Chapter 9
Painless Local Anaesthesia: Is It Possible?
Aim
The aim of this chapter is to consider factors that influence the discomfort of dental local anaesthetic injections.
Outcome
After reading this chapter you should have an understanding of the factors that produce pain during local anaesthesia in dentistry and appreciate techniques that can reduce injection sensation.
Introduction
It is unfortunate that the methods used to control dental operative pain may themselves produce discomfort. It should be the aim of all caring practitioners to reduce injection sensation to a minimum. The following factors can influence injection discomfort:
-
the expectation of pain
-
the needle
-
the syringe
-
the area of the mouth injected
-
the technique
-
the anaesthetic solution
-
the order of injection.
The dentist can influence all of these factors and thus can control the degree of discomfort produced during intraoral injections. Each of these elements will be considered.
The expectation of pain
Patients with low pain expectancy experience less injection discomfort than those with a high pain expectancy. The belief that patients are going to receive a topical anaesthetic can reduce their pain expectancy. This means that suggestion can be used to reduce the pain experience. Taking this a stage further may involve formal hypnosis. Some patients can experience total pain control by hypnosis, in others the technique can be used to reduce injection discomfort.
The needle
As far as the patient is concerned, it is probably the needle that is the most obvious cause of pain. The use of systems such as jet injectors could eliminate the needle altogether. These devices are not 100% effective in reducing operative pain. Indeed, in some studies subjects report more discomfort with the use of jet injection compared to infiltration anaesthesia. Factors that could influence the pain produced by needle insertion include:
needle gauge
needle condition
surface preparation
relative analgesia.
Needle gauge
It might appear obvious that the narrower the gauge of the needle the less discomfort produced by the injection. There is no evidence in the dental literature that supports this view. The gauges used in dentistry in the UK (27 and 30) appear to produce the same amount of discomfort and thus needle selection within these gauges does not influence injection pain.
Needle condition
Dental needles are provided with sharp points to enable easy penetration of the tissues. When they have been used the point loses its sharpness (Fig 9-1). Thus it would appear prudent to use a fresh needle for every tissue puncture.
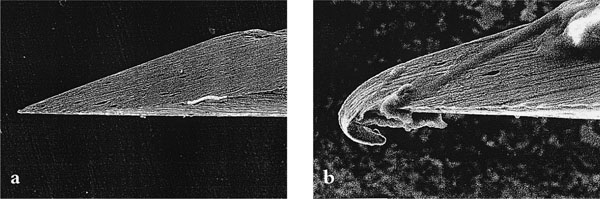
Fig 9-1 Scanning electron micrographs of an unused needle (9.1a) and a needle after contact with bone (9.1b). Note the deformation of the point after use. (Photographs kindly supplied by Dr John Rout).
Surface preparation
A number of methods of surface preparation may be employed. These include:
-
refrigeration
-
topical anaesthesia
-
jet injection
-
transcutaneous electronic nerve stimulation.
Refrigeration
The use of refrigeration has been suggested to reduce the discomfort of needle penetration in the palate. The tissue is treated for 5 seconds with an ice ball prior to needle insertion. Treating a cotton pellet with a volatile liquid, such as ethyl chloride, produces the ice ball (Fig 9-2).

Fig 9-2 An iceball produced by spraying a cotton bud with ethyl chloride.
Topical anaesthesia
Topical anaesthetics may have both a psychological and a pharmacological effect. It was mentioned above that the suggestion that a topical anaesthetic will be used reduces pain expectation. Is this the only benefit or do topicals produce a pharmacological benefit? There is evidence that topical anaesthetics do produce a pharmacological effect. As discussed in Chapter 6, the following factors influence the pharmacological efficacy of topical anaesthetics:
-
the agent selected
-
the duration of application
-
the site of application.
The topical anaesthetic agent
There is evidence that anaesthetic agents are better than placebo at reducing injection discomfort. In addition, not all anaesthetic agents show the same efficacy. A dose response has been demonstrated with lidocaine. For example, patches containing 20% lidocaine are more effective than those containing 10% lidocaine. In addition, the eutectic mixture of lidocaine and prilocaine has been shown to be more effective than lidocaine alone. Unfortunately, this preparation is not licensed for intraoral use at present.
The duration of application
In order to achieve a pharmacological effect, the topical anaesthetic must be present for more tha/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


