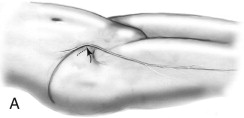
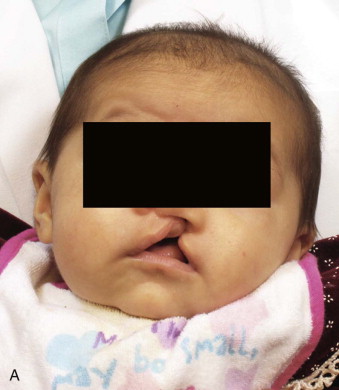
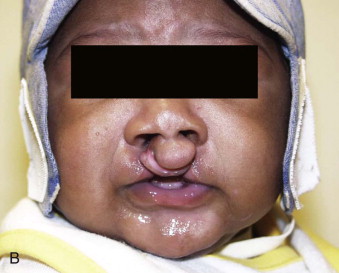
Cleft lip and palate deformities are the second most frequently occurring congenital anomalies. In both the unilateral and bilateral complete cleft lip and palate deformity, there is a bony deficiency of the maxilla. The degree of hypoplasia of the maxilla is usually proportionate to the severity of the cleft lip deformity. In the incomplete cleft lip patient, there is usually minimal or no deformity of the maxilla. This is in contrast to the typical cleft lip and palate patient with maxillary alveolar bone involvement. In the unilateral complete cleft, there are varying degrees of hypoplasia of the maxilla on the cleft side, usually associated with a malpositioned maxillary segment and an absent or malformed lateral incisor ( Fig. 87-1, A ). In the bilateral cleft patient, the bony maxillary deformity is usually symmetrical and relative to the position of the premaxilla ( Fig. 87-1, B ). Clefts of the alveolar process of the maxilla inhibit the eruption and maintenance of the permanent dentition and can affect facial growth and symmetry. The key to treatment of cleft lip and palate patients with maxillary deformities is early diagnosis of the skeletal and dental involvement and combined surgical and orthodontic care.
Alveolar Clefts
Early Treatment
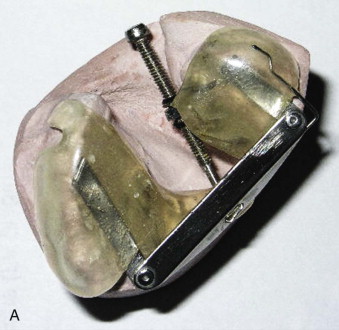
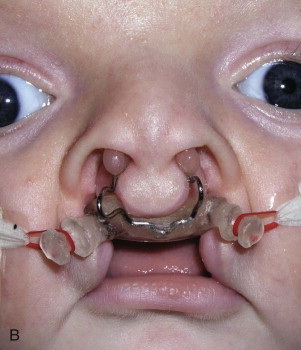
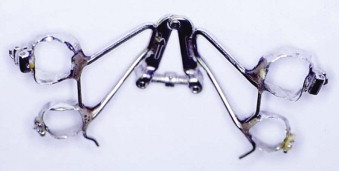
Early management of the cleft patient with a maxillary deformity will often involve presurgical orthopedics to realign the maxillary segments. Alignment of the maxillary segments will allow easier repair of the cleft lip and nasal deformity. Either active traction devices, such as the Latham pinned appliance ( Fig. 87-2, A ), or passive molding appliances ( Fig. 87-2, B ) can be used. Presurgical orthopedics is often initiated within the first few months of life to promote alignment of the maxillary segments prior to closure of the cleft lip. If the alveolar segments are brought to within 2 mm of each other, some cleft surgeons will advocate performing a gingivoperiosteoplasty as part of the primary lip and palate repair. This procedure can result in bony bridging across the alveolar cleft and obviate the need for delayed secondary alveolar bone grafting, but it is still controversial whether this may also result in decreased maxillary growth.
Early primary grafting of the alveolar cleft defect with rib grafts, performed at the time of initial lip repair, was initially thought to be beneficial in that it might correct the alveolar defect early and minimize the extent of the maxillary deformity. Unfortunately, this “early”-phase bone grafting has been associated with reports of moderate to severe long-term maxillary growth restriction.
Delayed Treatment (Mixed Dentition Phase)
Delayed secondary bone grafting in the mixed dentition phase (between 7 and 10 years of age) after initial cleft lip and palate closure is considered the more accepted time period for bone grafting of alveolar defects. Bone grafting should be completed prior to eruption of the permanent canine through the cleft site so that appropriate support for the erupting teeth around the cleft is present. In addition to providing support for the erupting teeth, the bone graft will also provide additional support for the alar base and pyriform aperture as well as minimize perialveolar fistula development. Delaying the bone grafting until the mixed dentition phase allows for increased maxillary growth in both the transverse and horizontal planes. Numerous studies have demonstrated the advantages of delayed secondary alveolar bone grafting both from an occlusal and periodontal standpoint.
Treatment Considerations
Orthodontic/Dental Treatment
In the mixed dentition phase the goal of orthodontic care is to align the maxillary arch in preparation for the bone graft. This usually involves expansion of the arch in a transverse diameter and results in opening up the alveolar cleft to some degree. A lingual expansion device, such as a quadhelix, is most often used ( Fig. 87-3 ). Meticulous dental care addresses treatment of any periodontal disease and/or extraction of any aberrant teeth to prepare the cleft site for bone grafting. Significant periodontal disease at the time of bone grafting can result in postoperative infection, further resulting in loss of the graft.
Surgical Technique for Bone Grafting
Several donor sites are available for obtaining bone for grafting into the alveolar cleft, including rib, cranial bone, mandibular symphysis, and iliac crest. The iliac crest is the most widely used for harvesting cancellous bone, which has been shown to have the greatest viability when grafted into alveolar cleft defects. The iliac crest also has adequate volume to harvest for either a unilateral or bilateral alveolar cleft. The cranium can also provide adequate bone for an alveolar cleft and can be readily harvested with the use of a Hudson brace. The mandibular symphysis can provide adequate bone for grafting but usually only in small amounts.
The authors’ choice is to use cancellous bone from the iliac crest. Iliac crest cancellous bone can be harvested either by splitting the cartilaginous cap and removing the cancellous bone with curettes or by using a bone harvester ( Figs. 87-4 and 87-5 ). Once adequate bone is harvested, the alveolar cleft site is prepared for grafting. Complete exposure of the alveolar cleft deformity, whether unilateral or bilateral, is obtained by elevation of labial and palatal flaps. Separation of the nasal and oral mucosa is necessary so that the nasal lining can be closed. Once the nasal lining has been completely closed, the cancellous bone can be packed into the entire cleft defect. The labial and palatal flaps can then be advanced and closed over the bone graft ( Fig. 87-6 ). The elevation of the labial and palatal flaps is the most difficult part of the surgical procedure and requires meticulous dissection, because there is often previously scarred and somewhat friable tissue along the cleft.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses