Adult maxillary and mandible arch expansion without a surgical approach can be uncertain when long-term stability is considered. This case report describes the treatment of a 19-year-old woman with an Angle Class I malocclusion with constricted maxillary and mandibular arches. The patient’s main complaint was mandibular anterior crowding. The treatment plan included expansion of the mandibular arch concurrent with semirapid maxillary expansion. An edgewise appliance was used to adjust the final occlusion. Smile esthetics and dental alignment were improved without straightening the profile. This outcome was followed up with serial dental casts for 22 years after treatment. At the end of that period, the occlusion and tooth alignment were clinically satisfactory, further supported by mandibular fixed retention. However, the transverse widths were continuously and gradually reduced over time, superposing orthodontic transverse relapse and natural arch constriction caused by aging.
Highlights
- •
Aging can cause treatment results to change over time.
- •
An adult patient with constricted maxillary and mandibular arches was treated.
- •
Results of mandibular and semirapid maxillary expansion were followed for 22 years.
Successful orthodontic treatment is also referred to as long-term stability. However, orthodontic relapse and physiologic changes with age can produce dental arch instability. Longitudinal studies have shown that tooth position can be physiologically changed with aging in untreated subjects because of progressive arch constriction. These 2 phenomena are probably superposed in treated subjects during the postretention period.
As regards the transverse dimension, constricted arch problems have been solved through expansion, and increments in arch dimensions have been clearly demonstrated. However, most studies on maxillary and mandibular arch expansion have dealt with subjects in the mixed and early permanent dentitions, and only a few authors have studied long-term results. In young adults, the prognoses for rapid maxillary expansion and semirapid maxillary expansion (SRME) in terms of palatal suture opening are uncertain due to the rigidity of the skeletal components with advancing maturity. This prevents or limits the extent of suture opening and results in a greater dentoalveolar than a skeletal response, with an unpredictable long-term outcome. On the other hand, the response of mandibular arch expansion is only dentoalveolar, and it has been recommended in the case of a constricted arch. Nevertheless, the changes in mandibular arch form have controversial results and could adversely affect long-term stability and treatment outcomes. In contrast, other studies have shown that mandibular arch forms can be successfully expanded in the early stages.
Because dental and skeletal long-term stability is a key objective in orthodontics, and the tendency toward relapse is a real problem superposed by changes caused by aging, information on patients monitored over a long period could be valuable and help to clarify this issue. We present the treatment of an adult with a Class I malocclusion and constricted maxillary and mandibular arches. The outcome of the expanded mandibular arch concurrent with SRME was followed for 22 years after treatment.
Diagnosis and etiology
A 19-year-old woman, complaining mainly of tooth crowding, came for orthodontic treatment at a private office. She reported being satisfied with her facial appearance and had no serious medical impairment. A facial analysis showed a well-balanced face, a mesocephalic growth pattern, and a straight profile. The ratio of lower to upper facial heights was normal. The patient had competent lips and the nasolabial angle was within the normal range, but considering her slightly hooked nose and retruded upper lip, the mentolabial sulcus was somewhat deep, and her lower lip was slightly thicker than the upper lip although it did not impair the relationship between them. She had a high smile, exposing more than 2 mm of gingivae, and increased buccal corridors.
An intraoral evaluation showed a Class I molar relationship with maxillary and mandibular atresic dental arches. A crowding discrepancy of −5.0 mm was present in the anterior segment of the mandibular arch and was responsible for the irregular gingival alignment. The maxillary anterior teeth showed a buccal proclination with a slight midline diastema because of the central incisor divergence. On the right side, the canine had a Class II relationship. A single dental crossbite was present between the second premolars on the left side. A deep overbite was detected, with the maxillary incisors covering 60% of the mandibular incisors, and overjet was 6 mm ( Figs 1-3 ). No intermaxillary tooth-size discrepancy was found before treatment.
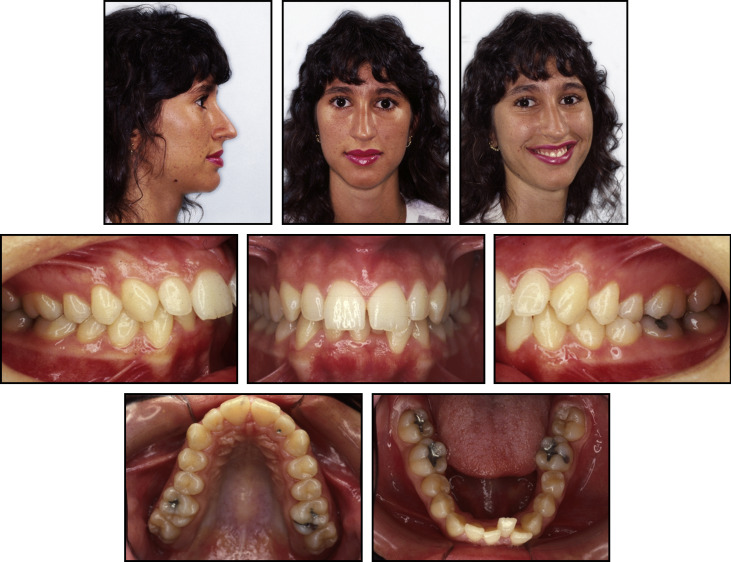
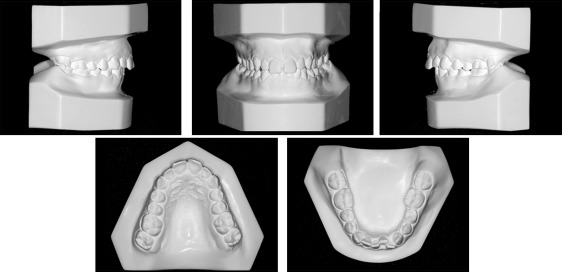
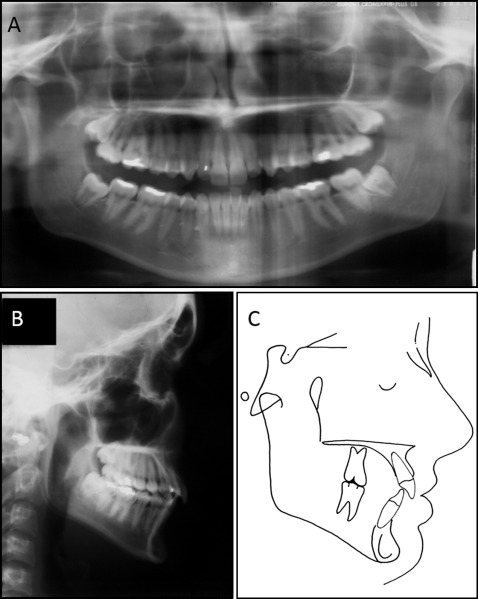
Most of these morphologic changes were probably related to her oral breathing developed with the increase in upper airway resistance during infancy. The Table shows the patient’s cephalometric measurements.
| Variable | Norm | Pretreatment 19 y 11 mo (T1) | Posttreatment 22 y 11 mo (T2) | Postretention 44 y 9 mo (T4) |
|---|---|---|---|---|
| Skeletal (°) | ||||
| ANB | 2.0 | 2.0 | 2.0 | 2.5 |
| SNA | 82.0 | 80.0 | 82.5 | 80.0 |
| SNB | 80.0 | 78.0 | 79.5 | 77.5 |
| SN.GoGn | 32.0 | 34.0 | 31.5 | 33.5 |
| FMA | 25.0 | 25.0 | 26.0 | 25.0 |
| Dental | ||||
| 1.NA (°) | 22 | 31.0 | 24.5 | 24.0 |
| 1-NA (mm) | 4 | 8.0 | 6.5 | 6 |
| 1.NB (°) | 25 | 21.5 | 35.5 | 33.0 |
| 1-NB (mm) | 4 | 5.0 | 8.0 | 6 |
| IMPA (°) | 90 | 90.5 | 110.5 | 102.5 |
| Overjet (mm) | 2-3 | 6.0 | 2.0 | 3.0 |
| Overbite (mm) | 2-3 | 5.0 | 2.0 | 3.0 |
| Profile (mm) | ||||
| S-Ls | 0 | −4.0 | −3.0 | −3.0 |
| S-Li | 0 | −1.0 | 0.5 | −1.0 |
Treatment alternatives
In view of the treatment objectives, the following treatment alternatives were presented to the patient: (1) SRME with mandibular dentoalveolar expansion followed by an orthodontic fixed appliance, (2) surgically assisted rapid maxillary expansion and mandibular dentoalveolar expansion followed by an orthodontic fixed appliance, (3) dental slice and fixed appliance, and (4) extraction of 4 premolars.
The first option was selected because of the principal problems and the patient’s wishes.
Treatment progress
In the expansion phase, the patient was treated with a Haas appliance and had her lingual arch expanded ( Fig 4 ). She was advised to activate the screw by 2 quarter turns per day for the first week, followed by a 1 quarter turn every other day, characterizing the SRME. After 16 days, she showed a low orthopedic response observed by a minimal median maxillary diastema and suspicions of a buccal alveolar fracture in the left first premolar. Two-dimensional radiographic images have limited access to any vestibular fracture, and no action was taken. The screw was then stabilized for retention. The 0.9-mm lingual arch of stainless steel wire was expanded 3 times during the SRME retention. For the activation, the lingual arch was first removed, the bands were labially torqued with a Weingart pliers, the lingual archwire was symmetrically expanded by 3 to 4 mm each time, and recemented. The aim of the active lingual arch was to correct the collapsed mandibular arch until the posterior teeth became upright, and thus contribute to improving the morphology of the mandibular dental arch. When both the Haas and the lingual arch expanders were removed after 5 months, there had been gains in the perimeters of the arches.




