) and incisors/canines (3 %) [28]. Here, particular attention should be paid to the reasons for extraction, which were mainly nonrestorable caries (>60 %), far ahead of persistent endodontic failure, nonrestorable root or cusp fracture, and iatrogenic perforation, which were in that study cited in about 9–12 % each.
The major tooth functions that need to be restored include mastication, occlusal stability, and protection of the marginal periodontal tissues by providing appropriate contact points with neighboring teeth. At the same time an esthetic result must be achieved, while this is typically less critical in the posterior than in the anterior dentition. The restoration of these functions is not specific to endodontically treated teeth, but common to all damaged teeth and will not be the focus of this chapter.
The second objective, to prevent infection or reinfection of the root canal space, is of prime importance regarding the long-term success of endodontic treatment, as will be discussed in the next section.
Finally, the third objective, to protect the residual tooth structure against further tissue damage (carious or noncarious causes), is particularly relevant to endodontically treated teeth. In cases of structural loss after caries removal or preparation, endodontically treated teeth require protection against fracture. This third objective is particularly important and critical in molars, since they receive most of the masticatory forces, as will be described further. Hence, this chapter will propose considerations to prevent this major cause for endodontic treatment failure.
7.5 Fluid-Tight Seal of the Root Canal System
After completion of endodontic treatment, the priority is to establish an adequate coronal seal to prevent any infection or reinfection of the root canal space. This important aspect is not specific to molars but common to all types of teeth. Is the quality of coronal restoration of equal importance as the quality of the root canal filling regarding the outcome of endodontic treatment? This question has been the subject of debate in the endodontic literature (Fig. 7.2). The discussion arose from a report that cases with good coronal restoration, regardless of the quality of endodontic treatment (conditions 3 and 4 in Fig. 7.2) were associated with a significantly higher success rate based on the absence of periapical lesion in a radiograph than the opposite situation (80 %, conditions 2 and 4 in Fig. 7.2) [29]. The same authors find, comparing the worst- and best-case scenarios (situations 1 and 4 in Fig. 7.1, respectively), success rates of about 20 % and 90 %, respectively.
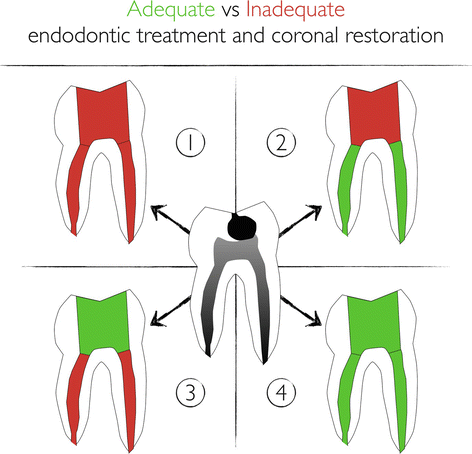

Fig. 7.2
Schematic diagram of possible clinical situations when restoring a root canal-treated molar (center). Clinical outcomes shown in cases 1–4 depend on the quality of both endodontics and restorative work, with better outcomes when both parts are done to quality criteria (red/green). See text for more details
Gillen and others [30] conducted a systematic literature review and meta-analysis of all papers published on this topic since the original work by Ray and Trope [29]. Based on new statistical analyses based on data from nine papers, they concluded that a better treatment outcome can be expected when performing both high-quality root canal treatment and restoration (situation 4 in Fig. 7.2) compared to either insufficient filling or root canal treatment (situations 2 and 3 in Fig. 7.2), where no significant difference in the odds of healing was observed [30].
In a best-practice approach, since it is clear that the highest treatment quality in both aspects results in the best chances of success, the joint and coordinated efforts of both endodontists and restorative dentists are necessary to achieve the best possible outcome. Importantly, these elements point out to endodontic specialists that a quality restoration is important for success of the endodontic treatment he/she performed. As mentioned above, a major reduction of survival after endodontic treatment is anticipated for teeth restored with temporary restorations compared to the teeth receiving a permanent restoration [1].
Along the same lines, in vitro data have pointed out that temporary materials (neither Cavit, conventional glass ionomer, or a combination of both) were unable to prevent bacterial leakage over a 2-month period, whereas a bonded-resin-based material was able to do so [31]. This problem becomes particularly striking, considering that nowadays the endodontic and restorative phases are more often in the hands of two different practitioners and treatment decisions are influenced by insurance coverage also. Hence, the joint and coordinated efforts of both endodontists and restorative dentists are necessary to achieve the best possible outcome for the patient.
Even when under the control of one general dentist, endodontic and restorative procedures are usually performed in two separate appointments. Therefore, one needs to consider approaches that can ensure immediate, reliable, and definitive sealing of the root canal system, very likely through an adhesive procedure. One possible approach is the one proposed by Magne’s group, called immediate dentin sealing (IDS). This procedure may consist of immediate placement of a bonding system at the surface of freshly cut dentin and was demonstrated to improve bond strength of indirect restorations as compared with delayed bonding procedure at the next appointment, when placing the restoration [32]. Hence, in the context of restoring endodontically treated teeth, IDS has a dual advantage: providing an immediate seal, and improving bond strength for the restoration to come (see Box 7.3). The additional placement of a thin layer of flowable resin-based composite at the entrance of the root canals and on the pulp chamber floor can also be recommended. It must finally be kept in mind that IDS requires the final restoration to be placed within the next 2 weeks after bonding placement. After longer periods, a reduction of the cohesion between bonding and resin-based composite was indeed observed [33], possibly due to the decay of free radicals within the adhesive layer, which reach undetectable levels in less than 1 month after light-curing [34]. An additional procedure including the placement of a silane agent is then required, as well as a fresh layer of bonding agent [35].
Box 7.3. Sealing the Endodontic Space
-
The combination of both good endodontic treatment and good coronal restoration results in significantly better endodontic treatment outcome
-
The placement of an adhesive resin-based composite layer at the entrance of root canals and over the whole surface of pulp-chamber and cavity immediately after completion of endodontic treatment represents the best way to prevent reinfection of the root canal system. This initial layer will serve as substrate for the subsequent adhesive restoration.
-
Immediate dentin sealing (IDS) is indicated first to reduce the risk of contamination of the root canal system associated with temporary restorations, and second, to increase bond strength of the future coronal restoration.
-
Ideally, the endodontist could/should take care of the placement of this initial layer. The subsequent placement of the permanent restoration as soon as possible requires agreement between both the endodontist and restorative dentist, both on best-practice restorative procedure and sequence.
As mentioned earlier, one of the objectives of the restoration of endodontically treated teeth is to protect the remaining tooth structure against further tissue damage, in particular tooth fracture. The major cause for increased susceptibility to fracture of endodontically treated teeth is the loss of hard tissue; it is important to weigh the impact of caries removal, preparation for coronal restorations, access cavities, or root canal preparation on tooth stiffness. This issue was evaluated in premolars in the classic work by Reeh and others [36], and the residual tooth stiffness relative to an unaltered tooth (100 %) was sequentially: 95 % after access cavity only, 80 % after occlusal cavity preparation, 54 % after two-surface cavity preparation, 37 % after MOD cavity preparation, 33 % after access cavity preparation, 34 % after root canal instrumentation, and only 32 % after root canal obturation.
In molars, the average residual tooth stiffness was reported to range between 81 and 95 % after an MO cavity preparation, and between 60 and 61 % after an MOD cavity preparation, depending on the cusp considered [37]. This is lower than what was observed for premolars, although it is problematic to directly compare the values of two separate studies. Nevertheless, it may be concluded that the reduction in tooth stiffness results mainly from cumulative tissue loss at the coronal level. To address this tooth weakening, three important clinical concepts need to be considered: the ferrule effect, the placement of post(s), and cuspal coverage.
7.6 The Ferrule Effect in Molars
The dental ferrule refers to a circumferential band of dentin of at least 1–2 mm of dentin coronal to the margin of the preparation for a full crown (Fig. 7.3). It has been suggested that the presence of a ferrule may reinforce endodontically treated teeth, the “ferrule effect,” especially in teeth restored with cast post and core [38]. It was also observed that an adequate ferrule lowers the impact of the other factors (post and core system, luting agents, or crown material) on the survival of endodontically restored teeth [39].
