9
Impacted Teeth in the Adult Patient
Neglect and disguise
Management
The need for temporary prostheses during the treatment
Supplementary clinical concerns
Tooth transposition and temporary prosthetic replacement
The unerupted third molar as a potential bridge abutment or antagonist for an unopposed tooth
Neglect and Disguise
A small but significant number of untreated impacted teeth will eventually find some way of erupting into the mouth without treatment, although this may be many years after their normal eruption time and then often into an ectopic eruption site. This is particularly true of maxillary canines [1] and, at least to a degree, in contradiction to the popular view that eruption potential is lost when the root apex closes [2]. Nevertheless, a good proportion will remain unerupted and asymptomatic for many years. Prosthodontists are aware of the occasional patient complaining of the eruption of a tooth under a denture often many years after the patient had become otherwise edentulous.
For the most part, during the childhood of the particular adult patient concerned, advice was probably sought and rejected, with the reasons for this being very varied. The patient may have been an orthodontically unmanageable child at the appropriate age; perhaps the dentist or orthodontist was insufficiently convincing in the task of informing the parent of the consequences of non-treatment; or the parents’ level of dental awareness was inadequate, the idea that surgery would be needed was possibly abhorrent to the parents or simply the cost and duration of the proposed treatment were unacceptable.
Just occasionally, a surgical exposure procedure would have been carried out at the appropriate time, but failed to elicit eruption and was not then followed up. Some impacted teeth, particularly maxillary canines, may simply have never been diagnosed. One further possibility that is not unfamiliar is that a dentist succumbed to the pleadings of the parent to ‘do something temporary to make it look good’, until they would be ready for the definitive treatment – a time that never arrived!
The Impacted Maxillary Central Incisor
It may be difficult for the orthodontist to imagine the situation where a patient has reached adulthood still with an impacted central incisor. This will have been obvious from around the age of 7 years, but the patient only sought treatment in his/her twenties or even later. This type of neglect is indeed unusual and its prevalence seems likely to vary from country to country, in inverse proportion to the level of dental awareness in the population. A country that offers its citizens some form of national dental insurance may be expected to have a lower prevalence among its adults, since one would hope that treatment would have been carried out at the appropriate time, given the relative freedom from financial constraints in a welfare state. Cost, however, is not the only factor, probably not even the dominant one.
Whatever the reason, the adult patient will usually present with the incisor anomaly unsuccessfully disguised in one of three ways:
1. A retained deciduous tooth may have been enlarged with the addition of composite material, although this will probably only have improved its length. Any increase in its width will be limited by the reduced mesio-distal space available to the tooth, the result of the marked mesial tipping of the adjacent lateral incisor and the central incisor of the opposite side.
2. This reduced space may have been maintained with a ‘flipper’ (spoon) partial denture, carrying a single and poorly matched small tooth (Figure 9.1a, b).
3. The lateral incisor may have been enlarged, with the use of composite material, in an attempt to simulate the shape of the impacted central incisor (Figure 9.2a).
Fig. 9.1 Impacted right maxillary central incisor (a) replaced by poorly matched artificial tooth on ‘flipper’ (spoon) denture (b).
