Fig. 6.1
Chronic pseudomembranous candidosis located in left upper deep bucal vestibule and hard palate in a patient submitted to the chemotherapy
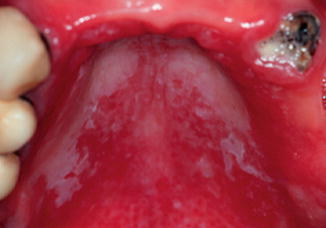
Fig. 6.2
Chronic pseudomembranous candidosis located in hard palate in a patient with an uncontrolled diabetes mellitus
The lesions are usually asymptomatic (Farah et al., 2010; Gonsalves et al., 2008); however, some patients can refer burning sensation, unpleasant salty or bitter taste (Gonsalves et al., 2008; Muzyka 2005; Neville et al., 2004; Regezi and Sciubba 2008). According to Muzyka (2005), these symptoms may compromise chewing and swallowing.
Pseudomembranous candidosis can be located in several anatomic sites of the oral mucosa surface, but the preference localization included mucosa of checks, deep buccal vestibule, oropharynx, and tongue (Farah et al., 2000; McCullough and Savage 2005; Neville et al., 2004). Gabler et al. (2008)) have identified that the main anatomic localization of the pseudomembranous candidosis in HIV patients were tongue (55.5 %), buccal mucosa (37 %), and palate (7.4 %).
Diagnosis
Candidosis diagnosis usually can be made according to the clinical findings (Muzyka 2005).
Basically, both acute and chronic pseudomembranous Candidosis are diagnosed by the white plaques removal using a soaked gauze or a wood spatula. Normally, after the removal, it is possible to see an underlying mucosa showing an erythematous surface. In advanced cases, the full oral mucosa can be affected (Shaffer et al., 1987). However, some authors state that the diagnosis of acute pseudomembranous candidosis has been overestimated during the last years and for this reason, in immunocompromised patients, a smear stained for Gram should be carried out to the differential diagnosis of acute pseudomembranous candidosis with yellow or white plaques caused by opportunistic bacteria (Scully 2009). Mostly, the associated symptoms are minimal, yet, in severe cases, the patients may complain of sensibility, burning, and dysphagia. Interestingly, some authors have described that the persistence of pseudomembranous candidosis can result in loss of pseudomembrane, with the presentation of a red lesion more generally known as acute erythematous candidosis. In these cases, along the dorsum of the tongue, it is possible to observe areas of depapillation and dekeratinization (Regezi and Sciubba 2008).
However, it is also important to highlight the patient’s history and the response to treatment with antifungal drugs (Gonsalves et al., 2008). In addition to the clinical findings, the diagnosis can be confirmed with exfoliative cytology, swab culture, imprint culture and, in specific cases, with mucosal biopsy (Gonsalves et al., 2008; Muzyka 2005). The exfoliative cytology is able to differentiate yeast and hyphal forms of the fungal, but is less sensitive than culture methods (Williams and Lewis 2000). Swab culture is the technique used to identify the microorganism and consists in obtaining a specimen by scraping the surface of the lesion using a swab. This specimen is deposited on a specific culture medium and incubated. Candida albicans grows after 2–3 days of incubation (Neville et al., 2004).
Exfoliative cytology, swab cultures, and biopsy are generally used to verify, qualitatively, the presence of different Candida species; however, these methods are less sensitive than culture. Imprint culture and salivary rinse techniques are able to quantify Candida species, and furthermore differentiate normal levels of Candida spp., those considered pathological, which are responsible for disease onset (Muzyka 2005).
Dendritic Cells × Candida albicans
The strategic location of dendritic cells in tissues, specifically in the epidermis and mucous membranes suggests that these cells assume a primary role in the onset of immune response against microorganisms such as Candida (Newman and Holly 2001). In addition, dendritic cells act differently on Candida albicans. For example, immature myeloid dendritic cells, phagocytose the fungus in both forms, effectively and quickly. However, those ones that remain in the filament or tubular form, known as “hypha”, are able to “escape” from the phagosomes. This occurs by different mechanisms of phagocytosis. When the microorganism is phagocytosed in its unicellular form, known as “yeast”, the fungus is surrounded by pseudopodia throughout its surface up to be fully enclosed, following the formation of the phagosome in which different stages of cell degradation is observed over a period of 4 h. However, in its hypha form, the fungus is engaged bilaterally by the emission of pseudopodia until its encapsulation, followed by the formation of the phagosome in which, surprisingly, within one hour, Candida seems to break the membrane of the phagosome, remaining free in the cell cytoplasm (d’Ostiani et al., 2000). Furthermore, the host resistance in candidosis is the result of Th1-mediated response along with the synthesis of cytokines such as IFN- and IL-12 ע, since they induce phagocytosis. Nevertheless, the response mediated by Th2 lymphocytes and their cytokines such as IL -4 and IL -10, inhibit Th1 development and inactivate cellular phagocytosis mechanism, allowing the disease progression (Bacci et al., 2002). Then, once taking the form of unicellular yeast, the Candida fungus induces dendritic cells to produce IL-12 cytokine, which in turn draws the Th1 lymphocytes, which are important in resistance to antigen in question. In contrast with in the tubular or filamentous form, the fungus induces dendritic cells to produce cytokine IL-4 by attracting Th2 lymphocytes, which act to inactivate the process of phagocytosis of Candida, as mentioned by Torosantucci et al. (2004).
References
Akpan A, Morgan R (2002) Oral candidiasis. Postgrad Med J 78:455–459PubMedCentralCrossRefPubMed
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