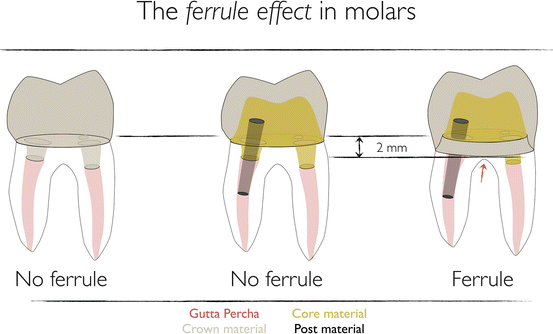

Fig. 7.3
From left to right, an endocrown (no ferrule), a post and core (either fiber post and resin composite core or metal cast post and core) covered by a full crown (no ferrule), and a crown covering a post and core with apical extension of preparation margin, providing a 2 mm ferrule. The red arrow symbolizes the risks the apical extension may represent, here regarding the furcation, but in general regarding the respect of the biological width space
Most research was done with single-rooted teeth and comparatively little data are available on molars. In the two major literature reviews that focus on the importance of the ferrule effect, one did not mention a single work devoted to molars [38] and the other reported the critical need for more clinical trials that investigate an effect on molars [39]. Only one clinical study focused specifically on endodontically treated, restored molars, and concluded that the amount of tooth structure available for ferrule (evaluated retrospectively from bitewing radiographs) may not be a significant prognostic parameter [40]. However, two other clinical studies included molars [41, 42] and both reported improved survival for teeth with ferrule (93 % at 3 years [41] and 98 % at 5 years [42]) compared to teeth without ferrule (74 % [41], 93 % [42]). Notably, in these two studies molars represented less than half of the teeth and a minority of the failures [42].
Therefore, while from a mechanical standpoint a ferrule is logical and recommended whenever possible, it is somewhat speculative to generalize and recommend ferrules for all molars based on these data alone. Moreover, it should be kept in mind that occlusal loads on molars are mostly axial, whereas the ferrule effect has mostly been demonstrated to be effective in protecting single-rooted teeth against lateral and oblique forces.
Interestingly, in an in vitro study comparing the importance of ferrule in endodontically treated molars restored with full metal crowns, it was reported that the presence of a 2 mm ferrule was a determinant factor on the fracture resistance and fracture mode. However, the forces required to induce fracture were well above the physiological forces, or even parafunctional levels, either in the ferrule group (2035–2934 N) or in the no-ferrule group (1528–1879 N) [43]. As stated before, results based on one type of teeth should no longer be generalized to all endodontically treated teeth without any distinction, as it is often the case in the literature.
Hence, given the lack of solid evidence in favor of the need of ferrule in molars, it is questionable whether it should be achieved at the expense of the remaining tooth structure (Fig. 7.3) and it is questionable to make the decision to extract a molar based solely on the lack of ferrule. Interestingly, when dentists are made aware of the additional tissue loss (3–45 %) associated with complete versus partial coverage restoration in molars, over 50 % of the clinicians altered their initial choice of restoration design from full to partial coverage [44]. Besides, the preparation of a ferrule at any cost in case of little remaining coronal tissue might be associated with additional problems. Notably, the subgingival margin placement can lead to a reduction of the biologic width space (distance between crown margin and alveolar crest) below the required 2–3 mm and to difficulties with the margin impression, excess luting cement removal, and cleaning of the area by the patient. The alternatives, crown lengthening or orthodontic extrusion, represent additional costs and delay for the patient; details of these procedures are beyond the scope of this text. Given the significant progress made in adhesive dentistry, preservation of coronal tissue should be contemplated instead of ferrule preparation in molars, and alternative approaches such as so-called endocrowns should be considered, as will be described further.
Admittedly, endodontic treatment in molars is typically rendered when a major portion of enamel and dentin has been already lost due to caries. Moreover, there are molars that may have a guarded prognosis (see also Chaps. 2 and 8) but still require a restoration (Fig. 7.4). Obviously, there is a range of clinical scenarios in the restoration of molar endodontics, and a variety of possible solutions will be discussed below.
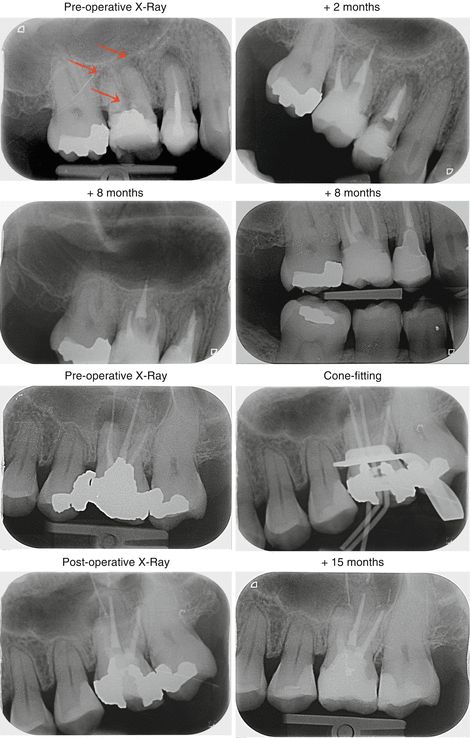

Fig. 7.4
(a) Teeth 15 and 16 (#4, 3) with periapical lesions, 16 (#3) with a perforation of pulp chamber floor (arrows). Both teeth received root canal (re-) treatment, and the perforation of tooth 16 (#3) as well as the vestibular canals were obturated. Direct composite restoration on tooth 16 (#3) and composite endocrown placed on tooth 15 (#4). Teeth are clinically asymptomatic at 8 months, and there are no signs of pathosis either in the periapical or in the furcal regions. (b) Tooth 26 (#14) presenting with a large periapical lesion with overextended fill and inadequate coronal obturation. The apical size of the MB root canal was very large and an apical plug was placed, followed by the placement of a direct composite restoration. At the 1-year follow-up, the tooth is asymptomatic and there is evidence of bone fill; the patient decided to keep the composite restoration
7.7 Post Placement in Endodontically Treated Molars
The question whether post placement is indicated in the restoration of endodontically treated teeth is quite difficult to answer with a clear yes or no based on the available literature. There are numerous factors involved, such as the post material or diameter, the quality of the bonding interface between post and dentin, the core material, the crown material, the amount of residual tooth structure, and others. This makes studies difficult to compare, and probably accounts for the contradicting results found in the literature. Importantly, tooth type is a major factor to consider, and most of the studies evaluating post placement were done on single-rooted teeth. The results obtained for incisors or premolars are not directly transferable to molars, and each tooth type has specific characteristics, notably the major differences in occlusal load intensity and directions [45]. Hence, only studies involving molars will be considered here. As regards the type of post, fiber-reinforced composite posts present characteristics that support their use instead of metal posts, since as already mentioned their elastic modulus is much closer to dental tissues, while at the same time displaying a fracture strength of 600–1100 MPa [22, 46], in other words, lower than metal posts (around 1400 MPa) but still much higher than dentin (200 MPa) [46]. It has also been suggested that the consequences of root fracture are more severe with metal posts than with fiber-reinforced composite posts [47]. In addition, the latter can be bonded to both root canal surface and resin-based restorative materials, which is not the case of their metallic counterparts. Hence, even if metal posts have been used for years in the clinics, the present chapter will only address the interest of using or not fiber posts in molar restoration.
7.8 Bonding in the Root Canal: The Worst-Case Scenario
Even in the event that a post is required (which as will be discussed below, does not seem to be clearly the case in molars), several aspects make its bonding procedure difficult.
First, it is not trivial to clean the root canal dentin and prepare it for bonding. Following endodontic treatment, obturation, and post space preparation, large areas of the root canal walls were indeed shown to be covered with smear layer, debris, and materials (sealer or gutta-percha) [48], which interfere with the post bonding efficiency. Since NaOCl was also demonstrated to decrease the bond strength [49], there may be an interest of neutralizing this effect by use of antioxidant such as sodium ascorbate [50, 51]. In Lai’s work, control of abundant rinse with water prior to bonding is lacking, while in Vongphan’s paper, there is no significant difference between control and when abundant water rinse is performed after NaOCl. Hence, it is still unclear whether or not this additional step is really beneficial.
Second, the ease of bonding procedure (etching, rinsing, primer application, drying, bonding application), resin-material injection, and photopolymerization is not as straightforward in the root canal space as in the coronal portion, which can result in lower bonding quality, more voids, or suboptimal resin polymerization [52].
Third, another major limitation of the bonding procedure in the root canal is related to the well-known polymerization shrinkage of resin-based composite, and the resulting stresses generated on the surrounding tooth structure. If the shrinkage stress exceeds the bond strength of the adhesive system to dentin, gaps form along the interface [52]. The magnitude of shrinkage stress is related to a parameter called “C-factor,” which refers to the ratio of the bonded surfaces to the unbonded ones [53]; the higher the C-factor, the greater is the shrinkage stress [54]. Significant bond strength reduction is already observed when increasing C-factor from 1 to 3 [55], and the C-factor values in root canals are expected to be much higher, since theoretically every dentin wall can be considered to have an opposing wall, and therefore very few surfaces are unbonded [52]. It is interesting to notice that the addition of a post as compared to filling the root canal with only resin results not only in a massive increase of C-factor, but also to a significant reduction of microtensile bond strength to root canal dentin (7.3–9.6 MPa with a post compared to 20.4–39.8 MPa without a post) while variations of resin volume by modifications of root canal width did not seem to affect bond strength [56].
Finally, higher bond strength values have been reported in coronal compared to apical dentin [57]. This questions the interest of preparing long post spaces, as compared to using only the coronal portion of the root canals, such as in the endocrown strategy, which will be described further.
All these limitations explain why bonding posts in the root canal is probably the worst-case scenario, with a particularly important risk of debonding and gap formation between post and root canal dentin, and low dentin bond strength. Additionally, there is concern of the stability of this little predictable bond with time, especially after repeated thermal, chemical, and mechanical stresses [58]. Indeed, Bouillaguet et al. [57] state that “clinical failure is not seen when sufficient coronal dentin is available because the restoration does not rely heavily on the bonding of the post to the root dentin.” This then logically questions the rationale of using posts to increase the restoration retention and/or reinforce the teeth.
7.8.1 Do Posts Reinforce Endodontically Treated Molars?
Based on in vitro studies, it is generally considered that the use of posts does not increase the fracture resistance of endodontically treated teeth [3], but these data are mostly based on metal post restorations, which do not bond to the dentin structure. Hence, it is worth revisiting this question with fiber-reinforced composite posts, and specifically regarding molar restoration.
Unlike for metal posts, in vitro data seem to highlight a possible strengthening effect of fiber posts on endodontically treated teeth. Again, a large majority of works addressing the use of posts to reinforce teeth included singe-rooted teeth. Let us consider those specifically focused on molars. In an in vitro work quoted earlier regarding the role of ferrule, a significantly higher fracture resistance was observed for teeth with posts (around 2900 N with ferrule, around 2000 N without ferrule and no significant difference between glass fiber and cast posts) than without posts (around 2000 N with ferrule, around 1500 N without ferrule).
