8
Management of Posterior Crossbites
Definition of Posterior Crossbite
In normal occlusion, the buccal surfaces of the upper posterior teeth project farther buccally than the buccal surfaces of the lower posterior teeth. This projection is termed buccal overjet. In posterior crossbite malocclusions, the buccal surfaces of lower teeth project farther buccally than the buccal surfaces of the upper posterior teeth. Posterior crossbites have six possible explanations: (1) The upper arch is too narrow, (2) the lower arch is too wide, (3) a lateral functional shift occurs during closure of the mandible, (4) one or more teeth are displaced toward the palate in the maxillary alveolar ridge, (5) one or more teeth are displaced toward the buccal side of the mandibular alveolar ridge, and (6) combinations of the above explanations.
The number of teeth in crossbite can vary from one upper tooth and one lower tooth to all the posterior teeth on one or both sides of the arch. The number of teeth involved in crossbite is a guide to the severity of the problem: the more teeth involved, the more difficult is the treatment.
Prevalence of Posterior Crossbite Malocclusions
The U.S. Public Health Service surveyed the incidence of posterior crossbites in a large sample of whites, blacks, and Mexican Americans from 1988 to 1991 (Table 8.1) (Brunelle, Bhat, and Lipton 1996). The prevalence of posterior crossbites for all persons was 9.4%. No significant differences were observed between the races and genders. A positive association was observed between increased prevalence of posterior crossbites and increased incisor irregularity.
Table 8.1. Prevalence of Posterior Crossbite by Age, Gender, and Race of Americans Ages 8 to 50 Years, 1988–1991
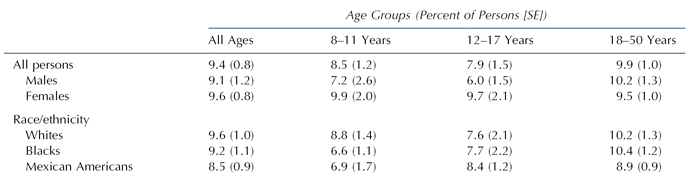
From Brunelle, Bhat, and Lipton (1996).
Angle Classification
Patients having Class I occlusions without crowding are the best candidates for limited treatment of posterior crossbites. Patients who have Class II and Class III malocclusions with posterior crossbites are best treated by a specialist, because their treatment is complex and lengthy.
Intermolar Width Measurements
In unilateral and bilateral posterior crossbite malocclusions, measurement of the upper and lower intermolar widths and comparison of these widths to the widths of males and females who have normal occlusion will help determine whether the upper arch, lower arch, or both are part of the etiology of the crossbite (adult arch width norms are given in Figure 3.5, chapter 3).
The difference between the upper and lower intermolar widths will provide an estimate for the amount of expansion needed to correct the crossbite. Approximately 1.5 mm in males and 1.2 mm in females should be added (absolute sum) to the intermolar width difference to expand the arch enough to ensure normal buccal overjet. The intermolar width difference is also a guide to select patients for limited treatment. Intermolar width differences between 1 mm and 6 mm are recommended for limited treatment. Patients with differences greater than 6 mm are best treated by specialists.
The intermolar width difference is also a guide for selecting appliances to correct the crossbite. Removable appliances are adequate for correcting crossbites requiring 1 mm to 5 mm of intermolar expansion. Corrections requiring 5 mm or more of intermolar expansion are best treated by fixed appliances, such as the quad helix and fixed W spring appliances. Crossbites requiring 6 mm or more of correction are best treated with rapid maxillary expansion (RME) appliances. Rapid expanders separate the maxillary suture, thereby treating the underlying etiology of skeletal narrowness and moving the teeth more bodily, which increases the probability of obtaining a more stable treatment of the posterior crossbite.
Age of Patient
Posterior crossbites are best treated in children and adolescents. Adults have maxillary sutures that are hard to open and many need surgically assisted RME (SARME) to effectively correct a posterior crossbite.
Buccolingual Inclination of the Posterior Teeth
If an upper molar in crossbite is inclined lingually, the inclination is favorable, because correcting the crossbite will improve its inclination by tipping the tooth to a more normal inclination. If an upper molar in crossbite is inclined buccally, the inclination is unfavorable, because correcting the crossbite will increase the buccal inclination to an even greater abnormal buccal inclination. Excessive buccal inclination of upper molars may be the result of a skeletal narrowness of the upper arch that caused a dental compensation (excessive buccal inclination) of the upper molars to accommodate for the skeletal discrepancy between the maxilla and mandible. In such cases, fixed RME appliances are recommended for treatment, because they will expand the suture and help control the inclination of the buccally inclined molars.
Abnormal buccal inclination of a lower molar in crossbite is favorable, because moving the molar to a more normal inclination will help to correct the crossbite. A lingually inclined lower molar in posterior crossbite is unfavorable. Excessive lingual inclination of the lower posterior teeth must be reckoned with in calculating the need for maxillary expansion. Buccal movement of lingually inclined lower posterior teeth to more normal inclination increases the goal for maxillary expansion. In patients with lingually inclined lower posterior teeth, the lower arch is expanded along with the upper arch.
Etiology of Bilateral and Unilateral Posterior Crossbites
In centric occlusion, two basic types of posterior crossbites are observed: bilateral and unilateral.
Bilateral posterior crossbites have a close correspondence between centric occlusion and centric relation in Class I and Class II malocclusions. In Class III malocclusions, an anterior crossbite is often associated with a bilateral posterior crossbite, thereby introducing the possibility of an anteroposterior functional shift. Bilateral posterior crossbites have two basic etiologies: (1) the upper arch has narrower than normal width and the lower arch has normal or larger than normal arch width and (2) the upper arch has normal width and the lower arch has larger than normal width. Bilateral crossbites with both of these etiologies are therefore treated with appliances that move teeth on both sides of the upper arch in a buccal direction. Measuring the upper and lower arch widths will help the clinician understand the etiology of the crossbite and decide how much expansion is needed to correct the posterior crossbite.
Unilateral posterior crossbites have five etiologies:
(1) The upper arch has narrower than normal width and the lower arch has normal or larger than normal width, (2) the upper arch has normal width and the lower arch has larger than normal width, (3) premature tooth contacts deflect the mandible laterally during closure and the upper and lower arch widths are normal, (4) etiology #1 in combination with premature tooth contacts, and (5) etiology #2 in combination with premature tooth contacts. Effective treatment of unilateral posterior crossbites requires a diagnosis based on careful clinical observation for premature tooth contacts and measuring the upper and lower arch widths and comparing them to a norm.
Most patients who have a unilateral posterior crossbite shift their mandibles toward the side of the crossbite when closing into centric occlusion. This lateral functional shift may be caused only by a premature contact (etiology No. 3) or by discrepancies in the upper and lower arch widths (Thilander and Lennartsson 2002). When a unilateral posterior crossbite is associated with a lateral functional shift and a discrepancy in arch widths, it is in reality a bilateral posterior crossbite treatable with appliances that move both sides of the upper arch in a buccal direction. Correction of the crossbite in these patients should eliminate the lateral functional shift. Studies have suggested that the relation between condyle and fossa in persons with unilateral posterior crossbites may become asymmetric (Miyawaki et al. 2004; Nerder, Bakke, and Solow 1999), possibly inducing asymmetric growth of the mandible (Lam, Sadowsky, and Omerza 1999; Pinto et al. 2001). It is further thought that the prolonged asymmetric closure of the mandible in patients with a unilateral crossbite may predispose them to disc displacement and temporomandicular joint (TMJ) clicking (Egermark, Magnusson, and Carlsson 2003; Pullinger, Seligman, and Gornbein 1993). Positive associations between unilateral posterior crossbite and TMJ clicking were reported in several studies (Egermark, Magnusson, and Carlsson 2003; Kritsineli and Shim 1992; Pullinger, Seligman, and Gornbein 1993; Thilander et al. 2002). A recent study of 1291 school-age children, 10 to 16 years old, found no association between posterior unilateral crossbite and TMJ clicking (Farella et al. 2007). Additional well-designed studies are needed to clarify the truth about these associations.
When a lateral shift cannot be readily observed in a patient with a unilateral posterior crossbite, ask the patient to open widely, to determine whether the upper and lower dental midlines are coincident in the open position. If the midlines are coincident when open and deviated when closed, this is evidence that a lateral shift is operating during closure of the mandible. A diagnostic splint can also be used to demonstrate the presence of absence of a lateral shift.
If no lateral shift can be detected, the patient may have a true unilateral posterior crossbite. Most appliances expand bilaterally. In patients with true unilateral posterior crossbites, an expander operating bilaterally will cause the non-crossbite side to move into buccal crossbite as the crossbite side is corrected. Unilateral mechanics such as cross arch elastics are used with a bilateral expander to treat the buccal crossbite side in true unilateral crossbites. In complex true unilateral posterior crossbite patients, surgically assisted RME may be an effective treatment. Patients with true unilateral crossbites should be referred to a specialist.
Vertical Dimension
Overbite is another predictor of difficulty in the treatment of posterior crossbites. Normal overbite is a favorable finding. During the treatment of most posterior crossbites, the bite is opened at least temporarily. If a patient has an anterior openbite or a very deep overbite associated with a posterior crossbite, he should be referred to a specialist.
Treatment of Posterior Crossbites
A systematic review of literature found five randomized clinical trials and eight controlled clinical trials that studied orthodontic treatment of posterior crossbites (Harrison and Ashby 2001). The review authors concluded that evidence reported by Lindner (1989) and Thilander et al. (1984) suggests that the removal of premature contacts of primary teeth is effective in preventing a posterior crossbite from being perpetuated to the mixed dentition and adult teeth. When grinding alone is not effective, using an upper removable expansion plate to expand the upper teeth will decrease the risk of a posterior crossbite from being perpetuated to the permanent dentition. We conclude that bilateral and unilateral posterior crossbites with a lateral functional shift should be corrected in the primary, mixed, or early permanent dentitions with an emphasis on early detection and treatment with the hope of not perpetuating the crossbite and functional shift to the adult dentition.
Correction of Posterior Crossbites with Removable Appliances
For best results, the upper molars of patients receiving expander treatment by a removable appliance should be upright or inclined lingually. Molars that are buccally inclined are not suitable for these appliances that primarily tip molars in a buccal direction. Retention for about 1 year with a Hawley retainer or a trans-palatal arch following active treatment is recommended.
The removable W spring expander is useful in mixed dentition patients who need less than 5 mm of maxillary arch expansion. The treatment of a 9-year 2-month-old mixed-dentition patient with a Class I molar relation and a unilateral posterior crossbite on her right side is shown in Figures 8.1 through 8.6. She had a lateral functional shift of her mandible toward the crossbite side that resulted in a deviation of her lower dental midline to the right side (Fig. 8.1). The crossbite involved the permanent and primary molars (Fig. 8.2). Her upper arch intermolar width was 2 standard deviations narrower than the mixed-dentition norm (Table 8.2) (Fig. 8.3). Her lower arch intermolar width was within normal limits. Her intermolar width difference was −1.2 mm. To create adequate buccal overjet, she needed an additional 1.2 mm expansion for a total of about 2.4 mm. A removable W spring expander is shown in the patient’s mouth (Fig. 8.4). Correction of the crossbite eliminated the functional shift, and the lower dental midline became coincident with the upper dental midline (Fig. 8.5). This correction was the result of a cooperative patient and excellent care by the orthodontist. The permanent and primary molars remained out of crossbite, and the permanent canine and first premolar were erupting 1 year 4 months after the start of treatment (Fig. 8.6).
Table 8.2. Arch Widths at Permanent First Molars in Mixed-Dentition White Subjects with Normal Occlusion at Age 8 Years
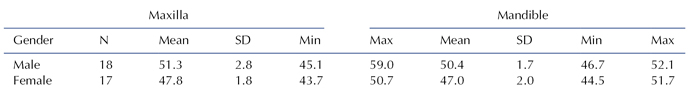
From Grabouski, J., Staley, R., Kummet, C., unpublished data.
Figure 8.1. Patient with a unilateral posterior crossbite and lateral functional shift to the right side. (Courtesy of Dr. John Casko.)
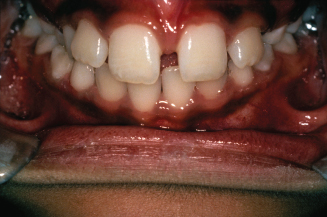
Figure 8.2. View of teeth in crossbite. (Courtesy of Dr. John Casko.)
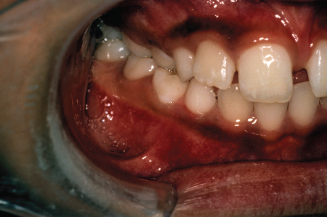
Figure 8.3. Occlusal view of the narrow upper arch. (Courtesy of Dr. John Casko.)
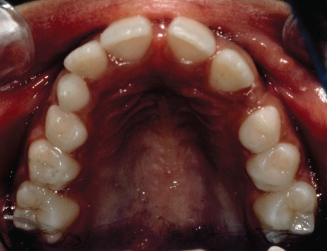
Figure 8.4. View of the removable W spring expander in the mouth. (Courtesy of Dr. John Casko.)
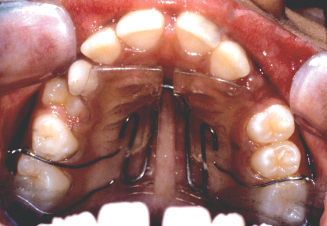
Figure 8.5. After correction of the crossbite, the functional shift was eliminated and the dental midlines were together. (Courtesy of Dr. John Casko.)
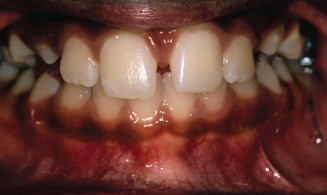
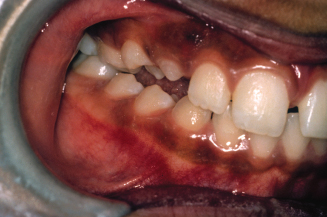
Figure 8.6. Teeth were no longer in crossbite on the right side. (Courtesy of Dr. John Casko.)
A laboratory prescription for a removable W spring expander is shown in Figure 8.7. Construction of the removable W spring expander appliance is illustrated in Figures 8.8 through 8.15. The W spring wire is bent from a 36-mil stainless steel wire. The two Adams clasps are bent from 26-mil stainless steel wire (Adams 1984). The W spring is shaped to fit the palatal contours (Figs. 8.8 to 8.10). The wire is separated from the palatal surface with a 1-mm layer of/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


