Management of Open-Bite Malocclusion
Flavio Andres Uribe, Nandakumar Janakiraman, Ravindra Nanda
Achieving an ideal treatment outcome depends on an accurate diagnosis in three dimensions, a good understanding of the interaction between the neuromuscular components of the orofacial region and the craniofacial skeleton, and the ability to provide individualized treatment mechanics.1 Early research in the 1950s and 1960s clearly showed the mutual dependence in three dimensions of the dentofacial complex.2 Despite the interest in three-dimensional (3D) diagnosis and treatment planning in orthodontics, the most widely used classification, introduced by Edward Angle, describes the malocclusion only in the anteroposterior dimension,2 providing little information about the vertical or transverse facial and dental relationships.
The importance of the vertical dimension of the face was first recognized by Downs and later discussed by Wylie and Johnson.3 Sassouni and Nanda2 comprehensively described the skeletal characteristics caused by dimensional and positional imbalances in both vertical and anteroposterior dimensions. Their classification of the facial types included an assessment of vertical disproportions. The terms skeletal deep bite and skeletal open bite were used to describe the two extremes observed in this dimension.2,4
Sassouni4 further investigated the vertical dimension of the dentofacial complex and found that disproportions in this dimension can be a cause for anteroposterior dysplasia. He further stated that addressing the vertical component of the malocclusion would bring about the desired outcome in the anteroposterior dimension.
During the same period, Schudy introduced the concept of facial divergence as the proportion of facial height to facial depth. He surmised that the ratio of depth to height affects not only the facial type but also the overbite. Hyperdivergent and hypodivergent facial types were described as the two extremes of facial divergence.5 Later, Nanda showed that these vertical patterns are established early in life, even before the eruption of permanent teeth.6
Various terms used to describe increased vertical facial dimension have been used interchangeably, describing angles, growth tendencies, and occlusal traits and even implying etiology. The following terms are used most commonly to describe an increased vertical facial pattern: dolichofacial, leptoprosopic, hyperdivergent, skeletal open bite, high angle, backward rotator, adenoid faces, long face syndrome, and vertical maxillary excess. Although the relationship is not necessarily direct, an increased vertical facial pattern has been associated with an anterior open-bite malocclusion.
Open bite has been defined as an occlusal characteristic in which upper and lower teeth are not in contact and vertical overlap does not exist. The term was first introduced by Caravelli as early as 1842.7 Although this type of malocclusion can occur unilaterally or bilaterally in the buccal segments, it most often occurs in the anterior segment. The anterior open-bite malocclusion is most obvious when a clearance is apparent between the upper and lower incisors from the frontal view. Of course, clinical diagnosis of an anterior open bite then becomes somewhat subjective because the diagnosis depends on the horizontal plane of assessment (Fig. 9-1).
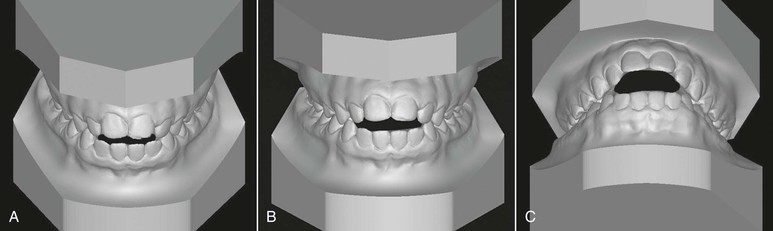
Figure 9-1 Evaluation of an anterior open bite from different planes. A, Minimal amount of anterior open bite is evident from the uppermost view angle. B, Increased open bite compared to A. Plane of assessment is almost perpendicular to the occlusal plane. C, The lowermost view angle reflects an extensive open bite, one that does not appear as extensive from the top view. The apparent magnitude of the open bite depends on the steepness of the occlusal plane and/or the plane of evaluation.
This chapter describes the characteristics of anterior open bite, its etiology and differential diagnosis, contemporary and evidence-based treatment approaches in growing and nongrowing patients, treatment alternatives and retention protocols for successful management, and increased predictability of stability in the long-term.
Characteristics of Anterior Open Bite
Björk8 described the skeletal and dental characteristics common in patients with anterior open bite. He discussed the morphological characteristics associated with downward and backward mandibular rotation during growth. These characteristics include distal condylar inclination, short ramus, antegonial notching, obtuse gonial angle, excessive maxillary height, straight mandibular canal, thin and long symphysis, long anterior facial height, short posterior facial height, steep mandibular plane, divergent occlusal planes, acute intermolar and interincisal angulation, anteriorly tipped-up palatal plane, and extruded molars. Among all of these characteristics, the steepness of the mandibular plane has been considered the key skeletal finding and thus the term high-angle patients.
Most soft tissue characteristics parallel those of the hard tissues: long lower facial height, steep mandibular plane, and short posterior facial height. In addition, a large interlabial gap is most evident on clinical examination of patients with a skeletal open bite9–11 (Fig. 9-2).
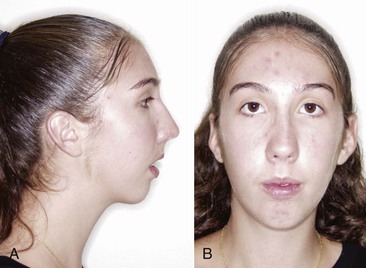
Figure 9-2 A large interlabial gap (>3 mm) is the most significant soft tissue characteristic of a skeletal open bite. A, Profile view. B, Frontal view with lips closed, showing the mentalis strain resulting from a large interlabial gap.
Although all of the skeletal characteristics just mentioned are associated with an anterior open bite, in one study12 only 13% of patients who had a cephalometric criterion for open-bite tendency had a vertical space between the incisors perpendicular to the occlusal plane. In many instances the skeletal open bite is camouflaged by overeruption of the anterior teeth. This issue makes classification of an open bite as either skeletal or dentoalveolar difficult. Often this malocclusion is the result of a combination of both factors.
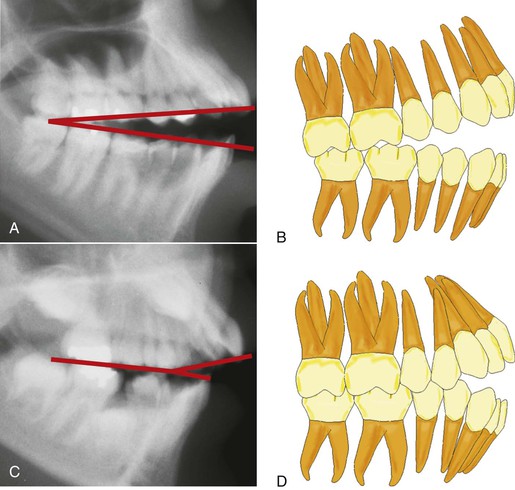
Studies10,11,13 have indicated that skeletal open bites are often related to excessive vertical growth of the dentoalveolar complex, especially in the region of the posterior maxillary molar (Fig. 9-3). Conversely, dental anterior open bites are primarily due to reduced incisor dentoalveolar vertical height14 (Fig. 9-4). The difference between these two types of open bites is also reflected in the occlusal planes. The skeletal type of malocclusion generally has occlusal contacts only at the molar level, with both occlusal planes diverging anteriorly,15 whereas the occlusal planes in the dentoalveolar open bite usually diverge from the first premolar forward (Fig. 9-5).
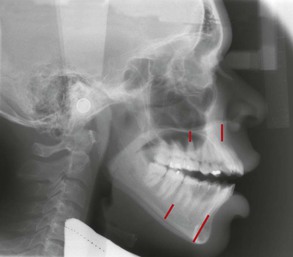
Figure 9-3 Excessive vertical height of the buccal segments is a common characteristic of skeletal anterior open-bite patients.
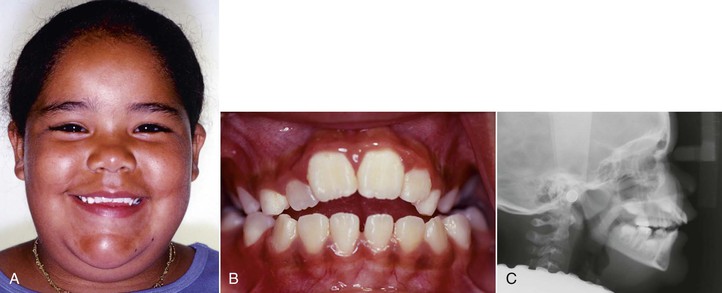
Figure 9-4 Reduced anterior dentoalveolar height characterizes a dental anterior open bite. A, Reduced incisal display as a result of restricted eruption of the maxillary incisors from a thumb-sucking habit. B, Anterior open bite from the finger habit. C, Reduced distance from the apex of the maxillary central incisors to the palatal plane.
Etiology
The causes of open-bite malocclusions are often related to the environment. Among the environmental factors, the concept of form following function has been singled out as a primary cause. An example is the role of the muscular posture affecting, directly or indirectly, the development of skeletal and dental open bites.
Airway and Craniofacial Pattern
Airway maintenance is an important factor in determining the posture of various orofacial musculatures. Nasopharyngeal obstruction induced experimentally in primates16,17 contributed to a lower position of the tongue and mandible, with the lips separated to maintain airway patency. This positional change led to increased anterior facial height, steeper mandibular plane, and larger gonial angle. Of note, the responses of the primates varied greatly. When extrapolating these findings to humans, clinicians should be aware of the individual variations in response to similar stimuli when assessing the contribution of mouth breathing to craniofacial deformity.16,17 Additionally, the experimental animal model does not translate well to humans because complete nasal obstruction is uncommon; the usual mode of respiration is oronasal.18
The association between mouth breathing and the vertical pattern of facial growth is rather weak. With the evidence available, predicting which children are at risk, at what age the growth pattern will change due to nasal obstruction, how much nasal obstruction must occur to alter the growth pattern, and finally if the acquired pattern is reversible is difficult.18 Fields et al.19 compared the mode of breathing in adolescents with normal and hyperdivergent vertical facial patterns. In patients with the hyperdivergent pattern, tidal volume and minimum nasal cross-sectional area were similar to those of patients with normal facial patterns but nasal respiration was significantly reduced. The authors concluded that the mode of breathing could be behaviorally determined rather than being anatomically dependent. Hence the relationship between nasopharyngeal obstruction and long face syndrome in children appears to be multifactorial.
Shanker et al.20 conducted a longitudinal assessment of the interrelationships between the upper respiratory parameters (nasal resistance, breathing mode) and dentofacial morphology in 8- to 12-year-old children. The results indicated that the pattern of respiration was neither constantly oral nor constantly nasal and that the children often switched from one pattern to the other over time. This alteration in breathing pattern over time may not have a clinically significant effect on the dentofacial complex. Further, in a comparison of the indicators of the long face pattern, no indicator differed significantly either statistically or clinically between nasal and oral breathers. On the basis of these findings, the transient mode of respiration may not significantly alter the pattern of craniofacial growth; thus surgical intervention to alter the mode of respiration may not be recommended. Souki et al.21 reported that the vertical growth pattern in a group of mouth breathers was no different after tonsillectomy and/or adenoidectomy than in a control group of mouth breathers.
With the advent of cone beam computed tomography (CBCT), research is being conducted to evaluate the relationship of the airway to the craniofacial dimensions.22,23 In the past, these studies focused on the airway relationship in the two dimensions registered by lateral cephalograms.24–26 With a 3D view, the contribution of the transverse dimension and the possibility of analyzing volumes will provide better evidence of this relationship. Three-dimensional CBCT-based evaluation of the upper airway is more accurate and more reliable than evaluation based on two-dimensional (2D) images.27
CBCT data may indicate an association between size of the airway and different craniofacial patterns and possibly relate the 3D anatomy to function. Using CBCT, Alves et al.28 found that the dimensions of the pharyngeal airway were greater in nasal breathers than in mouth breathers. However, a consideration of variables that might affect the findings of these studies is important. The variables include positioning of patients during image acquisition, impact of the respiratory phase, airway patency, head posture, mandibular morphology, and the position of the tongue and hyoid bone. Hence standardization of CBCT settings and definition of the anatomic boundaries of the airway are necessary.23,27 Because a standardized protocol for airway imaging is not available, making a reasoned judgment of the validity and reliability of upper airway models based on three-dimensional CBCT imaging is often difficult.29
Muscle and Its Contribution to Facial Pattern
A generally accepted notion is that hyperdivergent patients have weaker mandibular muscles and a weaker bite force than hypodivergent patients do. However, this relationship between the dentofacial complex (form) and jaw muscles (function) is still a matter of controversy. Whether or not the strength of the masticatory muscles is the primary determinant of the dentofacial complex is still not clear.30 The influence of muscles of mastication on the orofacial region is difficult to understand but can be at least theoretically determined by analyzing its geometric properties (size of the muscle, orientation of the muscle, and mechanical advantage), intrinsic properties (muscle fiber size and distribution), and muscle recruitment patterns.31
Muscle Size
The total force exerted by a muscle is directly related to its cross-sectional area of muscle fibers, which can be measured by using computed tomography (CT) and magnetic resonance imaging (MRI). The cross-sectional area can give some insight into the strength of the masticatory muscle in the various facial types. The size of masseter and medial pterygoid muscles was larger by 50% in brachyfacial subjects than in dolicofacial subjects. The size difference was about 30% larger in brachyfacial subjects for the temporalis muscles and about 6% larger for the anterior digastric muscle. Among the masticatory muscles, the cross-sectional area of the masseter is highly sensitive to the variation in long face subjects. The difference in size indicates a different loading pattern during function in hyperdivergent and hypodivergent patients.31
Muscle Orientation
When analyzed in the sagittal plane, the masseter was obliquely oriented in long face subjects and vertically oriented in short face subjects. Because of the difference in the spatial orientation of the masseter and medial pterygoid muscles in the two groups, the vertical force component of the muscles was 3% and 2% higher in short face subjects than in long face subjects respectively. Due to this difference in orientation of masseter and medial pterygoid muscles, Spronsen31 concludes that the brachyfacial subjects are more efficient in producing vertically directed bite forces. However, the differences in bite force between the two groups were quite small, even though they were statistically significant.31
The moment arm in the masticatory muscular force system is the perpendicular distance from the summit of the mandibular condyle to the line of action of the force. Small differences in values in the moment arm of the masseter and medial pterygoid muscles were observed in subjects with normal, hypodivergent, and hyperdivergent facial patterns. The moment arm at the region of the lower first molar was 8% smaller in the short face group than in the long face group. This difference is due to the morphology of the mandible and the spatial orientation of the masticatory muscles to the morphology between the short face and long face subjects. Because of the smaller moment arm and the associated biomechanical advantage, slightly larger bite forces were produced in brachyfacial subjects when compared with dolicofacial subjects.31
The maximum biting force was 155 N in long face subjects and 356 N in normal face subjects.32 In other studies33 bite force was 380 N in long face subjects and 720 N in short face subjects. However, the bite forces in children with hyperdivergent and normal facial patterns are similar,34 although the forces differ significantly in adults of both groups. Explaining why the maximum bite forces are lower in long face groups than in other groups is difficult. Can this difference in bite forces be due to differences in the composition of muscle fiber? Rowlerson et al.35 found that subjects with open bites had a higher percentage of type I fibers (slow contracting and fatigue resistant) in masseter muscle than did deep bite subjects. In contrast, compared with open-bite subjects, deep bite subjects had more type II fibers (fast contracting and relatively fatigable). A correlation exists between the vertical growth pattern and particular muscle fibers but further studies are necessary to evaluate the cause and effect relationship between the type of muscle fiber and vertical growth pattern of the face.
Based on the above findings, Van Spronsen31 concludes that the influences of muscle orientation, moment arms, and biomechanical advantage on the open-bite malocclusion are generally weak. The influence of maximum bite forces in determining craniofacial morphology is controversial, because electromyographic studies have shown that maximum bite forces are produced for only 6 minutes per day.36 The influence of the bite force of jaw muscle due to shorter duration of action on the developing craniofacial complex may be negligible or small.37 Furthermore, Ueda et al.38 reported that 90% of masticatory muscle activity is of low amplitude and may be related to long face morphology.
Finally, the vertical growth pattern is established early in life39,40; the craniofacial morphology is visible even before the development of weak musculature. Therefore the strength of association between the long face and weak musculature is rather weak and questionable. A hyperdivergent growth pattern, which is under a strong genetic influence, might result in a dentofacial morphology with weak musculature. These environmental interactions (weak musculature and others) on the genetically determined craniofacial structures could possibly determine the final expression of long face morphology.31
Role of the Tongue in Anterior Open Bite
Another major etiologic factor that reportedly contributes to open bites is an imbalance between the tongue and the perioral musculature.41 Various habits, such as tongue thrusting and thumb- and finger-sucking, and anatomic conditions, such as macroglossia, have been reported as causative factors. These factors contribute to the development of an open-bite malocclusion by adversely affecting the development of the anterior dentoalveolar complex and inhibiting the normal eruption of teeth.42 The force of the tongue or finger against the lingual surface of the incisors also causes concurrent flaring of the upper anterior teeth.43
Clinicians should carefully consider the role that the tongue plays in the etiology of open bite. Both the function and the anatomy of the tongue must be evaluated. From an anatomic point of view, a large tongue (macroglossia) can be responsible for splaying the anterior teeth and thus cause an open bite. Unfortunately, macroglossia is difficult to diagnose because no simple method is available to measure the volume of the tongue.44 Certain features noted during clinical examination that indicate macroglossia include spacing and flaring of the anterior teeth, indentations on the lateral borders of the tongue, and lateral extension of the tongue onto the occlusal surface of the lower teeth45 (Fig. 9-6).
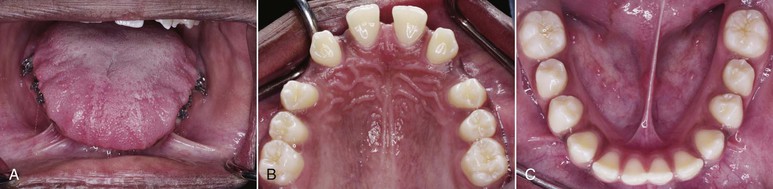
Figure 9-6 Patient with a large tongue. A, Intraoral clinical exam shows indentations on the lateral borders of the tongue and coverage of the occlusal surfaces of all lower teeth. B and C, Upper and lower arches depict generalized spacing.
From a functional point of view, deviant patterns of swallowing or tongue thrusting may contribute to the development of anterior open bite. However, some researchers claim that tongue thrusting appears to be a compensatory or adaptive behavior to the altered craniofacial skeleton. Swallowing, chewing, and speaking have little impact on the morphology of the dentition but the consequences of postural aberrations leading to changes in the resting pressure and posture of the tongue are marked.46 Some clinicians have proposed that the resting posture of the tongue is a more significant factor contributing to the open bite, compared to any of the temporal active functional muscular activity.
Several techniques, such as cineradiography, videofluoroscopy, ultrasonography, and, more recently, kinetic MRI, have been used to evaluate tongue movements during deglutition.47 Akin et al.47 used cine MRI to compare tongue movements during swallowing between subjects with anterior open bite and control subjects. The images were obtained during stage 1 (loss of contact of the dorsal tongue with the soft palate), stage 2 (passage of the bolus head across the posterior/inferior margin of the ramus of the mandible), and stage 3 (passage of the bolus head through the opening of the esophagus). Significant differences were found between stages 2 and 3, the pharyngeal and esophageal stages, which are involuntary. The posture of the tip of the tongue was more anterior during all stages in the open-bite subjects than in the control subjects. These results indicate that, during swallowing, the tip of the tongue is thrust forward in open-bite subjects to maintain the anterior oral seal. During normal swallowing the position of the posterior dorsum of the tongue was significantly elevated in stages 2 and 3, a change that might be a normal movement for propulsion of a food bolus and protection of the airway. However, in the open-bite group, the anterior part of the dorsum of the tongue is lowered and its middle part is elevated. As a compensatory mechanism to avoid aspiration during swallowing, the rear part of the tongue has minimal or no movement and marked movements occur in the anterior and middle parts of the tongue.
Thumb-Sucking
Prolonged thumb-sucking is another common environmental factor often associated with anterior open bite. Children who suck their thumbs have a higher prevalence of anterior open bite than do control subjects of a similar age group.48 Additionally, finger-sucking and a hyperdivergent facial pattern are significant risk factors not only for development but also for increased severity of an open bite.49
Trauma
Skeletofacial and dentoalveolar trauma are also etiologic factors of anterior open bite. Skeletal trauma involving the condyles can cause severe anterior open bites.50 Arrested condylar growth or ankylosis of the condyle results in altered vertical growth of the mandible, clinically manifested as an anterior open bite. Trauma to the dentition, particularly the incisors, can result in localized anterior open bite if the damaged teeth become ankylosed before the patient finishes growing51 (Fig. 9-7).
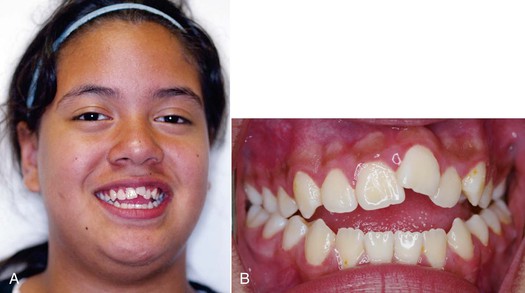
Figure 9-7 Anterior open bite exacerbated by an ankylosed maxillary left central incisor due to previous trauma. A, Smile view showing the reduced smile display in the ankylosed incisor. B, Frontal intraoral view showing the significant anterior open bite as a result of the ankylosed incisor.
Finally, anterior open bites may develop in patients with degenerative diseases involving the condyles. Idiopathic condylar resorption52 and juvenile rheumatoid arthritis53 are two pathological conditions that involve condylar resorption.
Genetics
The genetic component of an open bite is related primarily to the patient’s inherent growth potential. Traits such as anterior facial heights are, to a large degree, inherited.54 Obtaining a thorough family history will help in predicting a patient’s growth potential.
Although the main goal in a child is to predict the vertical skeletal relationships at the end of growth, growth patterns are established early in life and maintained in most people.55,56 Therefore a skeletal open-bite pattern could be evident in the early mixed dentition. Numerous cephalometric planes have been used independently and combined to detect the early skeletal open-bite pattern. The overbite depth indicator index of the primary dentition might be useful for predicting a skeletal open-bite tendency in adolescence.57 This index is a composite of cephalometric measurements involving the mandibular and palatal plane angles in relation to the A-B line and the Frankfort horizontal plane, respectively.
The Björk indicators are another useful method to help predict vertical growth patterns. However, these indicators are based on patients with extreme variations in vertical facial growth; thus they may be of limited value in patients with less severe open-bite skeletal patterns.58,59
The genetic component is an important contributing factor to open-bite malocclusion. Control of the vertical growth pattern by orthodontic means alone is difficult. However, changes in the dentoalveolar complex may directly affect the most representative skeletal features of an anterior open bite. For example, controlling the vertical eruption of the molars allows the mandible to rotate in a counterclockwise direction, reducing the excessive vertical skeletofacial pattern.
Treatment Strategies
As described in Chapter 1, treatment strategies should address the cause of the malocclusion. Environmental factors that contribute to a patient’s malocclusion, such as thumb-sucking or finger-sucking, should be identified during the clinical examination and then eliminated. The treatment of excess in the vertical dimension often mimics that of the treatment of anterior open bite. The different approaches can be separated according to the age of the patient. In growing patients, the focus of the approach is controlling the eruption of the molars, thereby affecting the skeleton. The same focus will also be beneficial if the patient has an anterior open bite. In adults, the excess vertical length has traditionally been treated with surgery, especially if the hyperdivergent features are associated with a marked dentofacial deformity that affects esthetics. These features are maxillary excess, increased mandibular plane angle, excessive gingival display, retrognathic mandible, long lower facial height, and excessive interlabial gap. Recently, these patients have been treated by using temporary anchorage devices (TADs). However, this approach is most often attempted only when the vertical excess is associated with an anterior open bite.
Treatment of Thumb-Sucking or Finger-Sucking
Children often have a habit of sucking on a finger or a thumb. Many children stop this habit on their own; others need assistance. Children should be encouraged by their parents to stop the sucking habit before the age of 4 years. Before this age, most adverse dental and skeletal effects caused by the habit usually return to the original state, creating a favorable environment for the eruption of permanent teeth.42 Communication and positive reinforcement by the parents may help to modify any undesirable behaviors but unless a child is willing to stop the habit, these attempts may be unsuccessful.60
To help a child stop the habit, parents should note the time of the day at which the behavior occurs and then try to intervene. For example, if a child sucks a thumb or finger during sleep, mechanically obstructing the hand with a sleeping gown may be helpful.61 If initial attempts are unsuccessful, an intraoral appliance that acts as a mechanical obstruction and reminder can be used.
Different intraoral appliances are available for behavior modification. These appliances consist of a stiff archwire with a series of loops that sit closely to the anterior part of the palate and attach to two upper molar bands. The loops act as a mechanical obstruction and a reminder of the habit. Usually, after 3 months spontaneous correction of any dentoalveolar or eruption problem occurs without use of any other appliance (Fig. 9-8).
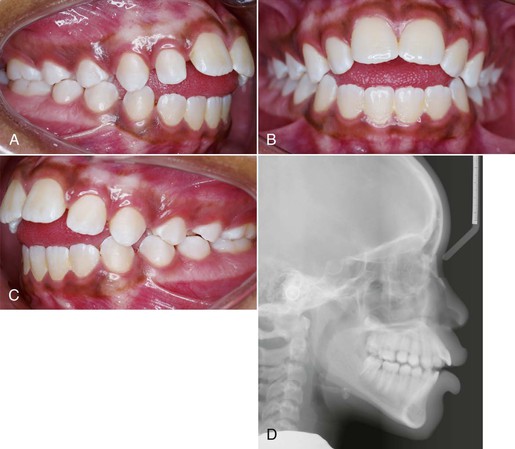
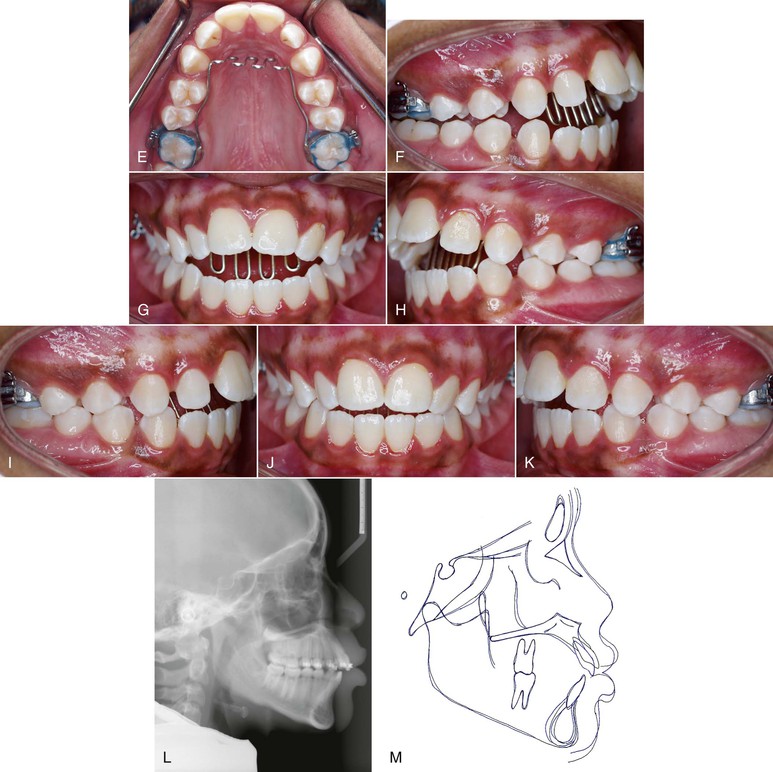
Figure 9-8 A–C, Patient with a finger-sucking habit resulting in an anterior open bite mesial to the first premolars. D, Lateral cephalogram showing characteristics of a dental open bite. E–H, Habit appliance with loops acting as a mechanical obstruction in close approximation to the anterior portion of the palate. I–K, Spontaneous correction of the anterior open bite after habit appliance delivery. L, Lateral cephalogram showing the open-bite closure. M, Superimposition reflecting the incisor extrusion that results with spontaneous closure of an anterior open bite with the habit appliance.
Treatment of Tongue Thrusting
Patients with tongue thrusting can be treated effectively in the same manner as that used for patients who suck on a thumb or finger (Fig. 9-9), although different appliances, such as the habit appliance with lingual spurs or cribs (Fig. 9-10), have been suggested. In one study,62 immediately after crib placement the tip of the tongue was positioned posteriorly during all stages of deglutition. Additionally, the anterior and middle parts of the dorsum of the tongue were at a lower position, reflecting a compensatory functional change for bolus propulsion and airway protection. However, no significant change occurred in the posterior part of the dorsum. Taslan et al.63 reported a decrease in resting tongue pressure and swallowing pressure from 21 g/cm2 to 13 g/cm2 and 216 g/cm2 to 143 g/cm2, respectively, after 10 months of tongue crib therapy in patients with anterior open bite. This decrease in tongue pressure at rest and swallowing pressure after crib therapy was suggestive of tongue adaptation in response to the altered environmental changes. This altered tongue posture aided in the correction of an anterior open bite through an increase in overbite of 3.6-mm. The increase in overbite was attained by lingual inclination of the maxillary and mandibular incisors by 4 degrees each and by extrusion of 1.4-mm and 1-mm, respectively.64
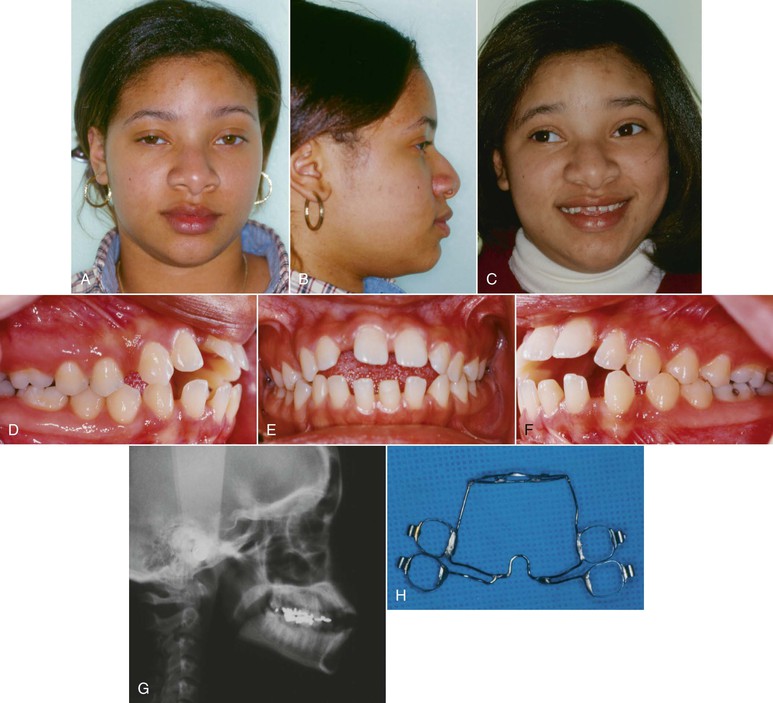
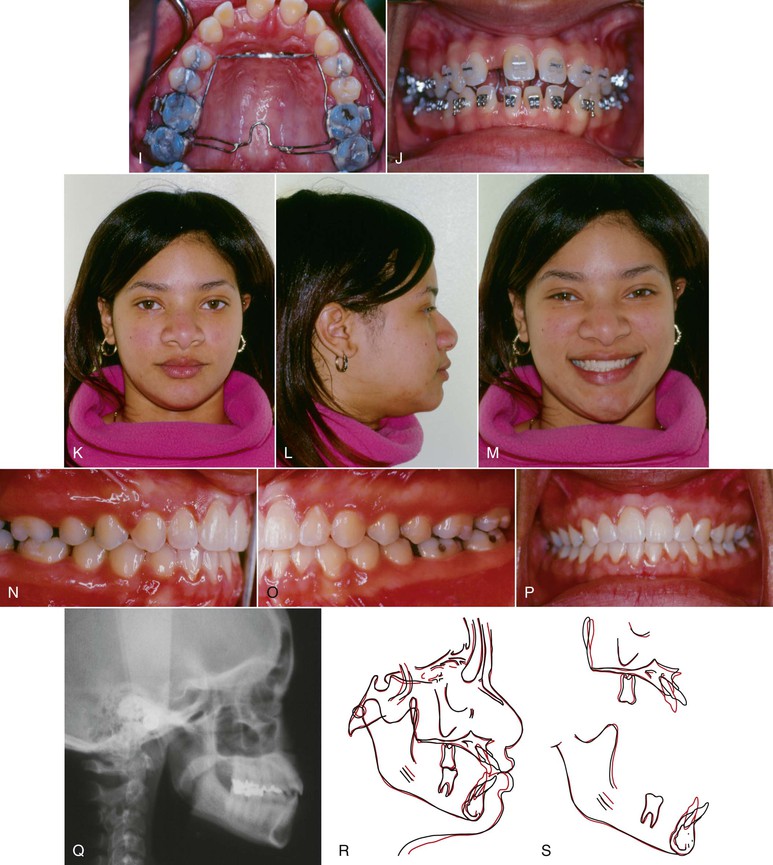
Figure 9-9 Female patient, age 18, with a tongue thrust. A–C, Extraoral views. On smile, only 50% of the incisors are displayed and an anterior tongue posture is evident. A reverse smile arc is consistent with the tongue thrusting habit. D–F, Intraoral views show a 3-mm anterior open bite with divergent occlusal planes from the first premolars. G, Lateral cephalogram shows a dental anterior open bite with dentoalveolar protrusion. H, Habit appliance with first and second molar bands and anterior loop design close to the palate. I, Intraoral view of the cemented habit appliance. J, Brackets are placed after 6 months of exclusive treatment with the habit appliance. Fifty percent of the negative open bite self-corrected. K–M, Extraoral views after treatment. A positive smile arc was obtained, with approximately 90% incisor show on smile. N–P, Adequate overbite was achieved with a good Class I relationship. Q, Final lateral cephalogram shows the overbite correction. R, General superimposition shows no maxillary or mandibular growth. Controlled lingual tipping of the upper and lower incisors reduced the dentoalveolar protrusion and anterior open bite. S, Regional maxillary and mandibular superimpositions show the same dental movements described previously (pre-treatment age, 18.8 years; post-treatment age, 21.5 years).
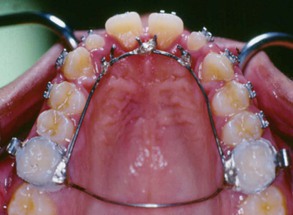
Figure 9-10 Habit-breaking appliance with lingual spurs.
Other devices to retrain the tongue posture, known as myofunctional appliances, are also effective in treating tongue thrusts. Myofunctional therapy aids in muscle retraining by using a series of tongue exercises to correct the deleterious resting and functional postures65 and corrects the tendency for hyperdivergent growth. Types of functional appliances include the Frankel functional regulator, bionators, activators, and twin blocks.
In a longitudinal study,66 considerable decreases in mandibular plane angle, palatal plane to mandibular plane angle, and gonial angle occurred in a group of patients treated with functional regulators. Compared with findings in the control group, the ratio of the upper to the lower anterior facial height and the ratio of the anterior to the posterior facial height changed to normal values in the treatment group. Improvement in skeletal open bite was due to lengthening of the ramus and favorable compensatory growth at the condyles. The functional regulator did not remove the wedge by intruding the molars. The authors66 hypothesize that the forward rotation of the mandible is due to postural balance between the forward and backward rotating muscles brought about by lip seal exercises. Of note, the goal of most treatment strategies for patients with hyperdivergent facial patterns is to intrude the molars. On the contrary, correction with the functional regulator was primarily achieved by changing the existing deviant functional pattern of muscular environment.
Treatment of Macroglossia
If macroglossia is diagnosed, surgical resection may be performed to reduce the volume of the tongue. The open bite can then be corrected by retraction of the anterior teeth. After treatment, stability most likely will be enhanced, because the reduced tongue volume will better match the reduced arch length obtained after retraction of the incisors (Fig. 9-11). Although this procedure may help in the reduction and stability of anterior open-bite correction, the morbidity of the procedure, with potential sequelae in taste, sensation, and motor dysfunction, explains why this approach is not often chosen.45,67
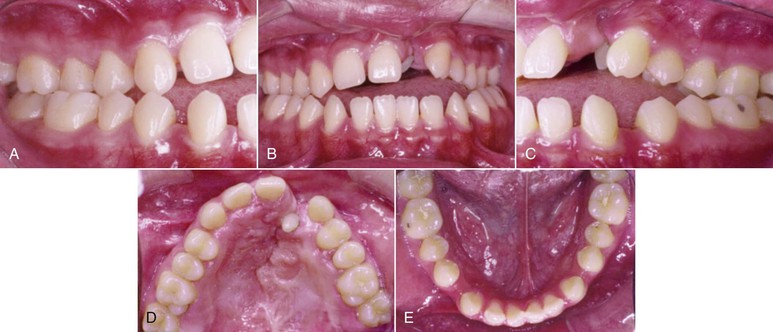
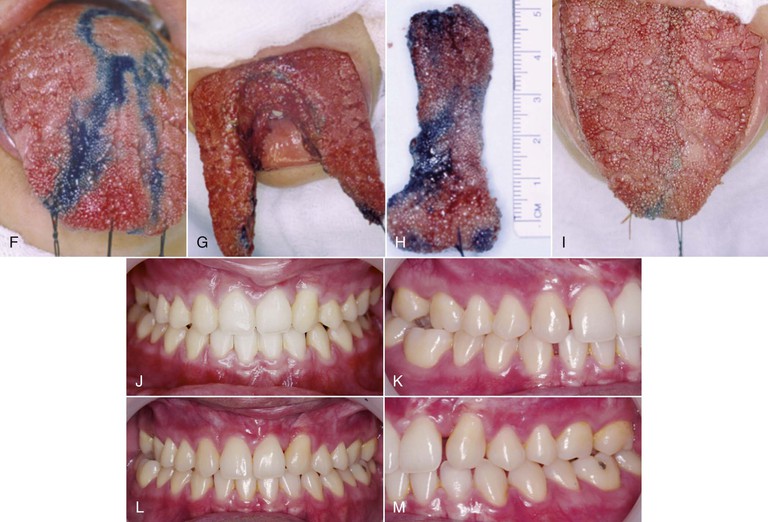
Figure 9-11 A–E, Intraoral views of a patient with a unilateral left cleft lip and palate. Significant spacing is observed in the lower arch due to a large tongue. F, Keyhole-design glossectomy. G–I, Lateral borders of the tongue to be approximated after tissue mass reduction. J, Anterior open-bite closure after surgical orthodontic treatment. K–M, Intraoral views illustrating 9-year stable result.
Treatment of Airway Obstruction
Procedures that promote better breathing through the nose (turbinate surgery, adenoid and tonsil removal, allergy treatment) may help to reestablish normal growth patterns.68 However, the growth direction of the mandible among patients varies greatly after any of these procedures.69 This variability makes the decision to intervene with a resective surgical procedure difficult. Therefore the diagnosis of upper airway obstruction and the decision for surgical intervention should always be made by an appropriate team of specialists.
Correction of Open Bite by Incisor Extrusion
Extrusion of the upper and lower incisors is a common orthodontic treatment for anterior open bites. This treatment is appropriate if the patient has an open bite with a normal skeletal pattern but may also be used in patients with vertical dysplasias who have deficient incisor display at rest and when they smile. However, most patients with long face morphology and anterior open bite have posterior as well as anterior vertical maxillary excess (Fig. 9-12
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses