Facial resurfacing has been used as a modality of therapy as far back as 1500 bc when it was practiced by the ancient Egyptians. It has evolved through chemical and abrasive techniques to include different laser technologies. Technical advancements have heralded improved results with less morbidity, which has led to a great surge in the popularity of facial resurfacing. As a surgical treatment, ablative facial resurfacing will be the focus of this chapter. It primarily includes dermabrasion, chemical peeling, and laser resurfacing. The primary focus of treatments will be on the most common dermatopathologic entities that can be improved by resurfacing. Finally, a brief review of potential complications and their prevention will be presented.
Etiopathogenesis/Causative Factors
The primary causative factors for which patients seek facial resurfacing include intrinsic age-related and extrinsic environmentally associated changes which cause dyspigmentation, dyskeratosis, and cutis laxa. Additionally, facial resurfacing is commonly sought for the treatment of facial scars, including acne scarring. Resurfacing has also been used for many dermatopathologic entities, such as keloids, rhinophyma, xanthelasma, seborrheic keratosis, and actinic keratosis.
As patients age , intrinsic changes result in the epidermis becoming more fragile with weaker cell adhesion and a thinner stratum corneum. Deeper dermal changes include flattening of the papillary dermis, decreased number of appendages and sensory organs, and decreased vascularity. Age-related degradation and disorganization in elastin and collagen and decreased ground substance lead to less resilient skin that is more lax and prone to rhytidosis. These changes are compounded in women after menopause with the depletion of estrogenic support (1) This all contributes to decreased water content, which results in increased surface roughness and xerosis. Senile decrease in melanocytes and dysfunction of these cells give rise to areas of uneven color. Additionally, as women cycle through hormonal exposure, including pregnancy, birth control, and hormone replacement therapy, melanocytes can be stimulated to produce more melanin when exposed to the sun, This results in areas of hyperpigmentation.
In regards to extrinsic factors, as sun exposure occurs, the ultraviolet (UV) radiation associated damage accumulates. Interestingly, up to 50% of a person’s exposure to UV radiation occurs before the age of 18. Repeated sun exposure causes cellular abnormality and decreased healing ability. The pathognomonic changes include accentuation of elastotic changes in the upper dermis. Basically, sun exposure accelerates intrinsic aging.
Finally, with regard to scarring, up to 95% of patients with acne will have some extent of scarring. This is due to inflammation and necrosis of the pilosebaceous unit, which can cause “ice pick” type scars. Alternatively, wider-spread inflammation in the subcuticular layer can result in more diffuse fat necrosis and larger crater-like defects.
Pathologic Anatomy
Among its other functions, the skin serves as a barrier to insult from the harsh external environment. The skin is divided microscopically into different layers based on its cellular content. The epidermis is the “superficial” layer of the skin and includes a layer of continuously regenerating squamous epithelial cells. Additionally, this layer contains melanocytes, which are responsible for pigmentation; Langerhans cells, which are responsible for macrophage activity; and Merkel cells, which have sensory function. Thus, this layer is largely responsible for the color and texture of the skin. It has no collagen fibers and little inherent strength.
Underneath the epidermis is the dermis with its more superficial papillary layer and deeper reticular layer. The papillary layer is loosely arranged with a vascular arcade. The reticular layer forms the bulk of the dermis with its interlacing collagen and elastic fibers. The main cell of the dermis is the fibroblast, which produces the ground substance and the collagen and elastin. The dermis serves to support and provide nourishment to the epidermis.
Finally, underneath the dermis is loose subcutaneous tissue that contains adipose tissue and larger vessels. Most of the adnexal structures, including hair follicles and sweat glands, originate from this layer ( Fig. 109-1 ).
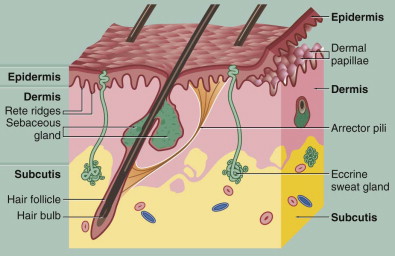
Pathologic Anatomy
Among its other functions, the skin serves as a barrier to insult from the harsh external environment. The skin is divided microscopically into different layers based on its cellular content. The epidermis is the “superficial” layer of the skin and includes a layer of continuously regenerating squamous epithelial cells. Additionally, this layer contains melanocytes, which are responsible for pigmentation; Langerhans cells, which are responsible for macrophage activity; and Merkel cells, which have sensory function. Thus, this layer is largely responsible for the color and texture of the skin. It has no collagen fibers and little inherent strength.
Underneath the epidermis is the dermis with its more superficial papillary layer and deeper reticular layer. The papillary layer is loosely arranged with a vascular arcade. The reticular layer forms the bulk of the dermis with its interlacing collagen and elastic fibers. The main cell of the dermis is the fibroblast, which produces the ground substance and the collagen and elastin. The dermis serves to support and provide nourishment to the epidermis.
Finally, underneath the dermis is loose subcutaneous tissue that contains adipose tissue and larger vessels. Most of the adnexal structures, including hair follicles and sweat glands, originate from this layer ( Fig. 109-1 ).
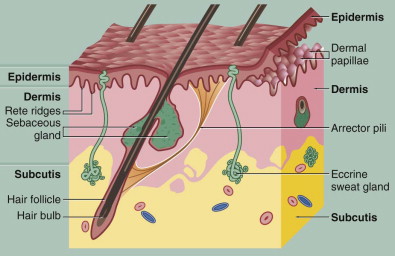
Diagnostic Studies
A good subjective history, including the goals of the patient, and the physical examination are perhaps the most important diagnostic resources. Besides determining how realistic the patient’s goals are, other important subjective history includes the patient’s sun exposure history, skin care regimen, co-morbid conditions, medication history, and skin cancer history.
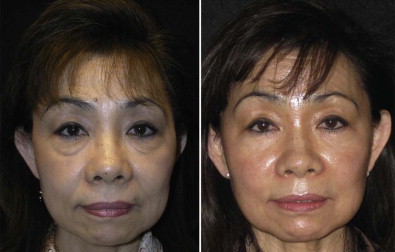
Evaluation of the skin includes complexion, texture, thickness, oiliness, and degree of photoaging, specfically the severity of rhytidosis and laxity. The Fitzpatrick and Glogau classifications are very useful for guidance toward these ends. Matching the patient’s skin type and complexion with the appropriate treatment will maximize the resurfacing effect while minimizing postoperative complications. The Fitzpatrick classification system ranks the skin’s tendency to tan or burn in association with the patient’s skin, hair, and eye color. This is illustrated in Table 109-1 . Patients in classes I to III with more sun-reactive skin types tend to have better results than darker skinned patients. These patients have lighter hair, eye, and/or skin color and usually burn easier when exposed to the sun. They have a lower incidence of post-treatment hyperpigmentation but a higher incidence of post-treatment hypopigmentation. They will also be prone to premature skin aging without proper UV protection. Patients with a type IV or greater complexion are at higher risk for unfavorable post laser pigmentary changes and may be more suitable candidates for non-ablative techniques. Patients with darker skin types who desire resurfacing first require a test spot behind the ear or in an inconspicuous area to evaluate the results. Even normal healing here does not guarantee the final overall skin response. The transitional patients may require multiple less aggressive treatments to obtain the same endpoint goal as the Asian patient in Fig. 109-2 . Luckily, the darker patients rarely seek resurfacing treatment because their skin is more resistant to photoaging. Although the Fitzpatrick classification is useful, probably the simplest criterion for judging the patient’s skin type is its response to sun exposure.
