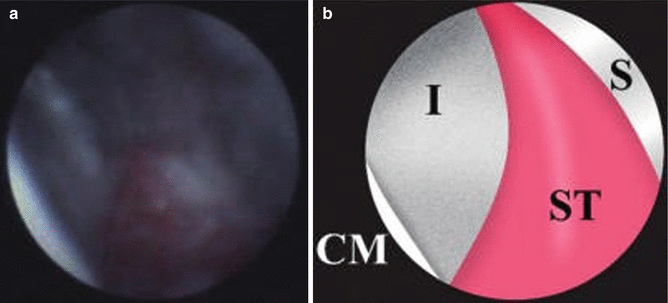
Fig. 2.1
(a, b) These two examples show residual excess cement and how it relates to the destruction of the implant-supporting tissues. Is it possible that the cement behavior was active in this process, or did it simply occur because the cement presented an overhang of material?
The Science and Studies—Microbial Interaction: T.G. Wilson’s Study on the Clinical Relationship Between Residual Excess Cement and Peri-implant Disease
By definition, peri-implant diseases are inflammatory in nature. Many of the same pathogenic bacteria associated with periodontal diseases are also associated with peri-implant disease. Several case reports found these inflammatory lesions (peri-implant mucositis and periimplantitis) were associated with residual cement.
A prospective inception cohort study on the relationship of excess cement to peri-implant disease was published in 2009. A dental endoscope was employed to view the subgingival peri-implant space. Inflammation around fixtures was often found associated with dental cement adhering to the implant superstructure or to the fixture its superstructure.
Individuals presenting with clinical signs of peri-implant mucositis (bleeding upon probing, color change) had the peri-implant space debrided and their oral hygiene reinforced and were instructed to irrigate the affected area with chlorhexidine 0.12 % twice daily for 30 days. If bleeding or other signs of clinical inflammation were still present 30 days later, the patient was entered into the study. Patients who presented with suppuration, had increased probing depths, or had radiographic evidence of continued bone loss were entered directly into the study. Thirty-nine consecutive patients with 42 implants were entered. Twelve of these patients had 20 similar implants that had no signs of peri-implant disease. These last implants served as controls. All test and control implants had received cemented single-unit fixed partial dentures. Both groups had the subgingival peri-implant site explored using a dental endoscope (Fig. 2.2a, b).
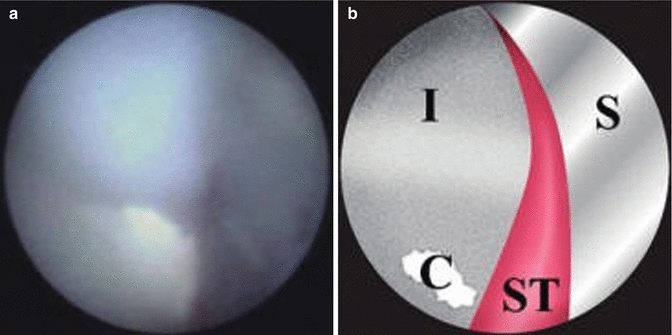

Fig. 2.2
(a) A piece of cement, 0.5 mm in diameter, attached to the implant surface is seen in the lower left quadrant of the screen grab from the endoscope. (b) An illustration of A. I implant, S shield, C cement, ST soft tissue (Reproduced with permission from the American Academy of Periodontology: Wilson (2009))
The presence or absence of materials adherent to the implant itself, the crown, and any material visualized in the surrounding soft tissues was recorded. This generation of endoscope dental cement has a brilliant white reflectivity; calculus is dull brown and biofilm gray/blue. Biofilm can be easily removed with the tip of the endoscopic explorer. Removal of any adherent material was accomplished using the scope for visualization and combinations of hand and/or mechanical methods until no further material could be visualized. The endoscope explorer was then rotated 180°, and any materials visualized in the soft tissues were removed, if possible (Fig. 2.3a, b).
Cement was found on 81 % of the test implants and on none of the control fixtures. At the 1-month evaluation, after removal of foreign matter, 76 % of the clinical and endoscopic signs of inflammation around the test implants had resolved. Three of the test implants required surgical entries to resolve the inflammatory process. Studies of biopsies from these three cases, as well as a number of additional cases, are currently underway.
One of the most disturbing aspects of this data was that the earliest signs of peri-implant disease did not appear until 4 months after cementation, while the longest was 9 1/2 years after placement (Fig. 2.4). The findings of this study have been duplicated by others.
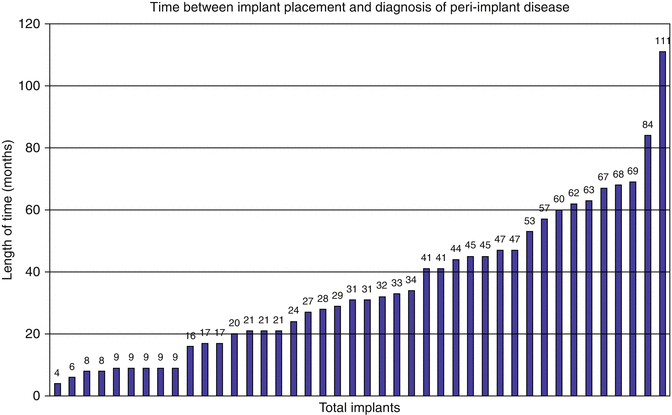

Fig. 2.4
The presence of peri-implant disease was discovered as soon as 4 months after cementing the fixed partial denture and as long as 111 months. Each bar represents an individual implant (Mean 2.93 years) (Reproduced with permission from the American Academy of Periodontology: Wilson (2009, 1390))
While in this study the type of cement used did not appear to affect the disease process, recent evidence suggests that some cement types may have an active role in the disease process.
As a result of the cumulative information available, so far it appears that modifying surgical and prosthetic approaches when using cemented crowns are important. Prosthetic modifications and the use of alternative types of cement are addressed in other chapters of this book.
Surgical modifications include reduction of excess soft tissues, which may interfere with cement removal, flattening posterior ridges to eliminate redundant soft tissue, the use of implants with smooth gingival collars designed to raise the crown/implant margin coronal to the soft tissues, and placing the coronal portion of the implant as shallow as possible, while keeping esthetic and functional aspects in mind.
Treating implants that have lost bone attachment as a result of periimplantitis remains problematical. At present, the only proven way to stop the progress of periimplantitis is to remove the rough surface of the implant. This presents obvious esthetic and food impaction problems. One of the keys to achieving new bony attachment on an implant surface previously covered by biofilm is the successful removal of the bacteria and their byproducts. While many approaches have been tried, the final answer is not yet available. One technological advance, the video scope, allows increased visualization and a greater potential to remove implant-borne and soft tissue-associated particles. These particles are frequently found to be cement and titanium. Studies on their role in the etiology of peri-implant diseases, as well as the treatment of these diseases, continue.
At present, it is important to educate dental professionals about the problem and to periodically evaluate the peri-implant tissues monitoring for early indications of disease. When peri-implant mucositis is detected early, treatment should be immediately employed to prevent this evolving into periimplantitis with associated bone loss.
Case Reports Where Residual Cement Was Associated with Peri-implant Disease
Figure 2.5a shows a female patient who presented with cervical resorption of the maxillary right canine with symptoms of irreversible pulpitis. Radiograph is shown in Fig. 2.5b. Treatment of choice was extraction and implant placement.
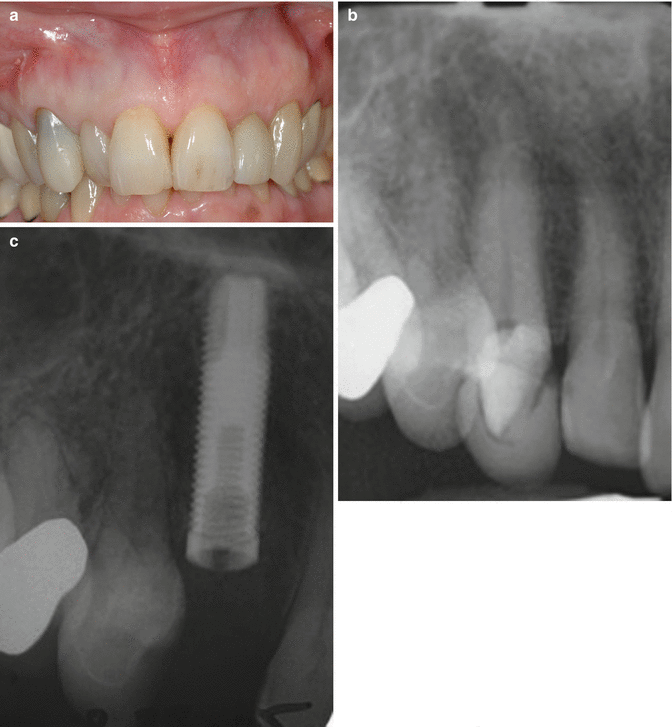
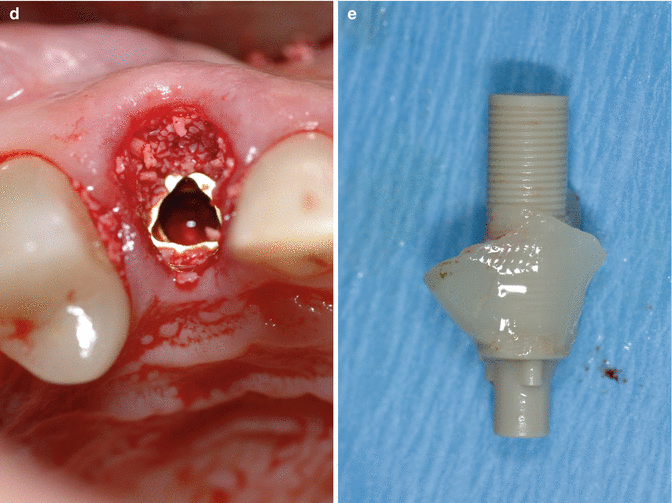


Fig. 2.5
(a) This female patient presented with cervical resorption of the maxillary right canine with symptoms of irreversible pulpitis. (b) Radiograph is shown. Treatment of choice was extraction and implant placement. (c–e) Post extraction, the surgical site was carefully evaluated and bone thickness recorded. This was considered appropriate for immediate implant placement (Implant: Nobel Biocare Replace). (c) Radiograph showing implant placed. (d) Cervical area augments with allograft particulate matter (Bio-Oss). (e) Custom healing abutment being fabricated, using a temporary plastic cylinder. This was provided to maintain the soft tissue profile during the healing phase. The implant was left to integrate for 3 months prior to referral back to the restoring clinician
Post extraction, the surgical site was carefully evaluated and bone thickness recorded. This was considered appropriate for immediate implant placement (Implant: Nobel Biocare Replace). Figure 2.5(c-d) Radiographic imaging showed the implant to be in a good position, the soft tissue was supported by the use of allograft particulate material (Bio-Oss, Giestlich). To prtects and support the soft tissues further a custom healing abutment was fabricated Figure 2.5e. The implant was left to integrate for 3 months prior to referral back to the restoring clinician.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses