Case 4
The patient with diabetes mellitus and xerostomia
Ira B. Lamster, DDS, MMSc; Nurit Bittner, DDS, MS; and Daniel Lorber, MD
A 67-year-old male presented with the chief complaint, “My top partial denture bothers me and the teeth on my top right hurt.” The patient noticed some bleeding when brushing. He also mentioned that his mouth was feeling dry. The patient has not been to the dentist in the past three years.
Medical history
The patient is 5ʹ 6ʺ tall and he weighs 185 pounds. He states that he has no allergies. The patient was diagnosed with type 2 diabetes mellitus eight years ago. At that time his HbA1c was 9.5%. He was given a course of treatment consisting of lifestyle changes (exercise and diet control) and oral medications (metformin 1,000 mg bid and glimepiride 2 mg qd). He has minimal follow-up with his primary care physician and does not see an endocrinologist.
With questioning, he notes paresthesia of his feet (“It feels like I am walking on clouds”) and recently fractured his wrist with minimal trauma. The orthopedist noted bone loss on his examination and recommend a test for bone density, which has not yet been performed.
His last medical visit was three months ago, revealing an HbA1c of 9.1%. His primary care physician referred him to an endocrinologist; the appointment is pending.
The patient does not smoke cigarettes, and denies any history of alcohol abuse. He has not used recreational drugs for the past 20 years.
Dental history and history of the current problem
All of the patient’s restorations, including the porcelain fused to metal splinted crowns on the maxillary premolars and the single crowns on the maxillary first molars, were delivered more than seven years ago, in conjunction with the maxillary and mandibular removable partial dentures.
The last dental visit was three years ago. At that time the patient’s current maxillary removable partial denture was repaired as tooth #9 was added to the denture when the natural tooth fractured (Figure 1).
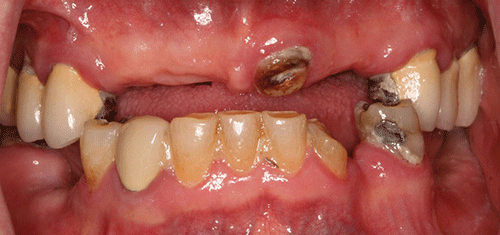
Figure 1 Maximum intercuspation, anterior view.
The muscles of mastication and facial expression were all within normal limits. The temporomandibular joint was also within normal limits. The skin around the lips appeared dry and flaky. Areas of the tongue, floor of the mouth, hard and soft palate, and buccal mucosa had an erythematous appearance. A screening for oral cancer was negative.
Moderate plaque and subgingival calculus deposits were observed; moderate to severe gingival inflammation was present. The mouth appeared dry, with minimal saliva. Probing depths ranged from 2 mm to 10 mm, with pronounced bleeding on probing. The maxillary right first molar and the mandibular left central incisor had grade three mobility. Furcation involvement was also noted on the maxillary right first molar. In some areas the papillae were absent, and more commonly hyperplasia and severe inflammation were noted (Figures 2 and 3). Recurrent caries were noted for many teeth. The patient claims to brush his teeth twice a day but he does not use dental floss.
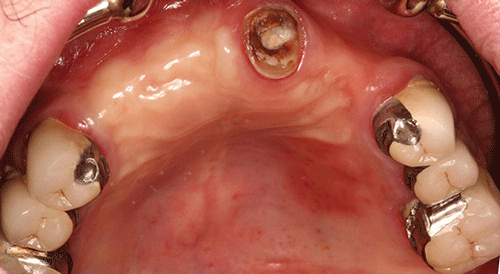
Figure 2 Maxillary occlusal view.
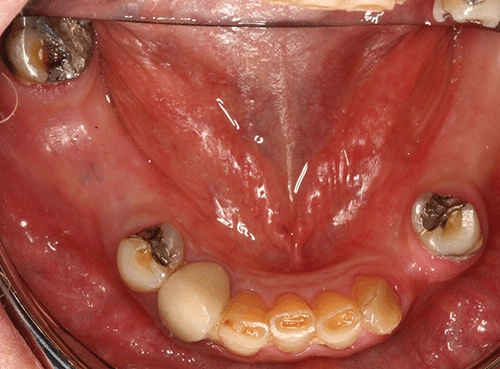
Figure 3 Mandibular occlusal view.
All maxillary porcelain fused to metal crowns (#3, 4, 5, 12, 13, and 14) demonstrated recurrent caries. The root tip of tooth #9 was still present, with coronal decay. Teeth #21, 28, and 32 presented with defective amalgam restorations with recurrent caries. Tooth #27 presented with a defective porcelain fused to metal crown, and recurrent caries.
Pulp testing was completed for the maxillary right side because the patient complained of pain. It was determined that teeth #3 and 4 had irreversible pulpitis.
Although the patient was partially edentulous and an occlusal classification could not be made, with his current removable partial denture the patient showed an Angle’s Class III occlusal scheme, which is related to the patient’s maxillo-mandibular ridge relationship. No interferences were observed on excursive movements.
Full mouth series and panoramic radiographs were taken. The lamina dura was visible. Radiographic evaluation revealed minimum generalized horizontal bone loss. Teeth #9 and 13 had endodontic treatment, both demonstrating a periapical radiolucency.
Teeth #3, 4, 5, 12, 13, 14, 21, 27, 28, and 31 presented with recurrent decay. The recurrent decay was more advanced on teeth #3, 4, 5, 12, 13, and 14, with both coronal and subgingival (root) involvement.
The follo/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


