(1)
Department of Orthodontics, College of Dentistry, University of Illinois, Chicago, IL, USA
(2)
South Florida Cleft Palate Clinic, University of Miami School of Medicine, Miami, FL, USA
(3)
Craniofacial Anomalies Program, Miami Children’s Hospital, Miami, FL, USA
(4)
Division of Plastic Surgery, Miami Children’s Hospital, W-3100 SW 62nd Ave, Miami, FL, USA
Abstract
One of the most widely debated areas in the treatment of cleft lip and palate involves the use of presurgical orthopedics and periosteoplasty with lip adhesion (POPLA) designed by Ralph Latham (orthodontist) and D. Ralph Millard, Jr. (plastic surgeon). They contend that the POPLA procedure is superior to a conservative nonpresurgical orthopedic treatment (non-POPLA) for producing more aesthetically appealing lip/nose surgery, while still allowing for good midfacial growth and dental occlusion in complete unilateral cleft lip and palate (CUCLP) and complete bilateral cleft lip and palate (CBCLP) patients. This chapter compares the dental occlusion of POPLA with conservative, nonpresurgical orthopedic treatment (non-POPLA), which Millard had been using between 1960 and 1980. POPLA proponents and others, who use this or a similar method, favor the same presurgical orthopedic procedure, such as nasoalveolar molding and gingivoperiosteoplasty (NAM + GPP). In CBCLP, patients forcefully retract the protruding premaxilla to favor the attainment of improved lip and nose aesthetics and anterior alveolar arch alignment soon after birth. They speculate that the early aesthetic benefits will remain as the face grows and develops.
In CUCLP and CBCLP, presurgical orthopedics, to align the anterior alveolar arches, is usually followed by periosteoplasty in the expectation that the resulting bone bridging will avert the need for secondary alveolar bone grafts at a later date.
This chapter challenges the rationale for presurgical orthopedics and periosteoplasty in the neonate.
Serial retrospective dental occlusal study covers more than 40 years of recording treatment outcomes with serial dental casts, the sequential influences of both the POPLA and conservative non-POPLA procedures on palatal development, and the anterior and buccal dental occlusion. These records test the efficacy of the POPLA procedure compared to the non-POPLA treatment.
21.1 Dental Occlusion
One of the most widely debated areas in the treatment of cleft lip and palate involves the use of presurgical orthopedics and periosteoplasty with lip adhesion (POPLA) designed by Ralph Latham (orthodontist) and D. Ralph Millard, Jr. (plastic surgeon) (Millard 1980, 1986). They contend the POPLA procedure is superior to a conservative nonpresurgical orthopedic treatment (non-POPLA) for producing more aesthetically appealing lip/nose surgery, while still allowing for good midfacial growth and dental occlusion in complete unilateral cleft lip and palate (CUCLP) and complete bilateral cleft lip and palate (CBCLP) patients. This study compares the dental occlusion of POPLA with conservative, nonpresurgical orthopedic treatment (non-POPLA), which Millard had been using between 1960 and 1980 (Berkowitz 1996a, b). POPLA proponents and others, who may not resort to a lip adhesion but who still use the same presurgical orthopedic procedure designed by Latham in CBCLP patients for forcefully retracting the protruding premaxilla, favor the attainment of improved facial aesthetics and palatal arch alignment soon after birth with or without periosteoplasty. They speculate that the early aesthetic benefits will remain as the face grows and develops (Millard and Latham 1990; Dufresne and So 1992; Millard et al. 1998; Mulliken 2001).
In CUCLP and CBCLP, presurgical orthopedics is usually followed by periosteoplasty in the expectation that the resulting bone bridging created will avert the need for secondary alveolar bone grafts at a later date.
It is not a simple or a lightly assumed task to offer a brief challenging the rationale for presurgical orthopedics and periosteoplasty for infants with complete unilateral or complete bilateral cleft lip and palate. Advocates of the POPLA concept, or a variant of it, are few but well respected. Their proposed goal of making things right and whole as early as possible seems sensible and has great emotional appeal.
This first of a two-part serial retrospective dental occlusal and facial study covers more than 40 years of recording with serial dental casts and lateral cephaloradiographs, the sequential influences of both the POPLA and conservative non-POPLA procedures on palatal development, and the anterior and buccal dental occlusion. Part one of this study uses serial dental casts to determine the extent of anterior and buccal crossbites. Detailed dental occlusal analyses of these records test the efficacy of the POPLA procedure compared to the non-POPLA treatment employed by Millard and Berkowitz from 1960 to 1980 prior to the POPLA treatment years.
Part two of this study will analyze facial changes using serial lateral cephaloradiographs.
21.1.1 Method and Materials
The complete unilateral and bilateral clefts of the lip and palate cases, treated by either presurgical orthopedics (POPLA) or the nonpresurgical orthopedics (non-POPLA) procedure, were chosen from the files of the longitudinal facial and palatal growth studies of the Miami Craniofacial Anomalies Foundation of patients from the South Florida Cleft Palate Clinic, the University of Miami School of Medicine. Dr. Ralph Millard, Jr., performed lip, nose, and palatal surgery in both test samples. Secondary alveolar bone grafts and maxillary and/or mandibular osteotomies and maxillary distraction osteogenesis were performed by S.A. Wolfe. Samuel Berkowitz documented growth changes with dental casts, lateral cephaloradiographs, panorexes, and photographs and performed all treatment orthodontics other than presurgical orthopedics (Millard et al. 1988, 1998). Berkowitz treated a number of children in the POPLA group who had extensive anterior crossbites starting when they were about 9 years of age so that beginning at this age, there is a reduction in the frequency of the cases with anterior crossbites.
21.1.1.1 POPLA: Presurgical Orthopedics with Lip Adhesion (Millard et al. 1998) (Fig. 21.1a, b)
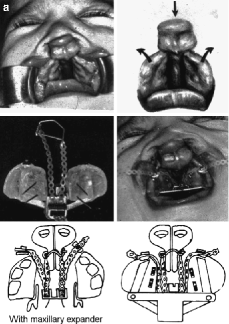
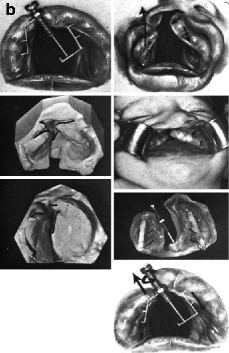
Fig. 21.1
(a) CBCLP. Latham’s presurgical orthopedic appliance. The elastic chain creates the activating forces to retract the premaxilla while expanding the palatal segments. The posterior segment is pinned to the palate for approximately 2 weeks. The premaxillary pins, which are pulled by the elastic chain, are positioned anterior to the premaxillary vomerine suture. (b) CUCLP. Latham’s presurgical orthopedic appliance. The screw knob controls the movement of the pinned appliance. The premaxilla is bodily rotated mediopalatally while the cleft lesser segment is moved anteriorly approximately 2–3 mm to make contact with the smaller cleft segment
Ralph Latham supervised the plastic surgery residents in the manipulation of the palatally pinned presurgical orthopedic appliance. Another orthodontist later performed the same relatively simple procedure. Because of the training and close supervision involved in the treatments given, there was relatively little variation in this procedure over the years covered by the POPLA data. In CBCLP, the appliance mechanically expands the lateral palatal segments, allowing for the retraction of the protruding premaxilla into position within the alveolar arch (Figs. 21.2, 21.3, 21.4, 21.5, and 21.6). In CUCLP cases, the mechanical forces bring the premaxillary portion of the larger segment mediopalatally, and in most instances, the lesser segment is carried forward 2–3 mm to make contact with each other (Fig. 21.5a, b). Afterward, the floor of the nose is surgically closed, and a periosteoplasty is performed to permit the migration of alveolar osteoblasts to bridge the alveolar gap space. After the premaxillary retraction, a lip adhesion is performed followed 6–8 months later by definitive lip surgery with “forked” flaps.
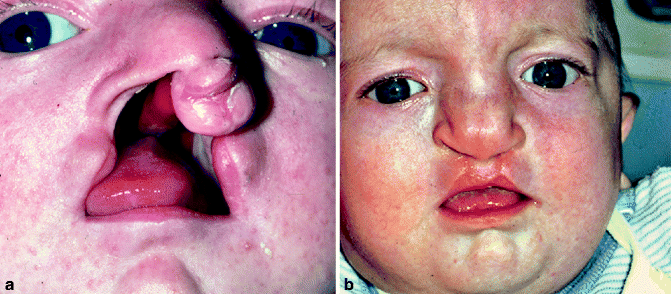
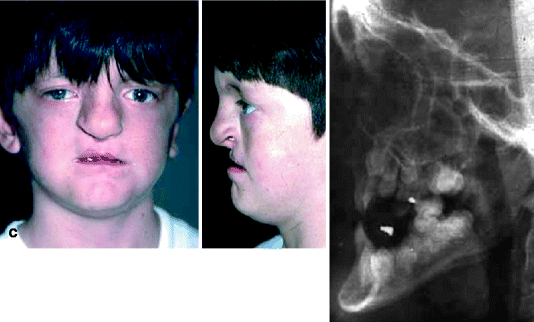
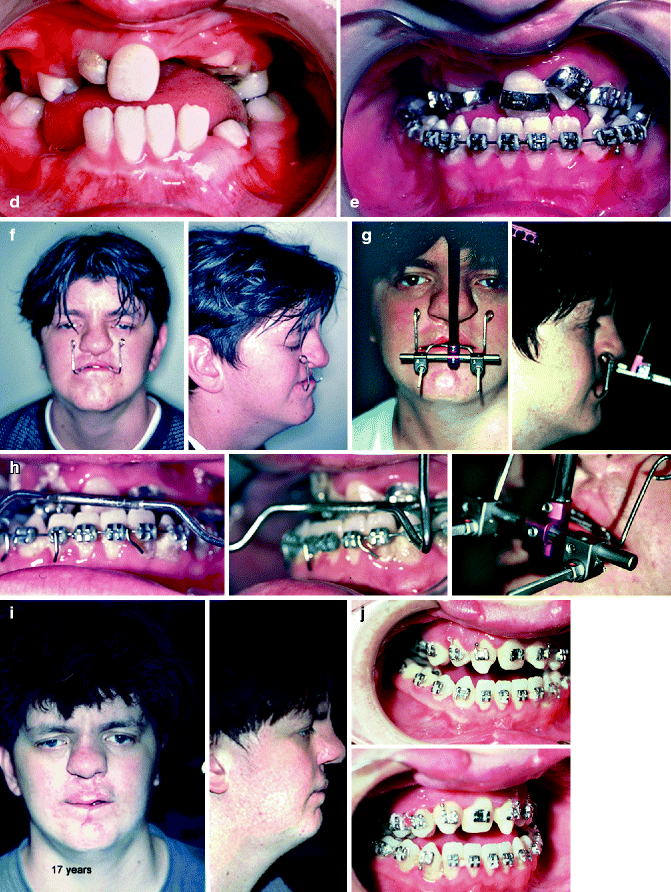
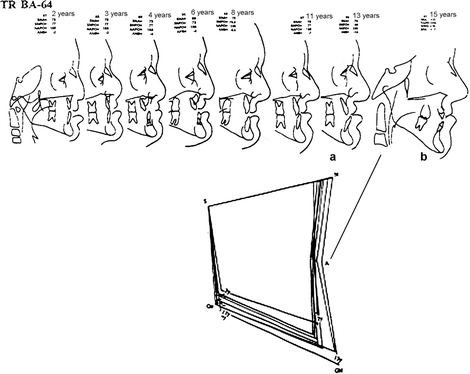
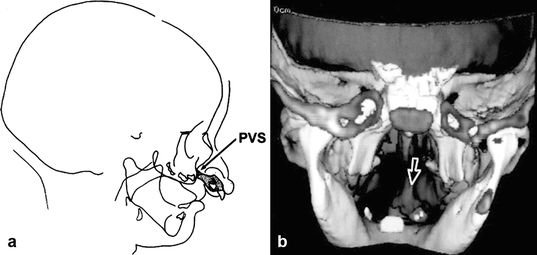
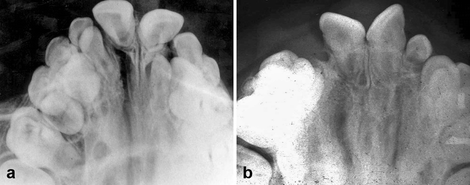
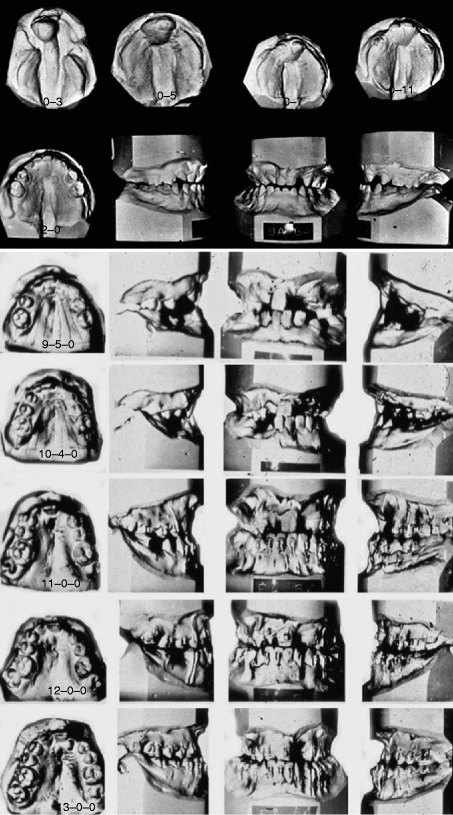



Fig. 21.2
(a–j). (a) Newborn. A small asymmetric protruding premaxilla. (b) After premaxillary retrusion. Lip adhesion followed by definitive lip surgery and gingivoperiosteoplasty (POPLA). (c) Midfacial deficiency due to retruded premaxilla (d) Retruded premaxilla showing some missing incisor teeth. (e) Orthodontic appliances placed to correct anterior crossbite and missing incisor spaces. Protraction facial mask with Class III mechanics was unsatisfactory in correcting this problem. The use of protraction facial mask was not successful in reducing midfacial deficiency due to upper and lower facial growth. This necessitated the use of maxillary distraction osteogenesis (f, h) Osteogenic appliance. (g) After maxillary advancement. (i, j) Following distraction osteogenesis to advance the maxillary denture. (i) After protraction facial mask – no changing. (j) Distraction osteogenesis to tip occlusion – now hypernasality is present

Fig. 21.3
(a, b) Serial cephalometric tracings showing the stability of the midfacial recessiveness even after the use of a protraction facial mask. There was no change in the Class I buccal occlusion since the orthopedic forces were directed to only advance the retruded premaxilla. (b) Postmaxillary distraction osteogenesis. Due to server hypernasality, maxilla advancement was discontinued

Fig. 21.4
(a) Lateral cephalometric tracing of a newborn with a complete bilateral cleft lip and palate shows the location of the premaxillary vomerine suture (PVS) posterior to the protruding premaxilla. (b) Frontal computed tomography scan of a patient with complete bilateral cleft lip and palate who was treated with the presurgical orthopedics, gingivoperiosteoplasty, and lip adhesion protocol. Only the left palatal segment is fused to the premaxilla with a bone bridge. Note the premaxilla “telescoping” at the premaxillary vomerine suture (arrow), the junction with the nasal septum

Fig. 21.5
(a) Palatal radiograph of a patient with complete bilateral cleft lip and palate who was conservatively treated at birth with a head bonnet with an elastic strip over the protruding premaxilla. The premaxillary vomerine suture was still open years later. (b) Palatal radiograph after premaxillary retraction with a Latham appliance shows a synostosis of the premaxillary vomerine suture

Fig. 21.6
Presurgical orthopedics, periosteoplasty, and lip adhesion (POPLA). The premaxilla was retruded and positioned within the arch. Followed by periosteoplasty, the palatal cleft was closed at 2 1/2 years using a von Langenbeck procedure with a modified vomer flap 9–13 years: The use of a protraction facial mask to advance the premaxilla was unsuccessful. This was followed by midfacial distraction osteogenesis
21.1.1.2 Non-POPLA Conservative Treatment of CBCLP and CUCLP
The protruding premaxilla in CBCLP is ventroflexed by the forces generated by a head bonnet with elastic strip positioned across the prolabium, followed by lip adhesion surgery. No attempt is made to bodily retract the premaxilla and place it within the alveolar arch. Palatal cleft closure using a von Langenbeck procedure with a modified vomer flap is performed between 18 and 36 months, depending on the size of the cleft space. In non-POPLA as well as POPLA cases, palatal expansion is sometimes used at 5–6 years of age to correct the buccal crossbite in both groups.
Orthodontics between 8 and 10 years of age on POPLA and non-POPLA patients is used to align the anterior teeth. In non-POPLA cases, it is performed prior to bilateral or unilateral secondary alveolar bone grafting. In POPLA cases, the anterior crossbite correction with full orthodontic appliances and a protraction facial mask is initialized at 8–9 years when one or both of the permanent central incisors are erupted. An attempt at this age is made to correct the posterior occlusion. None of the test groups were in the Class III buccal occlusion at this age. Standard orthodontics follows to align all the permanent teeth. In CUCLP and CBCLP, lip adhesion is mostly performed at 3 months in both series followed by definitive lip surgery at 6–8 months of age.
21.2 Discussion
Millard and Berkowitz have been associated since 1961 with the South Florida Cleft Palate Clinic, where presurgical orthopedic treatment (PSOT) was not being used. Millard has always been a strong supporter of the importance of serially documenting treatment outcomes with lateral cephalometric radiographs, dental casts, panorexes, and facial/intraoral photographs. To that end, they have worked diligently.
After 20 years of performing nonpresurgical orthopedics (non-PSO) prior to the utilization of the POPLA treatment procedure, Millard published an operational plan to investigate and record facial–palatal changes when utilizing the Latham procedure (Millard et al. 1988). Today, Berkowitz has assembled an extensive collection of serial records that have always been available for review by any interested party. Kai Henkel (1997), a visiting professor of plastic surgery from Rostock, Germany, after reviewing the POPLA treatment serial case records, published a review stating that the procedure resulted in unsatisfactory facial aesthetics and dental function.
After 40 years of recording facial, palatal, and dental growth changes in POPLA and non-POPLA cases, the authors of this brief believe that criticism is in order for a clinical procedure whose outcome results have now been adequately reviewed using serial objective records.
It is unfortunate that a controversy still exists as to the utility of POPLA or similar treatment with or without lip adhesion 20+ years after its introduction and after the critiques to which it has been subjected (Berkowitz 1996a, b). First, Georgiade and Latham (1975) and Latham (Latham 1970, 1973, 1980) have failed to publish any outcome studies. More recently, Millard and Latham have published a limited outcome report using Berkowitz’s palatal cast records (Berkowitz 1996a, b). Millard and Latham’s coauthors Huifen, Spiro, and Morovic performed linear measurements of the changing palatal size rather than analyze the relative growth of the opposing jaws by reviewing the dental occlusion.
Dufresne and So, in their chapter supporting the presurgical orthopedic procedure for CBCLP and CUCLP patients, referred only to Millard’s original introductory statements of the POPLA procedure in Cleft Craft (Vol. III) (Millard 1980) and listed no other supporting references, yet advocate its use (Dufresne and So 1992). Cutting and Grayson (Cutting et al. 1998; Cutting and Grayson 2000) limited their PSOT report to the effect of periosteoplasty in successfully producing bone bridging of the alveolar cleft, yet no mention was made of its effect on the dental occlusion.
Berkowitz (1996a, b), in a preliminary report, compares Millard’s POPLA with Millard–Berkowitz’s conservatively (non-POPLA) treated CBCLP outcomes. That comparative outcome study confirmed the negative effects of POPLA on facial aesthetics and dental occlusion. The study presented herein expands on that report.
In 1996, Berkowitz and Latham were asked by the American Cleft Palate Craniofacial Association program committee to debate the utility of this procedure at their annual meeting in San Diego, California. At that meeting, Berkowitz and LaRossa (plastic surgeon) presented long-term case reports that were critical of the procedure, but no supporting case studies were forthcoming from Latham and Morales (plastic surgeon).
Many clinicians who advocate the use of Latham’s or any other presurgical orthopedics (PSO) state that one of the appliance’s benefits is to prevent “collapse” of the lateral palatal segments. The frequent use of the word “collapse” to describe palatal arch relationships after neonatal lip surgery is unfortunate and needs to be better understood. The term is misleading for it conjures up an unwarranted sense of foreboding.
The word “collapse” was introduced into the cleft-treatment lexicon in the 1960s by some surgeons and orthodontists to describe the palate’s physical state after uniting of the lip and causing medial palatal movement of overexpanded palatal segments. They evidently did not realize that in complete lip and palatal clefts, the resulting medial palatal movement (molding) is beneficial because it reduces palatal cleft size and corrects the overexpanded palatal segments relationship. Serial studies have shown that overlapping palatal segments in the deciduous and mixed dentition are of no clinical importance.
The word “collapse” implies that this condition is bad and should be prevented. However, after years of analyzing serial dental casts, many orthodontists have concluded that establishing lip muscle continuity leads to good geometric palatal changes no matter their temporary neonatal geometric relationship. Overlapped segments do not impede normal palatal growth, and in most cases, such overlapped segments can easily be properly realigned using relatively simple orthodontics. Cleft segments in posterior crossbite at an early age are not indicative of future palatal maldevelopment. Since the width of the cleft space influences the type and timing of surgical palatal closure, one would prefer to have a small cleft space prior to palatal surgery to reduce the possibility of creating growth-inhibiting scarring while producing a normal palatal vault space.
In contrast to conservative non-POPLA cases, POPLA-treated patients require extensive and costly orthodontic treatment to correct the anterior crossbites, regain lateral incisor spaces, and achieve upper to lower anterior arch congruency. Often the degree of facial and palatal distortion is so extensive in POPLA cases that additional surgical intervention is necessary at a later age. Some parents have reported their children’s experiencing psychosocial problems due to the lack of peer acceptance of the concave facial profile.
POPLA in CBCLP (Table 21.1): The bodily retracted protruding premaxilla is retracted and placed in excellent alignment within the alveolar segments (Fig. 21.1a, b). Since no lateral flexion of the nasal septum is seen in cat scans, it was concluded that the premaxilla is “telescoped” posteriorly at the premaxillary vomerine suture (PVS) (Fig. 21.4). The bending at the PVS is also seen in POPLA-treated CUCLP (Fig. 21.5). The PVS is not observed in follow-up palatal POPLA radiographs (Fig. 21.5).
Table 21.1
Number of cases at each age level in presurgical and nonpresurgical orthopedics treatment groups
|
Approximate age of participant
|
|||||
|---|---|---|---|---|---|
|
3 years
|
6 years
|
9 years
|
12 years
|
Total sample
|
|
|
Unilateral cleft
|
|||||
|
POPLA treatment
|
30
|
43
|
34
|
18
|
125
|
|
Non-POPLA treatment
|
51
|
54
|
46
|
33
|
184
|
|
Bilateral cleft
|
|||||
|
POPLA treatment
|
21
|
20
|
15
|
9
|
64
|
|
Non-POPLA treatment
|
49
|
49
|
40
|
35
|
173
|
The diagram (Fig. 21.7) is designed to show the error of palatal segmental movements in POPLA CUCLP cases. Our 3D analysis of the CUCLP palatal arch changes demonstrates that the premaxillary portion of the noncleft segment is brought mediopalatally while the smaller cleft segment is advanced, resulting in the loss of the lateral incisor space. This explains why an anterior dental crossbite is most likely to result.
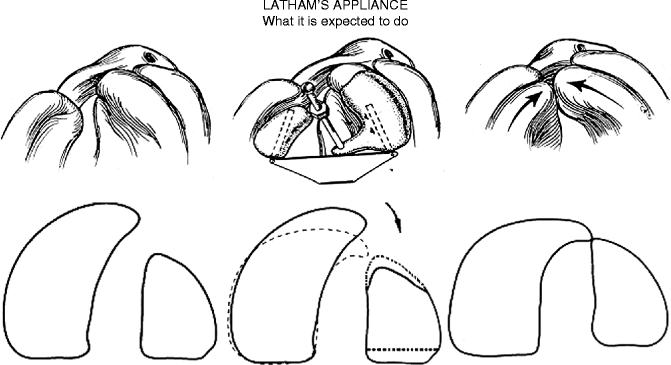

Fig. 21.7
(a) According to Latham, the mode of action of the appliance used in complete unilateral cleft lip and palate is the medial movement of both segments toward each other (Dufresne and So 1992). (b) None of our unilateral cleft cases, when activated with the Latham appliance, is shown below. The premaxillary portion of the noncleft segment is bent mediopalatally, while the lesser-cleft segment is carried slightly forward, into contact
Millard (1980) has written that premaxillary retraction and periosteoplasty might have a negative effect on palatal growth, but he nevertheless believes this trade-off is acceptable to obtain early aesthetics, to close the floor of the nose, and to avoid the need for secondary alveolar bone grafting.
The desire of some surgeons to establish a child’s well-balanced, aesthetically pleasing lips and nose soon after birth is understandable. However, extensive facial growth studies make clear that this should not be the top priority – that is, at the cost of good midfacial growth, dental occlusion, and speech at adolescence (Berkowitz 1996a, b; Pruzansky 1953; Pruzansky et al. 1973; Handelman and Pruzansky 1968; Friede and Pruzansky 1972; Friede 1973, 1977, 1978; Friede and Morgan 1976; Aduss et al. 1973
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