Cast posts were associated with the highest rate of nonrestorable failures (80–100 %), whereas nonrestorable failures were reported in only 10–30 % of teeth with fiber posts or without posts (25° load direction) [43]. In another in vitro study, it was concluded that fiber post placement does not increase fracture resistance of endodontically treated mandibular molars with one or two remaining cavity walls in case of indirect composite overlay placement (fracture resistance around 1000 N for restored teeth after fatigue compared to 2992 N for intact teeth) [59]. However, they also observed that fiber post insertion could lead to more restorable fractures in case of extra axial loads (65 % nonrestorable fractures without post and 30 % with post) (45° load direction). Similar observations were again made when comparing different onlay materials (gold, composite, and ceramics) on MOD cavities with buccal and lingual cusp coverage, that is, fracture resistance ranging from about 1600 N (for ceramic and composite inlays) to 2900 N (for gold inlays), again well above physiological and parafunctional forces in all cases [60]. The effect of fiber post placement was not significant for composite or ceramic onlays, but well for gold onlays (about 2300 N without post and about 2900 N with post). Another study investigated direct composite restorations of root canal-treated molars with or without fiber posts, and reported fracture resistance ranging from 700 to 1600 N, depending on the number of remaining cavity walls [61]. They concluded that fracture resistance is not affected by the presence of fiber posts, but depends mostly on the number of residual walls, with a significant reduction of fracture resistance observed with less than two remaining walls. A higher proportion of nonrestorable failure was observed for restorations with fiber posts (0–50 %) than without (40–70 %). Another study by the same group investigated fracture resistance of root canal-treated molars restored with zirconia crowns, with different degrees of coronal tissue loss. They reported a significant improvement in fracture resistance with fiber posts (average ranging from about 1200 to 1450 N, with 20–33.3 % of nonrestorable fractures) compared to without posts (average ranging from about 1150 to 1250 N, with 6.7–20 % of nonrestorable fractures) [62].
In summary, based on in vitro studies, there is no consensus on the effect of fiber posts on endodontically treated molars, since some of them support a reinforcement and others do not. The common finding of all these in vitro data points is that failure occurs above normal intraoral forces, or even parafunctional forces which have a range from 700 to 1000 N in the posterior mandible. Hence, it is questionable whether or not the differences observed well above physiological forces, as well as the conclusions regarding restorability after failure, are in any way related to the clinical reality. All the conditions might very well be equivalent under physiological forces.
Considering clinical data, a meta-analysis on the subject concluded that the use of post retention had no significant influence on tooth survival after endodontic treatment, and a substantial heterogeneity among the included studies was deplored [7]. By contrast, a prospective study on tooth survival by the same group reported that teeth with cast post-and-core restorations were 2.6 times more likely to be extracted [1]. Since almost 90 % of the extracted teeth with cast post and core were premolars and molars, they concluded that the use of such retention systems should better be avoided in posterior teeth, and replaced by alternative treatment options [1]. They also reported that despite the large number of teeth included (1,617 teeth), the statistical power was not sufficient to test the interaction between factors, notably tooth type or post and core material, due to the small number of failures. The lack of consideration of tooth type in the majority of the clinical studies on endodontically treated teeth survival is a major limitation to determine whether or not the placement of posts participate in the reinforcement of endodontically treated molars specifically. As pointed out earlier [3], more clinical studies taking into account tooth type are required to determine whether or not a post should be used.
Among the few studies including molars, two reported no influence of post placement on restoration survival, one comparing at 5 years between cast post and core, direct post and composite core restoration and post-free all-composite core restorations [42], and the other direct composite resin-core-crown reconstructions with or without prefabricated metal posts [63]. However, the use of metal posts with composites is not an appropriate association, as mentioned earlier, and molars represented only 20–25 % of the teeth in both studies.
Several other studies investigating fiber posts included molars, but all were lacking appropriate controls, that is, molars with comparable tissue loss and without fiber post were not included. For example, Mancebo et al. evaluated the survival of root-treated teeth restored with fiber post and composite core covered by a crown, but molars represented only 18 % of the teeth included, only 3/14 failures, and most importantly no control without posts were investigated [41]. Another retrospective study evaluated the long-term performance of three types of fiber posts after a service period of 7–11 years. Almost 1,000 posts were in the study, with a total of 79 failures, 39 for endodontic reasons and 40 actual restoration failures. It was concluded that fiber posts “may be used routinely for restoring endodontically treated teeth” [64]. The evidence provided is again insufficient to determine if fiber posts should be used, since again no control without posts were considered, and only about 20 % of the teeth were molars, which represented only 13 of the 40 restoration failures, all due either to post debonding or to crown dislodgement.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


