Fig. 5.1
Clear interface against cell, bacterial and tissue: The interface works as a barrier for transportation of molecules and conduction of biofunction (a). Unclear and graded interface at which smooth transportation of molecules occurs, both material and tissue are integrated together, and biofunctions are conducted (b)
5.3 Osseointegration of Titanium
Osseointegration is the first definition of the interface between a metallic material and living tissue. The definition of osseointegration is as follows: The formation of a direct interface between an implant and bone, without intervening soft tissue. No scar tissue, cartilage or ligament fibers are present between the bone and implant surface. The direct contact of bone and implant surface can be verified microscopically [1]. This “osseointegration” concept was immediately accepted by dentists and dental materials researchers in the world to show biocompatible advantage of titanium among metals that makes it possible that titanium occupies major position in dental implant bodies. After percolating the concept of osseointegration, the elucidation of osseointegration mechanism including the investigation on microscopic interface structure between titanium and bone tissue has been actively studied.
5.4 Mechanism of Osseointegration in Titanium
From the viewpoint of the property of titanium surface, mechanism and process of osseointegration has been discussed. Titanium and some of its alloys are known to be among the best biocompatible materials, and commercially the materials have been successfully used for orthopedic and dental implants. The question is why titanium and its alloys show such good biocompatibility compared with other alloys. The explanation to the question is generally believed to be that titanium passivates in aqueous solutions and that passive film is stable even in a biological system. Therefore, it was first thought that good hard tissue compatibility of titanium is caused by its high corrosion resistance. This hypothesis was false. For example, electric plating of platinum on titanium makes delay bone formation on itself, while the corrosion resistance increased [2]. Therefore, good hard tissue compatibility of titanium is caused not only by its high corrosion resistance but also other causes.
In this regard, the surface layer of titanium is essentially TiO2 before and after autoclaving and anodic oxidation treatment [3, 4]. However, it is questionable whether titanium oxide is stable and does not react with any electrolyte even in biological system. In this question, the mechanisms of passive dissolution of titanium in a model physiological environment were revealed [5]. They explained that dissolution of titanium depends on solution ligands and the surface oxide characteristics. They also revealed preferential molecular adsorption on titanium [6].
Composition of surface oxide film varies according to environmental changes, though the film is macroscopically stable. Passive surfaces co-exist in close contact with electrolytes, undergoing a continuous process of partial dissolution and re-precipitation from the microscopic viewpoint. In this sense, surface composition is always changing according to the environment (Fig. 5.2). The composition and properties of the oxide film regenerated in a biological environment may be different from those in water. When titanium which has been surgically implanted into the human jaw is characterized using Auger electron spectroscopy, its surface oxide film reveals constituents of calcium, phosphorus, and sulfur [7, 8]. By immersing titanium and its alloys in Hanks’ solution and other solutions [9–12] (Fig. 5.3), preferential adsorption of phosphate ions occurs. Even during cell culture on titanium, calcium phosphate is formed on it [13]. Extrapolating from here, it can be assumed that bone formation is faster on titanium implanted in hard tissue simply because the surface oxide film is titanium oxide. The surface oxide film on titanium is not completely oxidized and is relatively reactive; neither calcium nor phosphate stably exists alone on titanium, and calcium phosphate is naturally formed on it; calcium phosphate formed on titanium is stable and protective [14]. Surface oxide films as passive films on valve metals such as Ti are almost amorphous and different from titanium oxide bulk and crystalline ceramics with regard to its chemical property.
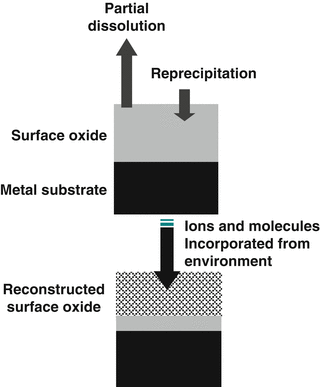
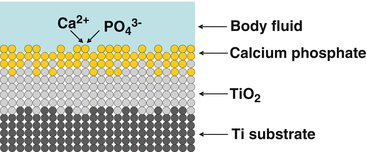

Fig. 5.2
Schematic model of reconstruction of the surface oxide film on metallic biomaterials