| SKIN TYPE | HAIR | EYE | SKIN | RESPONSE TO ULTRAVIOLET LIGHT EXPOSURE |
|---|---|---|---|---|
| I | Red | Green | Fair | Always burns |
| II | Blond | Blue | Fair | Burns with some tans |
| III | Brown | Brown | Medium | Tans with some burns |
| IV | Dark brown | Brown | Medium dark | Tans easily, rarely burns |
| V | Black | Black | Dark | Tans easily, vary rarely burns |
| VI | Black | Black | Black | Does not burn |
The degree of degenerative changes in the dermis and epidermis and the severity of photoaging are ranked to classify and guide treatment decisions in the Glogau classification scheme. This is shown in Table 109-2 . Patients classified as types III and IV are the best candidates for ablation with their marked dyspigmentation and dyskeratosis. These patients have the greatest margin for improvement but should be warned that moderate to severe skin laxity requires a lifting procedure for correction.
| SKIN TYPE | PHOTOAGING | CHANGES IN PIGMENTATION | PATHOLOGY | WRINKLES | AGE |
|---|---|---|---|---|---|
| I | Early | Mild | None | Minimal | 20-35 |
| II | Moderate | Senile lentigines | Non-visible dyskeratosis | Dynamic | 35-45 |
| III | Advanced | Marked dyschromia | Visible dyskeratosis, telangiectasia | Static | 50s |
| III | Senile | Yellow-gray | Actinic keratosis ± malignancy | Severe | 60s |
An alternative part of the diagnostic phase of treatment of these patients is recognizing which patients are not good candidates for these procedures. Such patients include those with collagen vascular diseases and those who are immunosuppressed. In addition, patients with compromised integrity of the adnexal structures, including those with a history of isotretinoin (Accutane) use within the last 6 months, those with a history of facial irradiation, and patients with burn scars, are not good candidates. Some relative contraindications include patients with multiple co-morbid conditions or poorly controlled health issues and those taking anticoagulation medications.
Resurfacing can cause activation of preexisting dermatopathologic entities such as eczema, rosacea, or atopic dermatitis. Caution is warranted in patients prone to hypertrophic or keloid scarring. Patients who have previously undergone facial surgery, including lower eyelid blepharoplasty, may also be poor candidates for resurfacing. These patients may be at increased risk for ectropion. As mentioned previously, darkly complected patients should be warned regarding their increased risk for postoperative hyperpigmentation or hypopigmentation. Of course, patients with a tendency toward body dysmorphia or secondary gain or those with unrealistic expectations should not be acceptable candidates for any cosmetic surgery. Finally, skin pathology suspicious for malignant changes should undergo biopsy and be treated before resurfacing.
Treatment/Reconstructive Goals
Goals of treatment include rejuvenated skin with less dyskeratosis, rhytidosis, and dyschromia. In addition, with regard to scarring, goals include lightening and reduction of the scarring. It is common to achieve only 50% improvement with ablative resurfacing when treating moderate to severe acne scarring. Another goal should be avoidance of complications through proper patient evaluation and selection of treatment.
Specific Treatment and Techniques
Pretreatment Conditioning
Although there is some controversy regarding the necessity for pre-treating skin, most practitioners would agree that pre-treatment with tretinoin and a bleaching agent speeds re-epithelialization and decreases the incidence of postoperative hyperpigmentation. Tretinoin, which is retinoic acid, acts by decreasing cellular adhesiveness and increasing cell turnover to restore normal epidermal thickness. The thinning of the stratum corneum allows better penetration of the resurfacing agent. Tretinoin also encourages collagen synthesis. Patients with thicker oilier skin tolerate and benefit from retinoic acid to a greater degree. Patients with thin atrophic skin may experience more dehydration and irritation. When patients cannot tolerate tretinoin, daily application of glycolic acid or weekly alpha-hydroxyl acid peels for 4 to 6 weeks can be substituted.