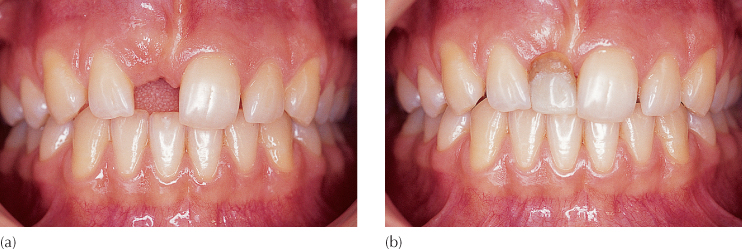
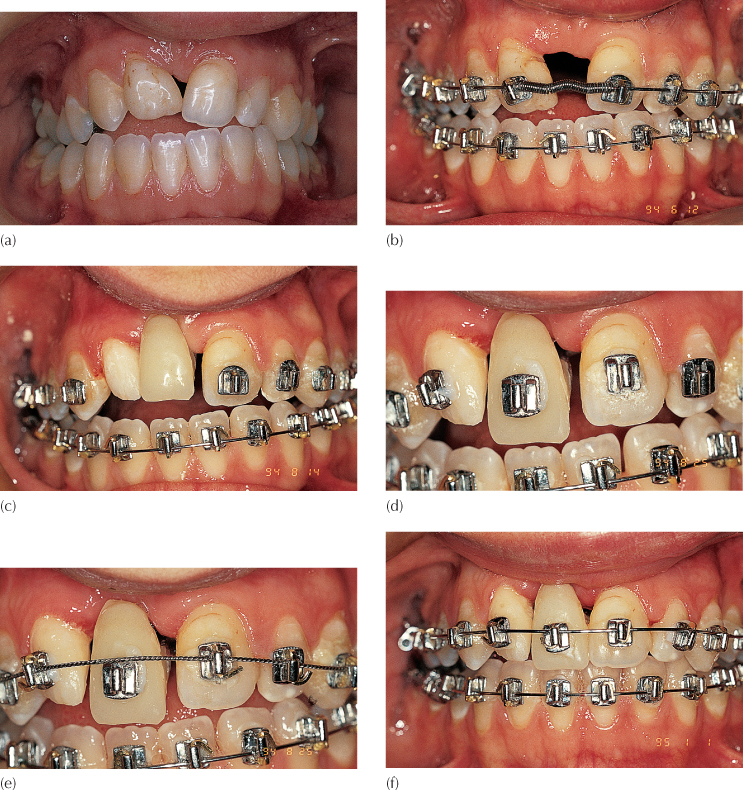
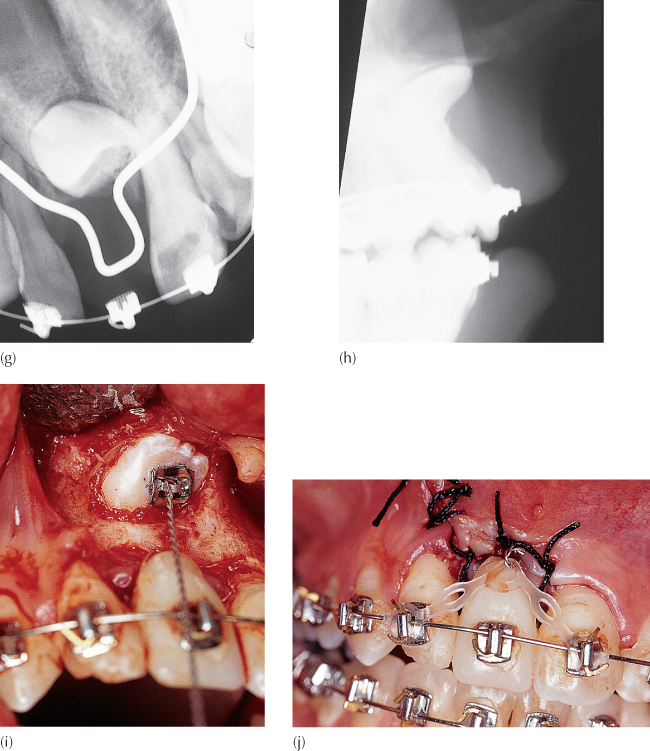
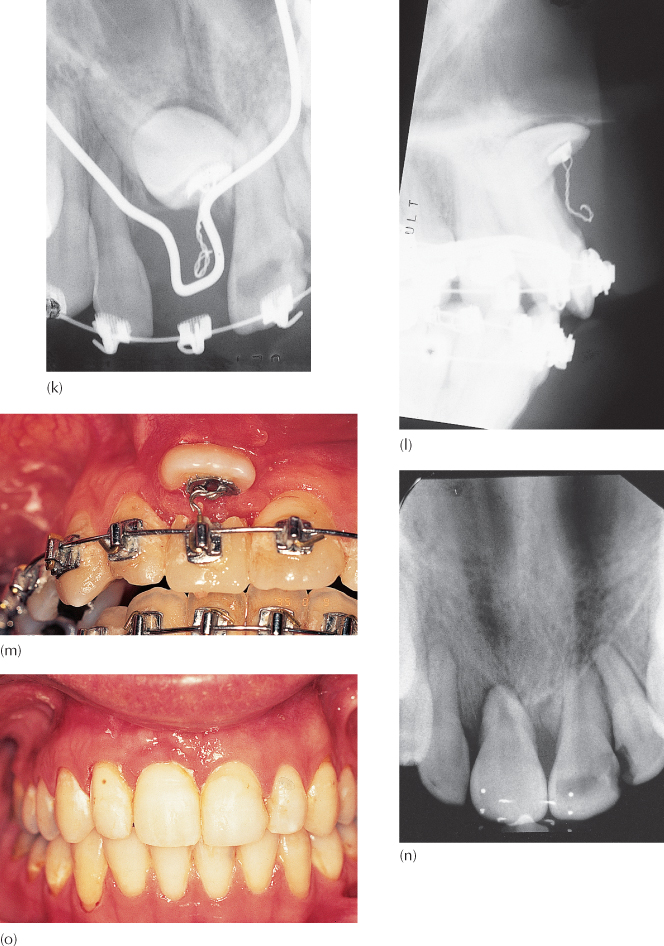
Fig. 9.2 (a) Impacted right maxillary central incisor. The right lateral incisor crown has been enlarged by a composite build-up. (b) Initial stages of alignment and space-opening. The composite build-up of the maxillary right lateral incisor is still in place. (c) Space has been reopened, the composite build-up of the lateral incisor has been removed and the artificial central incisor is in place, attached to the soldered palatal arch closing the anterior open bite. (d) The soldered arch has been deflected slightly vertically downwards to elongate the artificial tooth. (e) Placement of the archwire shows the degree of vertical displacement. The artificial tooth is now fully engaged in the archwire. (f) The extrusive force of the palatal archwire closes off the open bite. (g) The periapical view shows the impacted tooth to be dilacerated. The palatal arch is clearly seen, with the forward-pointing loop used to carry the radiolucent artificial tooth. An orthodontic bracket is also attached to this radiologically invisible tooth. (h) Pre-treatment tangential radiograph. (i) Bonding of an eyelet to the anatomically palatal aspect of the incisor crown. (j) The elastic chain is gently raised and ensnared in the pigtail to provide immediate and controlled vertical traction. (k) Post-surgical periapical view to show the bonded eyelet and pigtail ligature. (l) The tangential view post-surgery showing the length of the unseen part of the ligature and the relative heights of the tooth, the ligature extremity, and the occlusal plane. (m) The impacted tooth has erupted five months later: note the reduction of the cervical portion of the artificial tooth to allow for further progress. Traction was made to a newly placed labial attachment at this juncture. (n) Periapical view of the dilacerate incisor at the completion of treatment. (o) The orthodontic result: note the gingival appearance of the treated and untreated maxillary central incisors.
There are serious drawbacks with each of these treatment alternatives, which focus principally on the very poor appearance of the results. The absence or reduction in size of a central incisor is always obvious, as is any significant shift in a maxillary dental midline, even to the casual observer. The tipping of the two teeth adjacent to the impacted incisor is too severe for this to escape notice and the angle of the lateral incisor is too acute for its long axis to be visually ‘realigned’ by composite additions or by reshaping. The narrowness of the neck of the tooth makes an aesthetically convincing reconstruction, as a central incisor, difficult to achieve.
Management
It is quite clear that in these circumstances the first and most important prerequisite to any form of treatment for the missing tooth is to provide the maxillary dental arch with an ideal shape in each of the three planes of space. In practical terms, this means:
- Levelling and aligning the entire dental arch. All ectopically placed teeth will need to be brought into an ideal archform, teeth will need to be aligned in a single, uniform occlusal plane and all rotations dealt with.
- Reopening a space of suitable mesio-distal width in order to accommodate the impacted tooth in the arch. Correcting the palatal inclination of the canine and tipping the lateral incisor of the same side and the central and lateral incisor of the opposite side will usually provide adequate space, although distal movement, extraction or interproximal enamel stripping may need to be considered.
- Correcting the dental midline, to be continuous with the lower and with the midline of the face. This is normally achieved as a result of the reopening of space, but it may require the use of coil springs or anterior, oblique, intermaxillary elastics as part of a more comprehensive orthodontic appliance programme. The use of anterior intermaxillary elastics in the adult is often a difficult request to put before the patient for obvious social reasons. The judicious placement of temporary anchorage devices to permit forces to be applied unilaterally within the same arch is clearly to be preferred.
- Closing down an anterior open bite and bringing the teeth into occlusion. This may sometimes be achieved by properly aligning the molar tubes and by altering bracket height on the anterior teeth, thereby bringing about the desired extrusion of the teeth − and unpopular anterior vertical elastics are of material help in this situation. Often, however, an increased height of the lower third of the face and excessive vertical exposure of the maxillary anterior teeth and gingivae (gummy smile) may dictate the intrusion of the posterior teeth rather than extruding the anteriors. This may be achieved using zygomatic plates screwed into the inferior aspect of the zygomatic process of the maxilla, opposite the molar teeth. In this scenario, it should be understood that a force applied from a zygomatic plate, high in the sulcus, to the buccal tube on the molar will produce a rolling-out of the molar. It is therefore mandatory to use a transpalatal bar, preferably soldered from molar to molar. This bar should be prepared in such a manner as to be positioned a couple of millimetres away from the palatal mucosa to permit molar intrusion without palatal impingement.
Once these aims have been achieved, the patient is ready for that stage in treatment when all resources will need to be concentrated on the impacted tooth. The entire dental arch must be consolidated into a compound and united anchorage unit, to which the unerupted tooth will be drawn. In Chapters 6 and 7, it was noted that teeth that have been impacted for many years sometimes undergo pathological change which prevents their eruption [3], even when all other factors are favourable. It is by no means always possible to diagnose pathological change from a radiograph, unless there is a loss of the follicular sac and actual enamel resorption has become evident over wide areas of the surface of the unerupted tooth. It is therefore true to say that, whenever an adult patient presents for the treatment of an impacted tooth, a calculated risk is taken in offering this kind of treatment to resolve the impaction.
In the most adverse of circumstances, the central incisor tooth will have to be extracted and, perhaps, replaced with an implant-borne restoration. In that event, the preparation of the dental arch described above will have provided optimal clinical conditions to accept the implant or other form of artificial restoration of the space. An ideal pontic width is present, the roots of the adjacent teeth have been uprighted to make sufficient inter-radicular space for implant placement, all other teeth are aligned and the occlusion is good. However, the surgical removal of a grossly displaced impacted tooth, high above its normal position, will leave a considerable and unsightly bony defect. This will be difficult to conceal in the gingival area around a fixed prosthesis and will not lend itself to the placing of an implant without suitable and prior osseous ridge reconstruction [4–7].
The patient must be brought into the decision-making process from the outset and should be informed of the potential advantages of each of the stages of treatment. This is best done using a set of plaster models of the patient’s teeth, together with a wax duplicate set-up, to show a scheme of the proposed treatment result. Prognosis for the success of the pre-surgical stages of the treatment is excellent, but for the alignment of the impacted tooth it is not so certain. Offering the treatment plan to the patient is, therefore, probably best accomplished if it is based on explaining the benefits of the limited objectives, i.e. aligning the teeth for the purposes of achieving improved conditions for the construction of a conventional prosthodontic or implant-borne replacement. The added bonus, which will be derived from success in the resolution of the impaction, may then be properly brought into perspective to provide the desirable added incentive. By whatever means the value of the treatment is explained, care should be taken to fully inform the patient that the possibility of failure to bring the impacted tooth into the arch is real, but that contingency plans are available in this disappointing eventuality.
The Need for Temporary Prostheses During the Treatment
The Impacted Central Incisor
For the adult patient, planned orthodontic space opening for an unerupted anterior tooth is a daunting prospect. All central and lateral incisors and maxillary canines require some form of immediate temporary prosthetic replacement until such time as the permanent tooth comes into its place. With some patients, particularly those more concerned with their appearance or those who have a broad smile or a wide dental display which is evident in facial expression and social intercourse, there may be a need to artificially replace even premolar teeth.
Perhaps the most popular solution for an impacted incisor is to trim an artificial acrylic tooth to a suitable shape and size, bond a bracket to it and ligate it into the archwire of the appliance. In the early stages, the archwire is probably nickel−titanium and of round cross-section, which means that the new artificial pontic is very unstable and will rotate around or slide along the archwire. Placing a V-bend in the wire or welding a small piece of wire in the vertical position will prevent the rotation but complicate use of the archwire. It will also need to be copied into each of the subsequent archwires until a rectangular cross-section wire is used.
An artificial acrylic tooth may be bonded to the mesial surface of the contralateral central or ipsilateral lateral incisor, although this assumes that the archwire is absolutely passive when ligated into the bracket on these teeth. A minor rotatory movement will cause a major lateral or medial swing of the pontic, while an uprighting component will markedly intrude or extrude it at its opposite end.
Alternatively, the artificial restoration may take the form of a removable plate carrying a single tooth − a ‘flipper’ (spoon) denture. The average adult patient may have considerable difficulty becoming accustomed to it, even if its retention is adequate initially. Of greater concern, however, is the fact that the adjacent teeth and many other teeth need to be moved during the orthodontic treatment, which will rapidly make this artificial denture ill-fitting. Furthermore, the close adaptation of the acrylic base to the contour of the other teeth in the jaw may actually interfere with the planned orthodontic movement. For this type of artificial replacement to be successful, Adams clasps may have to be used on the second molars; alternatively, a modified circumferential clasp may hook over the buccal tubes of the first molars. These teeth are often excluded from the planned dental movements and may sometimes be helpful in retaining such a plate, although the distance between the clasps and an incisor pontic may be the cause of an unacceptable degree of instability.
Clearly, more satisfactory alternative methods of artificial replacement are essential to the successful pursuit of treatment for the adult patient, and these must provide an answer to the several shortcomings of the ‘flipper’ denture. Indeed, given a little thought in their design, and rather than their playing the role of the villain of the piece, assistance in the application of force to the impacted tooth may be derived from the method of artificial replacement, which may actually contribute to the smooth running of the active orthodontic appliance.
The Active Removable Plate
If a removable plate is to be worn to hold the artificial tooth in place, it makes good sense to augment that plate with active elements that will also produce tooth movement. Looked at in a different way, this means designing a simple removable orthodontic appliance carrying springs of one sort or another, which are aimed at realigning the teeth to reopen the anterior space and, at the same time, to fill that space with an artificial tooth.
This method has some important advantages. The active plate is straightforward and easy to use, requiring very limited expertise in adjustment of the forces applied and in their direction. Because the plate is removable and generally adjusted at the chair side out of the mouth, the size and shape of the artificial tooth may be easily altered in size or speedily replaced as space opening occurs, to maintain appearance.
However, the active removable appliance is unable to produce more than tipping movements of the adjacent teeth. Methods have been described where removable appliances have been used to produce the extrusive mo/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