Fig. 5.3
Calcium phosphate formation on titanium in a simulated body fluid such as Hanks’ solution
The surface oxide is always formed on conventional metallic biomaterials and the surface of the surface oxide is active. Therefore, the oxide surface immediately reacts with water molecules and hydroxyl groups are formed as shown in Fig. 5.4a. The surface hydroxyl groups contain both terminal OH and bridge OH in the equal amounts. Concentration of hydroxyl groups on the unit area of the surface is determined with various techniques. Active surface hydroxyl groups dissociates in aqueous solutions and forms electric charges as shown in Fig. 5.4b [15–18]. Positive or negative charge due to the dissociation is governed by pH of the surrounding aqueous solution: positive and negative charges are balanced and apparent charge is zero at a certain pH. This pH is the point of zero charge (pzc). The pzc is the unique value for an oxide and an indicator which the oxide shows acidic or basic property. For example, in the case of TiO2, the pzc of rutile is 5.3 and that of anatase is 6.2 [15] (Fig. 5.4c). In other words, anatase surface is acidic at smaller pH and basic at larger pH than 6.2. Active surface hydroxyl groups and electric charges formed by the dissociation of the groups play important roles for the bonding with polymers and immobilization of biomolecules. Therefore, the concentration of surface hydroxyl group and pH is important factors for the bonding with polymeric materials and immobilization of biomolecules.
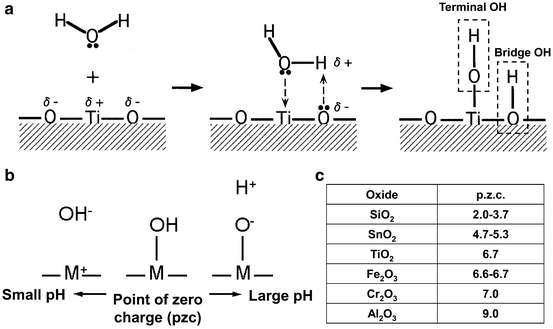

Fig. 5.4
Formation of surface hydroxyl groups on titanium oxide by the adsorption of water molecules (a), dissociation of hydroxyl groups in aqueous solutions including body fluid and showing positive and negative charges according to the environmental pH (b), and point of zero charge (pzc) of various oxide (c)
Proteins adsorption influences cells adhesion. Likewise, proteins denaturalization and fragmentation (which occur due to adsorption) may affect the function of the host body. To characterize proteins adsorbed to metals and metal oxides, various techniques can be used [19], especially that of ellipsometry [20]. To predict proteins adsorption, the wettability test is used where a liquid droplet is applied to the material [21]. Fibrinogen is much more naturally adsorbed on titanium surface than on gold surface, because the dielectric constant, the factor governing electrostatic force, of TiO2 is 80.1 and similar to that of water [22]. Therefore, fibrinogen remains its conformation even after the adsorption on titanium surface.
As described above, many researchers made their effort to elucidate the mechanism of osseointegration by characterization of titanium surface oxide (composition and change of it), surface hydroxyl groups, adsorption of proteins (amount, speed, change in the conformation, and denaturalization), and adhesion, proliferation and differentiation of cells. However, the true mechanism of osseointegration is still not clear.
5.5 Nanometer-Level Interface Structure
On the other hand, micrometer and nanometer-level observation of the interface between titanium and tissue has been studied. The intact bone-to-titanium interface consists of a fibrous tissue-free boundary zone with a 20–40 nm thick proteoglycan coat immediately adjacent to titanium oxide are revealed [23, 24]. Bundles of collagen appear at a minimum distance of 100–200 nm from the interface. Calcium deposits were sometimes seen in direct contacted (resolution level 30–50 nm) with the titanium oxide. The similar variation in interface ultrastructure within 50–100 nm of titanium surface [25]. The collagen fibrils did not reach the implant surface but were separated from it by an amorphous layer, being 300–500 nm thick which did not decrease in width with time [26]. An electron-dense lamina limitans-like line containing mineral was observed between the amorphous layer and the bone tissue. On the other hand, amorphous proteoglycan layer is not interposed at the interface between bone and titanium was observed [27]. In addition, this lamina limitans seems to consist of osteopontin and α2 HS-glycoprotein [28]. Recently, osteoblast-like cells made direct contact with titanium via a 20–50 nm thin amorphous zone is shown [29]. A 20–50 nm thin amorphous zone, a slender cell layer, and/or a poorly mineralized zone were interposed between bone and titanium. There is apparently a 20–50 nm amorphous layer containing proteoglycan on titanium oxide according to the above studies. Relatively high-resolutional observation using transmission electron microscopy is feasible in the findings regarding structure of the interface. However, it is difficult to make a tissue specimen with metallic material for TEM observation. Therefore, a couple of studies [24, 25] employed a foil and sputter-coated film of titanium instead of bulk material to be easily sectioned with a microtome. That is, the structure at the interface near titanium is unclear, while the observation of the interface is currently continued [30].
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


