Introduction
Flared and elongated incisors are associated with different types of periodontal bone defects, usually horizontal. Combined orthodontic-periodontal treatment is being used in periodontal patients with anterior displacement of the incisors. The purpose of this study was to investigate the changes in periodontal health and the shape of bone defects in the incisors after such combined treatment.
Methods
Fourteen adults were included in the study. In total, 56 elongated maxillary incisors with horizontal bone defects received orthodontic-periodontal treatment with circumferential supracrestal fibrotomy. To improve bone morphology, periodontal regenerative surgery and guided tissue regeneration were performed on the anterior teeth with angular bone defects after orthodontic treatment. Cone-beam computed tomography scans were taken before treatment (T0), at the end of the orthodontic intrusion (T1), and 6 months after the guided tissue regeneration surgery (T2). Probing pocket depth and clinical attachment loss were examined at T0, T1, and T2. The data were analyzed using paired t tests.
Results
From T0 to T1, clinical attachment loss decreased significantly by 0.29 mm ( P <0.05). The distance from the cementoenamel junction to the marginal bone crest decreased by 0.66 mm ( P <0.05). The labial side of alveolar bone thickness increased by 0.54 mm ( P <0.05), and the lingual side of alveolar bone thickness decreased by 0.46 mm ( P <0.05). The shape of the bone defect was changed from horizontal to vertical on some teeth. From T1 to T2, both probing pocket depth and clinical attachment loss improved significantly, and the radiographic examinations showed bone redepositions of 2.15 ± 0.68 mm ( P <0.05) vertically and 1.44 ± 0.92 mm ( P <0.05) horizontally. The distance from the most apical point of the bone defect to the cementoenamel junction after combined treatment decreased by 2.11 ± 1.30 mm ( P <0.05).
Conclusions
Combined orthodontic-periodontal treatment improved the periodontal conditions of the defective bone sites. Bone morphology, altered by orthodontic intrusion with fibrotomy, can improve the results of subsequent guided tissue regeneration.
Highlights
- •
An adult patient with bone loss was treated with a team approach.
- •
Orthodontic treatment and guided tissue regeneration improved the periodontal support.
- •
Changes in bone morphology were obtained with circumferential supracrestal fibrotomy.
Periodontitis is a common disease in patients visiting the dental clinic. Periodontal disease leads to the loss of supporting structures. When the supporting structures that maintain the physiologic tooth position are disturbed by periodontal disease, patients can have pathologic tooth migration, such as proclination, diastema, rotation, extrusion, and drifting. Periodontitis with anteriorly displaced incisors not only causes premature contact of occlusion, but also accelerates the loss of periodontal supporting structures and negatively affects dental esthetics. In the treatment of these patients, orthodontic movement is often required.
Periodontal regeneration can be described as de novo cementogenesis, osteogenesis, and regeneration of newly formed fibers in both newly formed cementum and alveolar bone. With adequate orthodontic-periodontal coordination, it is possible to reestablish a healthy and functional dentition. Orthodontic tooth movement is a process of occlusive reconstruction with alveolar bone remodeling and bone morphology changes. The bone loss during intrusion of teeth, inducing enlargement of the periodontal ligament space at the cervical area or deepening of the periodontal pockets, is attributable to displacement of junctional epithelium that would require resorption of marginal bone to preserve the periodontal width.
Meanwhile, circumferential supracrestal fibrotomy therapy often reduces relapse in rotated teeth. In recent years, it has been reported that orthodontic intrusion with circumferential supracrestal fibrotomy is an effective treatment for extrusion of anterior teeth. The circumferential supracrestal fibrotomy surgery controls the resorption of marginal bone after tooth intrusion, reducing the marginal bone loss. It may cause creation of a cone-shaped bone defect with the intrusion, so that the horizontal bone defect can be changed to angular. Clinically, periodontitis patients often have alveolar bone loss with 2 patterns: horizontal and vertical (angular). In angular bone loss, the resorption for one tooth sharing the septum is greater than that of the other tooth. Infrabony pockets, where the base of the pocket is apical to the alveolar crest, are associated with angular bone loss. Horizontal bone loss is the more common type of alveolar bone resorption. Bone is lost equally from the surfaces of 2 adjacent teeth, with the interproximal bone level remaining flat, and the deepest portion of the pocket located coronal to the alveolar crest.
It remains controversial whether orthodontic treatment can achieve new attachment. Both guided tissue regeneration and grafting procedures are means of achieving periodontal regeneration. However, flaring and elongated incisors usually have horizontal bone defects, which are not suitable for periodontal regenerative procedures. If the morphology of a bone defect can be changed from horizontal to angular by orthodontic treatment, guided tissue regeneration will enhance periodontal tissue improvement and long-term stability.
The purpose of this study was to evaluate the efficacy of a clinical protocol involving combined orthodontic-periodontal treatment to achieve periodontal regeneration.
Material and methods
In this study, 14 patients diagnosed with chronic periodontitis (11 women, 3 men), aged 22 to 41 years, were included in the treatment. This study was approved by the biomedical ethics committee of Peking University. All subjects signed an informed consent form before participating in the study.
The inclusion criteria were (1) no systemic disease; (2) good general health, with the women not pregnant or lactating; (3) nonsmoking status; (4) periodontal disease previously treated by scaling and root planing, and oral hygiene instructions; (5) good oral hygiene with full-mouth plaque score ≤15% and full-mouth bleeding score <25% at baseline (T0); (6) migration and extrusion of maxillary anterior teeth caused by periodontal disease; (7) panoramic radiographs showing that the shapes of the bone defects were horizontal; and (8) a need for orthodontic treatment.
The treatment procedures were the following.
- 1.
Initial periodontal therapy. Therapy consisted of scaling, root planing, and oral hygiene instructions before orthodontic treatment. Patients were treated periodontally until the inflammation was resolved through control of bacterial biofilm and oral hygiene maintenance (full-mouth plaque score, ≤15%; full-mouth bleeding score, <25%).
- 2.
The conventional circumferential supracrestal fibrotomy technique consists of inserting a surgical blade into the gingival sulcus and severing the epithelial attachment surrounding the involved teeth. The blade also transects the transeptal fibers by interdentally entering the periodontal ligament space. All circumferential supracrestal fibrotomy surgeries were performed by the same periodontist (L.X.) during intrusive movement of the incisors once per month. At the same time, root planing was performed to prevent the formation of inflammatory granulation tissue around periodontal space.
- 3.
For the orthodontic treatment, fixed appliances were placed on the maxillary incisors and first molars as anchorage. The patients were treated with an intrusive mechanism with a utility arch technique, made of 0.017 × 0.025-in beta-titanium alloy wire to intrude and realign the migrated incisors and to obtain space closure ( Fig 1 ); the appliances were loaded immediately after the first circumferential supracrestal fibrotomy. The forces used were light, 10 to 15 g per tooth, depending on the amount of residual periodontal support. After intrusion, the teeth other than the incisors and first molars were bonded to align and level the arch. During this period, the orthodontic appliance was adjusted every 4 weeks, and professional prophylaxis was performed at 3-month intervals. The active orthodontic treatments were continued for an average of 19 months. Thereafter, the fixed orthodontic appliances remained in the mouth until the guided tissue regeneration surgery.
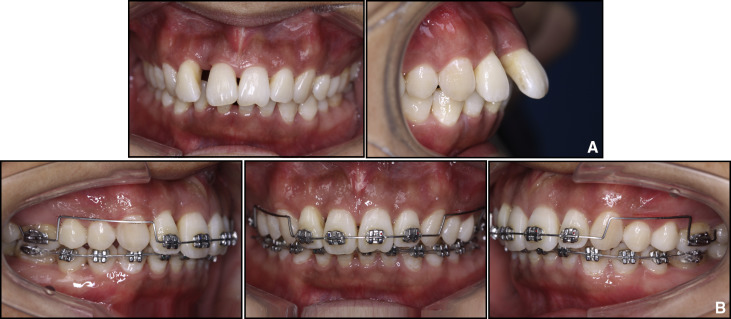
Fig 1 Intraoral images before and after orthodontic intrusion with circumferential supracrestal fibrotomy: A, frontal and lateral views of extruded anterior teeth after periodontal treatment; B, utility arch used to intrude and retract incisors. - 4.
Patients who had an angular bone defect around the maxillary incisors were included to receive guided tissue regeneration surgery. All teeth received periodontal regenerative surgery by the same periodontist.
- 5.
At the end of treatment, all patients received a resin-bonded splint on their lingual anterior teeth for retention.
To evaluate the changes in alveolar bone during maxillary incisor retraction, cone-beam computed tomography (CBCT) images were taken at T0, after orthodontic intrusion (T1), and 6 months after the guided tissue regeneration surgery (T2), which was undertaken in the same manner with the same machine (3D Accuitomo XYZ Slice View Tomograph; Morita, Tokyo, Japan). Exposure parameters were 60 kV, 3-5.5 mA based on patient size, and volume of 40 × 30 mm with a full 17-second scan rotation. Only the maxillary incisors were included in 1 imaged volume to decrease the radiation. The CBCT scans were taken for treatment purposes. The surgical procedure of guided tissue regeneration has strict indications. For the guided tissue regeneration treatment, we must obtain detailed information regarding the shape of the alveolar bone defect. CBCT images can provide better diagnostic and quantitative information than conventional radiography on periodontal bone levels in 3 dimensions.
Primary data reconstructions were performed using the acquisition software (i-Dixel) on the Accuitomo workstation, which provides axial, frontal, and sagittal views. Secondary reconstruction was then performed using the i-Dixel software to obtain a slice thickness and an interval of 1.0 mm.
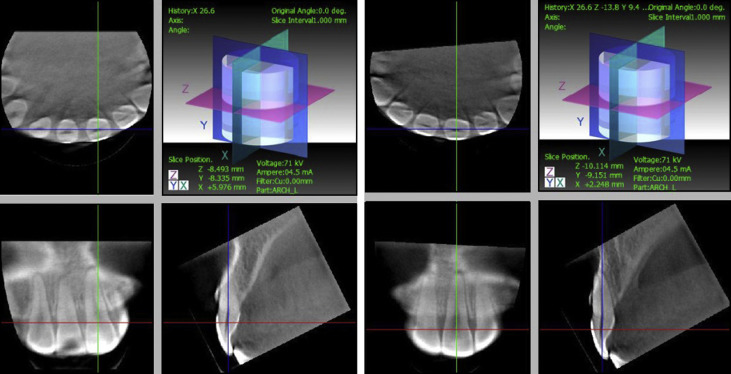
Reconstructions were completed so that the long axis of the tooth became parallel to the axes of 2 perpendicular, vertical image planes ( Fig 2 ). This provided optimal visualization of the tooth in the axial, coronal, and sagittal planes.
For the periodontal index examination, at T0 and T1, probing pocket depth and clinical attachment loss were determined with a williams probe (in millimeters) on each maxillary incisor. At T1 and T2, probing pocket depths and clinical attachment losses were assessed on the teeth that received the guided tissue regeneration surgery.
For the bone morphology measurements from T0 to T1, the following measurements were made.
- 1.
Marginal bone loss was assessed by measuring the distance from the marginal bone crest to the cementoenamel junction. Labial and palatal bone levels were measured in the sagittal plane, and mesial and distal bone levels were measured in the coronal plane ( Fig 3 ).
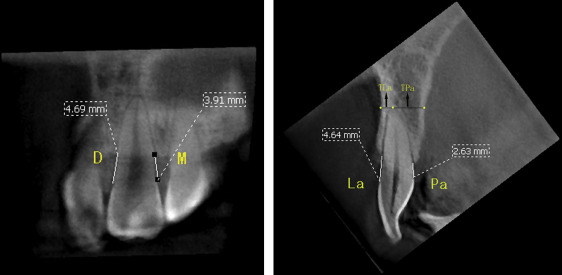
Fig 3 M , Mesial marginal bone level; D : distal marginal bone level; La , labial marginal bone level; Pa , palatal marginal bone level; TLa and TPa , thickness of the alveolar bone at the apical levels. - 2.
The labial, palatal, and total alveolar bone thicknesses were assessed at the apical level in the sagittal plane ( Fig 3 ).
- 3.
If orthodontic intrusion changed a horizontal bone defect into a deep and narrow defect, the bone defect angle was measured. The angle was defined by 2 lines: the first line was between the bottom of the bone defect and the most coronal extension of the interproximal bone crest, and the second line was the root surface. Labial and palatal bone defects were measured in the sagittal plane, and mesial and distal bone defects were measured in the coronal plane ( Fig 4 ).
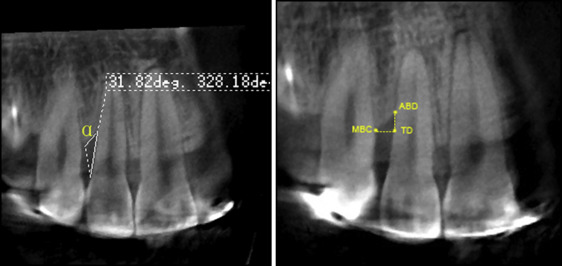
Fig 4 The bone defect angle ( α ) and infrabony defect measurement.
From T1 to T2, the changes of the infrabony defects after guided tissue regeneration were measured as follows. The vertical distance between the projection of the alveolar crest on the root surface and the most apical point of the bone defect, as well as the horizontal distance from the marginal bone crest and from the root surface, were assessed. Marginal bone loss on the infrabony defect site was assessed by the distance from the most apical point of the bone defect to the cementoenamel junction ( Fig 4 ).
For both the T0 to T1 and the T1 to T2 stages, the radiographs were evaluated twice. One observer (T.C.) performed all measurements at a 2-week interval. The average of the 2 measurements was calculated.
Statistical analysis
Pretreatment and posttreatment values of the parameters were compared. Statistical analyses were conducted using the Student t test for coupled data. P values <0.05 were considered statistically significant. The bone defect angle was recorded when changes in bone morphology were identified in the radiographic images.
Results
Table I shows the changes in periodontal health and shape in the alveolar bone, clinical attachment loss, and probing pocket depth from T0 to T1. There was a statistically significant improvement in clinical attachment loss with a 0.29-mm reduction, whereas probing pocket depth did not change significantly. For bone height, the marginal bone loss of the 4 surfaces decreased; the differences of 0.76, 0.73, 0.53, and 0.58 mm were all statistically significant. The mean marginal bone losses were 4.86 mm at T0 and 4.21 mm at T1; this difference was statistically significant. For bone thickness, the mean total alveolar bone thickness increased by 0.08 mm; this difference was not statistically significant. However, the labial thickness increased while the palatal thickness decreased significantly. For bone morphology, there were 17 angular bone defects in 14 teeth in 8 patients at the completion of the orthodontic treatment ( Fig 5 , A and B ). The 4 labial bone defect angles were 18.16°, 15.61°, 29.70°, and 15.79°. The 6 mesial bone defect angles were 25.11°, 31.89°, 34.38°, 26.88°, 36.38°, and 27.51°. The 7 distal bone defect angles were 24.80°, 39.74°, 30.93°, 31.75°, 20.70°, 20.13°, and 29.87°.
| Measurement (mm) | T0 | T1 | T1-T0 | t | P | |||
|---|---|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | Mean | SD | |||
| Mesial | 5.05 | 1.61 | 4.28 | 1.25 | −0.76 | 1.14 | −4.232 | <0.001 † |
| Distal | 5.42 | 1.70 | 4.69 | 1.45 | −0.73 | 0.84 | −5.547 | <0.001 † |
| Labial | 4.62 | 1.20 | 4.09 | 1.35 | −0.53 | 0.98 | −3.264 | 0.002 † |
| Palatal | 4.26 | 1.85 | 3.68 | 1.72 | −0.58 | 1.19 | −2.868 | 0.007 † |
| Mean | 4.86 | 1.65 | 4.21 | 1.48 | −0.66 | 1.04 | −7.786 | <0.001 † |
| TLa | 2.0 | 1.08 | 2.59 | 1.54 | 0.54 | 1.02 | 3.150 | 0.003 † |
| TPa | 5.67 | 1.65 | 5.21 | 1.81 | −0.46 | 1.22 | −2.221 | 0.033 ∗ |
| TLa + TPa | 7.72 | 1.38 | 7.81 | 1.53 | 0.08 | 0.91 | 0.537 | 0.595 |
| PPD | 2.75 | 0.92 | 2.68 | 0.80 | −0.07 | 0.75 | −1.03 | 0.304 |
| CAL | 3.39 | 1.47 | 3.10 | 1.16 | −0.29 | 0.17 | −2.97 | 0.004 † |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