Hydroquinone and kojic acid are bleaching agents that stabilize melanocytes and reduce dyspigmentation before laser treatment. They also decrease the risk for postoperative inflammatory hyperpigmentation. The mechanism of action includes inhibition of tyrosinase, which decreases melanin formation and increases melanin degradation. This is especially useful in patients with darker skin types.
Retinoic acid and hydroquinone have a synergistic effect on each other in that retinoic acid increases penetration of the hydroquinone and also works to suppress melanocyte metabolism. To be most effective, the bleaching agent should be applied twice daily and retinoic acid applied at bedtime. A mild steroid can be prescribed initially with the tretinoin to attenuate the irritation that the skin undergoes during the 2- to 4-week acclimation period. Additionally, patients can apply tretinoin every other day instead of every day until the dermatitis period resolves. Patients should use a sun block in the morning, including a moisturizer, preferably with UVA and UVB protection. The minimal amount of time necessary for patients to maximize the conditioning is typically 4 to 6 weeks because the epidermal cell cycle extends roughly this long.
Preoperative Medications
In the more immediate pretreatment period, patients require additional preparation. Ablative facial resurfacing typically necessitates some form of anesthesia, and thus patients require the appropriate pre-anesthesia instructions for sedation or general anesthesia as per recommendations of the American Society of Anesthesiology. Patients are asked to wash with an antimicrobial cleanser such as Hibiclens the night before and also the morning of the treatment. In a further attempt to reduce microbial load, the patient is given a preoperative dose of appropriate antibiotics, which is continued for 5-7 days postoperatively. Many studies have suggested benefit of antibiotic prophylaxis. This should especially be a consideration when an occlusive dressing is used.
Prophylactic administration of a nucleoside analogue antiviral has been demonstrated to prevent outbreaks and decrease the duration and severity of postoperative herpes simplex virus. infection. Up to 70% of patients without a previous history have a positive titer. The incidence of outbreaks in patients without a previous history has been shown to be as high as 10% in untreated patients undergoing resurfacing and 50% in those with a positive history. The antiviral should be started the day before and continued postoperatively until the skin is reepithelialized, usually in 10 to 14 days, depending on the depth of resurfacing. The antiviral inhibits viral replication only in intact epidermal cells, and thus the drug must be at a therapeutic level before the skin begins to reepithelialize. Some recommend prophylactic antifungal coverage, but studies have not found the incidence of post-resurfacing fungal infections to be high enough to warrant this additional therapeutic measure.
Dermabrasion
Dermabrasion is thought by many to be the most effective mode of treatment of facial scars, including acne and the post-traumatic variety. It is also very popular for the treatment of perioral rhytides and rhinophyma ( Fig. 109-3 ). It can be used for treating appropriate dermatopathologic conditions located from a superficial level to a mid-reticular level. Originally described by the Egyptians and performed with sandpaper, modern techniques have evolved through a wire brush to what is probably most commonly used today, a diamond fraise.
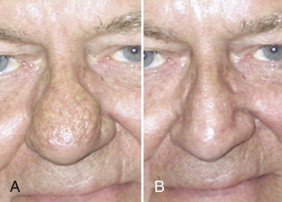
Dermabrasion is performed with a hand piece that rotates up to the 35,000-rpm range and has a variety of shapes, sizes, and coarseness of fraise tips. The procedure is usually done with the patient under sedation or general anesthesia, including tumescent or cryogenic preparation. The latter technique increases the rigidity of the tissue and control of the resurfacing. Increasing the rigidity of the surface allows more even abrasion and decreases “grabbing” of the skin by the fraise or brush. Hanke and associates recommend avoiding lowering the skin temperature below −30° C because this increases the risk for tissue necrosis.
A diamond fraise is a better selection for neophytes since it offers a larger margin of safety and is not as aggressive as the brush. The different shapes are very useful for the different contours of the face. Brushes are capable of more efficient removal of skin but have a greater tendency to “run” on the skin. They require a greater level of expertise.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


