Case 6
Prosthodontic treatment for the newly diagnosed patient with type 2 diabetes mellitus
Ira B. Lamster, DDS, MMSc; Nurit Bittner, DDS, MS; and Daniel Lorber, MD
A 31-year-old female presented with the chief complaint, “I need braces; my teeth have shifted.”
The patient noticed her teeth shifting about two years ago. She was always interested in orthodontic treatment to address the mandibular crowding and the palatal position of tooth #7, but postponed treatment for financial issues. She is now ready to begin.
The patient noticed some bleeding when brushing, but did not complain of pain or any other symptoms associated with her mouth.
She claimed to brush her teeth twice a day, but admitted to flossing “rarely.”
Medical history
The patient is 5ʹ1ʺ tall and she weighs 165 pounds. She has a history of asthma; however, the last episode was more than 19 years ago. She does not take any regular medications, and does not have any allergies. She does not see a physician regularly. She reported, “I’m fine except for my gums.” Her father died at age 55 of a “massive heart attack.” His height was 5ʹ9ʺ and weight was 195 lbs with increased abdominal obesity. Her mother is 63 years old and has “mild” diabetes and arthritis. On questioning by the dentist, the patient reveals that she was told her “sugar level was borderline” several years ago. At that time, she went on a diet, lost 15 lbs, and was then told that her blood sugar was “OK.” She has regained the weight that was lost. Based on the patient’s height and weight, her body mass index (BMI) is 31.2, which is considered obese (to calculate and classify BMI, go to http://nhlbisupport.com/bmi/bminojs.htm).
Dental history and history of the current problem
The last dental visit was six months ago for a “cleaning” in another office. The patient has had only intermittent dental care throughout her lifetime. At the initial examination, there were no significant extraoral findings. Muscles of mastication and facial expression were all within normal limits. The temporomandibular joint was also within normal limits. The intraoral examination did not reveal any abnormalities of the tongue, floor of the mouth, hard and soft palate, and buccal mucosa. The oral cancer screening was negative. The buccal mucosa in the anterior region appeared erythematous. The patient is partially edentulous; she is missing all third molars and the mandibular second molars (Figure 1).
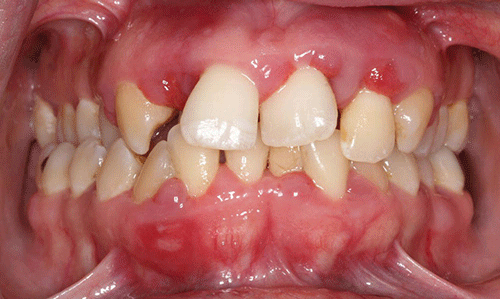
Figure 1 Maximum intercuspation, anterior view.
Moderate plaque and subgingival calculus deposits were observed; moderate to severe gingival inflammation was present. Probing depths ranged from 2 mm to 10 mm, with heavy bleeding on probing. In some areas the papillae were absent, and more commonly hyperplasia and severe inflammation were noted (Figures 2 and 3).
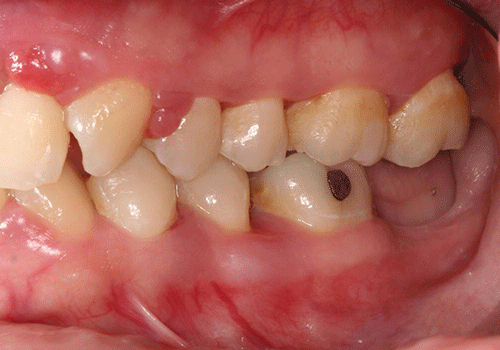
Figure 2 Maximum intercuspation, left lateral view.
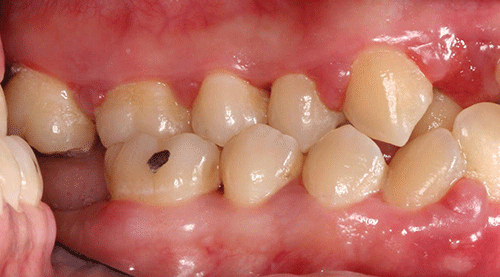
Figure 3 Maximum intercuspation, right lateral view.
The maxillary right second molar and the mandibular left central incisor had grade three mobility. Furcation involvement was also noted on the maxillary right second molar. No carious lesions were observed (Figures 4 and 5).
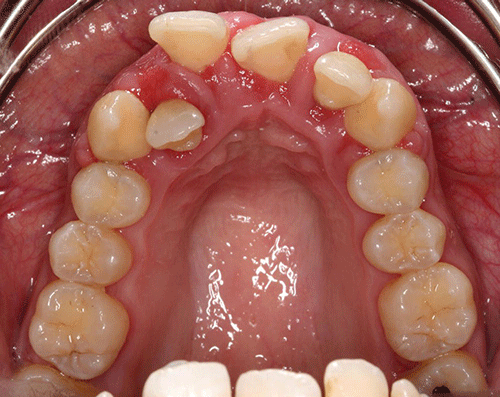
Figure 4 Maxillary occlusal view.
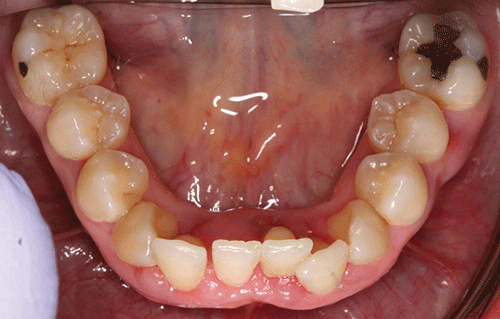
Figure 5 Mandibular occlusal view.
The patient has Class I Angle’s classification on her first molars and canines, with right side posterior crossbite. Her maxillary right lateral incisor is palatally positioned, creating a localized anterior crossbite. The patient presents interferences in right working lateral movement on the non-working side with contacts between the premolars. She has group function contacts on laterotrussive movements. No fremitus was detected.
Full mouth series and panoramic radiographs were taken (Figures 6 and 7). Radiographic evaluation revealed generalized horizontal bone loss with localized vertical bone loss about the maxillary lateral incisors. The mandibular left central incisor demonstrated a periapical radiolucency.
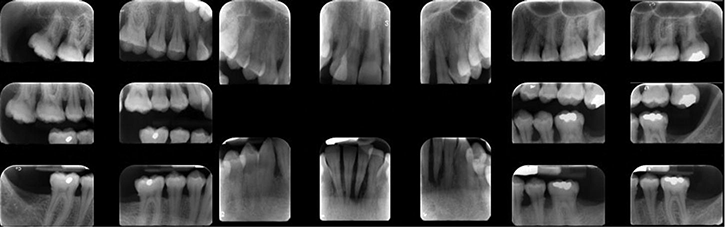
Figure 6 Full mouth series of radiographs.
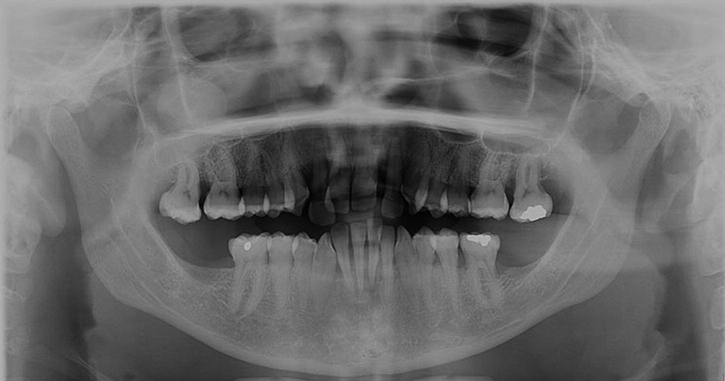
Figure 7 Panoramic radiograph.
The following problems list was compiled after review of the history and clinical and radiographic data:
- Generalized moderate chronic periodontitis, with areas of severe inflammation.
- Mucosal erythema.
- Peri-apical lesion associated with the mandibular left central incisor.
- Maloclusion with anterior and posterior crossbites.
Due to the nature of the gingival inflammation and erythematous mucosal lesions suggestive of Candida albicans infection, as well as her BMI, and since the patient’s last medical examination was more than one year ago, it was recommended to the patient to have a full medical evaluation, including assessment of her risk for diabetes mellitus.
Treatment plan
The patient realizes that she is at increased risk for diabetes. She then asks her dentist what she should do next. At this point, the dentist has several options:
- Refer her to a primary physician for further evaluation.
- Send her to a laboratory for an HbA1c determination and fasting blood glucose.
- Perform a point-of-care blood glucose and/or HbA1c in the office.
The American Diabetes Association recommen/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


